Bipolar disorders are common, recurrent mental health conditions of variable severity that are difficult to diagnose. Affected individuals have higher rates of other mental health disorders, substance use disorders, and comorbid chronic medical illnesses. New diagnostic criteria and specifiers with attention on mixed features and anxious distress aid the physician in recognizing episode severity and prognosis. Physicians should consider bipolar disorder in any patient presenting with depression. Pharmacotherapy with mood stabilizers, such as lithium, anticonvulsants, and antipsychotics, is a first-line treatment that should be continued indefinitely because of the risk of patient relapse. Active lifestyle approaches include good nutrition, exercise, sleep hygiene, and proper weight management. Monotherapy with antidepressants is contraindicated during episodes with mixed features, manic episodes, and in bipolar I disorder. Ongoing management involves monitoring for suicidal ideation, substance use disorders, treatment adherence, and recognizing medical complications of pharmacotherapy. Psychotherapy is a useful adjunct to pharmacotherapy. Patients and their support systems should be educated about the chronic nature of this illness, possible relapse, suicidality, environmental triggers (e.g., seasonal light changes, shift work, other circadian disruption), and the effectiveness of early intervention to reduce complications.
Bipolar disorders comprise recurrent episodes of elevated mood and depression.1 The relapse rate is more than 70% over five years.2 Definitions of the various types of bipolar disorders are provided in Table 13,4; diagnostic criteria are listed in Table 2.3 Hypomania can occur in bipolar I and II disorders, whereas mania, which may include psychosis, appears only in bipolar I disorder. The nature and prognosis of the current episode and the likelihood of future ones can be described with specific attributes3 (Table 33–5 ).
SORT: KEY RECOMMENDATIONS FOR PRACTICE
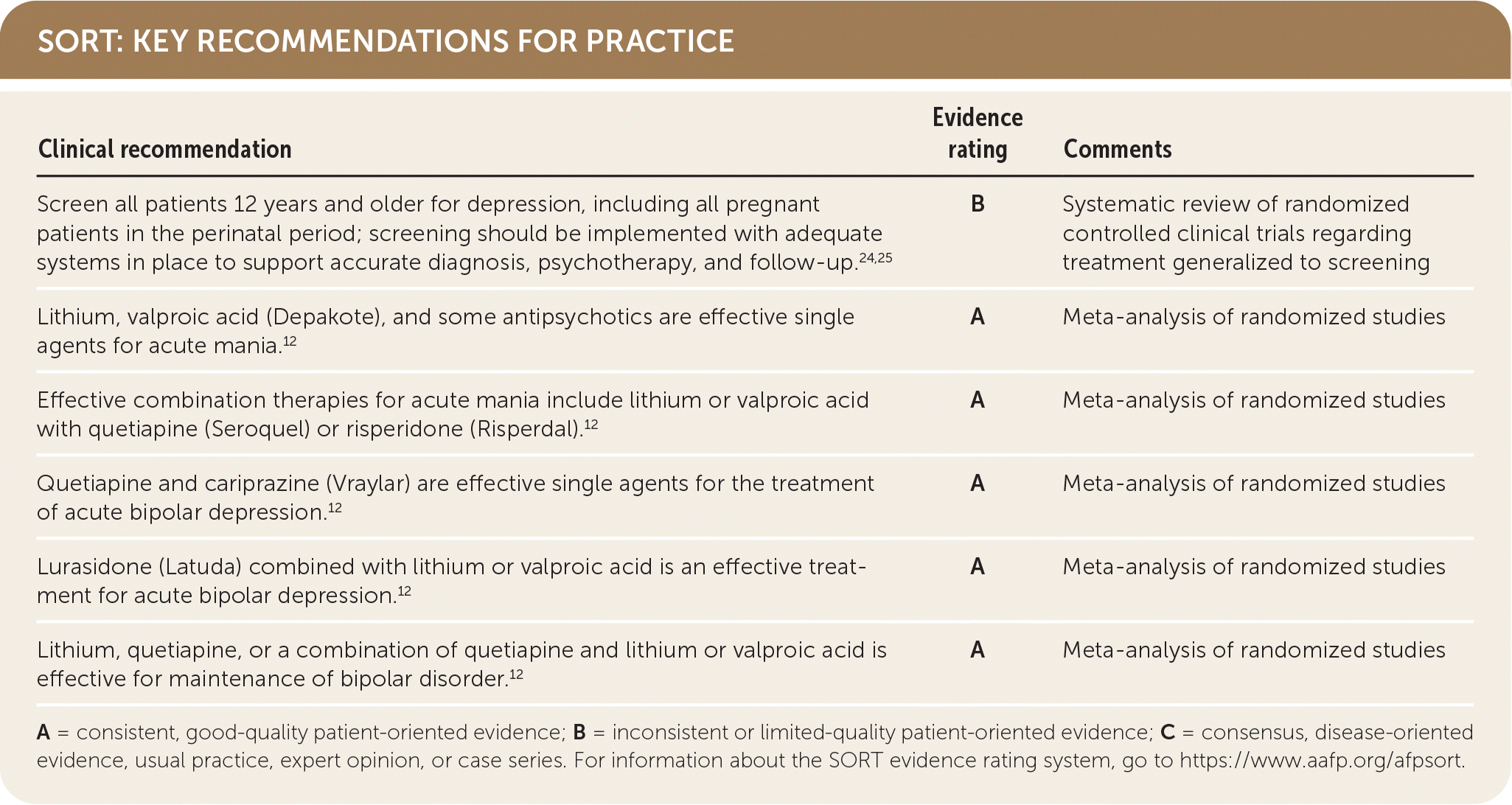
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
TABLE 1. Categories and Types of Bipolar Disorders

| Disorder | Definitions |
|---|---|
| Bipolar I disorder | Manic or mixed feature episode with or without psychosis and/or major depression |
| Bipolar II disorder | Hypomanic episode with major depression; no history of mania, but can have a history of hypomania |
| Cyclothymia | Hypomanic and depressive symptoms that do not meet bipolar II disorder criteria, no major depressive episodes, occurring over two years, with no more than two months free of symptoms |
| Bipolar disorder, not otherwise specified | Does not meet criteria for major depression, bipolar I disorder, bipolar II disorder, or cyclothymia (e.g., less than one week of manic symptoms, without psychosis or hospitalization) |
| Bipolar disorder, mixed features type or major depressive disorder, mixed features type | Mixed type, also known as mixed features, is a recent specifier that includes concurrent features of hypomania or mania and depression; patients who do not meet full criteria for bipolar disorders remain categorized as having unipolar depression |
| Substance-induced mania (include name of substance) | Examples include steroids, alcohol, cocaine, or prescription antidepressants |
| Unspecified | Used for suspicion (e.g., in emergency department) |
Note: See Table 3 for specifiers.
