Complex regional pain syndrome (CRPS) is a rare, chronic pain disorder. It is challenging for patients and physicians because it leads to significant morbidity due to chronic pain that may last for years. CRPS typically develops four to six weeks after direct trauma, such as an injury or surgery, and causes pain that is out of proportion to the inciting injury. It is associated with multiple physiologic mechanisms, affecting skin texture or localized sensory, motor, sudomotor, and vasomotor pathways. The diagnosis is made clinically using standardized diagnostic criteria. Ancillary testing is not necessary for the diagnosis of CRPS but can be useful to rule out alternative diagnoses. There are two types of CRPS, type 1 and type 2, although treatment is the same for both. There is no single proven treatment modality for CRPS, and there have been no large randomized controlled studies of CRPS treatments. Most treatments are based on studies of their use for other types of neuropathic pain. The mainstay of treatment is to improve function of the affected body part and to decrease pain; therefore, treatment requires multiple modalities, including medications, behavioral health interventions, and referral to a pain specialist.
Complex regional pain syndrome (CRPS) is a rare, chronic pain disorder. CRPS is challenging for patients and physicians because it leads to significant morbidity due to chronic pain that can last years. CRPS typically develops four to six weeks after direct trauma, such as an injury (e.g., fracture) or surgery.1 Many treatment recommendations for CRPS are based on smaller studies or consensus guidelines and on practice. Although most cases of CRPS resolve spontaneously without treatment,2 the pain, associated symptoms, psychological impact, and disability require a well-informed, patient-centered approach.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
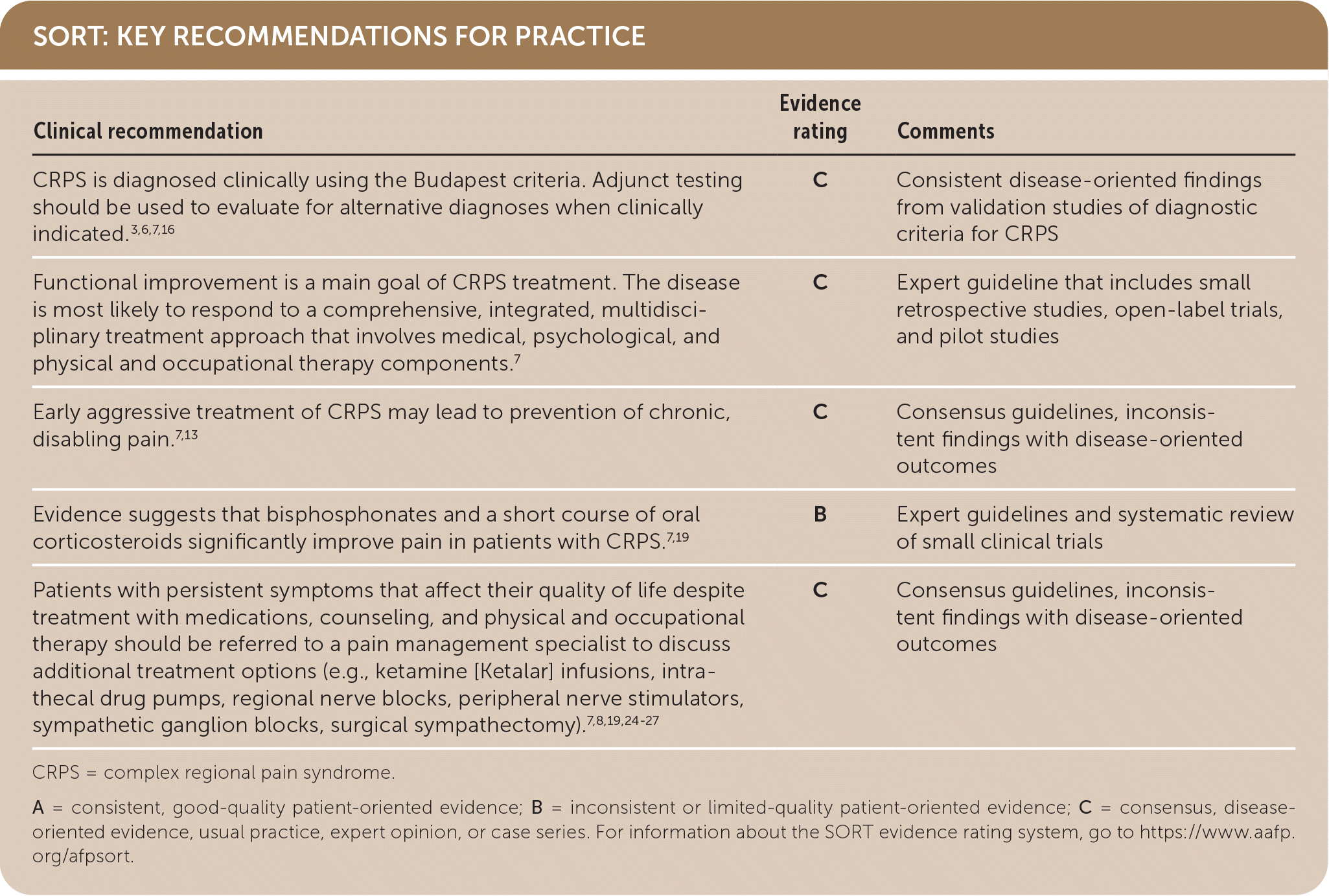
CRPS = complex regional pain syndrome.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Epidemiology
