This article summarizes the top 20 research studies of 2020 identified as POEMs (patient-oriented evidence that matters), including the two most highly rated guidelines of the year on gout and chronic obstructive pulmonary disease (COPD). Regarding COVID-19, handwashing and social distancing through stay-at-home orders or quarantine measures are effective at slowing the spread of illness. Use of proper face masks (not gaiters or bandanas) is also effective at preventing transmission. This is important because the virus can infect others during the presymptomatic phase. Aspirin can no longer be recommended for the primary prevention of cardiovascular disease. Human papillomavirus vaccination is strongly associated with reduced risk of invasive cervical cancer, especially in women who were vaccinated before 17 years of age. When a woman who is postmenopausal has a screening bone mineral density test, rechecking the test after three years does not help to identify those who will have a fragility fracture. A higher daily step count is associated with lower all-cause mortality. After one year of follow-up, physical therapy is preferred to glucocorticoid injections for osteoarthritis of the knee; acetaminophen is ineffective for acute low back pain or pain due to knee or hip osteoarthritis; and adding a muscle relaxant to ibuprofen does not improve functional outcomes or pain in people reporting moderate to severe back pain one week after starting treatment. Although short-term antibiotics and steroids are effective in treating acute exacerbations of COPD, not much else is. Successful communication with patients seeking an antibiotic for a flulike illness can be achieved with combinations of messaging, including information on antibiotic resistance and the self-limiting nature of the illness. A new prediction rule effectively identifies patients with a history of penicillin allergy who have a low likelihood of positive findings on allergy testing. Low-value screening tests in asymptomatic, low-risk patients often lead to further testing, diagnostic procedures, or referrals. A new tool helps determine the amount of change needed to signify a real difference between two laboratory values in the same person over time. Finally, a pillar of our specialty, continuity of care, is associated with decreased all-cause mortality.
Annually for 22 years, a team of clinicians has systematically reviewed English-language medical journals to identify original research most likely to change and improve primary care practice. The team includes experts in family medicine, pharmacology, hospital medicine, and women's health.1,2
The goal of this process is to identify POEMs (patient-oriented evidence that matters). A POEM must report at least one patient-oriented outcome, such as improvement in symptoms, morbidity, or mortality. It should also be free of important methodologic bias, making the results valid and trustworthy. Finally, if applied in practice, the results would change what some physicians do by prompting them to adopt a new practice or discontinue an old one that has been shown to be ineffective or harmful. Adopting POEMs in clinical practice should improve patient outcomes. Of more than 20,000 research studies published in 2020 in the journals reviewed by the POEMs team, 306 met criteria for validity, relevance, and practice change. These POEMs are emailed daily to subscribers of Essential Evidence Plus (Wiley-Blackwell, Inc.).
The Canadian Medical Association purchases a POEMs subscription for its members, many of whom receive the daily POEM. As these physicians read a POEM, they can rate it using a validated questionnaire. This process is called the Information Assessment Method (https://www.mcgill.ca/iam). POEM ratings address the domains of clinical relevance, cognitive impact, use of this information in practice, and expected health benefits if that POEM is applied to a specific patient.3,4 In 2020, each of the 306 daily POEMs was rated by an average of 1,230 physicians.
In this article, we present the 20 most clinically relevant POEMs as rated by Canadian Medical Association members in 2020. This is the 10th installment of our annual series (https://www.aafp.org/afp/toppoems). As we write this article, the pandemic rolls on. However, beyond COVID-19, our patients continue to face the usual (and unusual) health problems of everyday life. Thus, we summarize the clinical question and bottom-line answer for research studies identified as a top 20 POEM, organized by topic and followed by a brief discussion. This set of 20 POEMs includes the two most relevant practice guidelines of the year. The full POEMs are available online at https://www.aafp.org/afp/poems2020.
