Unintentional weight loss in people older than 65 years is associated with increased morbidity and mortality. Nonmalignant diseases are more common causes of unintentional weight loss in this population than malignant causes. However, malignancy accounts for up to one-third of cases of unintentional weight loss. Medication use and polypharmacy can interfere with the sense of taste or induce nausea and should not be overlooked as causative factors. Social factors such as isolation and financial constraints may contribute to unintentional weight loss. A readily identifiable cause is not found for 6% to 28% of cases. Recommended tests include age-appropriate cancer screenings, complete blood count, basic metabolic panel, liver function tests, thyroid function tests, C-reactive protein level, erythrocyte sedimentation rate, lactate dehydrogenase measurement, ferritin, protein electrophoresis, and urinalysis. Chest radiography and fecal occult blood testing should be performed. Further imaging and invasive testing may be considered based on initial evaluation. When the initial evaluation is unremarkable, a three- to six-month observation period is recommended with follow-up based on clinician and patient preferences. Treatment should focus on the underlying cause if known. Dietary modifications that consider patient preferences and chewing or swallowing disabilities should be considered. Appetite stimulants and high-calorie supplements are not recommended. Treatment should focus on feeding assistance, addressing contributing medications, providing appealing foods, and social support.
Weight loss in older adults can be intentional or unintentional. Unintentional weight loss in adults older than 65 years is generally defined as a 5% or greater loss of body weight in a six- to 12-month period and is associated with increased morbidity and mortality.1–3 Weight loss can be assessed by numerical documentation or, if no baseline weight is available, corroboration with a change in clothing size or from a relative may be used. The patient or relative should provide an estimate of the weight loss.2,3 Unintentional weight loss in older adults can be classified as unexplained, unintentional weight loss when no definable cause is found or as unintentional weight loss with a known origin.
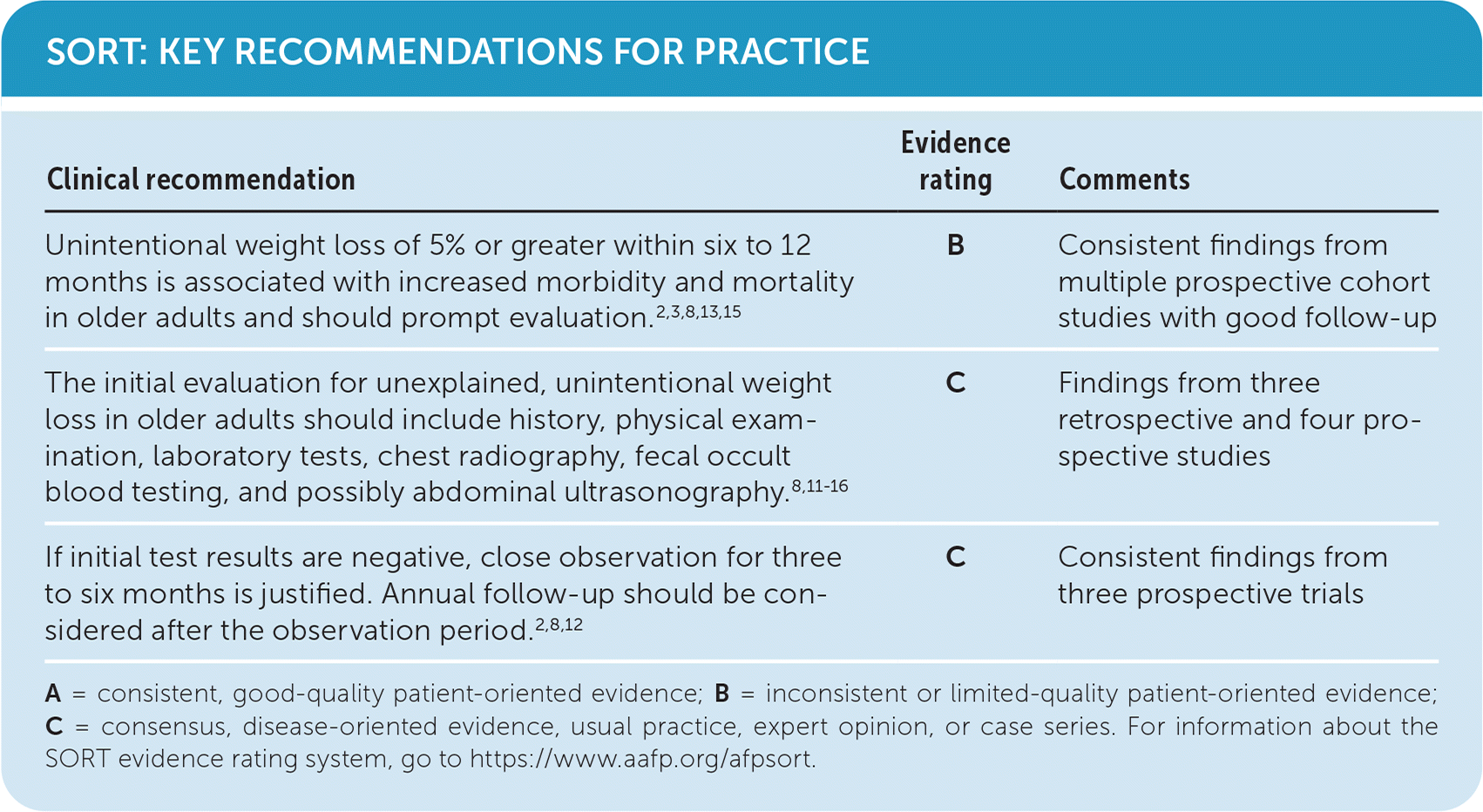
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | Comments |
|---|---|---|
