Clinical Question
Is magnetic resonance imaging (MRI) accurate in the early diagnosis of Alzheimer disease in patients with mild cognitive impairment (MCI)?
Evidence-Based Answer
There is insufficient evidence to recommend structural brain MRI to diagnose Alzheimer disease in patients with MCI. Because of its low accuracy, it should not be used as a stand-alone tool in identifying evidence of Alzheimer disease in patients with MCI.1 (Strength of Recommendation: B, based on inconsistent or limited-quality patient-oriented evidence.)
SUMMARY TABLE
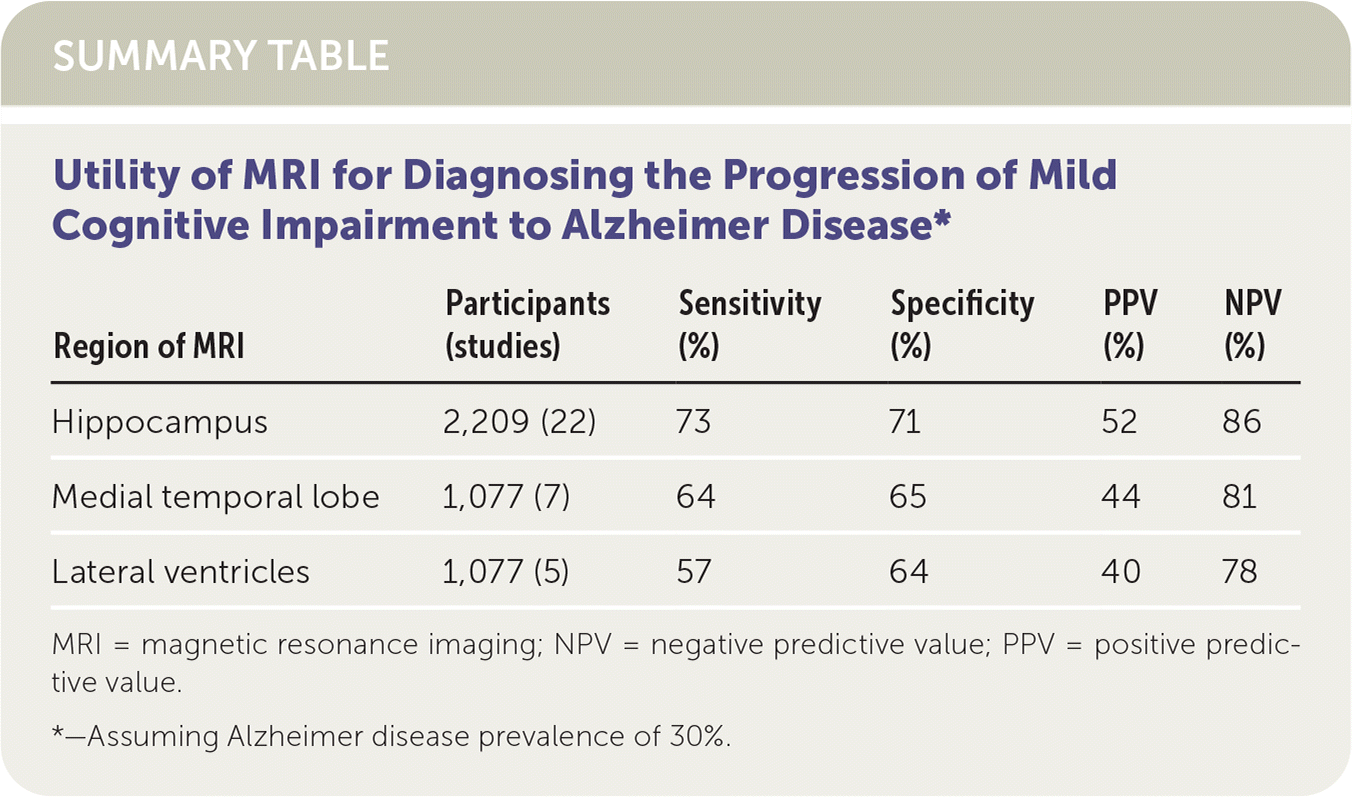
| Region of MRI | Participants (studies) | Sensitivity (%) | Specificity (%) | PPV (%) | NPV (%) |
|---|---|---|---|---|---|
| Hippocampus | 2,209 (22) | 73 | 71 | 52 | 86 |
| Medial temporal lobe | 1,077 (7) | 64 | 65 | 44 | 81 |
| Lateral ventricles | 1,077 (5) | 57 | 64 | 40 | 78 |
MRI = magnetic resonance imaging; NPV = negative predictive value; PPV = positive predictive value.