COVID-19
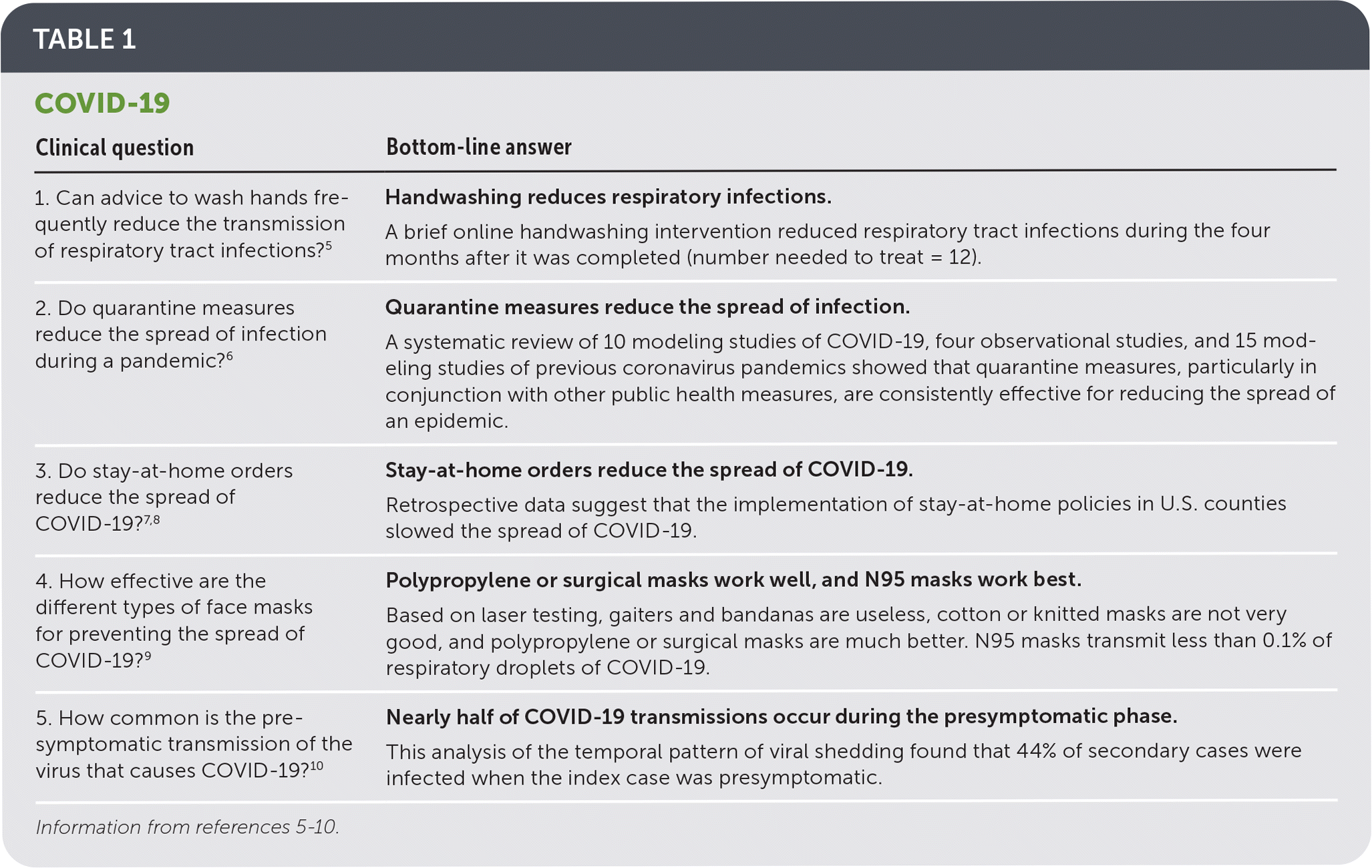
The year 2020 saw the emergence of SARS-CoV-2, a novel coronavirus that causes the COVID-19 illness, and 54 POEMs addressed the epidemiology, diagnosis, treatment, and prognosis of patients with COVID-19. Not surprisingly, the four most highly rated POEMs of the year and five in the top 20 provided evidence regarding preventive measures (Table 1).5–10 These were published early in the pandemic and provided important evidence for family physicians to share with their patients.
