
Am Fam Physician. 2021;104(2):135-136
Author disclosure: No relevant financial affiliations.

Details for This Review
Study Population: 1,178 patients, across 11 trials, with suspected small bowel obstruction
Efficacy End Points: Diagnosis of small bowel obstruction
Harm End Points: Data on harms not reported
Narrative: Small bowel obstruction comprises 2% of all patients presenting to the emergency department (ED) with abdominal pain, with more than 300,000 hospitalizations per year.1,2 If not appropriately diagnosed, small bowel obstruction can result in intestinal ischemia, necrosis, and perforation.3 Traditional methods for diagnosing the condition, such as plain radiography, have poor sensitivity and specificity (Table 14,5) and expose patients to radiation.4 Other imaging modalities include computed tomography (CT) and magnetic resonance imaging (MRI). However, they may be expensive, they are not available at all institutions, and CT is associated with radiation exposure.
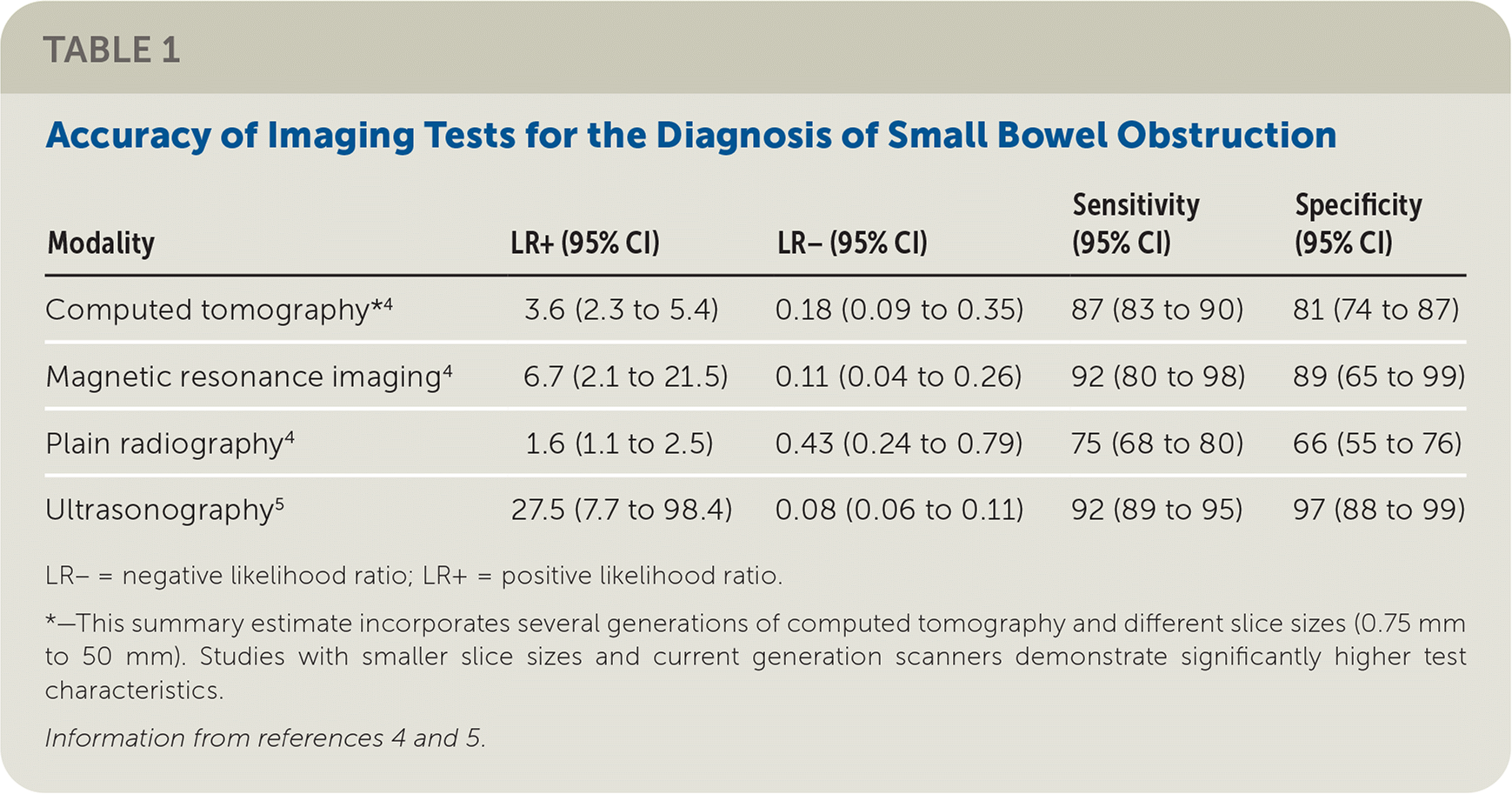
| Modality | LR+ (95% CI) | LR− (95% CI) | Sensitivity(95% CI) | Specificity(95% CI) |
|---|---|---|---|---|
| Computed tomography*4 | 3.6 (2.3 to 5.4) | 0.18 (0.09 to 0.35) | 87 (83 to 90) | 81 (74 to 87) |
| Magnetic resonance imaging4 | 6.7 (2.1 to 21.5) | 0.11 (0.04 to 0.26) | 92 (80 to 98) | 89 (65 to 99) |
| Plain radiography 4 | 1.6 (1.1 to 2.5) | 0.43 (0.24 to 0.79) | 75 (68 to 80) | 66 (55 to 76) |
| Ultrasonography5 | 27.5 (7.7 to 98.4) | 0.08 (0.06 to 0.11) | 92 (89 to 95) | 97 (88 to 99) |
Ultrasonography has demonstrated promise in the diagnosis of small bowel obstruction,6,7 and a meta-analysis including prospective observational studies evaluated the accuracy of ultrasonography for this use.5 The reference standard confirmatory test was determined by individual study definition and included CT, enteroclysis, diagnosis at surgery or discharge, or diagnosis at clinical follow-up. The primary outcome was diagnostic accuracy of ultrasonography for small bowel obstruction, with a subgroup analysis based on specific clinical setting (ED vs. non-ED setting). The authors of the meta-analysis also conducted a sensitivity analysis that categorized inconclusive ultrasound results as false-negatives.