TABLE 2. DSM-5 Criteria for Bipolar I Disorder

| Diagnostic criteria For a diagnosis of bipolar I disorder, it is necessary to meet the following criteria for a manic episode. The manic episode may have been preceded by and may be followed by hypomanic or major depressive episodes. | |||
Manic episode
Note: A full manic episode that emerges during antidepressant treatment (e.g., medication, electroconvulsive therapy) but persists at a fully syndromal level beyond the physiologic effect of that treatment is sufficient evidence for a manic episode and, therefore, a bipolar I diagnosis. Note: Criteria A–D constitute a manic episode. At least one lifetime manic episode is required for the diagnosis of bipolar I disorder. | |||
Hypomanic episode
Note: A full hypomanic episode that emerges during antidepressant treatment (e.g., medication, electroconvulsive therapy) but persists at a fully syndromal level beyond the physiologic effect of that treatment is sufficient evidence for a hypomanic episode diagnosis. However, caution is indicated so that one or two symptoms (particularly increased irritability, edginess, or agitation following antidepressant use) are not taken as sufficient for diagnosis of a hypomanic episode, nor necessarily indicative of a bipolar diathesis. Note: Criteria A–F constitute a hypomanic episode. Hypomanic episodes are common in bipolar I disorder but are not required for the diagnosis of bipolar I disorder. | |||
Major depressive episode
Note: Criteria A–C constitute a major depressive episode. Major depressive episodes are common in bipolar I disorder but are not required for the diagnosis of bipolar I disorder. Note: Responses to a significant loss (e.g., bereavement, financial ruin, losses from a natural disaster, a serious medical illness or disability) may include the feelings of intense sadness, rumination about the loss, insomnia, poor appetite, and weight loss noted in Criterion A, which may resemble a depressive episode. Although such symptoms may be understandable or considered appropriate to the loss, the presence of a major depressive episode in addition to the normal response to a significant loss should also be carefully considered. This decision inevitably requires the exercise of clinical judgment based on the individual's history and the cultural norms for the expression of distress in the context of loss. The occurrence of the manic and major depressive episode(s) is not better explained by schizoaffective disorder, schizophrenia, schizophreniform disorder, delusional disorder, or other specified or unspecified schizophrenia spectrum and other psychotic disorder. Specify: | |||
| With anxious distress | With melancholic features | With mood-incongruent psychotic features | With seasonal pattern |
| With mixed features | With atypical features | With catatonia | |
| With rapid cycling | With mood-congruent psychotic features | With peripartum onset | |
DSM-5 = Diagnostic and Statistical Manual of Mental Disorders, 5th ed.
Reprinted with permission from Diagnostic and Statistical Manual of Mental Disorders. 5th ed. American Psychiatric Association; 2013:123–127.
TABLE 3. Clinical Distinctions and DSM-5 Criteria for Mood Disorders Involved in Diagnosing Bipolar Disorders
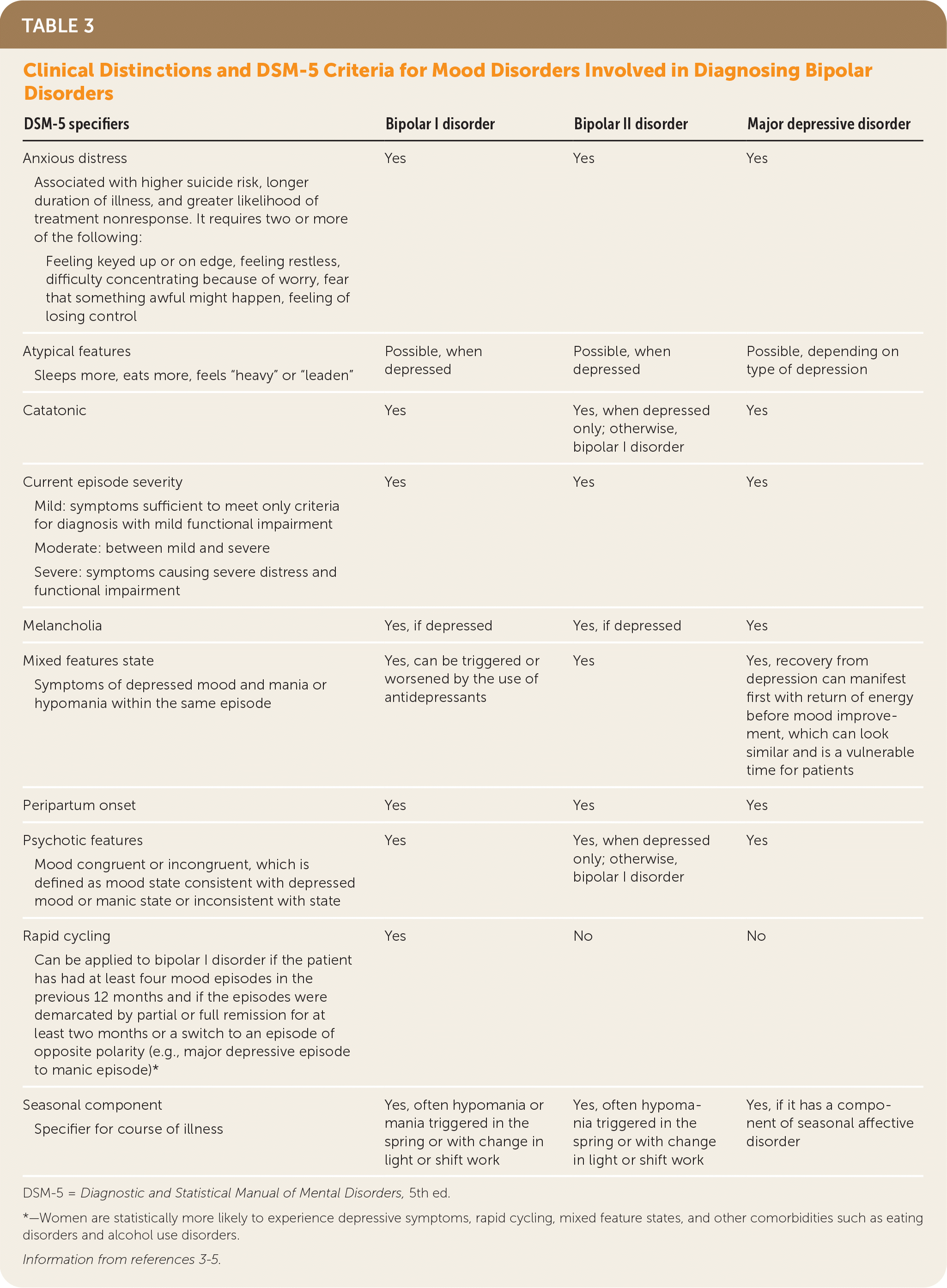
| DSM-5 specifiers | Bipolar I disorder | Bipolar II disorder | Major depressive disorder |
|---|---|---|---|
| Anxious distress Associated with higher suicide risk, longer duration of illness, and greater likelihood of treatment nonresponse. It requires two or more of the following: Feeling keyed up or on edge, feeling restless, difficulty concentrating because of worry, fear that something awful might happen, feeling of losing control | Yes | Yes | Yes |
| Atypical features Sleeps more, eats more, feels “heavy” or “leaden” | Possible, when depressed | Possible, when depressed | Possible, depending on type of depression |
| Catatonic | Yes | Yes, when depressed only; otherwise, bipolar I disorder | Yes |
| Current episode severity Mild: symptoms sufficient to meet only criteria for diagnosis with mild functional impairment Moderate: between mild and severe Severe: symptoms causing severe distress and functional impairment | Yes | Yes | Yes |
| Melancholia | Yes, if depressed | Yes, if depressed | Yes |
| Mixed features state Symptoms of depressed mood and mania or hypomania within the same episode | Yes, can be triggered or worsened by the use of antidepressants | Yes | Yes, recovery from depression can manifest first with return of energy before mood improvement, which can look similar and is a vulnerable time for patients |
| Peripartum onset | Yes | Yes | Yes |