TABLE 1. COVID-19
| Clinical question | Bottom-line answer |
|---|---|
| 1. Can advice to wash hands frequently reduce the transmission of respiratory tract infections?5 | Handwashing reduces respiratory infections. |
| A brief online handwashing intervention reduced respiratory tract infections during the four months after it was completed (number needed to treat = 12). | |
| 2. Do quarantine measures reduce the spread of infection during a pandemic?6 | Quarantine measures reduce the spread of infection. |
| A systematic review of 10 modeling studies of COVID-19, four observational studies, and 15 modeling studies of previous coronavirus pandemics showed that quarantine measures, particularly in conjunction with other public health measures, are consistently effective for reducing the spread of an epidemic. | |
| 3. Do stay-at-home orders reduce the spread of COVID-19?7,8 | Stay-at-home orders reduce the spread of COVID-19. |
| Retrospective data suggest that the implementation of stay-at-home policies in U.S. counties slowed the spread of COVID-19. | |
| 4. How effective are the different types of face masks for preventing the spread of COVID-19?9 | Polypropylene or surgical masks work well, and N95 masks work best. |
| Based on laser testing, gaiters and bandanas are useless, cotton or knitted masks are not very good, and polypropylene or surgical masks are much better. N95 masks transmit less than 0.1% of respiratory droplets of COVID-19. | |
| 5. How common is the presymptomatic transmission of the virus that causes COVID-19?10 | Nearly half of COVID-19 transmissions occur during the presymptomatic phase. |
| This analysis of the temporal pattern of viral shedding found that 44% of secondary cases were infected when the index case was presymptomatic. |
The most highly rated POEM was originally published in 2015 and reissued in 2020 after the content was updated for COVID-19. The study was a large pragmatic trial in the United Kingdom that randomized participants to a brief online hand-washing intervention or usual care. Those who completed the intervention had fewer respiratory tract infections over the next four months (51% vs. 59%; P < .001; number needed to treat = 12).5
The next COVID-19 POEM was a Cochrane review.6 The authors reviewed the results of modeling studies of COVID-19 and previous coronavirus pandemics, as well as four observational studies. They concluded that quarantine measures are effective in slowing the spread of infection, especially when implemented early and in conjunction with other public health measures.
The third POEM summarized the results of two ecologic studies. The first compared COVID-19 incidence rates in eight Iowa counties that did not have stay-at-home orders with seven neighboring Illinois counties that had such orders in place.7 The second compared a Georgia county that implemented stay-at-home orders approximately two weeks before the rest of Georgia with seven surrounding counties.8 In both studies, earlier implementation of stay-at-home orders was associated with a lower incidence of COVID-19.
Another POEM summarized the results of one of the earliest studies to evaluate the effectiveness of different kinds of masks for preventing the spread of respiratory droplets.9 Using laser technology, 14 types of masks were evaluated. Gaiters and bandanas were essentially useless, polypropylene and surgical masks were much better, and N95 masks were best.
An important factor in the rapid spread of COVID-19 was transmission by asymptomatic people. One of the first publications to report this was described in the next POEM. Chinese researchers studying infector-infectee transmission pairs found that the peak of infectiousness occurs about one day before symptom onset, and that 44% of secondary cases occur during the presymptomatic period.10 Another study (not among the top 20 POEMs) reviewed cohorts in which the entire group was tested for COVID-19 during an outbreak and found that the rates of asymptomatic or presymptomatic infection are 75% or higher in young adult populations and approximately 40% overall.11
Prevention and Screening
POEMs addressing prevention topics are summarized in Table 2.12–15 The first was a meta-analysis of randomized trials comparing aspirin with placebo as primary prevention. It compared four studies that recruited patients since 2005, with older studies that largely recruited patients in the 1980s and 1990s. The newer studies no longer found that patients taking aspirin for primary prevention have significant reductions in cancer incidence or mortality, cardiovascular mortality, or nonfatal myocardial infarction. Any benefits were countered by harms, such as increased gastrointestinal bleeding.12 Perhaps we are doing a better job of screening for cancer and preventing cardiovascular events through use of statins and antihypertensives, lessening the need for aspirin in prevention.