The authors of the meta-analysis identified 9,774 records, of which 11 prospective observational studies (n = 1,178) met the inclusion criteria.5 These studies enrolled patients with signs and symptoms of suspected acute small bowel obstruction, with most studies using a convenience sample. Five studies were conducted in the ED, and six were conducted in other settings, including gastroenterology or radiology clinics, or the setting was not reported. The ultrasonography was performed by an ED clinician in three studies and a radiologist in five studies, and the sonographer was not described in the remainder of studies. The mean age of patients was 50 years, and 74% of patients were male.
Overall, ultrasonography was 92.4% sensitive (95% CI, 89.0% to 94.7%) and 96.6% specific (95% CI, 88.4% to 99.1%), with a positive likelihood ratio of 27.5 (95% CI, 7.7 to 98.4) and a negative likelihood ratio of 0.08 (95% CI, 0.06 to 0.11).5
Caveats: Although ultrasonography can be a valuable tool in the diagnosis of small bowel obstruction, its usefulness depends on the individual clinician's ability to obtain and interpret appropriate images. This meta-analysis included studies with differences in sonographer experience and diagnostic criteria, which limit the applicability of the data. However, previous literature has suggested good diagnostic accuracy for identifying small bowel obstruction after a 10-minute training session and five practice ultrasound examinations.6 In most studies, ultrasonography was performed by a radiologist or the sonographer was not described. Clinicians in the ED were the primary sonographers in only three studies, limiting the analysis of this subset.
Most studies enrolled patients based on a convenience sample, which could be a source of selection bias. Several studies did not state whether clinicians were blinded to the confirmatory CT results, which may have led to potential bias. Inclusion of studies from different clinical settings can also contribute to spectrum bias; however, test characteristics for ultrasonography performed by ED clinicians did not differ significantly from other clinicians based on the authors' subgroup analysis.
A 2019 prospective observational study suggests that the diagnostic accuracy of ultrasonography for small bowel obstruction may be lower, with a sensitivity of 88% (95% CI, 80% to 94%) and specificity of 54% (95% CI, 45% to 63%).8 Of note, this study used clinicians with variable ultrasound experience and was performed at centers that did not regularly use ultrasonography to diagnose small bowel obstruction.8 Therefore, further studies evaluating the diagnostic accuracy among clinicians who are not radiologists are needed.
The studies included in the meta-analysis were at low to moderate risk of bias, and there were limited data on children.5 There was moderate heterogeneity in patient population and outcome assessment, and studies demonstrated mild heterogeneity for sensitivity and moderate heterogeneity for specificity. Sixteen examinations were nondiagnostic. Assuming all of the nondiagnostic examinations were false-negatives (worst-case scenario), a sensitivity analysis demonstrated a slightly lower sensitivity of 90.9% (95% CI, 86.0% to 94.2%) and positive likelihood ratio of 24.6 (95% CI, 7.2 to 84.3), but specificity and negative likelihood ratio remained similar.
Although ultrasonography offers several advantages compared with CT, including the ability to rapidly diagnose small bowel obstruction and assess its progression over time, CT may still be necessary to determine the underlying etiology, which can influence decisions regarding operative management.
Conclusion: According to the current available evidence, ultrasonography appears to be highly sensitive and specific in the diagnosis of small bowel obstruction. Although the exact test characteristics for diagnosing small bowel obstruction based on ultrasonography performed by clinicians other than radiologists are less clear, this modality is rapid, repeatable, inexpensive, easily available, and noninvasive; avoids radiation exposure; and can be performed at the bedside.
Although we assign a color rating of green (benefits outweigh harms) strictly based on diagnostic accuracy statistics, generalizability to family physicians and others performing point-of-care ultrasonography is limited from this review.
