A five-month-old child with a history of dry skin presented with a spreading rash that began two days earlier. The patient had one day of fever up to 103°F (39.4°C). The rash began on the patient's cheek and then spread over the trunk and extremities. The patient was feeding well and had no vomiting or diarrhea. The patient was delivered vaginally at full term and was up to date on routine immunizations.
Physical examination revealed that the patient was ill-appearing but nontoxic, with a temperature of 104.3°F (40.3°C). There were diffuse, eroded, and coalescing vesicles on the right cheek, chest, abdomen, back, extremities, and scalp (Figure 1 and Figure 2). The genitals, palms, and soles were spared. There was no lymphadenopathy.
FIGURE 1
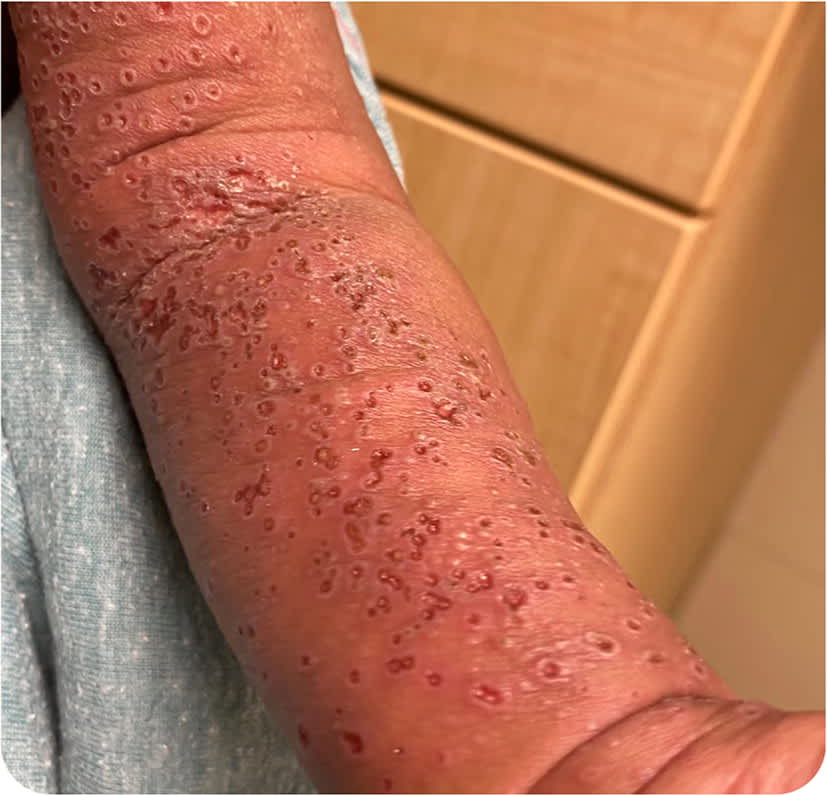
FIGURE 2
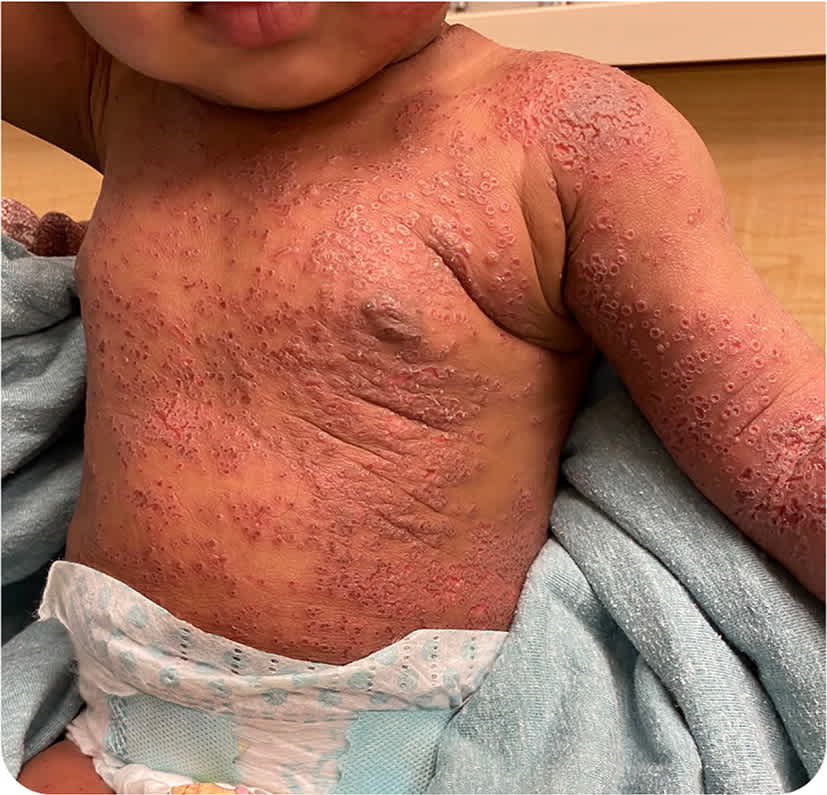
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
- A. Eczema coxsackium.
