A 23-year-old patient presented with a nonhealing wound in the submandibular area. The lesion began eight months earlier while the patient was working on a construction project in Cameroon, which involved frequent partial submersion in water.
The lesion began as a large, painful area around the angle of the left mandible (Figure 1) that was accompanied by fever, lymphadenopathy, and pain with swallowing. The abscess was drained, but no other treatment was provided because of limited resources.
FIGURE 1
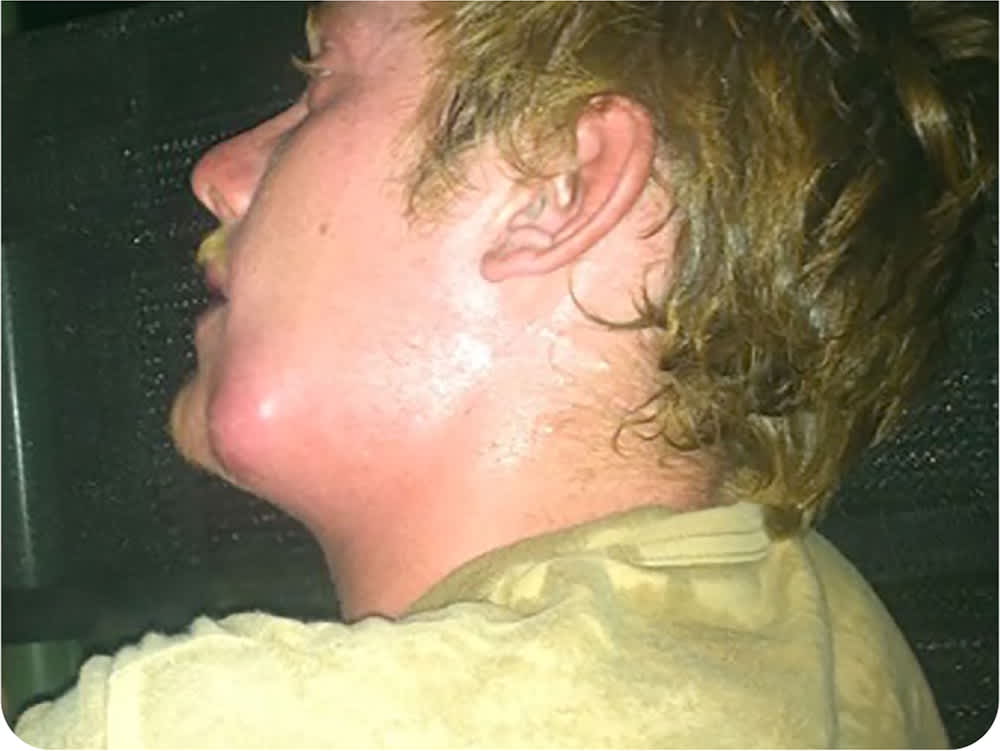
Eight months later, the lesion had decreased in size but never healed. It continually drained a small amount of pus and occasionally increased in size. The patient did not recall having any bites or scratches while in Cameroon and had no symptoms of common tropical diseases. No one else in the group in Cameroon reported having a similar condition. The patient did not have current fevers, chills, tooth pain, oral lesions, swollen glands, dysphagia, night sweats, weight loss, or other symptoms.
Physical examination was unremarkable except for a soft, nonfluctuant, nontender, 2-cm, oval-shaped lesion on the left jaw (Figure 2). A small amount of granulation tissue was present. Scanty white discharge could be expressed from the lesion through a 3-mm central opening. A complete blood count was normal. Wound culture grew Prevotella denticola.