CRPS is three or four times more common in women than in men, and the peak age of onset is between 50 and 70 years.2–4 Few studies have looked closely at the incidence of the disease, and most data are from retrospective reviews of medical databases. These reviews estimate that the incidence of CRPS is five to 26 per 100,000 people per year.2 Because diagnostic criteria have been revised over time across multiple specialties, the reported incidence may be underestimated.1,3 Research has shown that among patients with fracture, the incidence of CRPS is anywhere from 0.05% to 0.2% in older studies and 3% to 7% in more recent studies, although the diagnostic criteria varied.5
Because of the variety of symptoms and fluctuation of symptom severity over time, symptoms of CRPS may be attributed to malingering or somatization. However, no psychological or personality traits have been shown to predispose an individual to CRPS.6 Although comorbid Axis I disorders, especially major depression, are present in up to 49% of patients with CRPS, there is no evidence that comorbid psychiatric disorders are more common in those with CRPS compared with other patients who have chronic pain.7
Pathophysiology
CRPS has been subdivided into reflex sympathetic dystrophy (type 1) or causalgia (type 2). Type 1 CRPS accounts for 90% of cases and begins after an injury with no nerve involvement on nerve conduction testing. Confirmation of nerve injury on nerve conduction testing is the defining feature of type 2 CRPS.7 Both types are treated similarly.
The pathogenesis of CRPS is poorly understood, and although many causal mechanisms have been postulated, it is likely multifactorial. It is unclear why most cases of CRPS develop after an injury, but some do not. Possible causal mechanisms include combinations of local inflammatory cascades, direct small fiber nerve injury, dysfunction of the sympathetic nervous system, central pain processing, and emotional responses to painful stimuli.8,9 Some studies also suggest that an autoimmune process plays a role in CRPS.10,11 Genetic factors may be involved, but strong associations have not been identified.12
Clinical Presentation
