A healthy 34-year-old patient presented with a worsening facial rash that first appeared about two years earlier. The rash was initially painless but developed a moderately intense burning sensation with repeated flare-ups. There was no scarring or pruritus.
Two years earlier, the patient underwent a left total temporomandibular joint replacement. Bacitracin ointment was applied to the incision site postoperatively, causing an irritant contact dermatitis that was treated with topical triamcinolone. Two weeks after stopping the triamcinolone, a new perioral rash developed. This rash also cleared after a few days of triamcinolone treatment. This pattern of recurrence after discontinuation of triamcinolone continued, with each recurrence becoming more intense.
On physical examination, the patient had a normal body mass index and vital signs. Multiple clustered, erythematous papulopustules without scales were noted in the perioral area (Figure 1). The patient had no cervical lymphadenopathy or other clinical findings.
FIGURE 1
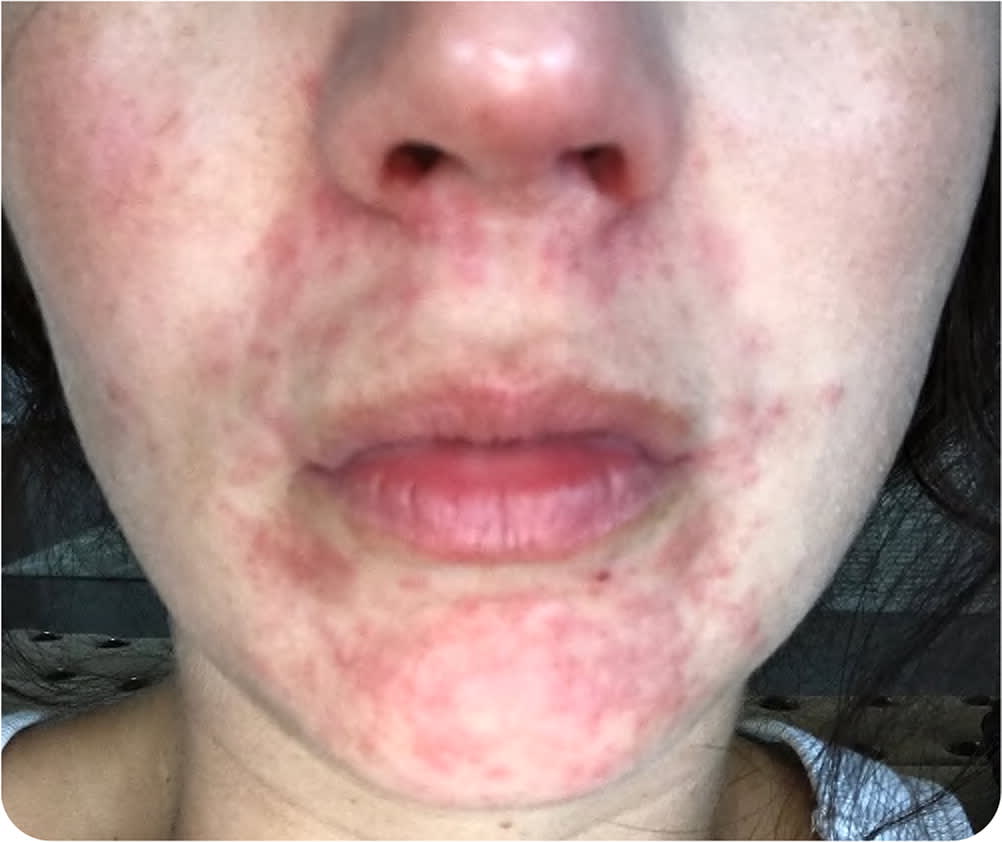
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
- A. Acne vulgaris.
- B. Allergic contact dermatitis.
- C. Impetigo.
- D. Perioral dermatitis.
- E. Rosacea.
Discussion
The answer is D: perioral dermatitis. Perioral dermatitis is a relatively common skin disorder that typically presents as small, clustered inflammatory papules around the mouth or nose. Although pathogenesis is not well understood, use of topical corticosteroids such as triamcinolone can be a contributing factor.1,2 Perioral dermatitis may be asymptomatic or associated with a mild to moderate burning sensation.3 The rash initially improves with topical corticosteroid treatment but recurs or worsens with continued use or attempts to discontinue treatment. Use of skin moisturizers, cosmetics, or fluoridated toothpaste may also be associated with perioral dermatitis.4
Perioral dermatitis is considered a self-limited condition. It may resolve spontaneously within a few months or persist for several years. Management begins with discontinuation of corticosteroids and any other irritants. The rash may be treated with topical erythromycin and metronidazole (Metrogel). Topical pimecrolimus 1% cream (Elidel) has good evidence of effectiveness but the high cost limits its use.5 For more severe disease, systemic treatment options include oral tetracyclines.6
Acne vulgaris is a common disorder in adolescents that is caused by inflammation of pilosebaceous units. It manifests as comedones and inflammatory papules or pustules, most often on the face and trunk. Nodules, cysts, and scarring can occur in more severe cases.
Allergic contact dermatitis is a type IV hypersensitivity reaction, which can be caused by contact with many substances, including soaps, cosmetics, fragrances, jewelry, and plants. Allergic contact dermatitis manifests as inflammatory papules and vesicles and often intense pruritus, typically in the area of contact.
Impetigo is a skin infection common in children that is caused by staphylococcal or streptococcal bacteria. The rash typically begins as red papules that become vesicles with honey-yellow crusting. The paranasal skin is a common site for the rash.
Rosacea presents as inflammatory papules and pustules primarily distributed on the central face, nose, and cheeks. Erythema and telangiectasias involving the cheeks often occur. Common rosacea triggers include heat, stress, alcohol, and spicy foods.
SUMMARY TABLE
| Condition | Characteristics |
|---|---|
| Acne vulgaris | Comedones and inflammatory papules or pustules, most often on the face and trunk; nodules, cysts, and scarring can occur in severe cases; common in adolescents |
| Allergic contact dermatitis | A type IV hypersensitivity reaction; inflammatory papules and vesicles; intense pruritus is common |
| Impetigo | Staphylococcal or streptococcal skin infection; red papules that become vesicles with honey-yellow crusting; common in children |
| Perioral dermatitis | Multiple small, clustered, inflammatory papules around the mouth or nose; associated with topical corticosteroid use |
| Rosacea | Inflammatory papules and pustules primarily distributed on the central face, nose, and cheeks; erythema and telangiectasias involving the cheeks; triggers include heat, stress, alcohol, and spicy foods |

