In 2019, regular surveillance of 110 English-language research journals identified 254 studies that met the criteria to become POEMs (patient-oriented evidence that matters). Physician members of the Canadian Medical Association rated these POEMs for their relevance to patients in their practices. This article summarizes the clinical questions and bottom-line answers from the top 20 POEMs of 2019. Taking blood pressure medications at night results in a large mortality reduction over six years compared with morning dosing. Automated devices are the best way to measure blood pressure. Nonfasting lipid profiles are preferred over fasting lipid profiles, and nonfasting and fasting lipid profiles are equally effective at predicting risk. The benefit of statins for primary prevention in people 75 years and older is uncertain at best. Aspirin has no net benefit for primary prevention of cardiovascular disease and has no effect on cancer outcomes. An Italian study found fecal immunochemical testing over five biennial screening cycles has a similar colorectal cancer yield as screening colonoscopy, whereas a meta-analysis found that taking aspirin, an anticoagulant, or a nonsteroidal anti-inflammatory drug has no impact on the positive predictive value of fecal immunochemical testing. Regarding infections, a meta-analysis showed that patients presenting with symptoms of acute respiratory tract infection are unlikely to have pneumonia if vital signs and the lung examination findings are normal. For streptococcal pharyngitis (strep throat), penicillin V at a dosage of 800 mg four times a day for five days is at least as effective as a dosage of 1,000 mg three times a day for 10 days. A primary care study in the United Kingdom reinforced that clinicians should counsel parents of children with lower respiratory tract symptoms to be patient, because these infections can take three weeks or more to fully resolve. Among direct oral anticoagulants, apixaban has the lowest bleeding risk, and cotreating with a proton pump inhibitor significantly reduces bleeding risk. Single ibuprofen doses from 400 to 800 mg significantly reduce acute pain to a similar degree. The two-dose recombinant zoster vaccine is much more effective than the single-dose live, attenuated vaccine but with a greater risk of injection site pain. Exercise helps reduce the risk of falls in older adults. Practice guidelines from 2019 on antithrombotics for atrial fibrillation, the management of type 2 diabetes mellitus, and screening for breast cancer were judged to be especially relevant.
Every year for the past 21 years, a team of experts in evidence-based medicine have systematically reviewed more than 110 English-language research journals to identify the original research most likely to change and improve primary care practice. The team includes experts in family medicine, pharmacology, hospital medicine, and women's health.1,2
The goal of this process is to identify POEMs (patient-oriented evidence that matters). A POEM must report at least one patient-oriented outcome, such as improvement in symptoms, morbidity, or mortality. It should also be free of important methodologic bias, making the results valid and trustworthy. Finally, if applied in practice, the results would change what some family physicians do in patient care by prompting them to adopt a beneficial new practice or discontinue one that is ineffective or harmful. This should improve patient outcomes. Of more than 20,000 research studies published in 2019 in the journals reviewed by the POEMs team, 254 met criteria for validity, relevance, and practice change.
The Canadian Medical Association (CMA) purchases a subscription to POEMs for its members, many of whom receive the daily POEM by email. When members read a POEM, they can rate it with a validated questionnaire called the Information Assessment Method. POEM ratings address the domains of clinical relevance, cognitive impact, use in practice, and expected health benefits if that POEM were to be applied in patient care.3,4 In 2019, each of the 254 POEMs were rated by an average of 1,530 physicians.
In this article, we present the 20 POEMs rated highest for clinical relevance by CMA members in 2019. This installment of our annual series (https://www.aafp.org/afp/toppoems) summarizes the clinical question and bottom-line answer for each research study identified as a top 20 POEM, organized by topic and followed by a brief discussion. We also present the three most relevant practice guidelines identified by CMA members. The full text of the POEMs in this article are available at https://www.aafp.org/journals/afp/content/top-poems/2019.html.