| Unintentional weight loss of 5% or greater within six to 12 months is associated with increased morbidity and mortality in older adults and should prompt evaluation.2,3,8,13,15 | B | Consistent findings from multiple prospective cohort studies with good follow-up |
| The initial evaluation for unexplained, unintentional weight loss in older adults should include history, physical examination, laboratory tests, chest radiography, fecal occult blood testing, and possibly abdominal ultrasonography.8,11–16 | C | Findings from three retrospective and four prospective studies |
| If initial test results are negative, close observation for three to six months is justified. Annual follow-up should be considered after the observation period.2,8,12 | C | Consistent findings from three prospective trials |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
BEST PRACTICES IN GERIATRIC MEDICINE

| Recommendation | Sponsoring organization |
|---|---|
| Avoid using prescription appetite stimulants or high-calorie supplements for the treatment of anorexia or cachexia in older adults; instead, optimize social supports, discontinue medications that may interfere with eating, provide appealing food and feeding assistance, and clarify patient goals and expectations. | American Geriatrics Society |
Source: For more information on the Choosing Wisely campaign, see https://www.choosingwisely.org. For supporting citations and to search Choosing Wisely recommendations relevant to primary care, see https://www.aafp.org/afp/recommendations/search.htm.
Cachexia syndrome is associated with weight loss (greater than 5%) within 12 months attributed to a known chronic illness such as cancer, chronic obstructive pulmonary disease, or chronic kidney disease. To diagnose cachexia syndrome, three of the following characteristics must be present: fatigue, anorexia, low fat-free mass index (amount of muscle mass to height), decreased muscle strength, and abnormal laboratory testing such as low serum albumin levels, anemia, or elevated inflammatory markers.2,4 Challenges in identifying weight loss in older adults include pre-existing obesity and subsequent intentional weight loss from diet and exercise, an expected decline in muscle mass between 50 and 60 years of age, normal daily weight fluctuations, and variations in health care systems' documentation of patient weight.1
Etiologies
