A healthy 10-year-old patient presented with a pruritic rash that developed when the palms were exposed to water and resolved when the hands were dried. The symptoms began about two years earlier. The patient had no significant personal or family history or allergies. The patient was born outside of the United States and had not received conventional newborn screening.
Physical examination initially showed no abnormalities. After the hands were exposed to tap water for 30 seconds, multiple flat, white lesions developed on both palms (Figure 1). There was no erythema.
FIGURE 1
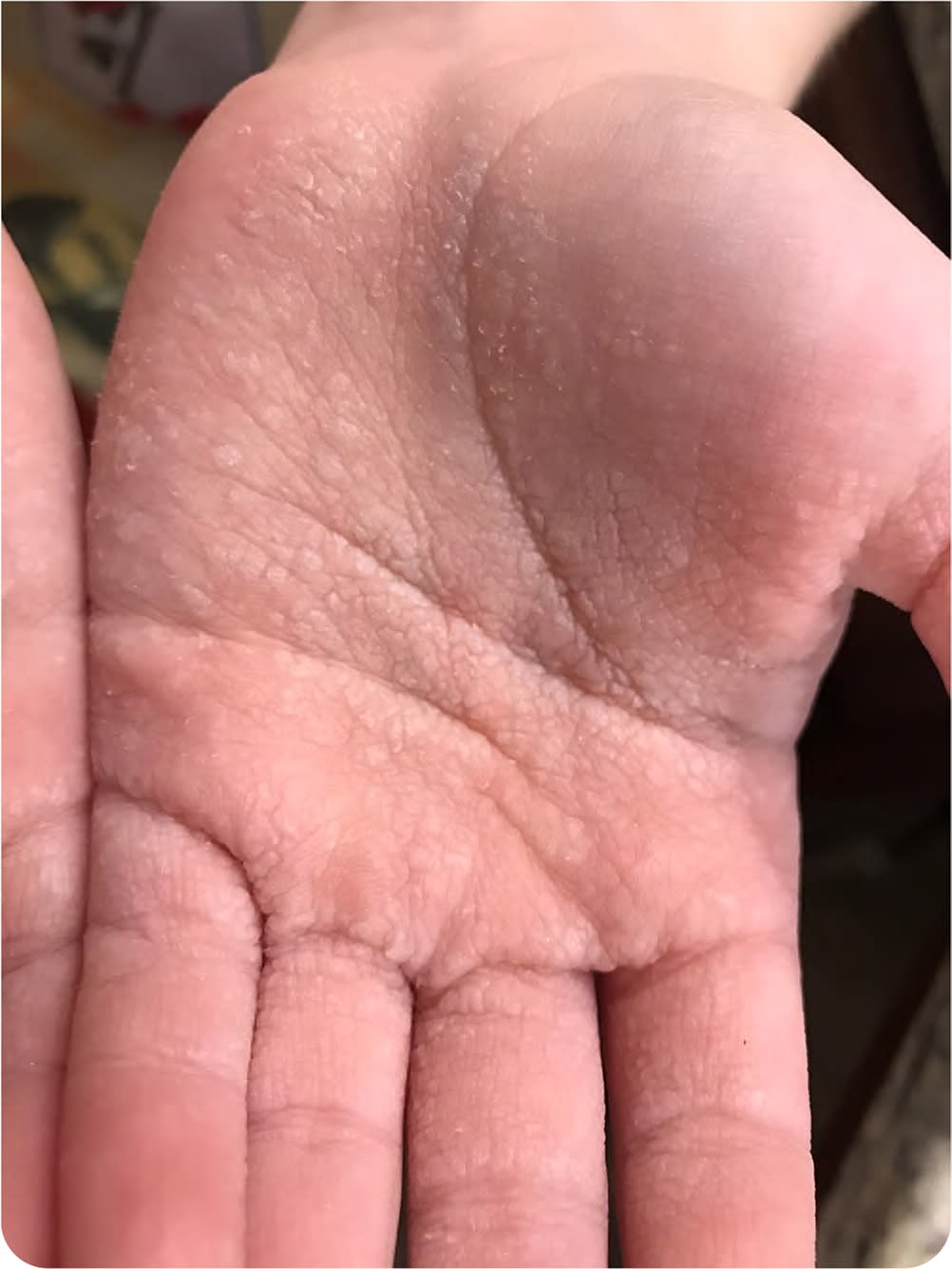
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
- A. Aquagenic palmoplantar keratoderma.
