A five-year-old child presented for evaluation of midline neck swelling that had been growing slowly for two weeks. The swelling was not painful and did not interfere with swallowing or speech. The child had no injury or trauma to the neck. The swelling had never drained, ruptured, or ulcerated. The child had a history of eczema and mild intermittent asthma that was treated with an albuterol inhaler as needed. The child's mother reported having a similar midline mass that was surgically removed when she was about the same age as the patient.
On physical examination, the swelling measured 5 cm × 3.5 cm in size (Figure 1 and Figure 2). It was nontender, well-circumscribed, smooth, and fluctuant, with mild surface erythema. The lesion elevated with tongue protrusion. Palpation indicated that it was deep to the hypodermis. Examination of the head, eyes, ears, nose, and throat was otherwise unremarkable.
FIGURE 1
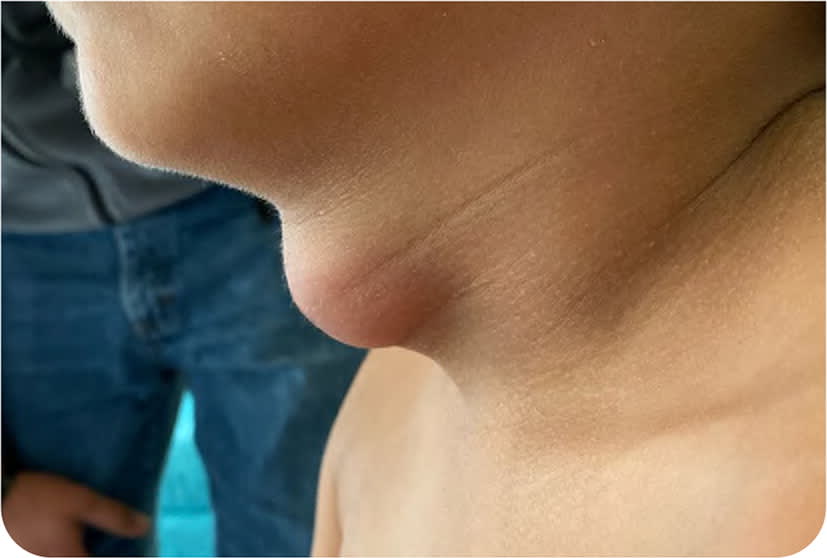
FIGURE 2
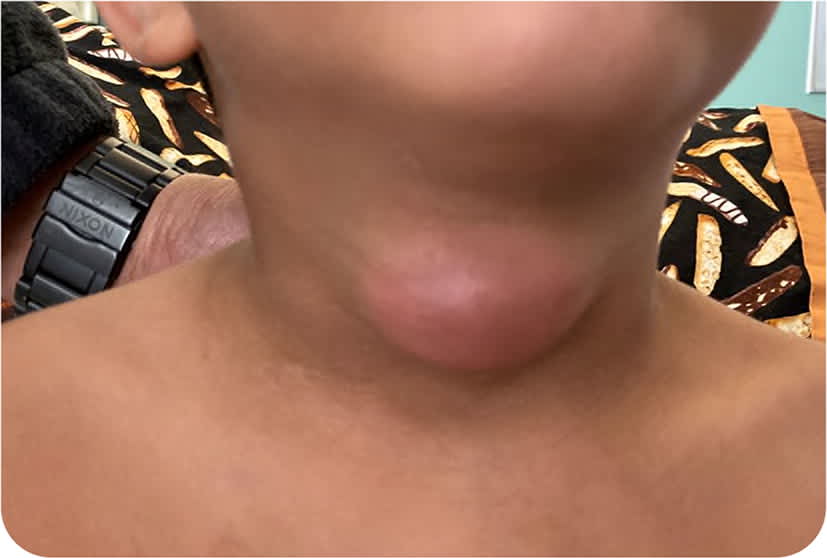
Ultrasonography of the swelling showed a mildly complex hypoechoic lesion anterior to the trachea. The patient's vital signs were normal. The metabolic panel and thyroid studies were within normal limits, but the compete blood count showed an elevated leukocyte level (16,500 per μL [16.50 × 109 per L]).
Question
Based on the patient's history, physical examination, and test findings, which one of the following is the most likely diagnosis?
- A. Infected branchial cleft cyst.
- B. Infected epidermal inclusion cyst.
- C. Infected thyroglossal duct cyst.
- D. Suppurative lymphadenitis.
- E. Thyroid nodule.
Discussion
The answer is C: infected thyroglossal duct cyst. Thyroglossal duct cysts and dermoid cysts are the most common anterior midline neck masses in children.1 Thyroglossal duct cysts are an epithelial remnant of thyroid gland development in the embryo. During the fourth week of gestation, a posterior portion of the tongue migrates down the neck toward the anterior tracheal rings. This thyroglossal tract consists of thyroid tissue and typically atrophies by the 10th week of gestation, leaving the thyroid gland in the anterior midline of the neck. Portions of the thyroglossal tract can persist and become infected, usually following an upper respiratory tract infection. Despite being a common cause of anterior neck masses, thyroglossal cysts are rarely familial.2 Thyroglossal duct cysts elevate with tongue protrusion or swallowing.