The pathophysiology of unintentional weight loss is not well understood. Multiple studies have looked at inflammatory cytokines such as tumor necrosis factor alpha, interleukin-1 beta, interleukin-6, and gut hormones such as cholecystokinin, glucagon-like peptide, and ghrelin.5,6 Although evidence supports that inflammation and inflammatory mediators play a role in weight regulation, the exact mechanism is not understood.7
Body composition and lean body mass decrease with age. Lean body mass can decrease up to 0.7 lb (0.3 kg) per year between 20 and 30 years of age. Fat mass continues to increase until 65 to 70 years of age. Therefore, total body weight usually peaks at 60 years of age with only small decreases after that. The normal reduction in appetite and food intake that occurs with aging should not lead to weight changes substantial enough to be confused with unintentional weight loss.8
Unintentional weight loss in older adults is a diagnostic challenge. There are no validated clinical guidelines, and the differential diagnosis is broad.2 However, once identified, unintentional weight loss should be evaluated. Patients 18 years and older presenting with weight loss are up to 12.5 times more likely than those without weight loss to have cancer. For people older than 60 years, more than one in 10 presenting with weight loss will be diagnosed with cancer. There is an overall risk of 11% to 14% in men and 3% to 7% in women above the normal age-associated cancer risk.1 The lifetime risk of cancer in adults by age is 24.4% (55 to 64 years), 28.2% (65 to 74 years), 18.2% (75 to 84 years), and 8.0% (older than 84 years).9 Weight loss is associated with increased frailty, recurrent falls, and overall worse health outcomes.10
In community-dwelling older adults, unintentional weight loss causes are most often classified as organic or psychosocial. Prospective and retrospective studies in inpatient and outpatient settings have demonstrated that overall non-malignant diseases are more common causes of unintentional weight loss than malignant causes. However, malignancy accounts for up to one-third of cases of unintentional weight loss. After the initial evaluation, the etiologies of unintentional weight loss are malignancy (19% to 36%), with gastrointestinal cancer being the most common, nonmalignant gastrointestinal disease (9% to 45%), and psychosocial disorders (9% to 24%).2,3,11–19 Table 1 lists the common disorders within these broader categories.2,3,12–17 Unintentional weight loss that is unexplained after an initial evaluation ranges from 6% to 28% of cases.2,3,12–16
TABLE 1. Etiologies of Unintentional Weight Loss in Older Adults