Hypertension
Hypertension is among the most common conditions managed by primary care physicians and is the topic of the two POEMs rated most relevant to readers in 2019 (Table 1).5,6 Researchers randomized 19,168 adults with hypertension to take their antihypertensive medications at bedtime or first thing in the morning.5 Patients were prescribed an antihypertensive from an approved list of the most common therapies. Patients taking their medications at bedtime had a lower likelihood of the composite outcome of myocardial infarction (MI), coronary revascularization, heart failure, stroke, or cardiovascular death (hazard ratio = 0.55; 95% CI, 0.50 to 0.61; number needed to treat to prevent one event over 6.3 years = 20). All-cause mortality was reduced to a similar extent. This is a large effect for a six-year study, and a practice-changer for many patients and physicians. Best of all, it costs nothing to make this change. See Editor's Note
TABLE 1. Hypertension

| Clinical question | Bottom-line answer |
|---|---|
| 1. Does bedtime ingestion instead of morning ingestion of hypertension medications produce better cardiovascular disease risk reduction in adults with hypertension?5 | Bedtime dosing of antihypertensives improves outcomes. This study found a significant reduction in mortality and morbidity among patients who took their once-daily antihypertensive medications at bedtime instead of on awakening in the morning. Although there was no significant difference in adherence rates between bedtime and morning ingestion times in this study, individual experiences may differ in clinical practice. See Editor's Note |
| 2. Is fully automated blood pressure measurement more accurate than manual sphygmomanometry?6 | Use automated blood pressure measurements to guide treatment. There are two takeaways from this analysis. (1) Automated measurement aligns better with ambulatory blood pressure monitoring (the best predictor of cardiovascular events) than manual measurement. (2) Manual readings are an average of 13.4 to 14.5 mm Hg (systolic) higher than daytime ambulatory or automated readings in patients with hypertension. |
How we measure blood pressure continues to be a subject of research. The next POEM was a meta-analysis of 31 studies, which included a total of 9,279 patients and compared automated in-office blood pressure readings with in-office manual measurements or ambulatory automated recordings during waking hours (the reference standard).6 Automated in-office measurements were performed without anyone present to activate the machine and used three to five readings separated by one- to two-minutes. Ambulatory automated measurements were 13.4/5.9 mm Hg lower than the manual in-office measurements and were similar to the in-office automated measurements. To avoid starting or intensifying antihypertensive medication unnecessarily, it is critical to measure blood pressure using an automated device. Patients should also bring in their home device so that it can be calibrated with the office device.
Behavioral Medicine
Behavioral medicine POEMs are summarized in Table 2.7–9 The first POEM in this group was a well-executed network meta-analysis of medical therapy for generalized anxiety disorder.7 A network meta-analysis includes studies comparing drugs with each other and with placebo, allowing for direct and indirect comparisons. The meta-analysis included 89 studies involving 25,000 patients and 22 different drugs; none of the studies were longer than 26 weeks. After excluding drugs that were poorly tolerated such as quetiapine (Seroquel), paroxetine (Paxil), and benzodiazepines, the most effective commercially available drugs overall were, in order of effectiveness, bupropion (Wellbutrin), duloxetine (Cymbalta), mirtazapine (Remeron), hydroxyzine, sertraline (Zoloft), pregabalin (Lyrica), venlafaxine, escitalopram (Lexapro), fluoxetine (Prozac), buspirone (Buspar), and citalopram (Celexa). Drugs that did not significantly decrease anxiety scores included imipramine, maprotiline, opipramol (not available in the United States), tiagabine (Gabitril), vilazodone (Viibryd), and vortioxetine (Trintellix). The drugs with the best combination of effectiveness and tolerability were duloxetine, pregabalin, venlafaxine, and escitalopram.
TABLE 2. Behavioral Medicine

| Clinical question | Bottom-line answer |
|---|---|
| 3. Which medications are effective in treating patients with generalized anxiety disorder?7 | Duloxetine, pregabalin, venlafaxine, and escitalopram were the most effective and best tolerated drugs for generalized anxiety disorder. In this network meta-analysis, the drugs that had the best combination of effectiveness and tolerability in patients with generalized anxiety disorder were duloxetine (Cymbalta), pregabalin (Lyrica), venlafaxine, and escitalopram (Lexapro). Quetiapine (Seroquel), paroxetine (Paxil), and benzodiazepines were effective but poorly tolerated. |
| 4. How often do patients fail to disclose their symptoms during a visit to their primary care physician?8 | Patients often fail to disclose important symptoms. Symptoms that are not often disclosed include those that patients may consider to be sensitive, such as anxiety, depression, and sexual or interpersonal problems. It is important that primary care physicians remain aware of this, look for cues, and make sure patients know they have permission and a safe space to discuss these issues. |
| 5. Does a lack of early symptom improvement in patients treated for depression predict treatment failure?9 | Stay the course with depression treatment; one-third of early nonresponders responded by six weeks of treatment. Response to treatment within the first two weeks predicts eventual response or remission, but a lack of early response does not predict treatment failure. Approximately one-third of patients who do not show an early response will respond by six weeks. No individual symptom response predicts eventual improvement. |
The next POEM included videotaped encounters between 252 patients and 15 English primary care physicians.8 Patients were asked about the main reason for their visit beforehand, and this reason was almost always addressed during the visit. However, of the 139 patients who identified at least one symptom in the previsit interview, 43 failed to disclose a total of 67 symptoms during the visit, most often stress, worries or sadness; tiredness or sleep problems; problems passing urine; headache; and intimate or other personal problems. Although physicians cannot ask every patient about all of their problems during a visit, it is important to know that patients may not fully disclose symptoms. Physicians should make patients feel as safe as possible while looking for cues to undisclosed symptoms, and routinely asking, “Is there anything else I can help you with?”