Initial symptoms of CRPS include pain out of proportion to the inciting injury that is usually described by patients as burning, tingling, stabbing, numbness, or an electric shock1 and is localized to a distal extremity (CRPS rarely develops in other parts of the body). Other symptoms at the site of pain include increased growth of hair or nails (trophic changes), increased sweating, localized swelling, and hyperemia.3 Of CRPS cases, 40% develop after a fracture.5
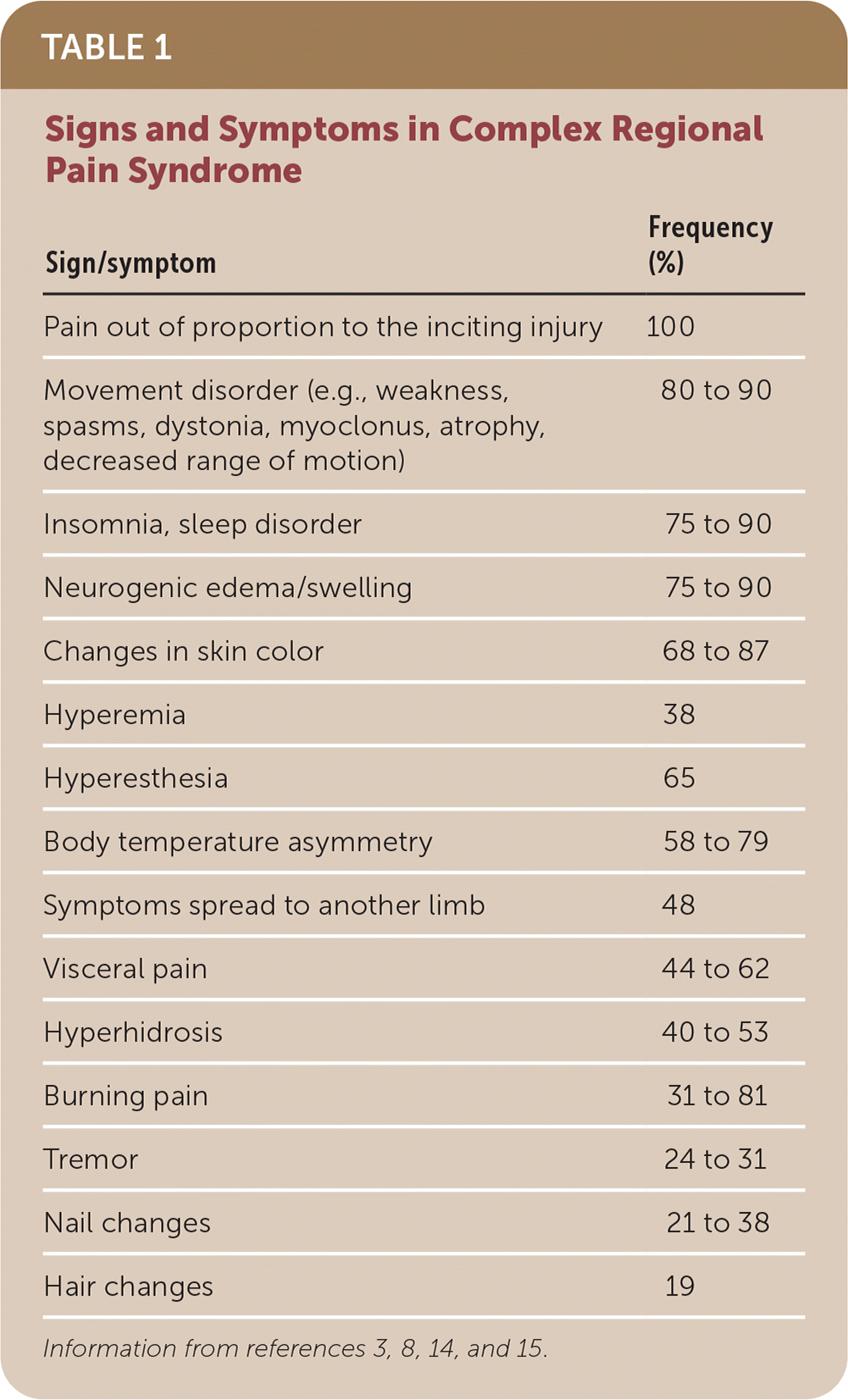
Symptoms typically begin within four to six weeks after the inciting incident, and the pain can last years. Pain associated with CRPS does not correspond to a dermatomal or nerve root distribution and usually is not associated with a specific nerve injury (type 1 CRPS). Many patients with CRPS are unable to use the affected extremity because movement can worsen the pain. The signs and symptoms of CRPS can vary widely between patients and within a disease course.13 Table 1 includes the documented frequency of signs and symptoms in patients with CRPS.3,8,14,15
TABLE 1. Signs and Symptoms in Complex Regional Pain Syndrome
| Sign/symptom | Frequency (%) |
|---|---|
| Pain out of proportion to the inciting injury | 100 |
| Movement disorder (e.g., weakness, spasms, dystonia, myoclonus, atrophy, decreased range of motion) | 80 to 90 |
| Insomnia, sleep disorder | 75 to 90 |
| Neurogenic edema/swelling | 75 to 90 |
| Changes in skin color | 68 to 87 |
| Hyperemia | 38 |
| Hyperesthesia | 65 |
| Body temperature asymmetry | 58 to 79 |
| Symptoms spread to another limb | 48 |
| Visceral pain | 44 to 62 |
| Hyperhidrosis | 40 to 53 |
| Burning pain | 31 to 81 |
| Tremor | 24 to 31 |
| Nail changes | 21 to 38 |
| Hair changes | 19 |
CRPS is often described in terms of “warm” changes and “cold” changes, although they are not separate diagnostic categories. Warm CRPS is associated with a warm, erythematous, edematous extremity and tends to be correlated with inflammatory changes earlier in the disease course; one study described these changes within the first eight months.3 Cold CRPS is associated with a cold, dusky, sweaty extremity and is more often associated with chronic CRPS; in one study, cold symptoms lasted for more than nine months.3 The same extremity can have both warm and cold symptoms, and the disease pattern and clinical course vary among patients.1,7,14
Diagnosis
