A 51-year-old patient presented with several years of diffuse pain in the right shoulder. The pain, which the patient rated as 10 out of 10 on a pain scale, was exacerbated by any activity. The patient reported shoulder stiffness and subjective weakness in the arm. The patient had no history of injury or surgery to the shoulder but had undergone bilateral hip replacements and right ankle fusion. The patient had a history of type 2 diabetes mellitus and hypertension.
On physical examination, the patient's right shoulder was diffusely tender and mildly warm. The range of motion was significantly decreased in all planes. Rotator cuff strength could not be evaluated because of pain. Results of the Hawkins and Neer impingement tests, empty can test, lift off test, and drop arm test were grossly positive. The patient could not tolerate further testing because of pain. Shoulder radiography (anteroposterior view; Figure 1) and magnetic resonance imaging (T2 frontal view; Figure 2) were performed.
FIGURE 1
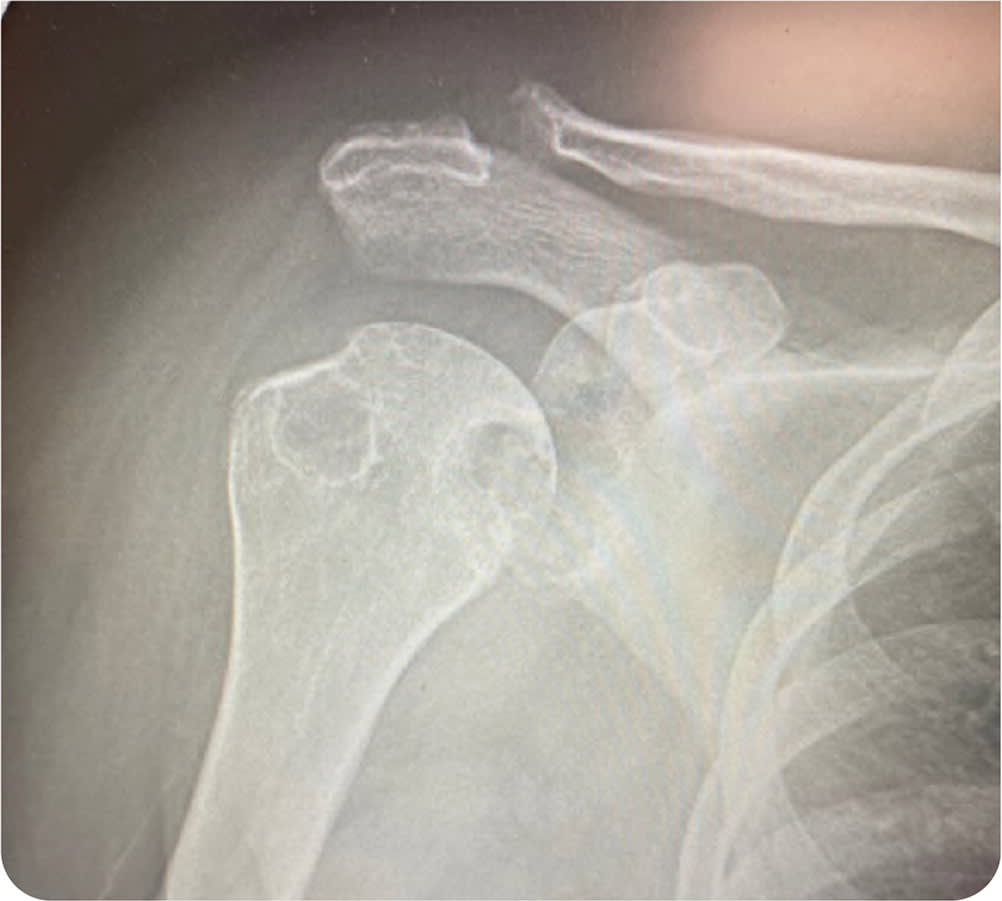
FIGURE 2
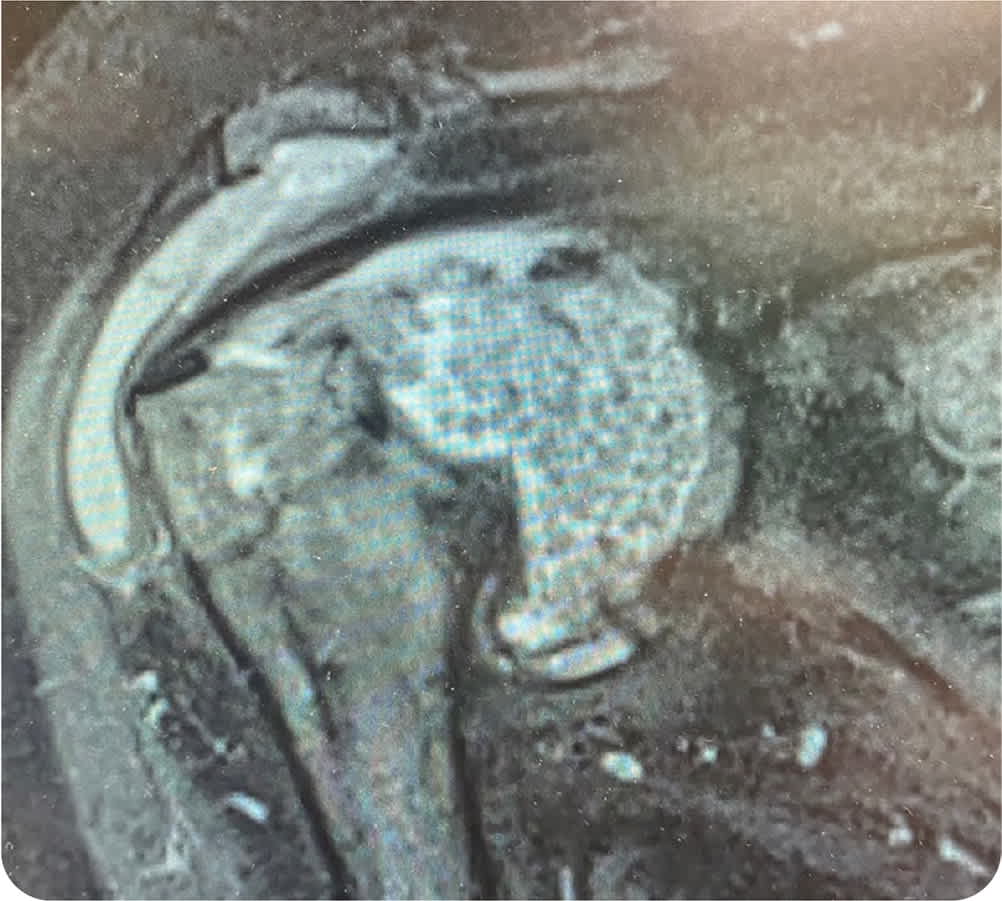
Question
Based on the patient's history, physical examination, and imaging findings, which one of the following is the most likely diagnosis?
- A. Adhesive capsulitis.
- B. Inflammatory arthritis.
- C. Rotator cuff tear.
- D. Synovial chondromatosis.
Discussion
The answer is B: inflammatory arthritis. Inflammatory arthritis encompasses multiple conditions that are categorized as autoimmune connective tissue disease (e.g., rheumatoid arthritis, systemic lupus erythematosus, vasculitis), spondyloarthritis (e.g., ankylosing spondylitis, psoriatic arthritis, reactive arthritis, inflammatory bowel disease–related arthritis), infectious arthritis (e.g., bacterial, viral), and crystal arthritis (e.g., gout, calcium pyrophosphate deposition disease).1
Large erosions on radiography and magnetic resonance imaging (MRI) can be typical findings in patients with rheumatoid arthritis, psoriatic arthritis, and gout. This patient's MRI demonstrates a large glenohumeral joint effusion that contains multiple intra-articular bodies known as rice bodies. Rice bodies are believed to be an end product of chronically inflamed synovium that infarcts and sloughs into the synovial space.2 Rice bodies can occur in several types of inflammatory arthritis.