- B. Eczema herpeticum.
- C. Eczema vaccinatum.
- D. Impetigo.
- E. Primary varicella.
Discussion
The answer is B: eczema herpeticum (also known as Kaposi varicelliform eruption). Eczema herpeticum is a serious complication in patients with chronic skin disease, primarily atopic dermatitis, and is caused by herpes simplex virus 1 infection. Atopic dermatitis, which has a prevalence of up to 17%, results in disruption of the epidermal barrier and impaired cell-mediated immunity.1 This leads to intensely pruritic, inflamed skin and allows for microbial infection.2
Eczema herpeticum is a potentially life-threatening illness that can cause blindness if the eyes are involved and death if severe or untreated. Patients with eczema herpeticum present with herpetic vesicles, usually on the face, neck, and upper trunk. The involved skin has monomorphic papulovesicular lesions that rupture to form small, punched out, crusted ulcers overlying an erythematous base. Patients may have associated symptoms, such as fever, malaise, and lymphadenopathy.
Diagnosis of eczema herpeticum is typically clinical, and treatment should be initiated immediately. Polymerase chain reaction testing, culture, or Tzanck smear can confirm the diagnosis and distinguish the infection from similarly appearing etiologies.
Eczema herpeticum is mainly treated with acyclovir. Systemic antiviral medications and hospitalization are recommended for patients who are immunocompromised or who have severe disease. Because secondary bacterial infections, such as Staphylococcus aureus infection, are common, prophylactic antibiotics (e.g., cephalexin [Keflex], clindamycin, doxycycline, trimethoprim/sulfamethoxazole) are often administered.3
Eczema coxsackium presents as papulovesicular lesions that progress to erosions localized to regions of chronic skin disease. The lesions are similar to eczema herpeticum but less pruritic. Eczema coxsackium typically affects the hands, feet, and oral mucosa, similarly to classic hand-foot-and-mouth disease. Eczema coxsackium leads to no serious long-term sequelae. Treatment is typically supportive and similar to an eczema exacerbation.4