CRPS is diagnosed clinically, with no standard objective assessment for the diagnosis.3,7,15 The Budapest criteria developed by the International Association for the Study of Pain is 99% sensitive and 68% specific for CRPS, with increased sensitivity as other diagnoses are ruled out.16 These criteria are outlined in Table 2.16 Adjunct testing should be used to evaluate for alternative diagnoses when clinically indicated.6
TABLE 2. Budapest Criteria for the Diagnosis of Complex Regional Pain Syndrome

| Must exhibit continuing pain that is disproportionate to any inciting event |
| Must report at least one symptom in three of the four following categories: |
| Sensory: hyperalgesia or allodynia |
| Vasomotor: temperature asymmetry, skin color changes, or skin color asymmetry |
| Sudomotor/edema: edema and/or sweating changes and/or sweating asymmetry |
| Motor/trophic: decreased range of motion and/or motor dysfunction (weakness, tremor, dystonia) and/ or trophic changes (hair, nails, skin) |
| Must display at least one sign at the time of evaluation in at least two of the following categories: |
| Sensory: hyperalgesia (to pinprick) and/or allodynia (to light touch or deep somatic pressure, or joint movement) |
| Vasomotor: temperature asymmetry and/or skin color changes and/or asymmetry |
| Sudomotor/edema: edema and/or sweating changes and/or sweating asymmetry |
| Motor/trophic: decreased range of motion and/or motor dysfunction (weakness, tremor, dystonia) and/or trophic changes (hair, nails, skin) |
| No other diagnosis better explains the signs and symptoms |
Adapted with permission from Harden RN, Bruehl S, Stanton-Hicks M, et al. Proposed new diagnostic criteria for complex regional pain syndrome. Pain Med . 2007;8(4):330.
Ultrasonography may be used to rule out other diagnoses that can cause unilateral pain, swelling, and changes in skin temperature, such as deep venous thrombosis or arterial ischemia. Other conditions to consider in the differential diagnosis (Table 31,7 ) include gout/pseudogout, tenosynovitis, nerve impingement (e.g., carpal tunnel syndrome), Charcot foot, and cellulitis; these usually can be distinguished from CRPS through the history and physical examination.