- B. Bothnian palmoplantar keratoderma.
- C. Aquagenic urticaria.
- D. Pityriasis versicolor.
- E. Primary hyperhidrosis.
Discussion
The answer is A: aquagenic palmoplantar keratoderma, also known as aquagenic wrinkling of the palms. It can be acquired or genetic and causes thickened skin and white or translucent lesions on the palms after water exposure. These changes can be accompanied by pruritus or a burning sensation. The condition is most common on the palms but rarely involves plantar surfaces. Other areas are spared. Symptoms resolve soon after drying.1,2
The pathogenesis of aquagenic palmoplantar keratoderma is unclear; increased epidermal salt concentrations may play a role because of an association with cystic fibrosis, infantile marasmus, and nonsteroidal anti-inflammatory drug (NSAID) use.2 Aquagenic palmoplantar keratoderma occurs in up to 84% of patients with cystic fibrosis and 25% of cystic fibrosis carriers.3 Autosomal recessive patterns have been described. This condition is more common in women.2
Palmoplantar keratodermas are a heterogeneous group of disorders that cause hyperkeratosis on the palms and soles. Patients with these conditions may also have nail changes, overlying fungal infections, hyperhidrosis, and severe pain. These disorders can be acquired (genetic predisposition, drug-induced, or associated with malignancy) or present at birth. They can be isolated or part of another multisystem syndrome. The heterogeneous nature of the disorders makes diagnosis difficult, and biopsy may be required.4 Although aquagenic palmoplantar keratoderma is sometimes labeled as a palmoplantar keratoderma, some argue that it should be categorized differently based on pathogenesis because aquagenic palmoplantar keratoderma involves abnormal skin electrolytes, whereas palmoplantar keratodermas involve hyperkeratosis.2
There is no cure for aquagenic palmoplantar keratoderma, but symptoms can be treated by using an emollient before water exposure and by applying aluminum chloride 20% on the palms nightly to decrease palmar sweating.1,2,5 OnabotulinumtoxinA (Botox) injections can be used for severe symptoms.6 It is important to test patients with aquagenic palmoplantar keratoderma for cystic fibrosis, to assess their nutritional status, and to ask about NSAID use.2
Bothnian palmoplantar keratoderma is a rare palmoplantar keratoderma that presents at birth. The condition results from a missense mutation of an aquaporin that causes a decrease in transepidermal water loss leading to hyperkeratosis. Initially discovered in northern Sweden (northwest of the Gulf of Bothnia), this form of palmoplantar keratoderma causes a boggy or sponge-like appearance of the palms and soles after exposure to water.7
Aquagenic urticaria is a genetic condition that causes urticarial eruptions after water exposure.4 Lesions mainly occur on the upper extremities but can appear anywhere. They may include intensely pruritic wheals and flares.
Pityriasis versicolor (also called tinea versicolor) is a common fungal infection caused by Malassezia furfur that results in flaky lesions on the neck, trunk, abdomen, and rarely the face.8 Palms are generally spared. The lesions can be white, salmon, tan, brown, or pink and are not precipitated or exacerbated by water exposure.