| Psychotic features Mood congruent or incongruent, which is defined as mood state consistent with depressed mood or manic state or inconsistent with state | Yes | Yes, when depressed only; otherwise, bipolar I disorder | Yes |
| Rapid cycling Can be applied to bipolar I disorder if the patient has had at least four mood episodes in the previous 12 months and if the episodes were demarcated by partial or full remission for at least two months or a switch to an episode of opposite polarity (e.g., major depressive episode to manic episode)* | Yes | No | No |
| Seasonal component Specifier for course of illness | Yes, often hypomania or mania triggered in the spring or with change in light or shift work | Yes, often hypomania triggered in the spring or with change in light or shift work | Yes, if it has a component of seasonal affective disorder |
DSM-5 = Diagnostic and Statistical Manual of Mental Disorders, 5th ed.
*—Women are statistically more likely to experience depressive symptoms, rapid cycling, mixed feature states, and other comorbidities such as eating disorders and alcohol use disorders.
Epidemiology
Bipolar disorders, affecting more than 1% of the world's population, have no predilection for race, sex, ethnicity, or socioeconomic status.4 Bipolar I disorder has a higher lifetime incidence than bipolar II disorder (0.6% and 0.4%, respectively).6 The mean age at onset is 18 years in bipolar I disorder and 22 years in bipolar II disorder.7
One-fourth of patients presenting with depression or anxiety in a primary care setting have been diagnosed with a bipolar disorder.8 Three-fourths of patients with bipolar disorder have a history of three additional and concurrent mental health conditions, most commonly anxiety disorders, impulse control and attention-deficit/hyperactivity disorders, and substance use disorders, which are associated with worse outcomes.9,10 One-third of patients who have been diagnosed with bipolar disorder will attempt suicide in their lifetime, 16% will have attempted suicide within the past year, and 6% to 7% complete suicide.11,12 Twenty-six percent of suicides occur within six weeks of a hospital discharge.11,12 Patients who have anxious distress have a higher risk of suicide, longer illness duration, and poorer response to medication.13
Etiology
Bipolar disorders are multifactorial conditions with a genetic predisposition affected by stress and the environment. Children of parents with bipolar disorders have a 4% to 15% risk of being affected, compared with a less than 2% risk in children of parents without bipolar disorder.12 Acute stressors are often associated with the initial onset of illness and sometimes with recurrence.5 These include stressful life events, adverse childhood events and trauma, suicide of a family member, and disruptions in the sleep cycle.14 Biologic susceptibility, central and peripheral nervous system inflammation, abnormal endocrine and neuronal pathways, and mitochondrial dysfunction inheritance patterns have been implicated in bipolar disorders.15,16
Clinical Presentation
Patients typically present for treatment with depression or anxiety or with mixed features, which include concurrent mania and depression.2,8 This depression may be indistinguishable from unipolar depression12 (Table 412,17,18 ) and often starts in early childhood.19 Women are more susceptible during hormonal fluctuations, such as during menses, childbirth, and menopause.20 Diagnosis may be delayed because a series of depressive episodes may occur before a mixed features, manic, or hypomanic episode manifests. Patients typically do not present for care with hypomania because, despite possible negative consequences, it is often seen as a desirable state by the patient.21 Physicians should specifically ask patients who are depressed about symptoms of mania or hypomania (Table 4).12,17,18 Shift work, travel across time zones, and seasonal light changes such as during daylight savings time can trigger hypomania and mania. As many as 25% of patients may present with a seasonal pattern.22,23
TABLE 4. Factors That Raise Suspicion for Bipolar Disorders

| Attempted suicide |
| Atypical behaviors/depression (particularly in men): hypersomnia, increased appetite, psychosis, pathologic guilt, labile mood |
| Drug or alcohol abuse |
| Episodic hypersexuality |
| Family history of multiple instances of suicide, incarceration, drug or alcohol abuse |
| Having a relative with a bipolar disorder |
| Intolerance of an antidepressant, steroid, or other medication, especially if the medication caused agitation or mania |