Patients with inflammatory arthritis typically have pain and stiffness, especially in the mornings, with multiple joint involvement.1 Physical examination often reveals erythema, warmth, swelling, tenderness, and decreased passive and active range of motion in the affected joint. Appropriate laboratory testing and specialist referral should be initiated if inflammatory arthritis is suspected.
Adhesive capsulitis, also known as a frozen shoulder, is a common condition that involves contracture of the shoulder capsule.3 Rotator cuff strength is usually intact, whereas range of motion is greatly reduced, particularly in the external plane. Plain radiographs are usually unremarkable, and MRI typically shows thickening of the coracohumeral ligament and axillary recess without a joint effusion or intraarticular debris/loose bodies.
Rotator cuff pathology, including partial- and full-thickness tears, typically presents as progressive anterolateral shoulder pain that can radiate into the deltoid and is often associated with nighttime pain and weakness.4 Although no one physical examination finding is reliably diagnostic for a rotator cuff tear, combining highly sensitive tests (Hawkins, painful arc) with highly specific tests (external lag, drop arm) can improve the accuracy of the physical examination. Plain radiography is not needed for the diagnosis but may help rule out other pathology.5 MRI can accurately show partial- and full-thickness tears. In the absence of other pathology, imaging generally does not show joint effusion or debris.
Synovial chondromatosis is a rare, benign condition of uncertain etiology in which synovial tissue forms cartilaginous nodules that can break off into the joint and ossify to form loose bodies.6 It is most common in the knee but can occur in any large joint. Patients can be asymptomatic or have pain; limited range of motion; swelling; joint effusions; and mechanical symptoms, such as locking. This condition can usually be diagnosed with multifocal calcific densities in the joint on radiography. MRI or computed tomography can help confirm the diagnosis.