Eczema vaccinatum is a rare complication of smallpox vaccination. The rapidly developing, generalized, vesiculopapular rash can occur in susceptible patients with atopic dermatitis who receive the smallpox vaccine or are exposed to a household contact who received the vaccine. Treatment is largely supportive, with hospitalization based on severity. Vaccinia immune globulin is the only approved treatment.5
Impetigo is a superficial skin infection, typically with S. aureus, that primarily affects children two to five years of age. The lesions manifest as papules with surrounding erythema that progress to vesicles and rupture, forming thick, adherent, honey-colored crusts, most commonly on the face. The rash is treated with topical or oral antibiotics.6
Primary varicella can occur in children younger than one year who are not immunized against varicella-zoster virus infection. Varicella is characterized by disseminated, pruritic, vesicular lesions on an erythematous base in different stages of development on the face, trunk, and extremities. The lesions, ranging from a few to an average of 500, occur in crops and progress from macules and papules to vesicles (“dewdrops on a rose”), then crust over. Treatment is typically supportive but may include acyclovir in individuals at high risk of complications.7
SUMMARY TABLE
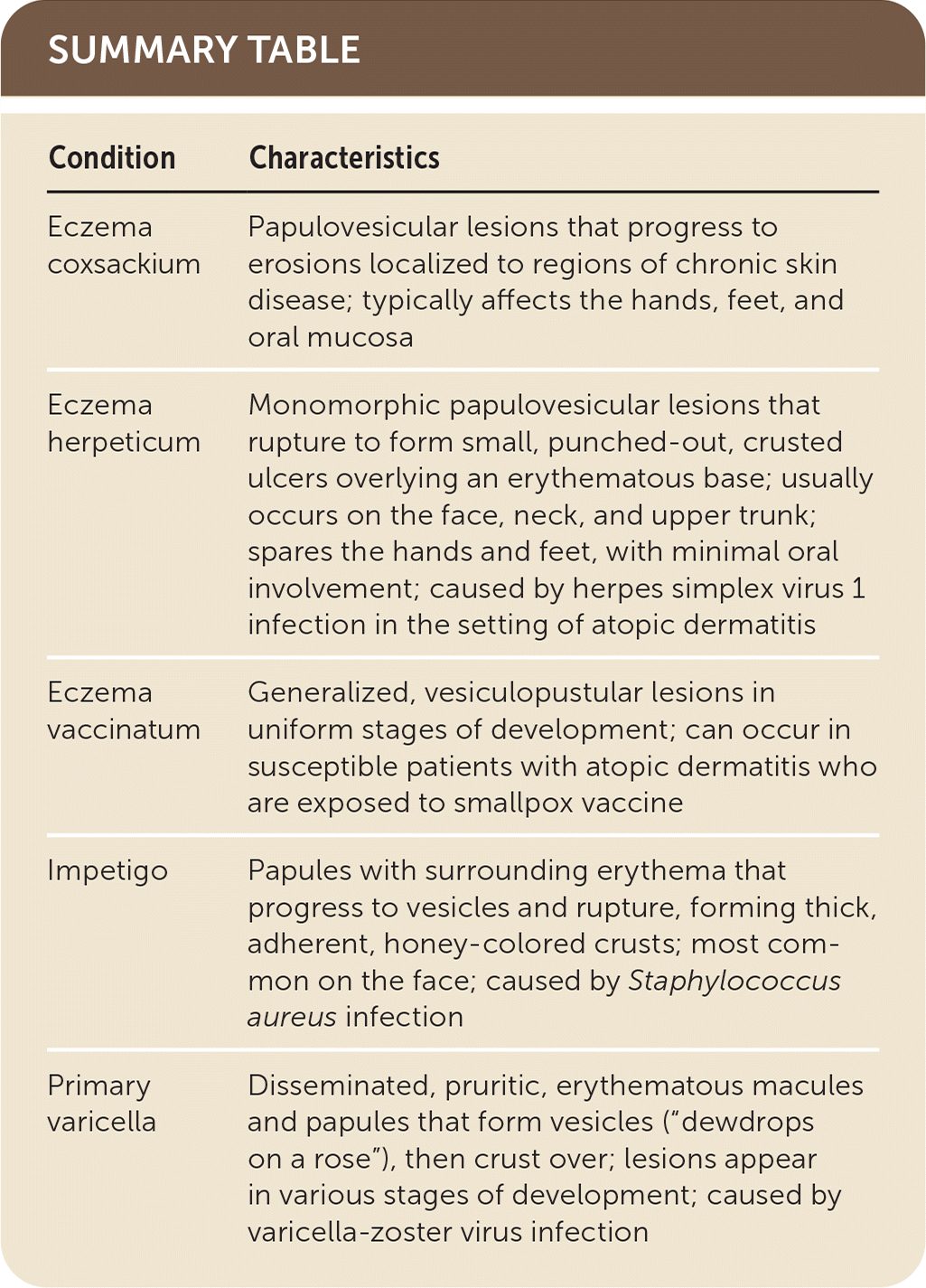
| Condition | Characteristics |
|---|---|
| Eczema coxsackium | Papulovesicular lesions that progress to erosions localized to regions of chronic skin disease; typically affects the hands, feet, and oral mucosa |
| Eczema herpeticum | Monomorphic papulovesicular lesions that rupture to form small, punched-out, crusted ulcers overlying an erythematous base; usually occurs on the face, neck, and upper trunk; spares the hands and feet, with minimal oral involvement; caused by herpes simplex virus 1 infection in the setting of atopic dermatitis |
| Eczema vaccinatum | Generalized, vesiculopustular lesions in uniform stages of development; can occur in susceptible patients with atopic dermatitis who are exposed to smallpox vaccine |
| Impetigo | Papules with surrounding erythema that progress to vesicles and rupture, forming thick, adherent, honey-colored crusts; most common on the face; caused by Staphylococcus aureus infection |
| Primary varicella | Disseminated, pruritic, erythematous macules and papules that form vesicles (“dewdrops on a rose”), then crust over; lesions appear in various stages of development; caused by varicella-zoster virus infection |