| Irregular mood changes from low to high in context of decreased need for sleep or periods of intense goal orientation |
| Irritability, impulsivity, irrationality (can be part of a mixed feature presentation) |
| Legal or financial problems |
| Multiple divorces |
| Multiple relatives with any of the following: anxiety, attention-deficit/hyperactivity disorder, depression, obsessive-compulsive disorder, panic disorder |
| No response to three or more antidepressant trials |
| Personal history of bipolar disorder |
| Prior episodes of depression, especially with early onset (e.g., 13 years or younger), seasonal variability |
| Prior episodes of mania or hypomania |
| Racing thoughts that prevent sleep initiation (can be part of a mixed feature presentation) |
| Recurrent job loss |
| Reduced need for sleep for a few days without feeling tired (in a hypomanic or manic phase) |
| Sleep disruptions (e.g., shift work, childcare, travel, time change, change in season, especially spring and fall) that trigger a manic or hypomanic event |
Evaluation
The U.S. Preventive Services Task Force recommends screening for depressive disorders for patients 12 years and older, including all pregnant patients in the perinatal period, in outpatient settings provided that systems are in place to support accurate diagnosis, psychotherapy, and follow-up.24,25 The most commonly used tool for screening is the age-appropriate Patient Health Questionnaire.26 Bipolar II disorder is often under-recognized in primary care practices unless physicians specifically look for it.27 Office-based tools, including the Mood Disorder Questionnaire (https://www.aafp.org/dam/AAFP/documents/patient_care/nrn/mood-disorder-questionnaire.pdf), can be useful in excluding bipolar disorders, but they are not sufficient to confirm a diagnosis.28 Other tests may be more sensitive, but the Mood Disorder Questionnaire is the most specific (0.90), with a sensitivity of 0.73.29,30
Additional online assessment measures are available for use at initial interviews and follow-up as part of the emerging measures, Section III, of the Diagnostic and Statistical Manual of Mental Disorders, 5th ed. (DSM-5).3,30
The use of mobile apps cannot currently be recommended as a stand-alone intervention for bipolar disorders or other mental health disorders because of a lack of evidence.31,32
Table 412,17,18 and Table 533 provide characteristics that distinguish bipolar disorders from other diagnoses.33–35
TABLE 5. Select Causes of Secondary Mania

| Diseases Collagen vascular disease: systemic lupus erythematosus Endocrine disease: Cushing disease, hyper- or hypothyroidism Infectious disease: herpes encephalitis, HIV encephalitis, influenza, neurosyphilis Neurologic disease: complex partial seizures, Huntington chorea, migraine headache, multiple sclerosis, neoplasm, stroke, traumatic brain injury, Wilson disease Vitamin deficiency: B12, folate, niacin, thiamine |
| Medications Cardiovascular: captopril, hydralazine Endocrine: bromocriptine (Parlodel), corticosteroids Neurologic agents: HIV medications, including integrase inhibitors and agents that cross the blood-brain barrier; levetiracetam (Keppra); levodopa Psychiatric: any antidepressant, disulfiram (Antabuse), methylphenidate (Ritalin) Other agents: baclofen (Lioresal), cimetidine (Tagamet), isoniazid |
| Substance use disorders Including alcohol, bath salts, hallucinogens, opiates, phencyclidine (PCP), stimulants (e.g., amphetamines, cocaine) |
Information from reference 33.
COMORBID MEDICAL CONDITIONS
General medical conditions are more common in patients with bipolar disorders compared with age-matched cohorts. For example, cardiovascular risk for patients who have a bipolar disorder is approximately double that for the general population.36 Appropriate evaluation for diabetes mellitus and lipid abnormalities, which are commonly associated with bipolar disorders, is needed. Table 6 lists tests that can be considered in the evaluation of patients with a suspected bipolar disorder.37 High-quality evidence supports the use of metformin for metabolic adverse effects of treatment.18
TABLE 6. Medical Tests to Consider in the Evaluation of Patients with a Suspected Bipolar Disorder
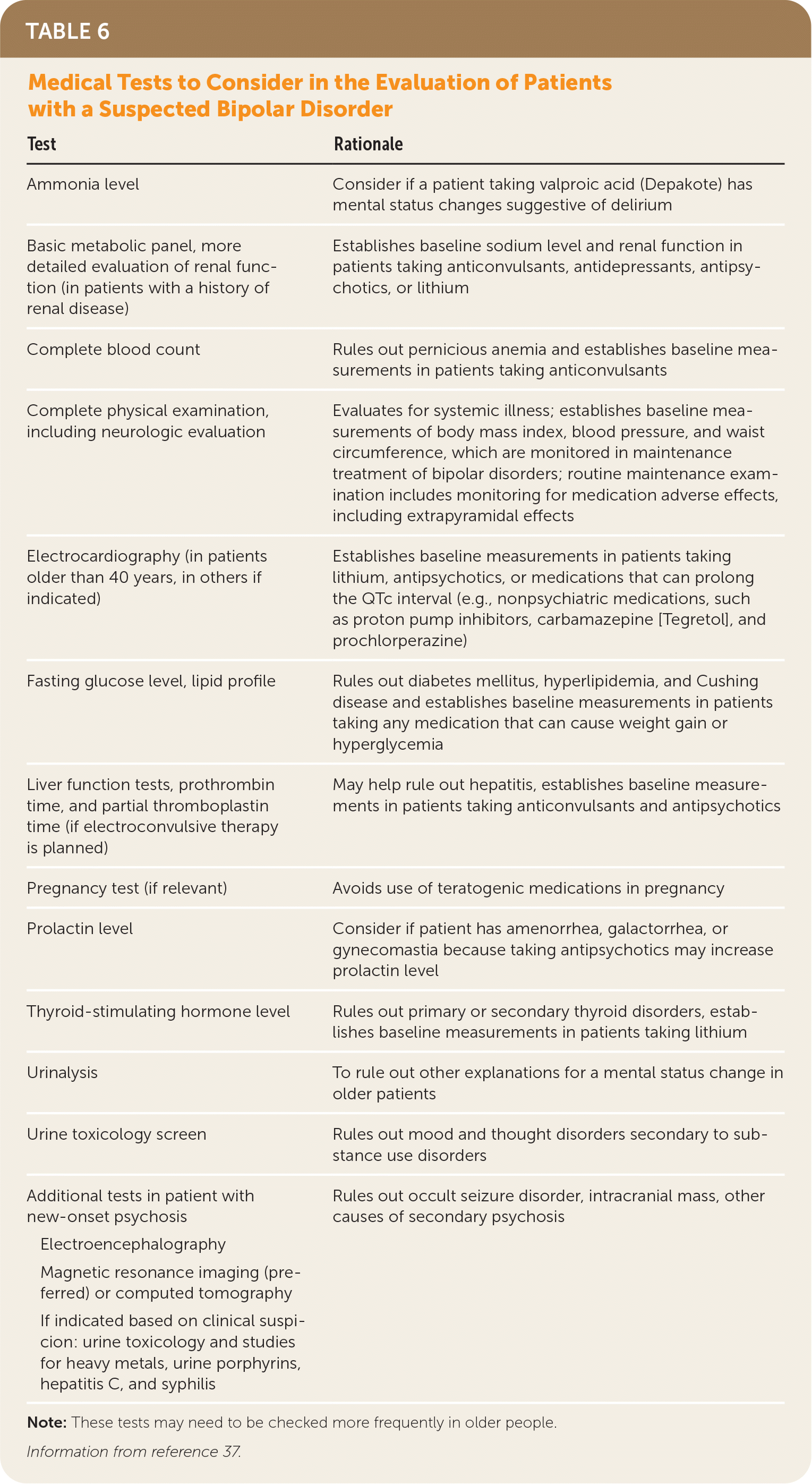
| Test | Rationale |
|---|---|
| Ammonia level | Consider if a patient taking valproic acid (Depakote) has mental status changes suggestive of delirium |
| Basic metabolic panel, more detailed evaluation of renal function (in patients with a history of renal disease) | Establishes baseline sodium level and renal function in patients taking anticonvulsants, antidepressants, antipsychotics, or lithium |