| Etiology | Percent |
|---|---|
| Cardiopulmonary 2,3,12 | 2 to 10 |
| Renal disease2,15 | 4 |
| Systemic autoimmune disorders2,13,16 | 4 to 9 |
| Polyarteritis nodosa; polymyalgia rheumatica, rheumatoid arthritis, systemic lupus erythematosus | |
| Endocrine2,12,14,15,17 | 4 to 11 |
| Hyperparathyroidism, thyroiditis, thyrotoxicosis, type 1 or 2 diabetes mellitus | |
| Infectious disease2,13,14 | 4 to 12 |
| HIV, parasitic disease, tuberculosis | |
| Unknown2,3,12–16 | 6 to 28 |
| Neurologic2,15 | 7 to 8 |
| Alcohol-related disease3 | 8 |
| Psychosocial disorders2,12–16 | 9 to 24 |
| Nonmalignant gastrointestinal disease2,3,12–16 | 9 to 45 |
| Colitis; esophageal disorders; malabsorption; mesenteric ischemia; oral, swallowing, or dental problems; peptic ulcer disease | |
| Malignancy 2,3,12–16 | 19 to 36 |
Medication adverse effects and polypharmacy can be factors in unintentional weight loss because both can alter the sense of taste or cause anorexia.2,11,17,20 Table 2 lists adverse effects of commonly used medications.11,16,17
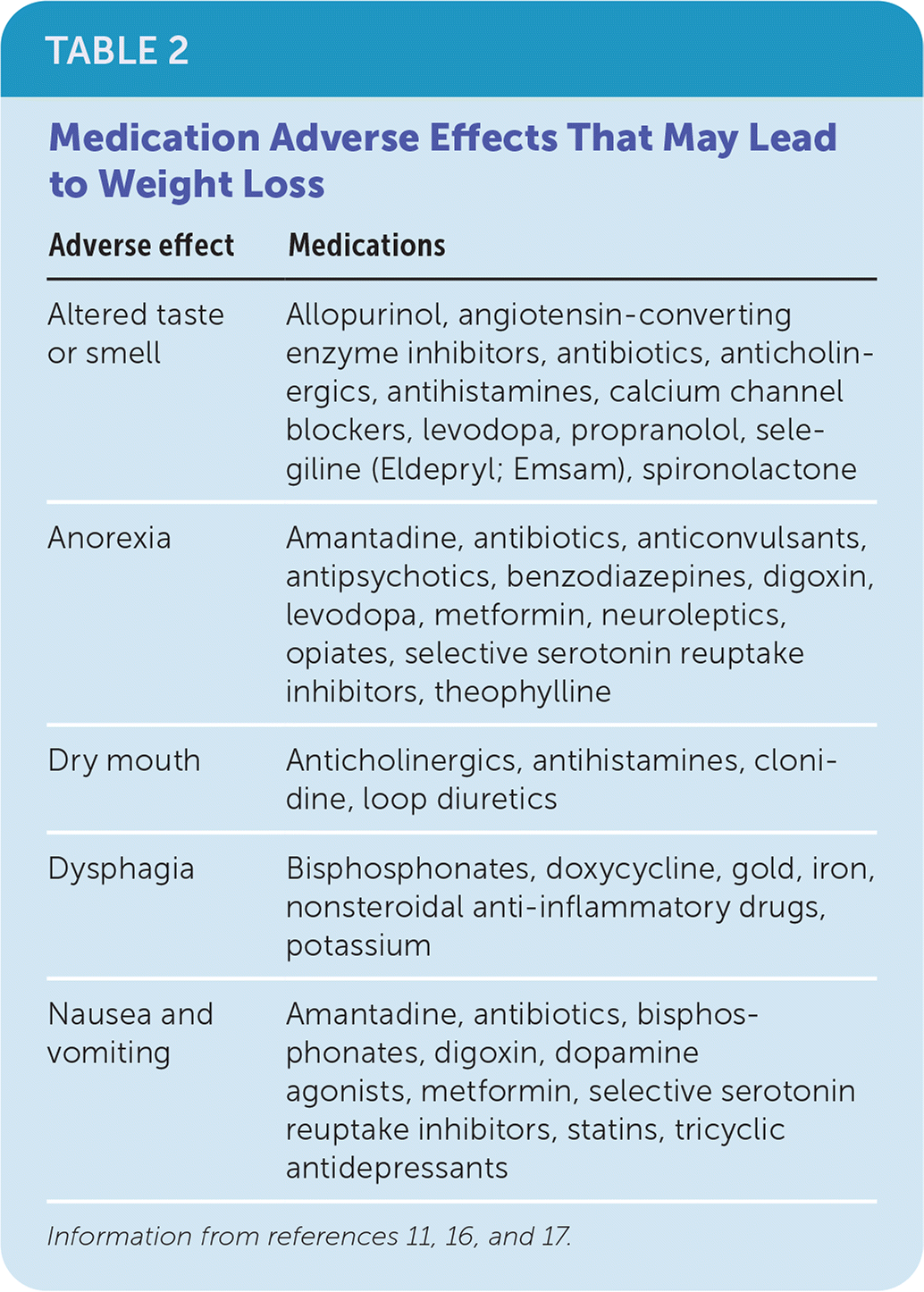
TABLE 2. Medication Adverse Effects That May Lead to Weight Loss
| Adverse effect | Medications |
|---|---|
| Altered taste or smell | Allopurinol, angiotensin-converting enzyme inhibitors, antibiotics, anticholinergics, antihistamines, calcium channel blockers, levodopa, propranolol, selegiline (Eldepryl; Emsam), spironolactone |
| Anorexia | Amantadine, antibiotics, anticonvulsants, antipsychotics, benzodiazepines, digoxin, levodopa, metformin, neuroleptics, opiates, selective serotonin reuptake inhibitors, theophylline |
| Dry mouth | Anticholinergics, antihistamines, clonidine, loop diuretics |
| Dysphagia | Bisphosphonates, doxycycline, gold, iron, nonsteroidal anti-inflammatory drugs, potassium |
| Nausea and vomiting | Amantadine, antibiotics, bisphosphonates, digoxin, dopamine agonists, metformin, selective serotonin reuptake inhibitors, statins, tricyclic antidepressants |
Social factors for unintentional weight loss include alcoholism, financial constraints, and difficulties obtaining food because of impairment in activities of daily living.11 Loss of friends, social groups, and family members can lead to isolation and worsen concomitant depression and loneliness, adding to inadequate nutritional intake.21 The Meals on Wheels and the 9 Ds mnemonics can help in remembering the etiologies of unintentional weight loss (Table 322 and Table 423 ).