Primary hyperhidrosis is a genetic condition that causes excessive sweating. It can affect any set of sweat glands, including the craniofacial, axillary, and palmar and plantar sweat glands. Primary hyperhidrosis can accompany some forms of palmoplantar keratoderma but does not cause lesions and is not affected by water exposure.5
SUMMARY TABLE
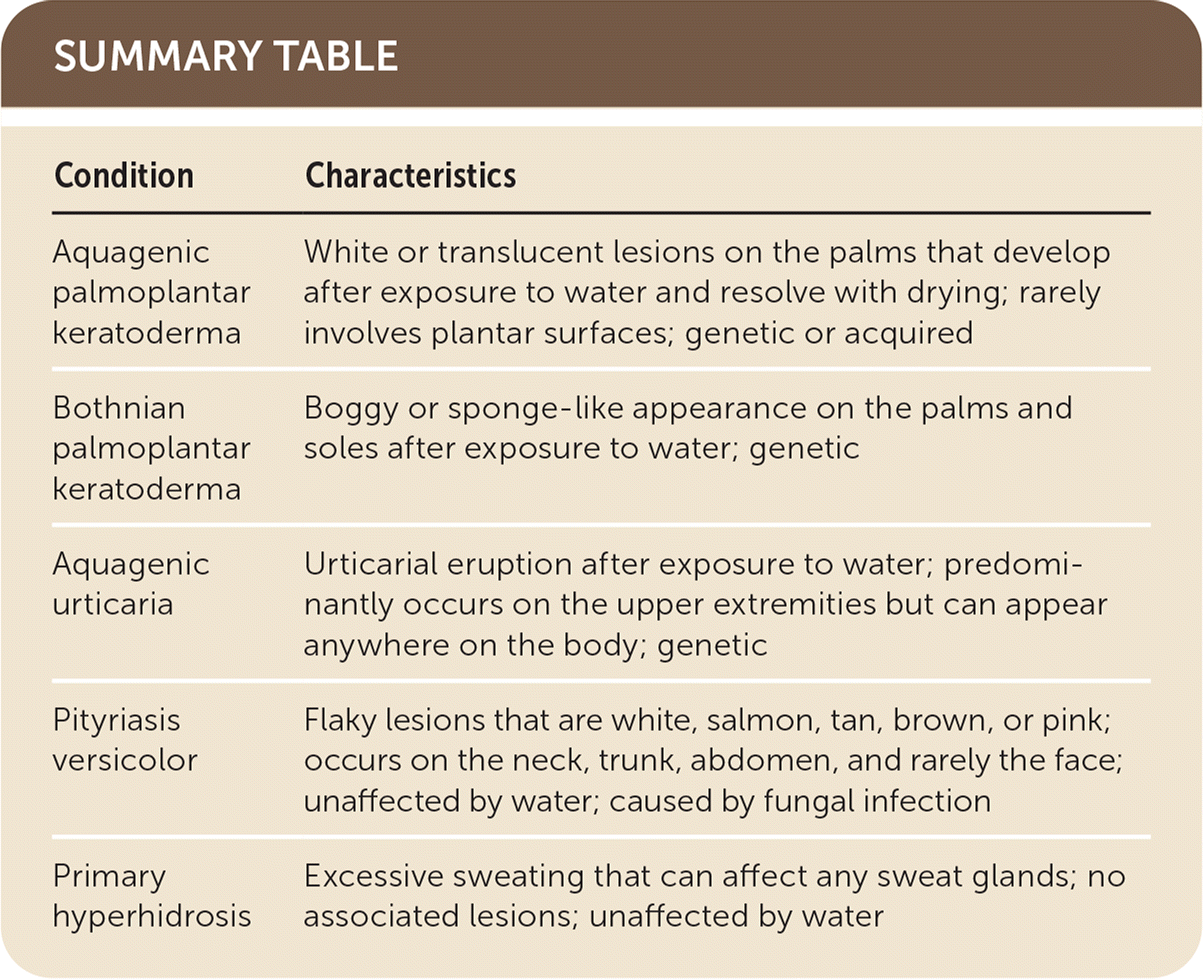
| Condition | Characteristics |
|---|---|
| Aquagenic palmoplantar keratoderma | White or translucent lesions on the palms that develop after exposure to water and resolve with drying; rarely involves plantar surfaces; genetic or acquired |
| Bothnian palmoplantar keratoderma | Boggy or sponge-like appearance on the palms and soles after exposure to water; genetic |
| Aquagenic urticaria | Urticarial eruption after exposure to water; predominantly occurs on the upper extremities but can appear anywhere on the body; genetic |
| Pityriasis versicolor | Flaky lesions that are white, salmon, tan, brown, or pink; occurs on the neck, trunk, abdomen, and rarely the face; unaffected by water; caused by fungal infection |
| Primary hyperhidrosis | Excessive sweating that can affect any sweat glands; no associated lesions; unaffected by water |
The contents of this article are solely the views of the authors and do not necessarily represent the official view of the U.S. Army, the U.S. Department of Defense, or the U.S. government.