| Complete blood count | Rules out pernicious anemia and establishes baseline measurements in patients taking anticonvulsants |
| Complete physical examination, including neurologic evaluation | Evaluates for systemic illness; establishes baseline measurements of body mass index, blood pressure, and waist circumference, which are monitored in maintenance treatment of bipolar disorders; routine maintenance examination includes monitoring for medication adverse effects, including extrapyramidal effects |
| Electrocardiography (in patients older than 40 years, in others if indicated) | Establishes baseline measurements in patients taking lithium, antipsychotics, or medications that can prolong the QTc interval (e.g., nonpsychiatric medications, such as proton pump inhibitors, carbamazepine [Tegretol], and prochlorperazine) |
| Fasting glucose level, lipid profile | Rules out diabetes mellitus, hyperlipidemia, and Cushing disease and establishes baseline measurements in patients taking any medication that can cause weight gain or hyperglycemia |
| Liver function tests, prothrombin time, and partial thromboplastin time (if electroconvulsive therapy is planned) | May help rule out hepatitis, establishes baseline measurements in patients taking anticonvulsants and antipsychotics |
| Pregnancy test (if relevant) | Avoids use of teratogenic medications in pregnancy |
| Prolactin level | Consider if patient has amenorrhea, galactorrhea, or gynecomastia because taking antipsychotics may increase prolactin level |
| Thyroid-stimulating hormone level | Rules out primary or secondary thyroid disorders, establishes baseline measurements in patients taking lithium |
| Urinalysis | To rule out other explanations for a mental status change in older patients |
| Urine toxicology screen | Rules out mood and thought disorders secondary to substance use disorders |
| Additional tests in patient with new-onset psychosis | Rules out occult seizure disorder, intracranial mass, other causes of secondary psychosis |
| Electroencephalography | |
| Magnetic resonance imaging (preferred) or computed tomography | |
| If indicated based on clinical suspicion: urine toxicology and studies for heavy metals, urine porphyrins, hepatitis C, and syphilis |
Note: These tests may need to be checked more frequently in older people.
Information from reference 37.
Treatment
Prompt diagnosis and treatment improve prognosis by reducing the risk of relapse and doubling the rate of response to medications.38 Medications are the mainstay of therapy and are selected depending on the presenting phase of illness, severity, and patient factors such as prior responses or current medications12,18,38 (Table 712,18 ). Among patients using pharmacotherapy, relapse occurs in up to 25% in the first year; the risk of relapse increases to 40% among patients who are untreated and to more than 70% of patients within five years, regardless of treatment approach.12,18,39 It is recommended that pharmacotherapy be continued indefinitely.12
TABLE 7. Drug Therapy for Patients with Bipolar Disorders
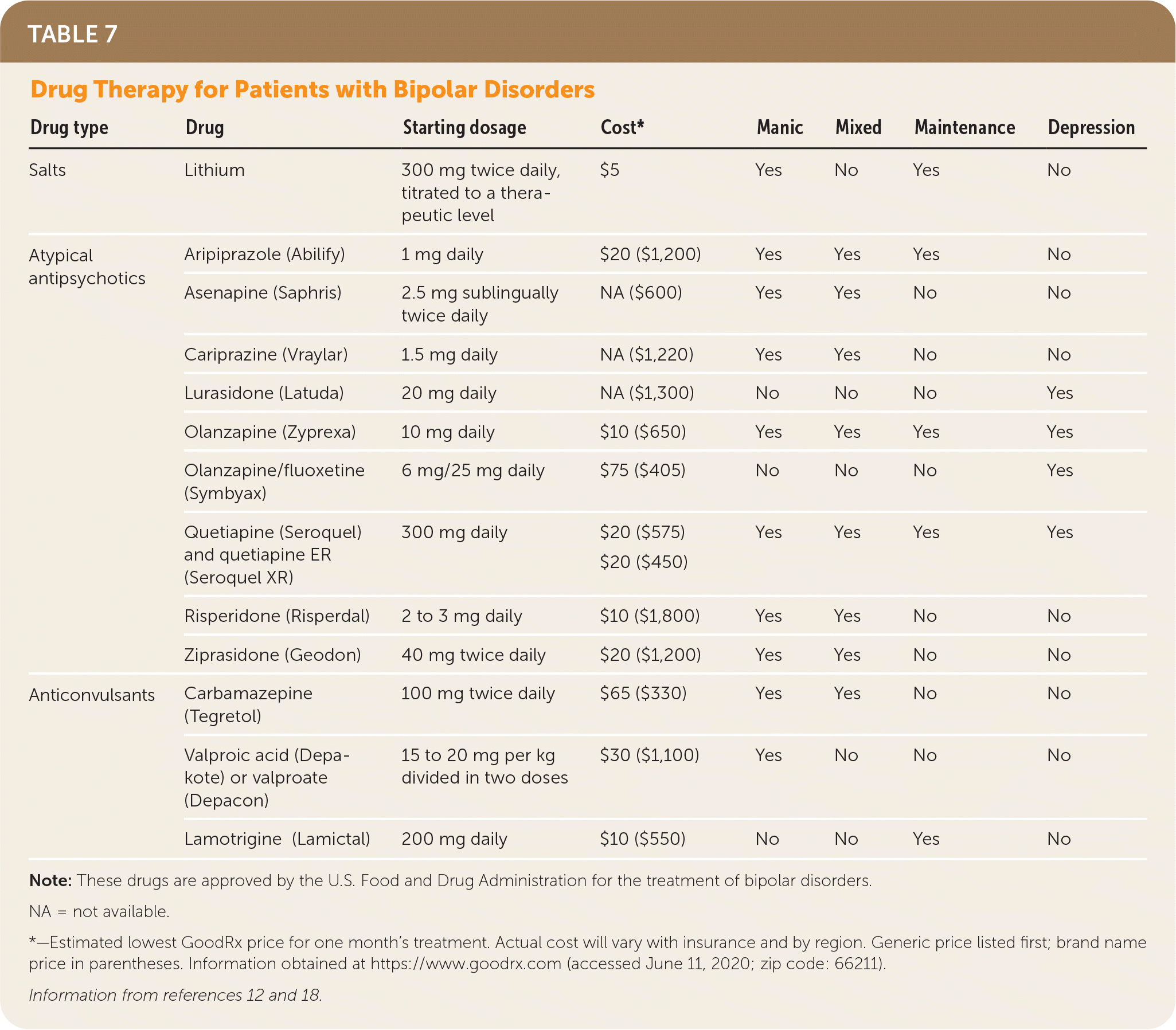
| Drug type | Drug | Starting dosage | Cost* | Manic | Mixed | Maintenance | Depression |
|---|---|---|---|---|---|---|---|
| Salts | Lithium | 300 mg twice daily, titrated to a therapeutic level | $5 | Yes | No | Yes | No |
| Atypical antipsychotics | Aripiprazole (Abilify) | 1 mg daily | $20 ($1,200) | Yes | Yes | Yes | No |
| Asenapine (Saphris) | 2.5 mg sublingually twice daily | NA ($600) | Yes | Yes | No | No | |
| Cariprazine (Vraylar) | 1.5 mg daily | NA ($1,220) | Yes | Yes | No | No | |
| Lurasidone (Latuda) | 20 mg daily | NA ($1,300) | No | No | No | Yes | |
| Olanzapine (Zyprexa) | 10 mg daily | $10 ($650) | Yes | Yes | Yes | Yes | |
| Olanzapine/fluoxetine (Symbyax) | 6 mg/25 mg daily | $75 ($405) | No | No | No | Yes | |
| Quetiapine (Seroquel) and quetiapine ER (Seroquel XR) | 300 mg daily | $20 ($575) $20 ($450) | Yes | Yes | Yes | Yes | |
| Risperidone (Risperdal) | 2 to 3 mg daily | $10 ($1,800) | Yes | Yes | No | No | |
| Ziprasidone (Geodon) | 40 mg twice daily | $20 ($1,200) | Yes | Yes | No | No | |
| Anticonvulsants | Carbamazepine (Tegretol) | 100 mg twice daily | $65 ($330) | Yes | Yes | No | No |
| Valproic acid (Depakote) or valproate (Depacon) | 15 to 20 mg per kg divided in two doses | $30 ($1,100) | Yes | No | No | No | |
| Lamotrigine (Lamictal) | 200 mg daily | $10 ($550) | No | No | Yes | No |
Note: These drugs are approved by the U.S. Food and Drug Administration for the treatment of bipolar disorders.
NA = not available.