TABLE 2. Prevention and Screening

| Clinical question | Bottom-line answer |
|---|---|
| 6. Does aspirin still provide a net benefit as primary prevention?12 | Aspirin is no longer recommended for primary prevention. |
| The balance of benefits and harms is equally weighted, so we should no longer recommend aspirin for primary prevention of cancer or cardiovascular disease. The European Society of Cardiology, American College of Cardiology, and American Heart Association agree and no longer recommend aspirin for primary prevention of cardiovascular disease. | |
| 7. Is the daily step count and/ or the intensity of the steps associated with the risk of premature mortality?13 | A higher daily step count is associated with reduced mortality. |
| This study found that a greater number of daily steps is significantly associated with lower all-cause mortality. Step intensity is not significantly associated with mortality after controlling for total daily steps. | |
| 8. Are repeat bone mineral density tests necessary to identify women who are susceptible to fracture?14 | Repeat bone mineral density testing is generally not needed. |
| Rechecking bone mineral density after three years does not add additional prognostic information. In other words, not much changes in three years with regard to estimating fracture risk and, presumably, the need for treatment, so serial testing is not useful. | |
| 9. Is HPV vaccination associated with a lower risk of invasive cervical cancer?15 | HPV vaccination reduces invasive cervical cancer. |
| HPV vaccination is associated with a significant reduction in the likelihood of invasive cervical cancer (adjusted incidence rate ratio = 0.37; 95% CI, 0.21 to 0.57). The magnitude of this reduction was greater in women who were vaccinated before 17 years of age (adjusted incidence rate ratio = 0.12; 95% CI, 0.00 to 0.34). |
HPV = human papillomavirus.
We often tell our patients to walk more, but does walking affect mortality? The next POEM used data from a national sample of U.S. residents whose daily steps were measured between 2003 and 2006.13 All-cause mortality was 77 per 1,000 person-years for those with less than 4,000 steps per day; 21 per 1,000 for those with 4,000 to 7,999 steps per day; 7 per 1,000 for those with 8,000 to 11,999 steps per day; and 4.8 per 1,000 for those with at least 12,000 steps per day. Step intensity was not significantly associated with mortality after controlling for total daily steps. Bottom line? Higher step counts are associated with lower all-cause mortality, suggesting our patients should keep walking.13
When a woman who is postmenopausal has a screening bone mineral density test, the question arises about whether to repeat the test and, if so, how often? The third POEM in this group is a cohort study from the Women's Health Initiative, which showed that information gained from a second test three years after the first does not add predictive value beyond the first test result. Because bone density changes little over time, one bone mineral density test at around 65 years of age is likely to be sufficient for the purpose of screening to prevent a fragility fracture.14
Studies have shown that human papillomavirus (HPV) vaccination can reduce the likelihood of precancerous abnormalities identified on a Papanicolaou (Pap) test. The next POEM is a Swedish study that used data from a national health registry to compare the risk of invasive cervical cancer in 527,871 vaccinated women vs. 1,145,112 unvaccinated women.15 After adjusting for differences between groups, the incidence rate ratio (IRR; the ratio of the incidence of cancer in vaccinated people to that in unvaccinated people) for invasive cervical cancer was 0.37 (95% CI, 0.21 to 0.57). For women who were vaccinated before 17 years of age, the IRR was only 0.12 (95% CI, 0.00 to 0.34), whereas for those vaccinated between 17 and 30 years of age, the IRR was 0.47 (95% CI, 0.27 to 0.75). HPV vaccination is strongly associated with a lower risk of invasive cervical cancer, especially when given early.