FIGURE 2
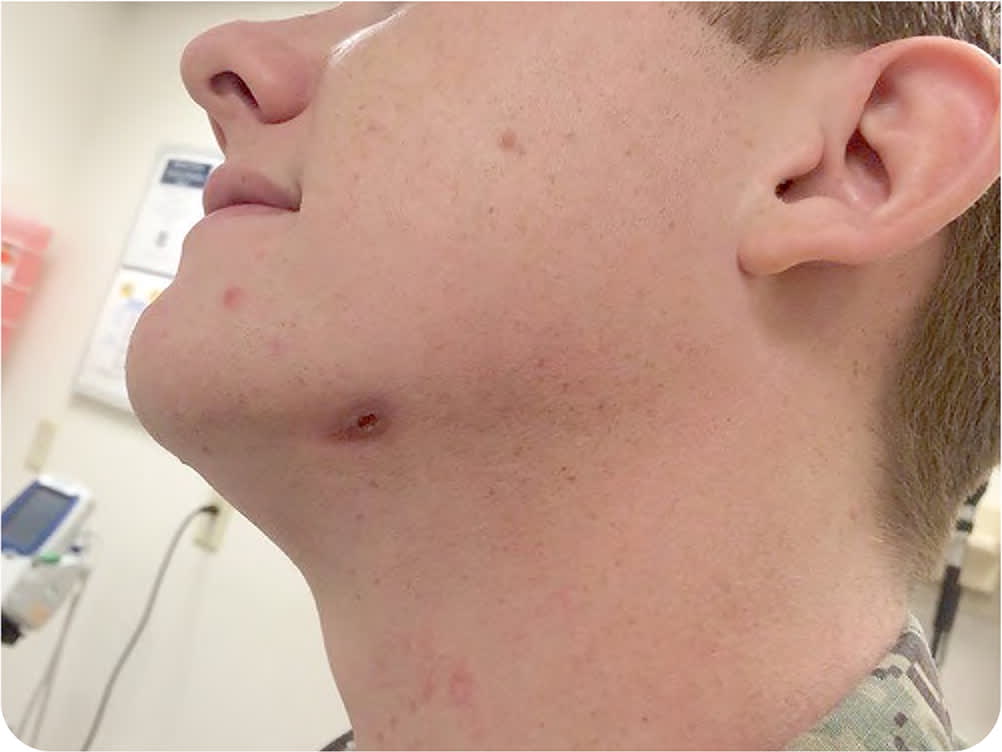
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
- A. Actinomycosis.
- B. Cutaneous leishmaniasis.
- C. Mycobacterium marinum infection.
- D. Periodontal abscess.
See the following page for discussion.
Discussion
The answer is D: periodontal abscess. Periodontal abscesses are common manifestations of untreated dental caries and periodontal disease. Periodontal infections can extend beyond their natural boundaries, causing infections in deep fascial spaces of the head and neck. If untreated, the infection can form a sinus tract to the external subcutaneous tissue.
Initially, the periodontal infection presents as pain and erythema at the site of the dental caries. Without treatment, it can progress to an abscess with edema, erythema, and pain at the remote space, such as the submandibular area, due to formation of a sinus tract that may rupture. Over time, a nonhealing ulceration or recurrent, draining abscess may develop. Wound cultures grow common anaerobic oral bacteria, such as Porphyromonas gingivalis, Prevotella intermedia, or Prevotella denticola.1
Actinomycosis is caused by Actinomyces israelii or related anaerobic, gram-positive bacteria that colonize the mouth and digestive tract but are not usually pathogenic unless the mucosa is damaged. The most common form of actinomycosis is a cervicofacial infection following an odontogenic infection, such as dental caries or periodontal disease. Actinomycosis usually presents as a slow-growing, painless, indurated area that progresses into a large abscess involving the perimandibular region, with or without a sinus tract or mandibular osteomyelitis.2
Cutaneous leishmaniasis is a parasitic infection transmitted by sand flies in the tropics, subtropics, and southern Europe. It is characterized by one or more erythematous papules that develop into nodules, ulcerate, and crust over. The lesions have distinct raised borders and are painless. Cutaneous leishmaniasis can occur on any area of exposed skin.3
Mycobacterium marinum is an acid-fast bacillus organism found in fresh and salt waters worldwide. An infection can occur through direct contact with contaminated water after a skin or soft tissue injury, typically on the extremities. M. marinum infection is characterized by erythematous, verrucous, or crusted plaques that may develop into a nodule, a series of nodules, or an ulceration. The surface of the lesion may exude a yellow, purulent discharge. The lesions generally resolve spontaneously but may persist for months.4
SUMMARY TABLE

| Condition | Characteristics | Organism |
|---|---|---|
| Actinomycosis | Slow-growing, painless, indurated area that progresses into a large abscess involving the perimandibular region, with or without a sinus tract or osteomyelitis | Actinomyces israelii or related anaerobic, gram-positive bacteria that colonize the mouth or digestive tract |
| Cutaneous leishmaniasis | One or more erythematous, painless papules with raised borders that develop into nodules, ulcerate, and crust over; can occur on any area of exposed skin | Leishmania parasite; transmitted by sand flies |
| Mycobacterium marinum infection | Erythematous, verrucous, or crusted plaques that may develop into a nodule, a series of nodules, or an ulceration, usually on the extremities | M. marinum, an acid-fast bacillus found in fresh and salt waters worldwide |
| Periodontal abscess | Painful, erythematous abscess progressing to a nonhealing ulceration or recurrent, draining abscess through a sinus tract to the submandibular area; caused by untreated dental caries or periodontal disease | Common anaerobic oral bacteria, such as Porphyromonas gingivalis, Prevotella intermedia, or Prevotella denticola |
The opinions and assertions contained herein are the private views of the authors and are not to be construed as the official policy or position of the U.S. military, the Department of Defense, or the U.S. government.