TABLE 3. Meals on Wheels Mnemonic for the Etiologies of Unintentional Weight Loss

| M | Medication effects |
| E | Emotional problems (especially depression) |
| A | Anorexia nervosa and alcoholism |
| L | Late-life paranoia |
| S | Swallowing disorders |
| O | Oral factors (poorly fitting dentures and caries) |
| N | No money and nosocomial infections |
| W | Wandering or other dementia-related behaviors |
| H | Hyperthyroidism, hypercalcemia, hypoadrenalism |
| E | Enteric problems |
| E | Eating problems (inability to feed oneself) |
| L | Low-salt and low-cholesterol diets |
| S | Shopping and stones (cholecystitis) |
Adapted with permission from Morely JE. Undernutrition in older adults. Fam Pract. 2012;29(suppl 1):i91.
TABLE 4. 9 Ds Mnemonic for the Etiologies of Unintentional Weight Loss

| Dementia | |
| Dentition | |
| Depression | |
| Diarrhea | |
| Disease (acute and chronic) | |
| Drugs | |
| Dysfunction (functional disability) | |
| Dysgeusia (altered taste) | |
| Dysphagia |
Adapted with permission from Robbins LJ. Evaluation of weight loss in the elderly. Geriatrics. 1989;44(4):34.
Evaluation
A baseline evaluation for unintentional weight loss includes a complete history and physical examination focusing on symptoms that could indicate the cause of weight loss. An article on the comprehensive in-office geriatric assessment published in American Family Physician reviewed tools to assess cognitive impairment, depression, and functional status, all of which can lead to weight loss.24 Medication and supplement use should be reviewed. Nutritional impairment screening can be accomplished using the Mini Nutritional Assessment (https://www.mna-elderly.com).25 Body weight without shoes should be assessed on a clinical scale. Physical examinations should assess any concerning findings from the history and include assessment of the oral cavity and dentition and examination for heart, lung, gastrointestinal, or neurologic abnormalities. Table 5 lists common symptoms, diagnoses, and indicated tests in older adults with unintentional weight loss.26
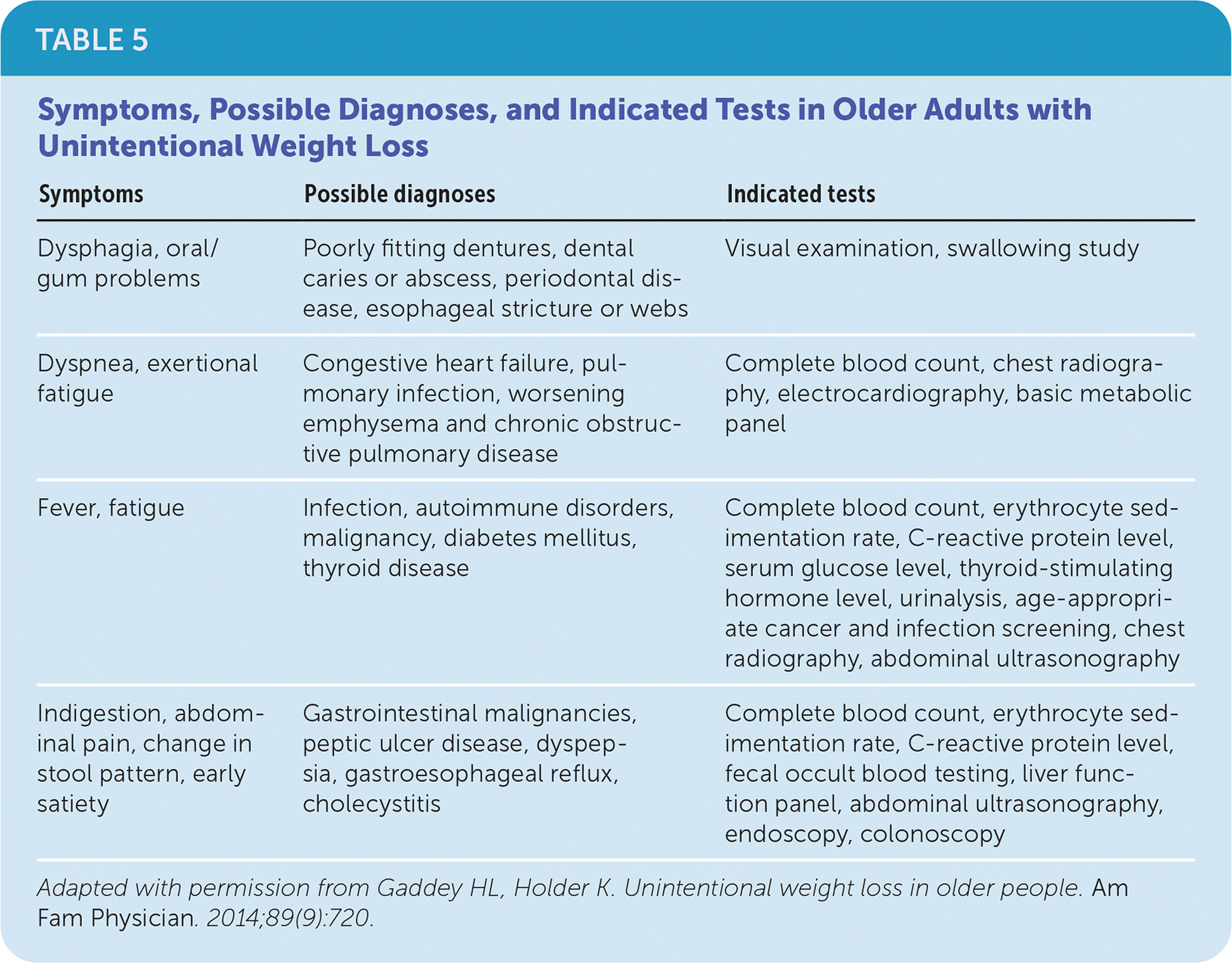