Musculoskeletal
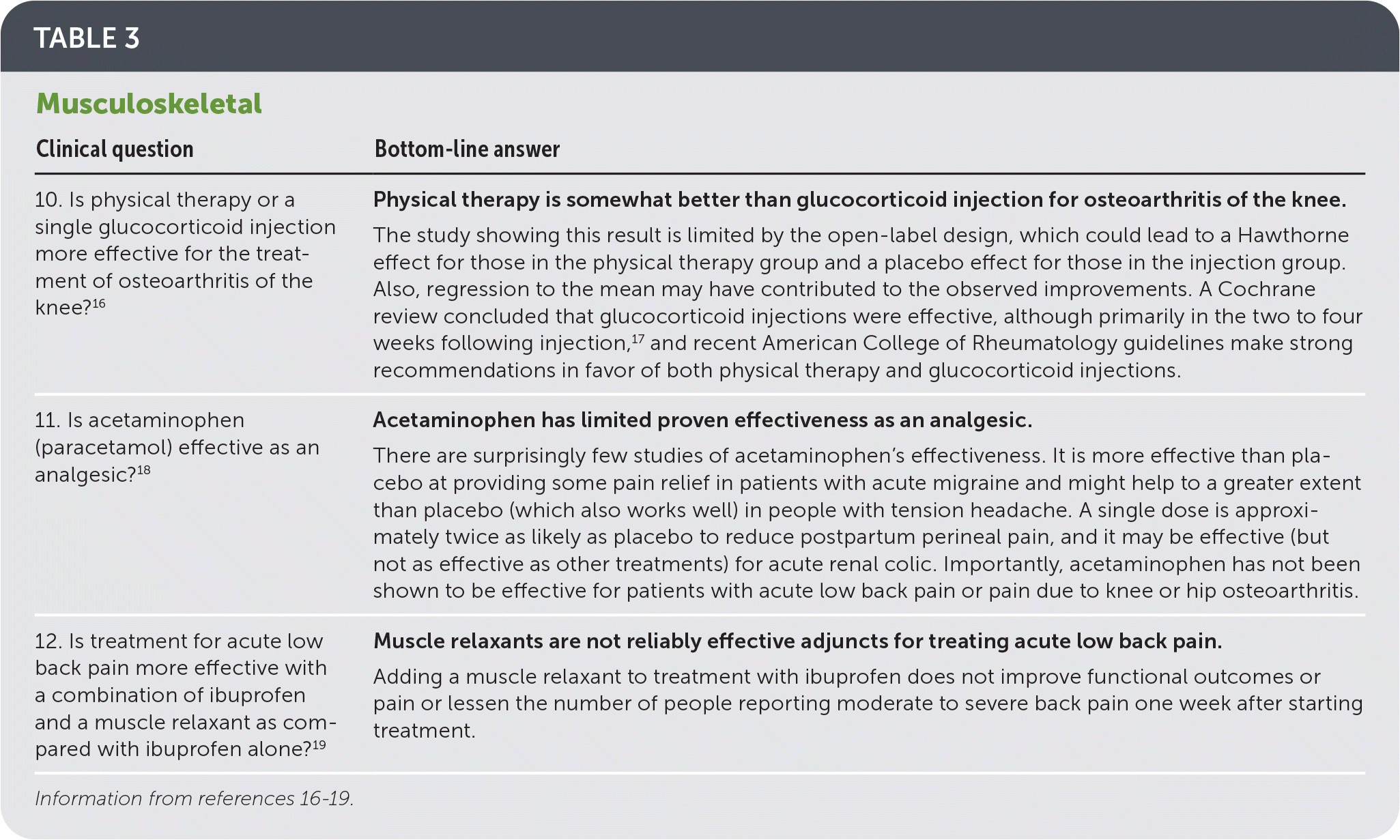
Three POEMs addressing musculoskeletal topics are summarized in Table 3.16–19 The first is a study that randomized adults with knee osteoarthritis to up to three corticosteroid injections or up to eight physical therapy sessions in the first six weeks, with additional sessions as needed.16 The rapid and large improvement in the first month for both groups is somewhat surprising, with relatively little further improvement the rest of the year. This suggests regression to the mean may have contributed to the observed improvement (i.e., patients were identified when their arthritis was flaring up and would have improved no matter what). Also, the open-label design may have contributed to a Hawthorne effect (alteration of behavior by the participants of a study who know they are being observed) for those in the physical therapy group and a placebo effect for those in the injection group. A Cochrane review concluded that glucocorticoid injections are effective, although primarily in the two to four weeks following injection.17 Overall, the physical therapy group did better at one year, with continued improvement, whereas the injection group plateaued after the first month.16
TABLE 3. Musculoskeletal
| Clinical question | Bottom-line answer |
|---|---|
| 10. Is physical therapy or a single glucocorticoid injection more effective for the treatment of osteoarthritis of the knee?16 | Physical therapy is somewhat better than glucocorticoid injection for osteoarthritis of the knee. |
| The study showing this result is limited by the open-label design, which could lead to a Hawthorne effect for those in the physical therapy group and a placebo effect for those in the injection group. Also, regression to the mean may have contributed to the observed improvements. A Cochrane review concluded that glucocorticoid injections were effective, although primarily in the two to four weeks following injection,17 and recent American College of Rheumatology guidelines make strong recommendations in favor of both physical therapy and glucocorticoid injections. | |
| 11. Is acetaminophen (paracetamol) effective as an analgesic?18 | Acetaminophen has limited proven effectiveness as an analgesic. |
| There are surprisingly few studies of acetaminophen's effectiveness. It is more effective than placebo at providing some pain relief in patients with acute migraine and might help to a greater extent than placebo (which also works well) in people with tension headache. A single dose is approximately twice as likely as placebo to reduce postpartum perineal pain, and it may be effective (but not as effective as other treatments) for acute renal colic. Importantly, acetaminophen has not been shown to be effective for patients with acute low back pain or pain due to knee or hip osteoarthritis. | |
| 12. Is treatment for acute low back pain more effective with a combination of ibuprofen and a muscle relaxant as compared with ibuprofen alone?19 | Muscle relaxants are not reliably effective adjuncts for treating acute low back pain. |