*—Estimated lowest GoodRx price for one month's treatment. Actual cost will vary with insurance and by region. Generic price listed first; brand name price in parentheses. Information obtained at https://www.goodrx.com (accessed June 11, 2020; zip code: 66211).
Comanagement with a psychiatrist can aid the primary care physician in navigating diagnostic and therapeutic challenges, including relapse, treatment resistance, comorbid psychiatric conditions, and the risk of self-harm. Patients should be educated about the teratogenic effects of many mood stabilizers (Table 88,10,12,40–50 ), the importance of using reliable contraception, and the possibility of risky sexual behavior during mania.12,18 Patients who have bipolar disorders should be encouraged to keep a record of the medications they have used in the past, including dosages, adverse effects, and effectiveness, to assist with therapy because of the chronic, relapsing nature of the disorder. Monotherapy with antidepressants is contraindicated in patients with mixed features, manic episodes, or bipolar I disorder.12
TABLE 8. Dosing and Monitoring of Medications for Bipolar Disorders

| Medication | Dosing information | Common adverse effects | Monitoring recommendations | Comments |
|---|---|---|---|---|
| Antipsychotics, atypical | Varies | Akathisia, dry mouth, extrapyramidal effects, hyperglycemia, hyperprolactinemia, neuroleptic malignant syndrome, orthostatic hypotension, sexual dysfunction, somnolence, tardive dyskinesia, weight gain | Lipid profile, fasting, baseline and annually; blood glucose level at baseline and as indicated; waist circumference, body weight, and CBC in patients with prior clinically significant leukopenia; measure at baseline and then as clinically indicated AIMS testing* at least twice per year40 | Risperidone (Risperdal) and ziprasidone (Geodon) increase the risk of extrapyramidal effects Aripiprazole (Abilify), ziprasidone, and lurasidone (Latuda) are less associated with metabolic adverse effects but have higher risk of akathisia Caution should be used when decreasing dosages because rebound anxiety and psychosis are possible Increased risk of death in older patients with dementia† |
| Antipsychotics, typical Haloperidol | 2 to 5 mg intramuscularly for acute episode; may repeat every hour as needed until symptoms are controlled; switch to oral form as soon as feasible Initial dosage is based on patient's age and severity of symptoms; dosage rarely should exceed 100 mg in 24 hours No recommendation for use after acute episode | Anxiety, blood dyscrasia, depression, extrapyramidal effects, headache, hyperprolactinemia, hypotension, insomnia, neuroleptic malignant syndrome, pneumonia, psychosis, QT prolongation, restlessness, sedation, seizures, tardive dyskinesia, weight gain | CBC (in patients with prior clinically significant leukopenia) at baseline and monthly in the first three months of therapy Prolactin level as clinically indicated Monitor for extrapyramidal effects, tardive dyskinesia (AIMS testing* at least twice per year),40 and neuroleptic malignant syndrome | Increased risk of death in older patients with dementia† Torsades de pointes possible, particularly with higher than recommended dosages |
| Benzodiazepines Lorazepam (Ativan) | 0.5 to 2 mg orally or intramuscularly, up to 4 mg per day Reduce dosage by 50% in patients who are older and debilitated, patients taking valproate (Depacon), and patients with hepatic or renal disease | Agitation, anterograde amnesia, blood dyscrasia, cognitive impairment, depression, extrapyramidal effects, nausea, respiratory hyponatremia, sedation, syndrome of inappropriate antidiuretic hormone | Periodic CBC and liver function testing for patients on long-term therapy | Contraindicated in patients with myasthenia gravis or acute narrow-angle glaucoma Avoid in patients with history of substance use disorder Continuous long-term use not recommended Paradoxical reactions are more likely in children and older persons; risk of seizure after discontinuation is greater in patients with preexisting seizure disorder and in those taking antidepressants |
| Carbamazepine (Tegretol) | 200 to 1,600 mg orally per day Begin with 200 mg twice per day, adjusting every day by 200 mg as tolerated Titrate to serum level of 4 to 12 mcg per mL | Ataxia; fatigue; headache; hyponatremia; leukopenia; nystagmus; rash, including Stevens-Johnson syndrome and toxic epidermal necrolysis† | Serum carbamazepine levels every one to two weeks initially, then every three to six months or before and after dosage changes CBC and liver function testing monthly for the first two months, then every three to 12 months thereafter Screening for HLA-B1502 in patients with Asian ancestry; patients with positive screening results should avoid carbamazepine because of the risk of Stevens-Johnson syndrome and toxic epidermal necrolysis | Slower titration mitigates adverse effects Hyponatremia occurs in up to 40% of patients Carbamazepine may induce its own metabolism; dose increase after initial titration may be required |