*—Assuming Alzheimer disease prevalence of 30%.
Practice Pointers
Alzheimer disease is the most common cause of dementia, accounting for 60% to 80% of dementia cases.2 Onset typically occurs after 65 years of age and is often preceded by a predementia phase called MCI.2 MCI has progressed to dementia when these cognitive changes significantly interfere with a person's work or usual daily activities.3 Identifying which patients with MCI will progress to Alzheimer disease could be helpful in early intervention and planning for patients and their families.
MCI is characterized by a noticeable decline in cognition or memory with preserved function in daily living.4 Although memory difficulty is the most common symptom in patients with MCI, there can also be deficits in attention, executive functioning, language, and visuospatial skills. People with MCI and memory loss develop Alzheimer disease at a rate of about 10% to 15% annually compared with 1% to 2% per year in the general population.5 Currently there is no clinical tool to reliably identify which patients with MCI will go on to develop Alzheimer disease.
The authors of this Cochrane review assessed the diagnostic accuracy of structural brain MRI in detecting Alzheimer disease in patients with MCI.1 They included 33 prospective cohort studies (N = 3,935) published from 1999 to 2019 from tertiary care centers in Europe (19 studies), North America (nine studies), North America and Europe (three studies), Taiwan (one study), and Australia (one study).
Patients were diagnosed with MCI by history and neuropsychological testing; their baseline Mini Mental State Examination score was 22 to 29 (median = 27). Because the criteria for diagnosing MCI have changed over the past 20 years, the review authors accepted studies that used varying diagnostic criteria and included all subtypes of MCI (e.g., amnestic single domain, amnestic multiple domain, nonamnestic single domain, nonamnestic multiple domain). Patients with MCI and a median age of 73 years (range = 63 to 87 years) underwent MRI to detect atrophy in brain regions associated with cognition (hippocampus, 22 studies; medial temporal lobe, seven studies; lateral ventricles, five studies). This was compared with the reference standard of follow-up and progression to diagnosis of Alzheimer disease using standard clinical criteria.5
Of the almost 4,000 patients included in these 33 studies, 34% developed Alzheimer dementia during a mean clinical follow-up ranging from one to almost eight years (median = two years).2 Of the patients who did not advance to Alzheimer disease, the majority (99%) remained stable with MCI, whereas few (1%) developed other forms of dementia.
MRI of the hippocampus had the highest positive and negative predictive values. The authors concluded that MRI is not accurate enough to predict which patients with MCI will progress to Alzheimer disease because it will miss about 14% to 22% of cases and falsely predict approximately 48% to 60% of cases.
Overall, the results of this Cochrane review are limited because the studies used different methods for diagnosing MCI and performing brain MRI measurements, and length of patient follow-up varied widely.
Although brain imaging with computed tomography or MRI may be useful in detecting reversible causes of cognitive decline or vascular causes of dementia,6 MCI and dementia caused by Alzheimer disease are still diagnosed based on clinical evidence of a change in cognition with impairments in memory, executive functioning, attention, or language.3,4,7 There is not yet a reliable diagnostic tool to predict who will or will not develop Alzheimer disease.
The practice recommendations in this activity are available at http://www.cochrane.org/CD009628.
Editor's Note: The positive and negative predictive values reported in this Cochrane for Clinicians summary table were calculated by the authors based on raw data provided in the original Cochrane review.