| Adding a muscle relaxant to treatment with ibuprofen does not improve functional outcomes or pain or lessen the number of people reporting moderate to severe back pain one week after starting treatment. |
The next POEM is a systematic review of randomized controlled trials of acetaminophen compared with placebo for pain relief in adults.18 It showed that acetaminophen is more effective than placebo in providing some pain relief in patients with acute migraine and might be more beneficial than placebo (which also works well) for tension headaches. A single dose of acetaminophen is about twice as likely as placebo to reduce postpartum perineal pain, and it may be effective (but not as effective as other treatments) for acute renal colic. Importantly, acetaminophen is ineffective for patients with acute low back pain or pain due to knee or hip osteoarthritis.
The last POEM in this category addresses a drug class often prescribed for back pain. In people with moderate to severe low back pain who are taking a nonsteroidal anti-inflammatory drug, such as ibuprofen (up to 600 mg three times per day), does the addition of a muscle relaxant improve function or reduce pain? No.19 This finding reminds us of an earlier randomized controlled trial from the same author that was a top POEM of 2015. At that time, we advised not adding cyclobenzaprine to naproxen for patients with acute low back pain.20
Respiratory
Two top POEMs on respiratory topics are summarized in Table 4.21,22 One is a meta-analysis of randomized controlled trials of treatment in patients with an exacerbation of chronic obstructive pulmonary disease.21 This shows that antibiotics and corticosteroids are effective in treating acute exacerbations in outpatient and inpatient settings, regardless of the severity of the exacerbation. Current research does not provide good guidance on which antibiotic is best or on the optimal dose or duration of corticosteroid treatment. Notably, studies performed in critically ill patients were not included in this analysis.
TABLE 4. Respiratory

| Clinical question | Bottom-line answer |
|---|---|
| 13. Which treatments are effective for patients with an exacerbation of COPD?21 | Antibiotics and corticosteroids improve exacerbations of COPD. |
| Short-term antibiotic treatment and short-term systemic corticosteroids are both associated with a faster resolution of COPD symptoms and fewer treatment failures. Other treatment approaches do not help. | |
| 14. What is the most effective message to reduce antibiotic-seeking behavior for respiratory tract infections?22 | Messaging/counseling reduces antibiotic-seeking behavior for acute respiratory tract infections. |
| When talking to patients about antimicrobial resistance, it is important to combine a fear-based message (e.g., resistance is increasing, antibiotics may not be there for you when you really need them) with empowering information (e.g., antibiotics are not helpful, these infections are self-limited but may last a couple of weeks, there are many other things you can do to feel better). It may also be helpful for physicians to avoid the term “acute bronchitis” and instead say “chest cold,” which sounds much less frightening to patients. |
COPD = chronic obstructive pulmonary disease.