TABLE 3. Differential Diagnosis for Complex Regional Pain Syndrome

| Diagnosis | Key distinguishing features |
|---|---|
| Charcot foot | Chronic foot inflammation with classic midfoot deformity, linked with diabetic neuropathy and diabetes mellitus |
| Compartment syndrome | Tense, swollen extremity; pain limited to fascial boundaries |
| Deep venous thrombosis or peripheral arterial obstruction | Positive findings on duplex ultrasonography |
| Diabetic neuropathy | Symmetrical, bilateral lower extremity distribution; concurrent diabetes |
| Gout, pseudogout | Rapid onset; lower extremity pain; crystals in synovial fluid aspiration |
| Nerve impingement | Symptoms limited to nerve distribution |
| Peripheral neuropathy | Symmetrical; confirm with electromyography |
| Postherpetic neuralgia | Dermatomal distribution with shingles rash preceding neuropathic pain |
| Raynaud phenomenon | Sharply demarcated color changes in fingers when exposed to cold |
| Rheumatologic disease | Symmetrical; positive for serum autoantibodies, such as anti–cyclic citrullinated peptide and rheumatoid factor; elevated C-reactive protein level or erythrocyte sedimentation rate |
| Soft tissue infection (cellulitis, osteomyelitis, abscess) | Leukocytosis; elevated C-reactive protein level or erythrocyte sedimentation rate |
| Stress fractures | Gradual progression of activity-related pain, usually after increased activity; positive findings on computed tomography or magnetic resonance imaging |
| Tenosynovitis | Focal tenderness at insertion site; can affect any joint, causing pain, swelling, and redness; linked to injury or overuse of a muscle tendon |
Because bone remodeling has been associated with CRPS, bone scintigraphy with technetium Tc 99m may show evidence of increased bone resorption at the site of symptoms. This test is not useful in clinical practice because it is neither sensitive nor specific for CRPS, and it is not part of the diagnostic criteria for CRPS.17
Treatment
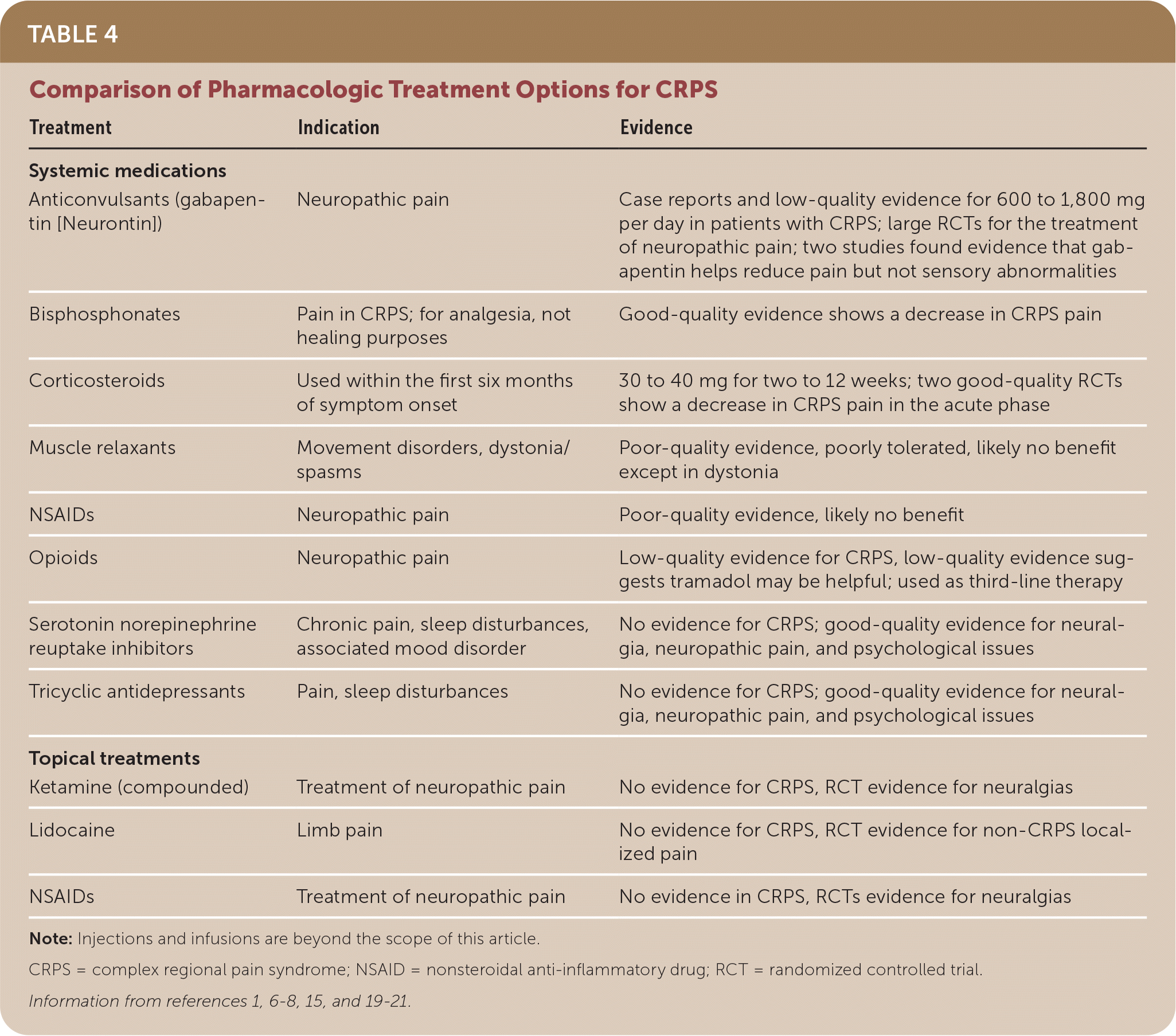