The last POEM in the behavioral medicine group was an individual patient data meta-analysis of how early treatment response impacts later outcomes in patients with depression.9 The researchers combined the individual patient data from 30 randomized trials, with 2,184 patients receiving placebo and 6,058 receiving active therapy. After six weeks of treatment, about 50% of patients in the active treatment group responded to treatment, with 32% achieving remission of symptoms. Response was defined as at least a 50% reduction in the Hamilton Rating Scale for Depression score, and remission was defined as a score of 7 points or less. By 12 weeks, the response rate was 68% in the active treatment group, with 49% achieving remission. Patients with improvement at two weeks were more likely to respond by six weeks, whereas among patients without early improvement, 33% responded by six weeks and 43% by 12 weeks. The absence of an early response does not preclude later response; therefore, physicians should not be too quick to change antidepressant medications.
Cardiovascular
Cardiovascular medicine POEMs are summarized in Table 3.10–14 The first two POEMs in this group address statin use. Many physicians and laboratory staff continue to insist that patients be fasting for lipid profile testing. The first POEM compared fasting and nonfasting lipid profiles in the same patients four weeks apart.10 There was little difference between fasting and nonfasting measurements of low-density and high-density lipoprotein cholesterol levels and only a small increase in triglyceride levels (25 mg per dL [0.28 mmol per L]) with nonfasting measurements. Most importantly, the association between lipid levels and subsequent cardiovascular events was identical for fasting and nonfasting lipid measurements. Guidelines support nonfasting lipid measurements.15,16 It is time to simplify our patients' lives and educate local laboratory staff, who often turn away patients who disclose that they are not fasting.
TABLE 3. Cardiovascular

| Clinical question | Bottom-line answer |
|---|---|
| 6. Are fasting lipid levels more predictive of cardiovascular outcomes than nonfasting lipid levels?10 | Do not require patients to fast for lipid level measurements. Guidelines recommend checking lipid levels in nonfasting patients. This is easier on patients, and the study found that nonfasting and fasting levels are equally predictive of subsequent cardiovascular events. Although triglyceride levels may be slightly higher in nonfasting patients, cholesterol levels are similar in both groups. |
| 7. Are statins effective in patients older than 75 years?11 | In patients older than 75 years without cardiovascular disease, statins are not effective for primary prevention. Statins are effective in preventing major coronary events in patients older than 75 years, but this effect is significant only in those with established cardiovascular disease. This is consistent with results from the ALLHAT trial, which also showed no benefit for primary prevention and additionally showed a trend toward harm in those older than 75 years. |
| 8. Does low-dose aspirin prevent cardiovascular events and cardiovascular-related death in otherwise healthy older people?12 | Do not use low-dose aspirin for cardiovascular primary prevention in otherwise healthy older adults. Low-dose aspirin does not reduce the likelihood that these patients will experience a major cardiovascular event during nearly five years of follow-up. |
| 9. Does aspirin improve disability-free survival in otherwise healthy older people?13 | Do not use aspirin for noncardiovascular primary prevention in otherwise healthy older adults. In this landmark study of a contemporary population, in which risk factors such as hyperlipidemia and hypertension are more likely to be addressed, aspirin did not provide a benefit in terms of death, dementia, or disability in a largely white group of older patients. |
| 10. What are the benefits and harms of low-dose aspirin in adults with diabetes mellitus?14 | The benefits and harms of low-dose aspirin in adults with diabetes are mixed. The 7,740 patients taking low-dose aspirin experienced 51 fewer of the composite outcome of cardiovascular death, nonfatal myocardial infarction, or nonfatal ischemic stroke; and trends toward 29 fewer transient ischemic attacks and 44 fewer revascularizations than patients taking placebo over a mean of 7.4 years. This is balanced by an additional 69 major bleeding episodes in patients taking aspirin during that period, with no effect on cardiovascular-related or all-cause deaths and no difference in the incidence of cancer. |
ALLHAT = Antihypertensive and Lipid-Lowering Treatment to Prevent Heart Attack Trial.