Imaging is not initially required in patients with a thyroglossal duct cyst, but a trial of antibiotics for two or three days should be considered if there is suspicion for infection. If there is no improvement, imaging is required to rule out abscess formation and the need for surgical intervention.1 Definitive treatment is surgical removal of the cyst and remaining portions of the tract. There is a low risk of papillary carcinoma within remnants of the tract.3,4
Branchial cleft cysts are an embryonic remnant of the branchial apparatus. Cysts most commonly originate from the first and second branchial cleft and are located anterior to the sternocleidomastoid on the lower third of the neck.1,5 They can be unilateral or bilateral.
Epidermal inclusion cysts occur in the anterior midline neck. They are superficial nodules, usually with a central punctum. Unlike thyroglossal duct cysts, epidermal cysts are stationary even with tongue protrusion.
Suppurative lymphadenitis is most often secondary to infection. The swellings usually present as tender lymph nodes and may be unilateral or bilateral.
Thyroid nodules are a common cause of anterior neck masses, occurring in up to 7% of adults. They are more difficult to detect if less than 1 cm in size.6
SUMMARY TABLE
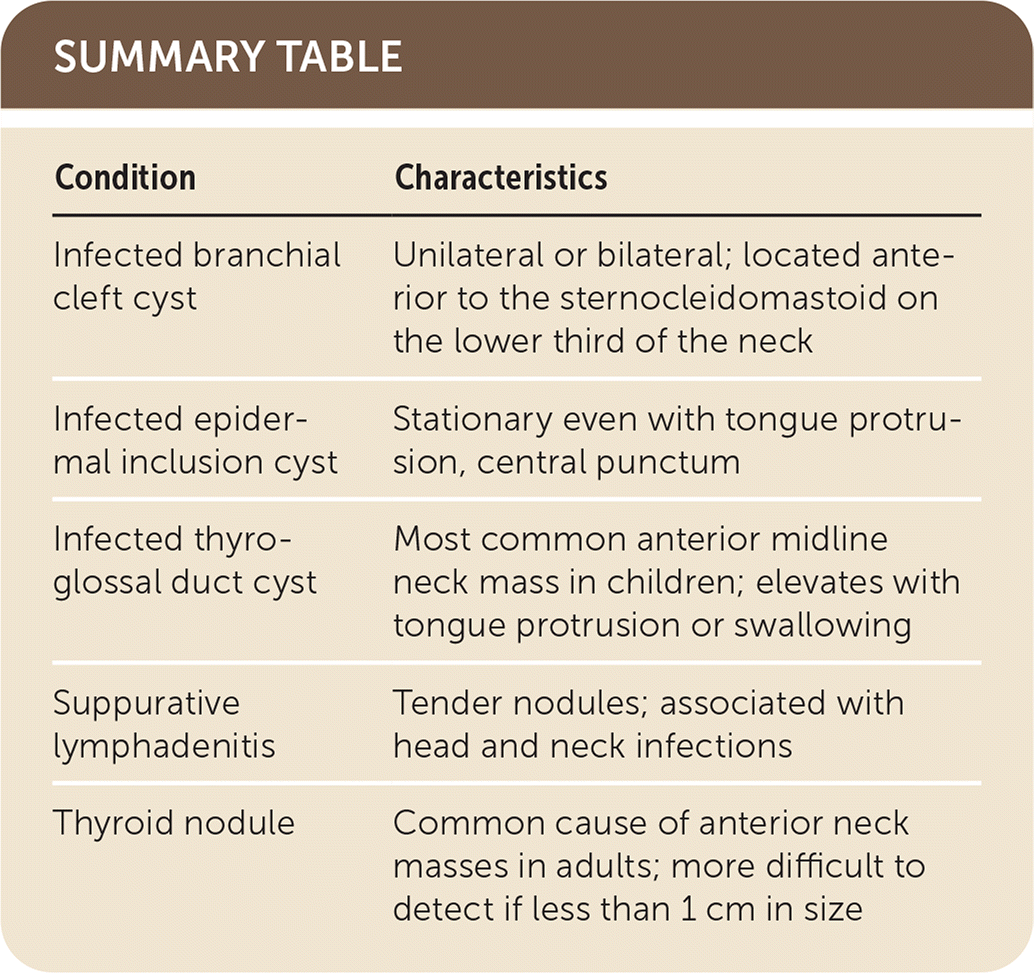
| Condition | Characteristics |
|---|---|
| Infected branchial cleft cyst | Unilateral or bilateral; located anterior to the sternocleidomastoid on the lower third of the neck |
| Infected epidermal inclusion cyst | Stationary even with tongue protrusion, central punctum |
| Infected thyroglossal duct cyst | Most common anterior midline neck mass in children; elevates with tongue protrusion or swallowing |
| Suppurative lymphadenitis | Tender nodules; associated with head and neck infections |
| Thyroid nodule | Common cause of anterior neck masses in adults; more difficult to detect if less than 1 cm in size |