Because the pathophysiology of CRPS is multifactorial, there is no single proven treatment modality. There are no large randomized controlled studies analyzing treatments for CRPS,18 and most treatments are based on studies of their use for other types of neuropathic pain.7 Table 4 includes treatment modalities and indications.1,6–8,15,19–21
TABLE 4. Comparison of Pharmacologic Treatment Options for CRPS
| Treatment | Indication | Evidence |
|---|---|---|
| Systemic medications | ||
| Anticonvulsants (gabapentin [Neurontin]) | Neuropathic pain | Case reports and low-quality evidence for 600 to 1,800 mg per day in patients with CRPS; large RCTs for the treatment of neuropathic pain; two studies found evidence that gabapentin helps reduce pain but not sensory abnormalities |
| Bisphosphonates | Pain in CRPS; for analgesia, not healing purposes | Good-quality evidence shows a decrease in CRPS pain |
| Corticosteroids | Used within the first six months of symptom onset | 30 to 40 mg for two to 12 weeks; two good-quality RCTs show a decrease in CRPS pain in the acute phase |
| Muscle relaxants | Movement disorders, dystonia/spasms | Poor-quality evidence, poorly tolerated, likely no benefit except in dystonia |
| NSAIDs | Neuropathic pain | Poor-quality evidence, likely no benefit |
| Opioids | Neuropathic pain | Low-quality evidence for CRPS, low-quality evidence suggests tramadol may be helpful; used as third-line therapy |
| Serotonin norepinephrine reuptake inhibitors | Chronic pain, sleep disturbances, associated mood disorder | No evidence for CRPS; good-quality evidence for neuralgia, neuropathic pain, and psychological issues |
| Tricyclic antidepressants | Pain, sleep disturbances | No evidence for CRPS; good-quality evidence for neuralgia, neuropathic pain, and psychological issues |
| Topical treatments | ||
| Ketamine (compounded) | Treatment of neuropathic pain | No evidence for CRPS, RCT evidence for neuralgias |
| Lidocaine | Limb pain | No evidence for CRPS, RCT evidence for non-CRPS localized pain |
| NSAIDs | Treatment of neuropathic pain | No evidence in CRPS, RCTs evidence for neuralgias |
Note: Injections and infusions are beyond the scope of this article.
CRPS = complex regional pain syndrome; NSAID = nonsteroidal anti-inflammatory drug; RCT = randomized controlled trial.