In the next POEM, data were pooled from 28 randomized trials of statins with more than 186,000 total patients.11 This report focused on the 14,000 patients who were 75 years or older; the median follow-up was five years. There was only a small reduction in the composite outcome of MI and cardiovascular death among all patients (2.6% with statins vs. 3.0% with placebo; number needed to treat = 250 per year); the benefit was significant only in patients with preexisting cardiovascular disease. Statins had no effect on revascularization, stroke, cancer incidence, or cancer mortality.
This was a big year for aspirin studies. The next three POEMs, from two separate trials, examine the benefits and harms of aspirin therapy for primary prevention in contemporary populations. Prior studies that found a net benefit of aspirin for the primary prevention of cardiovascular disease and cancer (mostly colorectal) all recruited patients before 2002. In more recent years, fewer patients smoke or have uncontrolled hypertension, more are taking a statin, and we have widespread colorectal cancer screening. In this context, does aspirin still have a role?
Two aspirin POEMs were from the ASPREE (Aspirin in Reducing Events in the Elderly) trial, which included 19,114 adults 70 years and older in the United States and Australia (65 and older if black or Hispanic). Patients without known cardiovascular disease were randomized to aspirin, 100 mg, or placebo and were followed for a median of 4.7 years. The first POEM found no significant reduction in the likelihood of cardiovascular disease with aspirin, including fatal cardiovascular disease, fatal or nonfatal MI, and fatal or nonfatal ischemic stroke. However, they found a significant increase in major hemorrhages with aspirin.12 The second POEM from the ASPREE trial found no difference between groups for disability-free survival, defined as a composite of death, dementia, or persistent physical disability.13 A separate report from the ASPREE investigators (not one of the top 20 POEMs) found an increase in all-cause mortality with aspirin, primarily due to a significant increase in cancer-specific mortality (3.1% vs. 2.3%).
The third aspirin POEM was from the ASCEND (A Study of Cardiovascular Events in Diabetes) trial and included 15,480 adults 40 years and older with diabetes mellitus but no known cardiovascular disease. The patients were randomized to aspirin, 100 mg, or placebo and were followed for a median of 7.4 years.14 There was a reduction in the composite of nonfatal MI, nonfatal stroke, or cardiovascular death with aspirin, but a corresponding increase in major hemorrhage with no effect on cardiovascular or all-cause mortality.
What do we tell our patients? A recent meta-analysis compared trials of aspirin therapy that recruited patients from 1978 to 2002 with four large trials that recruited patients since 2005.17 The newer studies showed fewer cardiovascular benefits and no reduction in cancer incidence or mortality with aspirin as primary prevention. Based on a meta-analysis of the four most recent studies with a total of 61,604 patients, for every 1,200 patients taking aspirin instead of placebo for five years, there would be four fewer major cardiovascular events and three fewer ischemic strokes but eight more major hemorrhages, including three more intracranial hemorrhages. This study agrees with recent European guidelines that no longer recommend aspirin for primary prevention.18 The 2016 U.S. Preventive Services Task Force (USPSTF) and 2019 American College of Cardiology guidelines recommend consideration of aspirin for primary prevention only in selected patients at high cardiovascular risk and low bleeding risk.19,20 The USPSTF recommendation is currently being updated.21
Cancer Screening
The three POEMs on cancer screening (Table 4) address colorectal cancer.22–24 Fecal immunochemical testing (FIT) is the recommended method for colorectal cancer screening in most countries that have screening programs and is the subject of the first two POEMs in this group. The first POEM is an Italian study that reported the diagnostic yield of five rounds of biennial FIT in persons 50 to 69 years of age submitting a single specimen.22 The highest rates of detection occurred in the first round, as prevalent cancers were detected, and declined and then stabilized in later rounds. Over the 10-year study, about 25% of men and 18% of women had a positive test result requiring a follow-up colonoscopy. The cumulative rate was 6% for advanced adenoma and 0.85% for colorectal cancer, which are similar to findings in studies of colonoscopy in Italy and the United States.25,26 These results mean we can have confidence in FIT as a screening test while we wait for the results of ongoing randomized trials of FIT vs. colonoscopy-based screening.
