Clinical Question
How effective is kinesiology taping (elastic tape applied to the knee to create patellar tension) for osteoarthritis pain of the knee?
Evidence-Based Answer
Kinesiology taping probably does not produce a clinically significant reduction in knee pain from osteoarthritis. Compared with sham taping, kinesiology taping only minimally reduces standardized pain scores in middle-aged patients with moderate pain from nondeforming osteoarthritis of the knee. It does not cause any clinically significant adverse effects. (Strength of Recommendation: B, based on small randomized controlled trials [RCTs] with conflicting results.)
Evidence Summary
Five double-blind RCTs 1–5 (n = 293) and six single-blind RCTs6–11 (n = 281) evaluated kinesiology taping vs. sham taping in patients with osteoarthritis of the knee. All studies included patient-reported pain scores as an outcome. Researchers randomized patients with radiologically confirmed knee osteoarthritis without deformities on inspection to kinesiology taping (applying elastic adhesive tape with tension to the skin starting just superior to the medial quadriceps tendon and extending inferiorly, circling the patella, and ending near the tibial tuberosity) vs. a sham taping control (applying adhesive tape to the skin but without tension and in a nondynamic circumferential pattern).
All of the studies recruited patients with moderate pain (baseline of five to seven points on a 10-point visual analog scale [VAS]) from chronic knee osteoarthritis; participants were generally 50 to 70 years of age, with a slight majority of women. The participants in nine studies used a 10-point VAS to assess knee pain (two studies used an 11-point VAS). In most cases, they used a global subjective pain rating, typically at rest. Investigators used kinesiology taping and sham taping for periods lasting from one to seven days, with the length of the experimental protocol ranging from a single taping application up to four applications (Table 1).1–11 In five studies, investigators removed the tape before the outcome was measured, blinding the evaluator to which group participants belonged (i.e., double-blinding). Investigators evaluated VAS pain scores for differences between groups initially and again after the tape was in place for various periods of time.
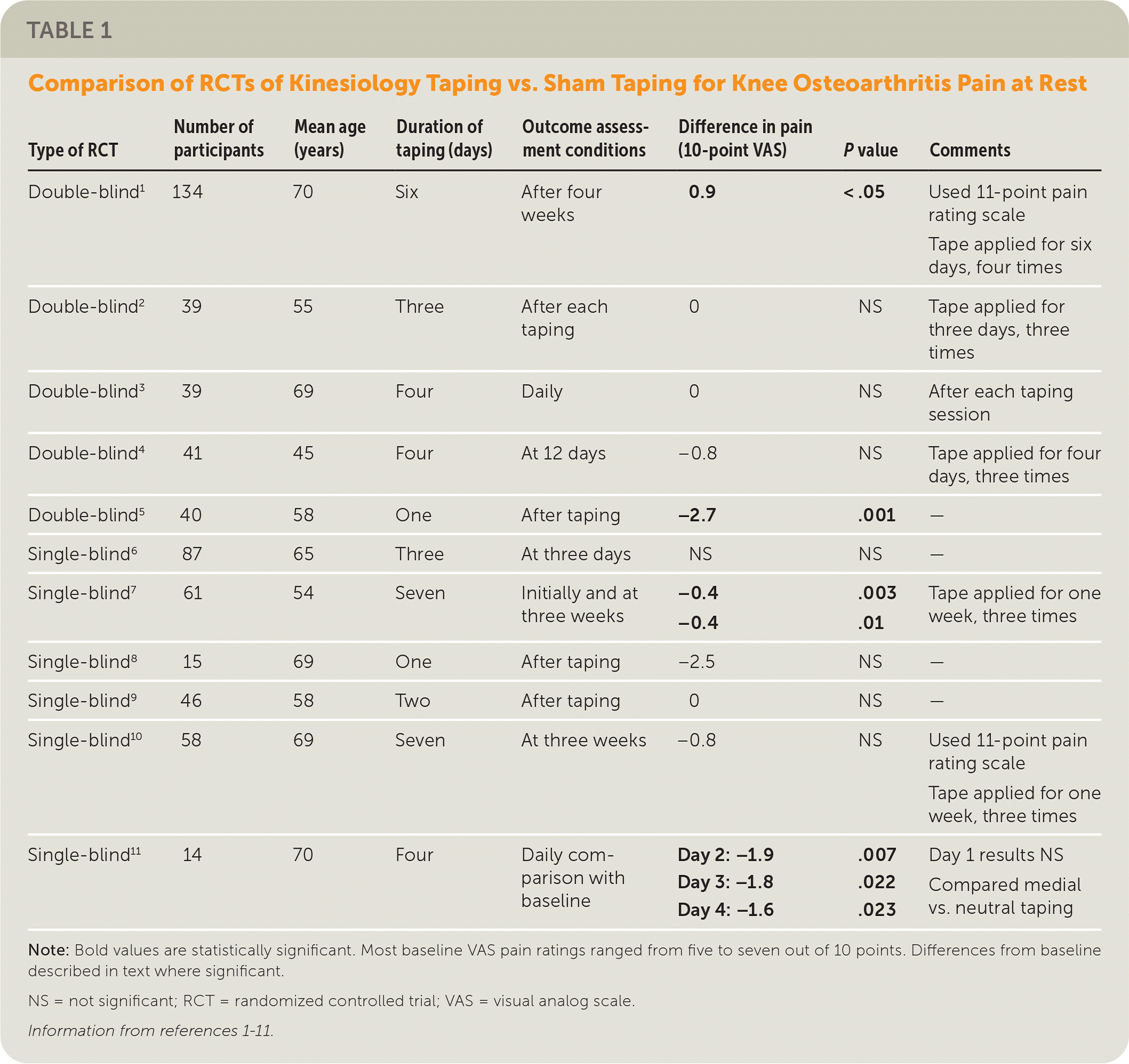
TABLE 1. Comparison of RCTs of Kinesiology Taping vs. Sham Taping for Knee Osteoarthritis Pain at Rest
| Type of RCT | Number of participants | Mean age (years) | Duration of taping (days) | Outcome assessment conditions | Difference in pain (10-point VAS) | P value | Comments |
|---|---|---|---|---|---|---|---|
| Double-blind1 | 134 | 70 | Six | After four weeks | 0.9 | < .05 | Used 11-point pain rating scale Tape applied for six days, four times |
| Double-blind2 | 39 | 55 | Three | After each taping | 0 | NS | Tape applied for three days, three times |