| Valproic acid (Depakote) | Target dosage: 1,000 to 3,000 mg orally per day 15 to 20 mg per kg load in patients with acute mania; may also start with 500 to 750 mg per day in divided doses and adjust every two to three days as tolerated Titrate to serum level of 50 to 125 mcg per mL | Diarrhea, elevated liver transaminase levels, hair loss, hepatic failure,† leukopenia, nausea, pancreatitis,† polycystic ovary syndrome, sedation, thrombocytopenia, tremor, weight gain | Serum valproic acid levels every one to two weeks initially, then every three to six months or before and after dosage changes CBC and liver function testing monthly for the first two months, then every three to 12 months thereafter Can increase ammonia level, so consider testing for patients with mental status change or lethargy | Polycystic ovary syndrome is common in women who start treatment before 20 years of age Adding lamotrigine (Lamictal) to valproic acid increases the risk of serious rash Teratogenic† |
| Lamotrigine | 200 mg orally per day Begin with 25 mg per day and titrate over six weeks; titration and dosage adjustments differ for those taking valproic acid, carbamazepine, phenytoin (Dilantin), phenobarbital, primidone (Mysoline), rifampin, and oral contraceptives | Aseptic meningitis; dizziness; dry mouth; headache; hemophagocytic lymphohistiocytosis; leukopenia; nausea; pancytopenia; rash, including Stevens Johnson syndrome and toxic epidermal necrolysis†; somnolence; thrombocytopenia; tremor | CBC and liver function testing monthly for the first two months, then every three to 12 months thereafter Ask about any new rashes at each visit | Incidence of skin rash is reduced with slow titration and not exceeding recommended dosage; adding lamotrigine to a patient currently taking valproic acid increases the risk of serious rash Incidence of serious rash in adults is 0.08% with monotherapy Adverse reactions mainly occur in the first two to eight weeks of therapy, rarely as late as six months after treatment initiation |
| Lithium | 900 to 1,800 mg orally per day Begin with up to 300 mg twice per day and adjust dosage every two or three days as tolerated; titrate to serum level of 0.6 to 1.5 mEq per L | Cognitive effects, diabetes insipidus, diarrhea, hypothyroidism, nausea, polyuria, sedation, thirst, tremor, weight gain | Serum lithium levels every one to two weeks initially, then every three to six months thereafter or before and five days after dosage changes or with the addition of medications affecting renal function‡ Thyroid function testing§ and renal indices every two or three months in the first six months of therapy, then every six to 12 months thereafter | Toxicity is dose dependent; overdose can be fatal† Incidence of hypothyroidism is higher in women and increases with age High rates of withdrawal compared with valproic acid and lamotrigine in maintenance therapy |
AIMS = Abnormal Involuntary Movement Scale; CBC = complete blood count.
*—https://mmcp.health.maryland.gov/pap/docs/Abnormal%20Involuntary%20Movement%20Scale.pdf
†—U.S. Food and Drug Administration boxed warning.
‡—Nonsteroidal anti-inflammatory drugs, angiotensin-converting enzyme inhibitors, angiotensin receptor blockers, and others.
§—Thyroid-stimulating hormone, total thyroxine, thyroxine uptake.
Adapted with permission from Price AL, Marzani-Nissen GR. Bipolar disorders: a review. Am Fam Physician. 2012;85(5):490–491, with additional information from references 8, 10, 12, and 40–49.
ACUTE MANIA
Mania is defined as a distinct period of abnormally and persistently elevated, expansive, or irritable mood and by abnormally and persistently increased activity or energy that lasts at least one week and is present for most of the day, nearly every day (or any duration if hospitalization is necessary). Three (or more) of the symptoms (four of the symptoms if the mood is only irritable) found in Table 2 are present to a significant degree and represent a noticeable change from usual behavior.3 Early warning signs of a relapse include sleep disturbance, agitation, increased goal orientation, and a disruption in the patient's usual routine. Patients with acute mania require hospitalization because of risk of harm to self or others. Goals of initial treatment include adequate sleep and reduction of psychotic symptoms.