The other POEM addresses the tricky issue of communicating with patients who appear to be seeking an antibiotic for a flulike illness. It is a randomized trial conducted online in the United Kingdom showing that patients receiving the combination of a fear-based message about increased antibiotic resistance and an empowering message are less likely to visit a physician for their next respiratory tract infection (45.1% to 46.1% vs. 29.2%; P < .001) and less likely to request an antibiotic (52.5% to 54.7% vs. 42.3%; P < .001) than those receiving only fear-based messaging.22
Miscellaneous
Four top POEMs do not fall easily into a single category (Table 5).23–26 The first is about a new clinical prediction rule to identify patients who report a penicillin allergy but are unlikely to have a true allergy if tested. The FAST rule is as follows—five years or less since the reaction: 2 points; anaphylaxis, angioedema, or severe cutaneous reaction: 2 points; treatment required for reaction: 1 point. Patients with a score of 0 have a less than 1% likelihood of a positive result on allergy testing, and those with a score of 1 or 2 have a 5% likelihood.23
TABLE 5. Miscellaneous

| Clinical question | Bottom-line answer |
|---|---|
| 15. Which adult patients with penicillin allergy by history will have positive results on allergy testing?23 | The FAST prediction rule helps determine true allergy to penicillin. |
| A label of “penicillin allergy” clears the shelves of many effective treatments for various infections. The FAST rule is as follows—five years or less since the reaction: 2 points; anaphylaxis, angioedema, or severe cutaneous reaction: 2 points; treatment required for reaction: 1 point. Patients with a score of 0 had a less than 1% likelihood of a positive result on allergy testing, and those with a score of 1 or 2 had a 5% likelihood. | |
| 16. Are chest radiography, electrocardiography, and Pap tests in low-risk patients associated with subsequent additional health care?24 | In routine health evaluations, chest radiography and electrocardiography do not improve outcomes and may lead to harm. |
| Low-value tests (that is, screening tests in low-risk patients), such as chest radiography and electrocardiography in adults as part of an annual health examination and Pap tests in women younger than 21 years or older than 69 years, are associated with more visits to specialists, more diagnostic tests, and more procedures. | |
| 17. How much variation is there in clinical laboratory values, and how should we account for it?25 | Both analytic and physiologic variables may lead to variations in laboratory test results independent of treatment effects. |
| “The numbers don't lie.” How many times have you said that to yourself or to a patient? Although numbers may not lie, they may not tell the whole truth. For example, a single A1C test result of 6.3% (810.81 mg per dL [45 mmol per mol]) could be as low as 5.5% (702.70 mg per dL [39 mmol per mol]) or as high as 7.1% (918.92 mg per dL [51 mmol per mol]). This range is due to the inherent variability in the analytic process, as well as to biologic variability (i.e., the variation in the same person over the course of days caused by physiologic changes). As a result, it is hard to tell if a change in a blood level over time is real or just a reflection of these sources of variability. Bookmark this website: https://www.bmj.com/content/368/bmj.m149. It is a tool that determines the variability that can be expected in a single laboratory value and calculates the reference change value needed to signify a real difference between the values in the same person over time. | |
| 18. Is continuity of care associated with decreased mortality?26 | Continuity of care is associated with lower mortality. |
| Most studies in this systematic review found that greater primary care continuity was associated with lower all-cause mortality. |
Pap = Papanicolaou.
The COVID-19 pandemic upended medical practice, leading to large reductions in the use of health care services. For example, the Canadian Urological Association recommended the cessation of prostate-specific antigen screening for prostate cancer until the resolution of the pandemic.27 In this context, the next POEM reminds us to avoid low-value screening tests in asymptomatic, low-risk patients because they often lead to further testing, diagnostic procedures, or referrals.24 Specifically, screening tests in low-risk patients, such as chest radiography and electrocardiography in adults as part of an annual health examination and Pap tests in those younger than 21 years or older than 69 years, should be avoided.
