Am Fam Physician. 2020;102(5):272-273
Author disclosure: No relevant financial affiliations.
Clinical Question
Are corticosteroids safe and effective at reducing rates of mortality and clinical failure (i.e., death, worsening of imaging studies, or no clinical improvement) in adults and children hospitalized with community-acquired pneumonia (CAP)?
Evidence-Based Answer
For adults hospitalized with severe CAP, the use of corticosteroids may reduce the likelihood of mortality. (Strength of Recommendation [SOR]: B, based on inconsistent or limited-quality patient-oriented evidence.) For adults and children hospitalized with CAP, the use of corticosteroids may reduce the likelihood of early clinical failure. The risk of hyperglycemia is transient and of limited clinical significance.1 (SOR: A, based on consistent, good-quality patient-oriented evidence.)
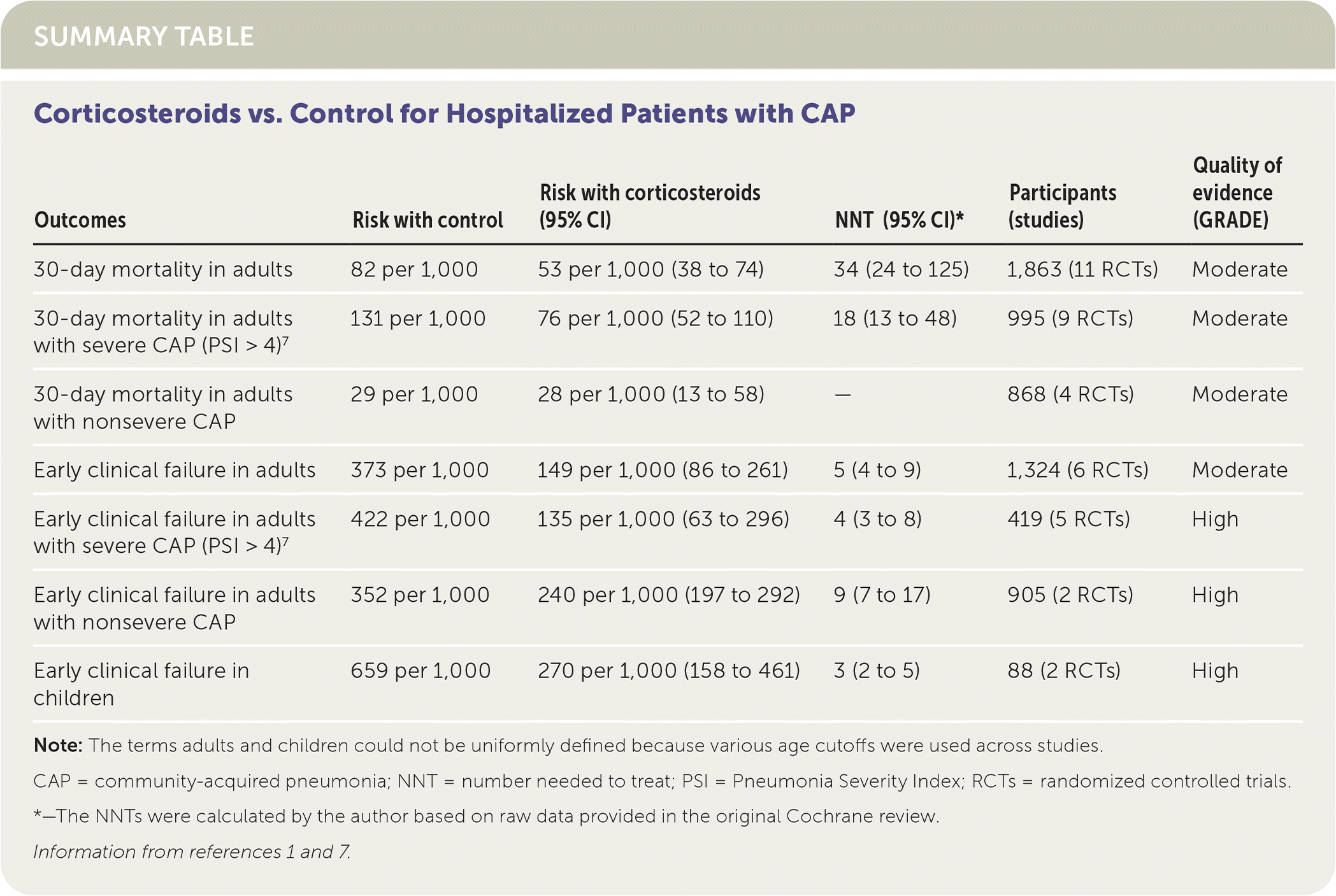
| Outcomes | Risk with control | Risk with corticosteroids (95% CI) | NNT (95% CI)* | Participants (studies) | Quality of evidence (GRADE) |
|---|---|---|---|---|---|
| 30-day mortality in adults | 82 per 1,000 | 53 per 1,000 (38 to 74) | 34 (24 to 125) | 1,863 (11 RCTs) | Moderate |
| 30-day mortality in adults with severe CAP (PSI > 4)7 | 131 per 1,000 | 76 per 1,000 (52 to 110) | 18 (13 to 48) | 995 (9 RCTs) | Moderate |
| 30-day mortality in adults with nonsevere CAP | 29 per 1,000 | 28 per 1,000 (13 to 58) | — | 868 (4 RCTs) | Moderate |
| Early clinical failure in adults | 373 per 1,000 | 149 per 1,000 (86 to 261) | 5 (4 to 9) | 1,324 (6 RCTs) | Moderate |
| Early clinical failure in adults with severe CAP (PSI > 4)7 | 422 per 1,000 | 135 per 1,000 (63 to 296) | 4 (3 to 8) | 419 (5 RCTs) | High |
| Early clinical failure in adults with nonsevere CAP | 352 per 1,000 | 240 per 1,000 (197 to 292) | 9 (7 to 17) | 905 (2 RCTs) | High |
| Early clinical failure in children | 659 per 1,000 | 270 per 1,000 (158 to 461) | 3 (2 to 5) | 88 (2 RCTs) | High |
Practice Pointers
CAP is a significant cause of morbidity and mortality in the United States. There were 257,000 emergency department visits because of CAP in 2016 and 49,157 deaths (approximately 15.1 per 100,000 people) from CAP in 2017.2,3 The authors of a previous Cochrane review found that “in most patients with pneumonia, corticosteroids are generally beneficial for accelerating the time to resolution of symptoms,”4 but the evidence was not deemed strong enough to make firm recommendations. Subsequently, a 2015 systematic review found that corticosteroids for adults hospitalized with CAP might reduce mortality, use of mechanical ventilation, and length of hospital stay.5 However, the most recent guidelines from the American Thoracic Society (ATS) and the Infectious Diseases Society of America (IDSA) do not recommend using corticosteroids for adults with nonsevere or severe CAP, and they endorse the use of corticosteroids only for patients with CAP and refractory septic shock.6