| Double-blind3 | 39 | 69 | Four | Daily | 0 | NS | After each taping session |
| Double-blind4 | 41 | 45 | Four | At 12 days | −0.8 | NS | Tape applied for four days, three times |
| Double-blind5 | 40 | 58 | One | After taping | −2.7 | .001 | — |
| Single-blind6 | 87 | 65 | Three | At three days | NS | NS | — |
| Single-blind7 | 61 | 54 | Seven | Initially and at three weeks | −0.4 −0.4 | .003 .01 | Tape applied for one week, three times |
| Single-blind8 | 15 | 69 | One | After taping | −2.5 | NS | — |
| Single-blind9 | 46 | 58 | Two | After taping | 0 | NS | — |
| Single-blind10 | 58 | 69 | Seven | At three weeks | −0.8 | NS | Used 11-point pain rating scale Tape applied for one week, three times |
| Single-blind11 | 14 | 70 | Four | Daily comparison with baseline | Day 2: −1.9 Day 3: −1.8 Day 4: −1.6 | .007 .022 .023 | Day 1 results NS Compared medial vs. neutral taping |
Note: Bold values are statistically significant. Most baseline VAS pain ratings ranged from five to seven out of 10 points. Differences from baseline described in text where significant.
NS = not significant; RCT = randomized controlled trial; VAS = visual analog scale.
Two double-blind trials1,5 (n = 174) found that kinesiology taping reduced pain scores by 0.9 and 2.7 points (13% and 36%), respectively, adjusted to a VAS 10-point scale, and three of the double-blind trials2–4 (n = 119) found that kinesiology taping produced no difference in VAS pain scores. Four of the single-blind trials6,8–10 (n = 206) found that kinesiology taping did not reduce pain significantly, whereas two trials7,11 (n = 75) found that it reduced pain scores by 0.4 and an average of 1.8 points (8% and baseline VAS not supplied), respectively. Several trials evaluated pain scores for up to a month after the interventions were discontinued, and no trial found persistent pain reductions once the taping was removed. A few patients reported skin irritation from the tape adhesive but described no other adverse effects. A potential weakness in blinding for all studies was that kinesiology taping involves application to the skin with tension whereas sham taping does not. If study participants were aware of this, they could potentially perceive the difference between the dynamic force of kinesiology taping and the tension-free sham taping.
Recommendations from Others
A 2011 Royal Australian College of General Practitioners guideline for nondrug interventions for knee osteoarthritis recommended taping, although they did not specify kinesiology taping, with other strategies such as exercise and weight loss to reduce pain. They also encouraged participation in land-based and aquatic resistance programs.12 The guideline speculated that taping may benefit patients even without applying appreciable force, perhaps by causing sensory changes or a placebo effect.