TABLE 4. Cancer Screening

| Clinical question | Bottom-line answer |
|---|---|
| 11. What is the yield of a screening program based on FIT every two years for 10 years?22 | For colorectal cancer screening, FIT compares favorably with colonoscopy. Over 10 years, the detection rates for colorectal cancer and advanced adenomas using FIT are similar to those seen in studies of screening colonoscopy. This is reassuring, but it does not prove that FIT reduces morbidity and mortality due to colorectal cancer as effectively as colonoscopy. Modeling concludes that a FIT-based screening program will result in one-half as many colonoscopies as a colonoscopy-based program, as well as a significant reduction in cost, burden, and harm of screening. |
| 12. Is modern FIT for occult blood in the stool less accurate in patients who are taking aspirin, an anticoagulant, or a nonsteroidal anti-inflammatory drug?23 | Aspirin, oral anticoagulants, and nonsteroidal anti-inflammatory drugs do not interfere with FIT. The use of these drugs has no clinically important effects on the positive predictive value of FIT in a screening population. |
| 13. What is the risk of colorectal cancer in family members of patients with colorectal cancer?24 | A family history of colorectal cancer increases personal risk. People with one first-degree relative (parent, sibling, or half sibling) or two second-degree relatives with colorectal cancer are at increased risk of developing the cancer over their lifetime when compared with the general population (6% vs. 4%). Having two or more siblings or a parent and sibling with colorectal cancer increases the risk to 9%. |
FIT = fecal immunochemical testing.
The second POEM about FIT was a meta-analysis evaluating the impact of aspirin, nonsteroidal anti-inflammatory drugs, and anticoagulants on the positive predictive value of the test.23 It could theoretically go in either direction, increasing false positives by making noncancerous lesions more likely to bleed or increasing true positives by making cancers and adenomas more likely to bleed. The researchers found that the use of any of these medications had almost no effect on the positive predictive value, which was approximately 6% for colorectal cancer and 40% for advanced neoplasia. FIT requires only a single specimen and no dietary preparation, and now we know that patients undergoing FIT can continue to take medications that increase bleeding risk.
Finally, a study used a Swedish cancer registry with 173,796 patients to determine the impact of family history on the risk of colorectal cancer.24 The relative risk of colorectal cancer using no affected relatives as the reference was 1.2 for a single second-degree relative with a history of colorectal cancer, 1.6 for a single first-degree relative or two second-degree relatives, 2.3 for one first-degree relative and one second-degree relative, 2.5 for two first-degree relatives, and 5.4 for one first-degree and two second-degree relatives. However, a previous study found that this family history–related risk is attenuated once patients reach 55 years of age.27
Infections
POEMs on managing infections are summarized in Table 5.28–30 The first POEM is a meta-analysis of studies that recruited outpatients with acute respiratory tract infections who received chest radiography.28 The goal was to identify the best sign, symptom, or combination that allows clinicians to rule out community-acquired pneumonia (CAP). The researchers found that for patients with the combination of normal vital signs and normal lung examination findings, the likelihood of CAP is low at 0.4%. This could help reduce unnecessary chest radiography if applied consistently.
TABLE 5. Infections

| Clinical question | Bottom-line answer |
|---|---|
| 14. What signs and symptoms are most useful for excluding the diagnosis of pneumonia in community-dwelling adults with an acute respiratory infection?28 | The combination of normal vital signs and normal lung examination findings essentially rules out CAP. Community-dwelling adults who present as outpatients with symptoms of acute respiratory tract infection but normal vital signs and normal findings on a pulmonary examination have only a 0.4% likelihood of CAP. |
| 15. Can strep throat in children and adults be treated with five days of oral penicillin V?29 | A five-day course of treatment for streptococcal pharyngitis (strep throat) relieves symptoms as well as a 10-day course. Five days of penicillin V, 800 mg four times per day, was not inferior to 10 days of penicillin V, 1,000 mg three times per day, with shorter symptom duration. This is not the first study to show similar benefits with a shorter duration of oral amoxicillin/clavulanate (Augmentin), amoxicillin, or a cephalosporin. |
| 16. How long do colds last in children?30 | Cold symptoms can last up to three weeks. Most respiratory illnesses in children are mild, do not require medical care, and do not result in school absences; however, symptoms can last up to three weeks. |
CAP = community-acquired pneumonia.
The second POEM in this group was selected as one of the top three research studies out of more than 400 presented at the 2019 North American Primary Care Research Group meeting.29 This Swedish study included 422 adults and children presenting to a primary care physician with moderately severe streptococcal pharyngitis (strep throat). Patients were randomized to penicillin V at a dosage of 800 mg four times a day for five days or 1,000 mg three times a day for 10 days. Those receiving the higher dose over a shorter course of treatment had similar cure rates as those receiving longer-duration therapy, with quicker symptom resolution and no increase in recurrence. Many other studies have found similar results with antibiotics for a range of infections.
An accurate prognosis can potentially help patients avoid unnecessary antibiotic use and return visits. The third POEM in this group recruited 485 healthy children in the United Kingdom, and parents were instructed to contact the researchers every time the child had a respiratory tract infection.30 One-half of the children had at least one infection, with a median duration of nine days; 90% recovered by day 23. Lower respiratory tract infections were associated with a longer duration of symptoms and ear infections were associated with a shorter duration. This reinforces that clinicians should counsel parents of children with lower respiratory tract symptoms to be patient.