The authors of this review incorporated 17 randomized controlled trials (RCTs) with a total of 2,264 patients: 15 RCTs including 1,954 adults (mean age = 69.8 years) and two RCTs including 310 children (mean age = 5.6 years).1 Although the authors searched broadly for studies examining all severities of pneumonia and all treatment settings, the only studies that met inclusion criteria were RCTs of corticosteroids used in the inpatient treatment of CAP. The included trials were conducted in Europe (eight studies), the Middle East (three studies), China (two studies), Japan (two studies), South Africa (one study), and Australia (one study). Thirteen of the 17 studies began in 2000 or later. For the main outcomes reported in the Cochrane review, the findings were generally consistent across the studies.
Definitions of pneumonia severity varied across studies, but for this review the authors defined severe CAP as a Pneumonia Severity Index (PSI) score of more than 4.7 There was variation among trials in corticosteroid duration (one to 10 days) and dosing, but most trials in adults used intravenous corticosteroid dosages equivalent to 40 to 50 mg of prednisone per day for five to 10 days, whereas the trials in children used varied doses of prednisolone, methylprednisolone, or dexamethasone. The studies in this review were assessed as being at low risk of attrition bias; low or unclear risk of selection bias; low, unclear, or high risk of performance and detection bias; and overall high risk of reporting bias.
The reviewers found moderate-quality evidence that prescribing corticosteroids to 18 patients would prevent one death (with mortality measured within 30 days of randomization) and high-quality evidence that prescribing corticosteroids to four patients would prevent one episode of early clinical failure (e.g., death from any cause, radiographic progression, clinical instability at day 5 to 8). For adults with nonsevere CAP, the estimates of effect size for preventing mortality by treating with corticosteroids were too broad to allow for any firm conclusion of risk or benefit, but there was high-quality evidence that treating nine patients with corticosteroids would prevent one episode of early clinical failure. Hyperglycemia was more common with corticosteroid treatment, but no differences were noted between groups in rates of gastrointestinal bleeding, neuropsychiatric events, or adverse cardiac events.
The two studies of treatment in children did not report any deaths, but high-quality evidence showed that using corticosteroids to treat three children with CAP would prevent one episode of early clinical failure. The two studies also reported no adverse events, and one trial reported that there were no cases of hyperglycemia.
The previous Cochrane review addressing corticosteroid treatment for CAP found insufficient evidence to support clinical recommendations,4 but subsequent meta-analyses have demonstrated improvements in morbidity8–10 and mortality5 when adjunctive corticosteroids are used in hospitalized patients with CAP. The recent ATS/IDSA guidelines6 were published after this Cochrane review, focus only on adults, and cite the four previous meta-analyses5,8–10; however, they do not address the findings of this review. The ATS/IDSA guidelines do not support routine use of corticosteroids in adults with severe or nonsevere CAP, but they call for further research in this area.6
The practice recommendations in this activity are available at http://www.cochrane.org/CD007720.
Editor's Note: This review was completed prior to the onset of the coronavirus disease 2019 (COVID-19) pandemic and thus should not be seen as evidence that corticosteroids have a role in the treatment of COVID-19 pneumonia.