TABLE 5. Symptoms, Possible Diagnoses, and Indicated Tests in Older Adults with Unintentional Weight Loss
| Symptoms | Possible diagnoses | Indicated tests |
|---|---|---|
| Dysphagia, oral/gum problems | Poorly fitting dentures, dental caries or abscess, periodontal disease, esophageal stricture or webs | Visual examination, swallowing study |
| Dyspnea, exertional fatigue | Congestive heart failure, pulmonary infection, worsening emphysema and chronic obstructive pulmonary disease | Complete blood count, chest radiography, electrocardiography, basic metabolic panel |
| Fever, fatigue | Infection, autoimmune disorders, malignancy, diabetes mellitus, thyroid disease | Complete blood count, erythrocyte sedimentation rate, C-reactive protein level, serum glucose level, thyroid-stimulating hormone level, urinalysis, age-appropriate cancer and infection screening, chest radiography, abdominal ultrasonography |
| Indigestion, abdominal pain, change in stool pattern, early satiety | Gastrointestinal malignancies, peptic ulcer disease, dyspepsia, gastroesophageal reflux, cholecystitis | Complete blood count, erythrocyte sedimentation rate, C-reactive protein level, fecal occult blood testing, liver function panel, abdominal ultrasonography, endoscopy, colonoscopy |
Adapted with permission from Gaddey HL, Holder K. Unintentional weight loss in older people. Am Fam Physician. 2014;89(9):720.
Diagnostic Studies
Shared decision-making and goals of care should guide diagnostic evaluation. Initial workup for most patients should include laboratory studies and imaging. Laboratory tests include complete blood count, basic metabolic panel, liver function tests, thyroid function tests, C-reactive protein level, erythrocyte sedimentation rate, glucose measurement, lactate dehydrogenase measurement, protein electrophoresis, ferritin, urinalysis, and fecal occult blood testing. Initial imaging should include chest radiography.2,11 Abdominal ultrasonography may be considered.13 The decision to perform further imaging or more invasive tests should be based on any symptoms or risk factors identified by history and the results of the initial workup.