Miscellaneous
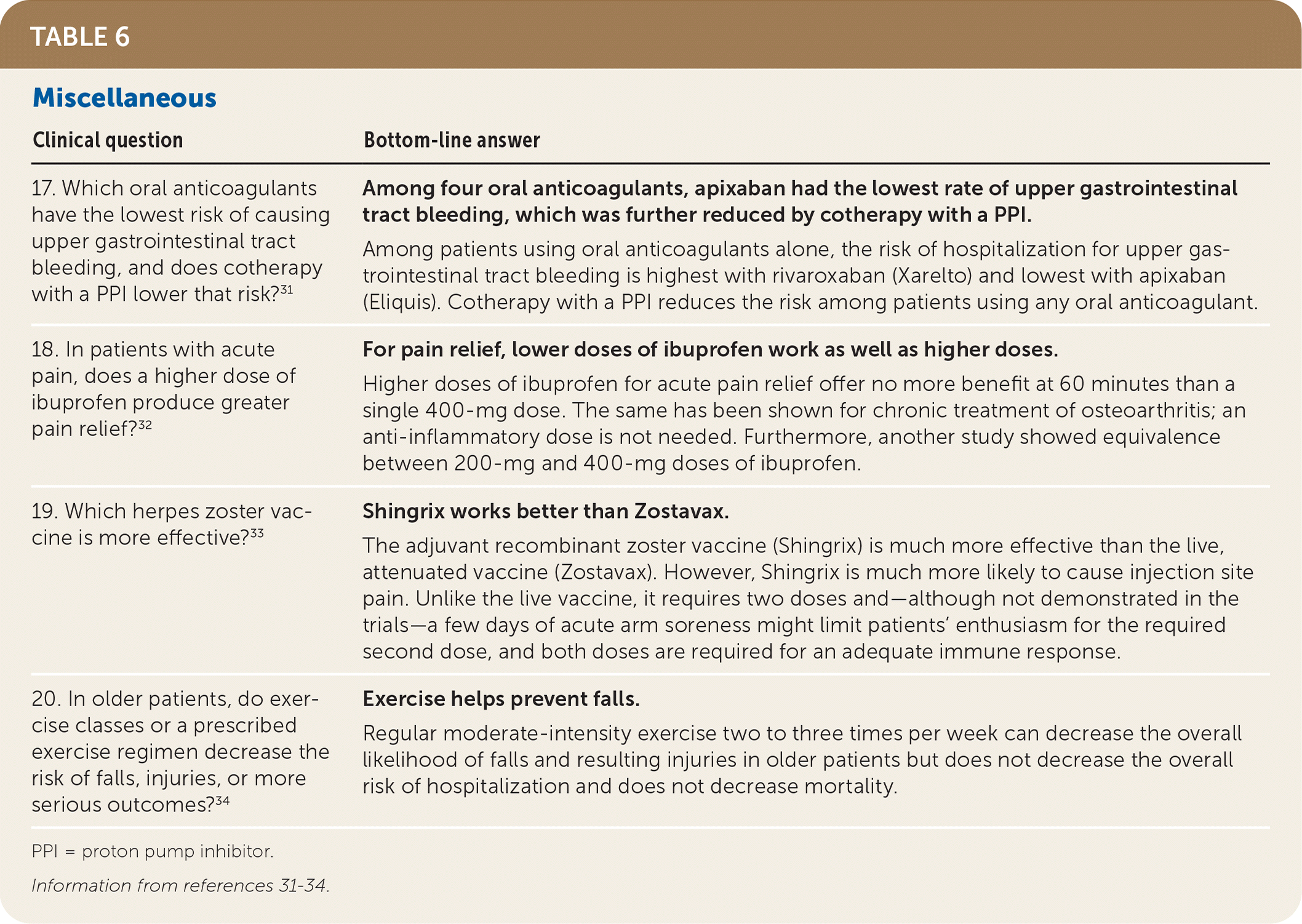
Four additional POEMs are summarized in Table 6.31–34 The first is a cohort study of more than 1.6 million Medicare beneficiaries who started an anticoagulant between 2011 and 2015.31 Bleeding rates were compared, adjusting for available covariates using propensity score matching (i.e., matching patients who were similar other than choice of anticoagulant). The adjusted incidence of hospitalization for upper gastrointestinal tract bleeding was significantly higher in those who received rivaroxaban (Xarelto) compared with those who received dabigatran (Pradaxa), warfarin (Coumadin), or apixaban (Eliquis); 144 per 10,000 person-years vs. 120, 113, and 73, respectively). For all agents combined, adding a proton pump inhibitor significantly reduced bleeding risk (76 out of 10,000 per year vs. 115 out of 10,000 per year; number needed to treat = 256), although rivaroxaban still had the highest bleeding rate.