How many patients still ask for annual blood tests despite physicians counseling them on the low yield for doing this? The next POEM was the top non–COVID-related POEM of 2020 for clinical relevance.25 This POEM describes a new online tool (https://www.bmj.com/content/368/bmj.m149) to illustrate the variability in a single laboratory value (such as the A1C test) and the amount of change needed to signify a real difference between two values in the same person over time. For example, given the variability inherent in total cholesterol measurements, it is difficult to detect a clinically important change within a one-year period.
Our final miscellaneous POEM is a systematic review of the value of a pillar of family medicine—personal continuity of care. This is defined by an ongoing relationship with a physician that builds the physician-patient relationship and promotes the healing power of interactions. This core principle of family medicine stands up to scientific scrutiny by demonstrating an associated reduction in mortality.26
Practice Guidelines
POEMs sometimes summarize high-impact clinical practice guidelines. Key messages from the two highest rated guidelines, addressing gout and chronic obstructive pulmonary disease, are summarized in Table 6.28,29
TABLE 6. Practice Guidelines

| Clinical question | Bottom-line answer |
|---|---|
| 19. How should clinicians manage patients with gout?28 | Allopurinol is the preferred first-line agent to lower serum urate; colchicine, NSAIDs, or glucocorticoids should be used for gout flare-ups. |
| The following are some of the strong recommendations from the ACR for managing patients with gout: | |
| Start urate-lowering therapy for all patients with tophi, frequent gout flare-ups (two or more per year), or radiographic evidence of joint damage attributable to gout. | |
| Use allopurinol as the preferred first-line medication, including for patients with stage 3 or worse chronic kidney disease. | |
| Treat patients to a serum urate target of less than 6 mg per dL (0.36 mmol per L). | |
| When initiating urate-lowering therapy, the ACR strongly recommends concomitant anti-inflammatory prophylactic therapy for at least three to six months. | |
| The ACR strongly recommends using colchicine, NSAIDs, or glucocorticoids (oral, intra-articular, or intramuscular) to manage gout flare-ups. | |
| 20. What is the optimal approach to the pharmacologic management of patients with COPD?29 | Treat COPD with a long-acting beta agonist and long-acting muscarinic antagonist; add inhaled corticosteroids in selected patients. |
| Patients with COPD should be treated with a combination of a long-acting beta agonist and long-acting muscarinic antagonist. | |
| The ATS makes conditional recommendations for the addition of inhaled corticosteroids to dual therapy in patients with ongoing dyspnea and exacerbation, and for the withdrawal of the inhaled corticosteroids after one year in patients who do well. | |
| The ATS makes no recommendation for or against the use of inhaled corticosteroids in patients with eosinophilia. | |
| The ATS makes conditional recommendations against the use of oral steroids in patients with severe and frequent exacerbations and for the use of opioids in patients with advanced refractory dyspnea despite optimal therapy. |
ACR = American College of Rheumatology; ATS = American Thoracic Society; COPD = chronic obstructive pulmonary disease; NSAID = nonsteroidal anti-inflammatory drug.
The full text of the POEMs discussed in this article is available at https://www.aafp.org/afp/poems2020.
A list of top POEMs from previous years is available at https://www.aafp.org/afp/toppoems.
Editor's Note: This article was cowritten by Dr. Mark Ebell, deputy editor for evidence-based medicine for AFP and cofounder and editor-in-chief of Essential Evidence Plus, published by Wiley-Blackwell, Inc. Because of Dr. Ebell's dual roles and ties to Essential Evidence Plus, the concept for this article was independently reviewed and approved by a group of AFP's medical editors. In addition, the article underwent peer review and editing by three of AFP's medical editors. Dr. Ebell was not involved in the editorial decision-making process.—Sumi Sexton, MD, Editor-in-Chief
The authors thank Wiley-Blackwell, Inc., for giving permission to excerpt the POEMs; Drs. Allen Shaughnessy, Henry Barry, David Slawson, Nita Kulkarni, and Linda Speer for selecting and writing the original POEMs; the academic family medicine fellows and faculty of the University of Missouri–Columbia for their work as peer reviewers; Joulé, Inc., for supporting the POEMs CME program in Canada; Pierre Pluye, PhD, for codeveloping the Information Assessment Method; and Maria Vlasak for her assistance with copyediting the POEMs.