The goal of treatment is to improve function and decrease pain. The disease is most likely to respond to a comprehensive, integrated, multi-disciplinary treatment approach that involves medical, psychological, and physical and occupational therapy components.7
There is some evidence that early, aggressive treatment of CRPS may prevent chronic, disabling pain.7,13 Early (within six months of symptom onset) treatment includes referral for physical and occupational therapy, a short course of oral corticosteroids, bisphosphonates, and transdermal lidocaine patches.7,19 Evidence suggests that bisphosphonates used for the first six months of symptoms and a short course (two to four weeks) of oral corticosteroids significantly improve pain in patients with CRPS.7
There is mixed evidence that vitamin C reduces the risk of CRPS after a fracture.22,23 Medications often used to treat neuropathic pain, such as anticonvulsants (e.g., gabapentin [Neurontin], topiramate [Topamax]), tricyclic antidepressants, serotonin-norepinephrine reuptake inhibitors (e.g., duloxetine [Cymbalta]), oral clonidine, and opioids (e.g., tapentadol [Nucynta]), do not show a clear benefit for CRPS, with little evidence regarding their use for this indication.7,24,25 Studies involving nonsteroidal anti-inflammatory drugs show mixed results.7
Physical and occupational therapy are recommended to encourage use of the affected extremity and to desensitize the patient to normal stimuli.7 Physical therapy may incorporate graded motor imagery and mirror therapy (a type of therapy used to rehabilitate the brain's response to pain), which have shown promise for CRPS-related pain.6,7
Although only one randomized controlled trial has studied the effectiveness of psychological interventions in the treatment of CRPS, evidence for referring patients to counseling is likely to be beneficial based on studies of behavior therapy for patients with other chronic pain disorders.7 Counseling may help patients gain self-management strategies and a greater sense of control of their pain, develop realistic treatment goals (e.g., medications or interventions may not fully relieve pain), and begin to understand that their pain does not indicate tissue damage (a belief that may be limiting them from participating in treatments to improve function, such as physical therapy).
Complementary therapies are not well studied in CRPS. Anecdotally, patients report pain improvement with cannabidiol oil, but there is limited evidence supporting its use, and further research is needed. Osteopathic manipulative treatment is not likely to be beneficial because patients generally cannot tolerate it due to hyperalgesia; this is also a topic for future research.
Because medications, counseling, and physical and occupational therapy often only partially alleviate pain and restore function, patients with persistent CRPS symptoms that affect their quality of life should be referred to a pain management specialist to discuss additional treatment options. These treatments may include ketamine (Ketalar) infusions, intrathecal drug pumps, regional nerve blocks, peripheral nerve stimulators, sympathetic ganglion blocks, and surgical sympathectomy.7,8,19,24–27
Prognosis
Retrospective chart reviews document a variety of outcomes in patients with CRPS, from full resolution of symptoms to persistent, chronic pain that lasts for years. One study suggests that CRPS usually resolves spontaneously without treatment, although the time frame is not specified.2 Two studies showed that only a minority of patients develop chronic and severely disabling symptoms. A Dutch study showed severe progression of symptoms in 16% of patients, and 54% of patients were stable. Of the 54 out of 102 patients who were working before the CRPS diagnosis, 41% returned to work without restrictions, 28% returned to work with some restrictions, and 31% were not able to return to work.4 A population-based study in the United States showed resolution of symptoms in 74% of patients.2 Worse outcomes are associated with upper extremity limb involvement and cold CRPS symptoms.4
Worsening psychological distress in conjunction with physical injury has been demonstrated to increase the risk of CRPS and the severity of CRPS symptoms at six- and 12-month intervals.8 Disuse of the painful extremity, a learned behavior for avoiding pain, is also predictive of severe CRPS symptoms, including joint pain with movement, hyperalgesia, hair growth changes, and changes in skin temperature.3
Data Sources: PubMed, the Cochrane Database of Systematic Reviews, and Essential Evidence Plus were searched using the terms complex regional pain syndrome, causalgia, and sympathetic reflex dystrophy. The Agency for Healthcare Research and Quality's Effective Healthcare Reports, National Center for Complementary and Integrative Health, and U.S. Preventive Services Task Force were also searched, but no additional useful information, including relevant guidelines, was found. Articles used in this paper were systematic reviews, including meta-analyses, randomized controlled trials, and some observational studies if no other information was available. Search dates: August to December 2019, March to April 2020, and February 2021.