High-quality evidence supports using the class of medications known as mood stabilizers. These include lithium, valproic acid (Depakote), and antipsychotics.12,18,36 Valproic acid is often used for acute mania because it can be titrated quickly.5 Lithium is the treatment of choice for classic euphoric mania, which is defined as a predominance of manic symptoms associated with elevated mood (can include irritability) rather than a mixed or depressed state. Lithium is a proven antisuicidal agent and requires five days to achieve a steady state in the patient.12 Lithium is often given in conjunction with an antipsychotic and a benzodiazepine (e.g., quetiapine [Seroquel], risperidone [Risperdal]), which can assist with sleep, in the acute phase because of the length of time for lithium titration.12
MIXED FEATURES
Mixed features is a specifier in the DSM-5 denoting clinical presentations that include features of depression and either hypomania or mania concurrently.3 Lithium does not benefit patients with mixed features or those who have rapid cycling, which comprises at least four episodes of any type during a 12-month period.3,18 Table 7 lists the medications approved for patients who have mixed features in bipolar disorders.12,18 Despite symptoms of depression, monotherapy with antidepressants for mixed features is contraindicated.
ACUTE DEPRESSION
All patients should be assessed for risks to themselves or others and the need for inpatient treatment. Although several agents are effective for acute depression, quetiapine (Seroquel), cariprazine (Vraylar), lurasidone (Latuda) in combination with lithium or valproic acid, and electroconvulsive therapy appear to be the most fast-acting therapeutic options.12 Although patients are highly responsive to antipsychotics, these medications are associated with weight gain, diabetes, and extrapyramidal effects.51
When mood stabilizers alone are insufficient (Table 712,18 ), augmentation of treatment with anti-depressant medications such as selective serotonin reuptake inhibitors or bupropion (Wellbutrin) may be considered.52 These therapies are less likely to induce mania compared with tricyclic antidepressants, monoamine oxidase inhibitors, or medications that have dual properties, such as venlafaxine.18 When treating sleep disturbance in patients who have depression, physicians should avoid prescribing trazodone because it can induce mania.53
MAINTENANCE THERAPY
High-quality evidence supports the use of lithium, lamotrigine (Lamictal), quetiapine, quetiapine in combination with lithium or valproic acid, aripiprazole (Abilify), and olanzapine (Zyprexa) for maintenance therapy in patients who have bipolar disorders(Table 7)12,18; each medication has specific advantages and disadvantages. The risk of suicide is lowered when patients are more satisfied with their care, when they use lithium therapy, and with treatment of alcohol and tobacco use disorders.36,54
AUGMENTING THERAPIES
Augmenting therapies such as omega-3 fatty acids, light therapy, N-acetylcysteine, ketamine, and probiotics show promise at different phases of illness. However, they lack sufficient evidence to recommend widespread use at this time.12,55,56
RECOGNIZING AND ADDRESSING ADVERSE EFFECTS
In the maintenance phase, patients should receive regular clinical examinations that focus on depressive, manic, and sleep symptoms; suicide risk; substance use disorders; comorbid conditions; and general medical health.12 Extra-pyramidal effects often manifest early and can include akathisia (i.e., subjective sense of motor restlessness); parkinsonism (i.e., cogwheel rigidity of tendons, masked facies, muscle stiffness or rigidity); and other movement disorders, such as dystonias and dyskinesias. Akathisia requires vigilant monitoring because agitation, pacing, and a subjective sense of motor restlessness can also appear to be a worsening of mania or anxiety.57 Often a change in regimen is required because akathisia can lead to suicide.58,59 Tardive dyskinesia is a potentially irreversible movement disorder that can occur within months of initiating antipsychotic therapy in older people, who are also at risk for stroke and other cardiovascular events, and in patients with neurologic vulnerability (e.g., those with HIV infection or other central nervous system diseases). Patients taking antipsychotics should be evaluated using the Abnormal Involuntary Movement Scale (https://mmcp.health.maryland.gov/pap/docs/Abnormal%20Involuntary%20Movement%20Scale.pdf) at least twice annually.40
Dosage reduction should be considered regularly in patients taking antipsychotic medications. Lower dosages may be required in children or older adults, patients with chronic disease, and those who are underweight. Higher dosages are required for patients with severe psychosis.41 Table 8 summarizes dosing and monitoring recommendations for pharmacotherapy and provides specific considerations for individual agents and patient selection.8,10,12,40–50
NONPHARMACOLOGIC THERAPIES
Electroconvulsive therapy is effective for mania and psychotic depression. It is often reserved for older patients and for those who have refractory illness and catatonia for which pharmacotherapy has failed. It can be used for emergent situations, such as in patients with acute psychosis who have suicidal behavior.60
Psychosocial stress is known to trigger manic and depressive symptoms. Behavioral interventions, including basic psychoeducation and cognitive behavior therapy, are evidence-based adjuncts to pharmacotherapy that improve social function and reduce the need for medications, number of hospitalizations, and relapse rates.12,36,61–63
In addition to pharmacotherapy, nutrition, exercise, coping strategies, and positive attitudes toward good health have been beneficial.64 Although there are limited and heterogeneous data that support family interventions for patients who have bipolar disorders,65 patients who have social support in recognizing early warning signs of recurrence appear to have less risk of recurrence and hospitalization and have better functioning.63 Patients who receive intensive psychotherapy12 or group therapy61 have fewer relapses and longer periods of relative wellness compared with patients who receive brief therapy.
Patients with frequent episodes of mania may benefit from strategies that emphasize medication adherence, whereas those with more depressive symptoms benefit from treatments focused on coping strategies and cognitive behavior therapy.12 Patients, families, and caregivers should establish a plan to immediately address suicidal and homicidal ideation if they become apparent.
This article updates previous articles on this topic by Price and Marzani-Nissen50 and Griswold and Pessar.66
Data Sources: We searched the Cochrane Database of Systematic Reviews, Essential Evidence Plus, the U.S. Preventive Services Task Force, the Agency for Healthcare Research and Quality, and Clinical Evidence. A PubMed Clinical Query was completed using the search terms bipolar disorder and bipolar disorder treatment. Search dates: October 4 and December 12, 2019; and August 30, 2020.