TABLE 6. Miscellaneous
| Clinical question | Bottom-line answer |
|---|---|
| 17. Which oral anticoagulants have the lowest risk of causing upper gastrointestinal tract bleeding, and does cotherapy with a PPI lower that risk?31 | Among four oral anticoagulants, apixaban had the lowest rate of upper gastrointestinal tract bleeding, which was further reduced by cotherapy with a PPI. Among patients using oral anticoagulants alone, the risk of hospitalization for upper gastrointestinal tract bleeding is highest with rivaroxaban (Xarelto) and lowest with apixaban (Eliquis). Cotherapy with a PPI reduces the risk among patients using any oral anticoagulant. |
| 18. In patients with acute pain, does a higher dose of ibuprofen produce greater pain relief?32 | For pain relief, lower doses of ibuprofen work as well as higher doses. Higher doses of ibuprofen for acute pain relief offer no more benefit at 60 minutes than a single 400-mg dose. The same has been shown for chronic treatment of osteoarthritis; an anti-inflammatory dose is not needed. Furthermore, another study showed equivalence between 200-mg and 400-mg doses of ibuprofen. |
| 19. Which herpes zoster vaccine is more effective?33 | Shingrix works better than Zostavax. The adjuvant recombinant zoster vaccine (Shingrix) is much more effective than the live, attenuated vaccine (Zostavax). However, Shingrix is much more likely to cause injection site pain. Unlike the live vaccine, it requires two doses and—although not demonstrated in the trials—a few days of acute arm soreness might limit patients' enthusiasm for the required second dose, and both doses are required for an adequate immune response. |
| 20. In older patients, do exercise classes or a prescribed exercise regimen decrease the risk of falls, injuries, or more serious outcomes?34 | Exercise helps prevent falls. Regular moderate-intensity exercise two to three times per week can decrease the overall likelihood of falls and resulting injuries in older patients but does not decrease the overall risk of hospitalization and does not decrease mortality. |
PPI = proton pump inhibitor.
The next POEM identified 225 adults presenting to the emergency department with acute pain (mostly musculoskeletal); the average pain score was 6 to 7 out of 10.32 They were then randomized to a single dose of 400-mg, 600-mg, or 800-mg ibuprofen. An hour after taking the medication, there was no difference between groups, which all had pain scores between 4.4 and 4.5.
The third POEM in this group is a meta-analysis of studies comparing two doses of the recombinant zoster vaccine (Shingrix) with one dose of the live, attenuated vaccine (Zostavax) for the prevention of shingles.33 Shingrix was more effective but caused more systemic adverse events, although mild, and more injection site pain.
Finally, a systematic review identified 46 studies of the impact of exercise on fall risk in patients 59 years or older.34 Most of the programs used moderate-intensity exercise, with about one hour of exercise three times per week. The researchers found that exercise significantly decreased the overall risk of falls and resulting injuries but did not affect the risk of multiple falls, hospitalization, or mortality. Fractures were less likely in the exercise group but not significantly.
Practice Guidelines
POEMs sometimes summarize high-impact practice guidelines from important organizations. Key messages from the three highest-rated guidelines are summarized in Table 7.35–37
TABLE 7. Practice Guidelines

| Organization/topic | Key recommendations |
|---|---|
| AACP: antithrombotic therapy for atrial fibrillation35 | Use risk scores when deciding on therapy to prevent stroke; direct oral anticoagulants are generally preferred over warfarin or aspirin with or without clopidogrel. Use the CHA2DS2 -VASc score to assess the risk of stroke. Men with a score of 0 and women with a score of 1 are at low risk of stroke and do not require anticoagulation. Direct oral anticoagulants are the preferred agents for most patients with newly diagnosed atrial fibrillation, although this decision should be individualized. Do not use aspirin or aspirin plus clopidogrel (Plavix) for antithrombotic prophylaxis for atrial fibrillation. Use the HAS-BLED score to assess bleeding risk; if the score is 3 or higher, look for ways to reduce risk, educate the patient about what to watch for regarding bleeding, and consider following up more closely. For patients currently taking warfarin (Coumadin), consider switching to a direct oral anticoagulant if they are in the international normalized ratio range less than 65% of the time. If patients are also taking aspirin, first make sure they really need it, then use a low dose (75 to 100 mg) and treat with a concomitant proton pump inhibitor. |