Low albumin and elevated total white blood cell count, platelets, calcium, or inflammatory markers are most associated with cancer. Although normal laboratory test results may be reassuring, they do not effectively rule out cancer, and further workup should be based on each patient's presentation and evaluation.27
Appropriate follow-up of patients with unexplained, unintentional weight loss is needed if the initial evaluation is unclear. Studies suggested that if the initial evaluation was normal and screening tests were negative, no further workup is needed, and a three- to six-month observation period is warranted.12,13 However, a more recent study with more extensive follow-up (up to 66 months) in 2,677 patients indicated that extended follow-up would result in identifiable causes of weight loss (most often undetected malignancy) and, typically, a diagnosis was found within six to 28 months of the initial evaluation.2 Autopsies were required to establish the diagnosis in 14 patients. The length and frequency of follow-up should be specific to the clinician and patient. Follow-up at least annually is prudent if the initial evaluation does not determine a cause for the unintentional weight loss.2
Treatment
Treatment should focus on the underlying cause and often involves a multidisciplinary team, including dentists; dietitians; speech, occupational, or physical therapists; and social service workers. Common strategies to address unintentional weight loss in older adults are dietary changes, environmental modifications, nutritional supplements, flavor enhancers, and appetite stimulants.28
Decreased saliva production, ill-fitting dentures, periodontal disease, and weakened mastication muscles can lead to poor dentition and impaired chewing.29 A cross-sectional, self-administered study distributed to more than 100,000 community-dwelling older adults in Japan found a significant correlation between having fewer teeth and lower weight in both sexes. Having fewer teeth is associated with more insufficient nutritional intake because of the decreased variety of foods consumed.30 Poor oral health limits the ability to consume foods such as fruits, vegetables, and protein, leading to nutritional deficits.31,32 Diet modification incorporating patient preferences, softer food consistency to accommodate for chewing or swallowing disabilities, and assisted feeding may lead to weight gain and improved laboratory parameters; however, results of this approach are mixed.33–35 Simulating a leisurely in-home dining experience may improve nutrition in nursing home residents.36
According to the Choosing Wisely campaign by the American Geriatrics Society, appetite stimulants and high-calorie supplements should be avoided secondary to lack of evidence on long-term survival and quality of life.37 Treatment should instead focus on feeding assistance, addressing contributing medications, providing appealing foods, and social support as indicated.37 Supplementation, if given, should provide extra calories but not replace scheduled meals and snacks. A Cochrane review of mostly poor-quality studies (N = 10,187) noted that supplementation provides a small but consistent weight gain in older patients; however, there was no statistically significant change in mortality overall. When limited to undernourished patients (n = 2,461), supplementation had a statistically significant mortality benefit (relative risk = 0.79; 95% CI, 0.64 to 0.97). The authors concluded that more studies were needed to assess the effects of supplementation in this population.38
Despite the lack of evidence of benefits and potential harms, appetite stimulants such as megestrol (Megace) and mirtazapine (Remeron) are prescribed. Adverse effects of megestrol include gastrointestinal upset, insomnia, impotence, hypertension, thromboembolic events, and adrenal insufficiency.20,21 Mirtazapine, a serotonin antagonist used to treat depression, has weight gain as a known adverse effect in up to 12% of patients. However, no literature exists solely looking at mirtazapine use for unintentional weight loss. Adverse effects of mirtazapine include dizziness, fatigue, nausea, and somnolence, which can increase fall risk in older adults.21
Data Sources: A PubMed search was completed in clinical queries. Key terms: unintentional weight loss, involuntary, weight loss, geriatrics, elderly, appetite stimulants, cachexia/drug therapy, nutrition, aging, and oral care. The search included meta-analyses, randomized controlled trials, clinical trials, and reviews. Also searched were Agency for Healthcare Research and Quality Effective Healthcare Reports, the Cochrane database, Dynamed, and Essential Evidence Plus. Search dates: December 13, 2020 and April 12, 2021.
The contents of this article are solely the views of the authors and do not necessarily represent the official views of the Uniformed Services University of the Health Sciences, the U.S. Air Force, the U.S. Army, the U.S. Navy, the U.S. military at large, the U.S. Department of Defense, or the U.S. government.