SUMMARY TABLE
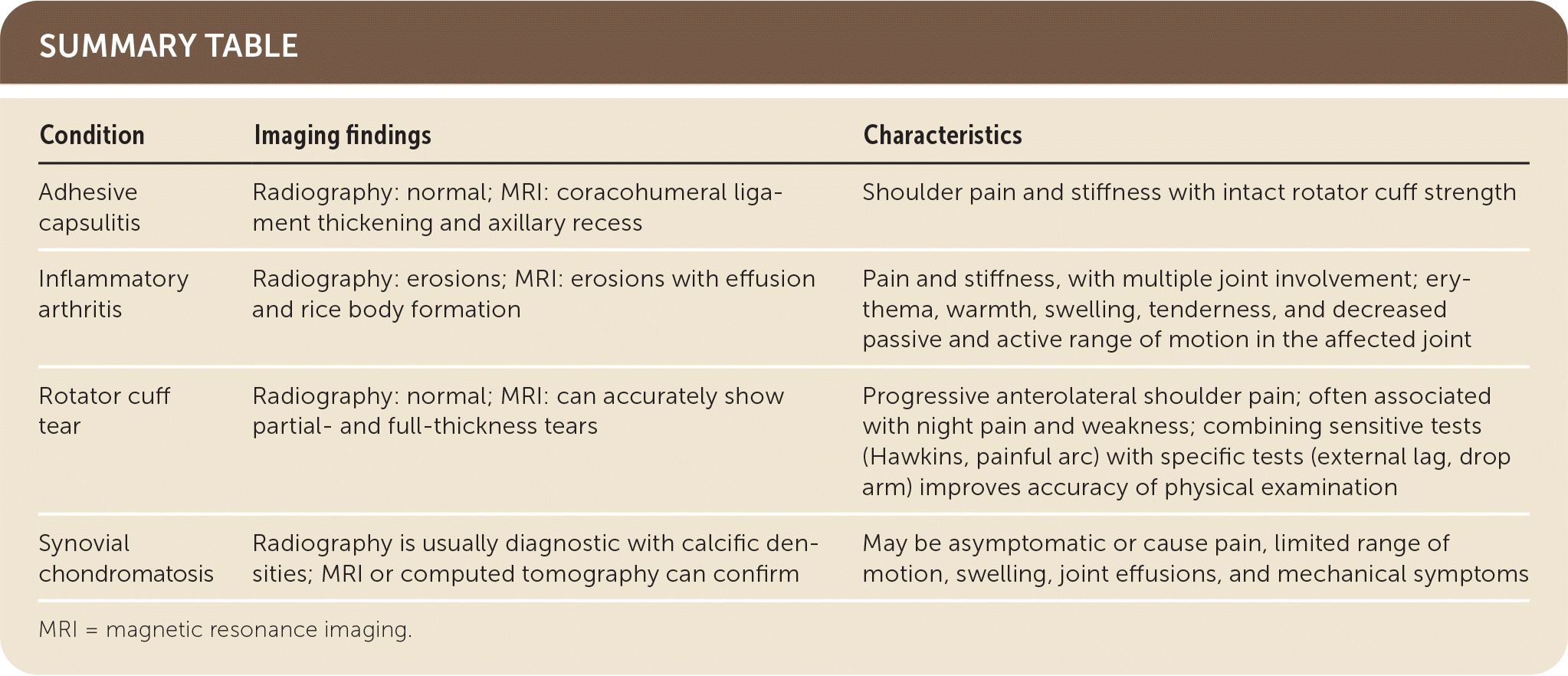
| Condition | Imaging findings | Characteristics |
|---|---|---|
| Adhesive capsulitis | Radiography: normal; MRI: coracohumeral ligament thickening and axillary recess | Shoulder pain and stiffness with intact rotator cuff strength |
| Inflammatory arthritis | Radiography: erosions; MRI: erosions with effusion and rice body formation | Pain and stiffness, with multiple joint involvement; erythema, warmth, swelling, tenderness, and decreased passive and active range of motion in the affected joint |
| Rotator cuff tear | Radiography: normal; MRI: can accurately show partial- and full-thickness tears | Progressive anterolateral shoulder pain; often associated with night pain and weakness; combining sensitive tests (Hawkins, painful arc) with specific tests (external lag, drop arm) improves accuracy of physical examination |
| Synovial chondromatosis | Radiography is usually diagnostic with calcific densities; MRI or computed tomography can confirm | May be asymptomatic or cause pain, limited range of motion, swelling, joint effusions, and mechanical symptoms |
MRI = magnetic resonance imaging.