| ADA/EASD: type 2 diabetes mellitus36 | Empower patients to manage their diabetes; metformin is first-line therapy, and second-line therapies include GLP-1 receptor antagonists or SGLT-2 inhibitors. These expert consensus recommendations attempt to shift responsibility and decision-making to where it belongs—with the patients. The recommendations suggest making self-management education and support a cornerstone of treatment. Another pillar of this new approach is selecting medication treatment according to which one is most likely to be taken regularly and over time by a particular patient. The third pillar continues to be metformin. If additional control is needed, adding one or more oral hypoglycemics to the metformin regimen is recommended. For patients with known heart disease, additional treatment with a GLP-1 receptor antagonist such as liraglutide (Victoza) or an SGLT-2 inhibitor such as empagliflozin (Jardiance) is recommended. Sulfonylureas and glitazones (also called thiazolidinediones) are less expensive options. |
| ACP: breast cancer screening37 | Use shared decision-making for women 40 to 49 years of age, screen every two years in women 50 to 74 years of age, and stop screening at 75 years of age or when life expectancy is less than 10 years; do not use clinical breast examinations for screening. Citing that the harms of screening (false-positive results, benign biopsies, and overdiagnosis) outweigh the benefits of early diagnosis, the guideline does not recommend routine screening of women 40 to 49 years of age. Instead, physicians should have a discussion with these patients about the benefits and harms of screening. Women 50 to 74 years of age should be offered screening every two years, stopping when life expectancy is less than 10 years. Patients 75 years or older should not be screened. Clinical breast examinations should no longer be used for screening in women who undergo routine mammography. |
AACP = American College of Chest Physicians; ACP = American College of Physicians; ADA = American Diabetes Association; CHA2DS2-VASc = congestive heart failure; hypertension; age 75 years or older [doubled]; diabetes mellitus; prior stroke, transient ischemic attack, or thromboembolism [doubled]; vascular disease; EASD = European Association for the Study of Diabetes; GLP-1 = glucagon-like peptide 1; HAS-BLED = hypertension, abnormal renal function and liver function, stroke, bleeding, labile international normalized ratio, elderly [older than 65 years], drugs and alcohol; SGLT-2 = sodium-glucose cotransporter 2.
The American College of Chest Physicians recommends initiating direct oral anticoagulant therapy in patients with newly diagnosed atrial fibrillation, avoiding aspirin or aspirin plus clopidogrel (Plavix) to prevent thromboembolism, using risk scores for stroke and bleeding, and avoiding cotreatment with aspirin and an anticoagulant if possible.35
The American Diabetes Association/European Association for the Study of Diabetes guideline for type 2 diabetes mellitus continues to recommend educating patients about diabetes self-management and providing support as the cornerstone of therapy, and metformin as the preferred initial therapy.36 If a second agent is needed, there are many options, although glucagon-like peptide 1 receptor antagonists or sodium-glucose cotransporter 2 inhibitors are recommended for patients with established heart disease; sodium-glucose cotransporter 2 inhibitors are preferred for patients with heart failure or chronic kidney disease.
The American College of Physicians recommendations for breast cancer screening generally parallel those of the USPSTF, which are supported by the American Academy of Family Physicians. Recommendations include shared decision-making in women 40 to 49 years of age, biennial mammography from 50 to 74 years of age or until the woman's life expectancy is less than 10 years, and eliminating the clinical breast examination as a screening test for women who undergo regular mammography.37–39
The full text of the POEMs discussed in this article is available at https://www.aafp.org/journals/afp/content/top-poems/2019.html.
A list of top POEMs from previous years is available at https://www.aafp.org/afp/toppoems.
Editor's Note: This article was cowritten by Dr. Mark Ebell, who is deputy editor for evidence-based medicine for AFP and cofounder and editor-in-chief of Essential Evidence Plus, published by Wiley-Blackwell, Inc. Because of Dr. Ebell's dual roles and ties to Essential Evidence Plus, the concept for this article was independently reviewed and approved by a group of AFP's medical editors. In addition, the article underwent peer review and editing by three of AFP's medical editors. Dr. Ebell was not involved in the editorial decision-making process.—Sumi Sexton, MD, Editor-in-Chief.
The authors thank Wiley-Blackwell, Inc., for giving permission to excerpt the POEMs; Drs. Allen Shaughnessy, Henry Barry, David Slawson, Nita Kulkarni, and Linda Speer for their work in selecting and writing the original POEMs; the academic family medicine fellows and faculty of the University of Missouri–Columbia for their work as peer reviewers; Pierre Pluye, PhD, for his work in codeveloping the Information Assessment Method; and Maria Vlasak for her assistance with copyediting the POEMs for the past 26 years.

