Approximately 19 million students attend college in the United States. Although they are generally healthy, about 20% of youth have special health care needs, including asthma, diabetes mellitus, and learning, mental health, and substance use disorders. Physicians can facilitate the transition of a youth to an adult model of health care by using structured processes to orient the youth to self-care before entry into college. Stimulant medications are effective for treatment of students with attention-deficit/hyperactivity disorder, but physicians should monitor for signs of drug diversion. Learning disorders may manifest with emotional or physical symptoms and are managed in a multidisciplinary fashion. Depression, anxiety, sleep problems, and posttraumatic stress and eating disorders are common in this population and can affect school performance. Screening and/or interventions for obesity, depression, anxiety, violence, nicotine use, and substance use are effective. Immunizations for influenza, human papillomavirus, meningococcus, and pertussis are crucial in this high-risk population. Lesbian, bisexual, gay, transgender, and queer students have unique health care needs.
Approximately 19 million full- and part-time students were enrolled in U.S. colleges in 2018.1 Although they are generally healthy, many of these individuals have special health care needs such as asthma, diabetes mellitus, mental health concerns, and learning disorders. Understanding and managing the needs of this dynamic population involve addressing the unique psychosocial stressors related to this life transition that manifest before and while attending college. Common self-reported medical conditions among college students are presented in Table 1.2
WHAT'S NEW ON THIS TOPIC

SORT: KEY RECOMMENDATIONS FOR PRACTICE
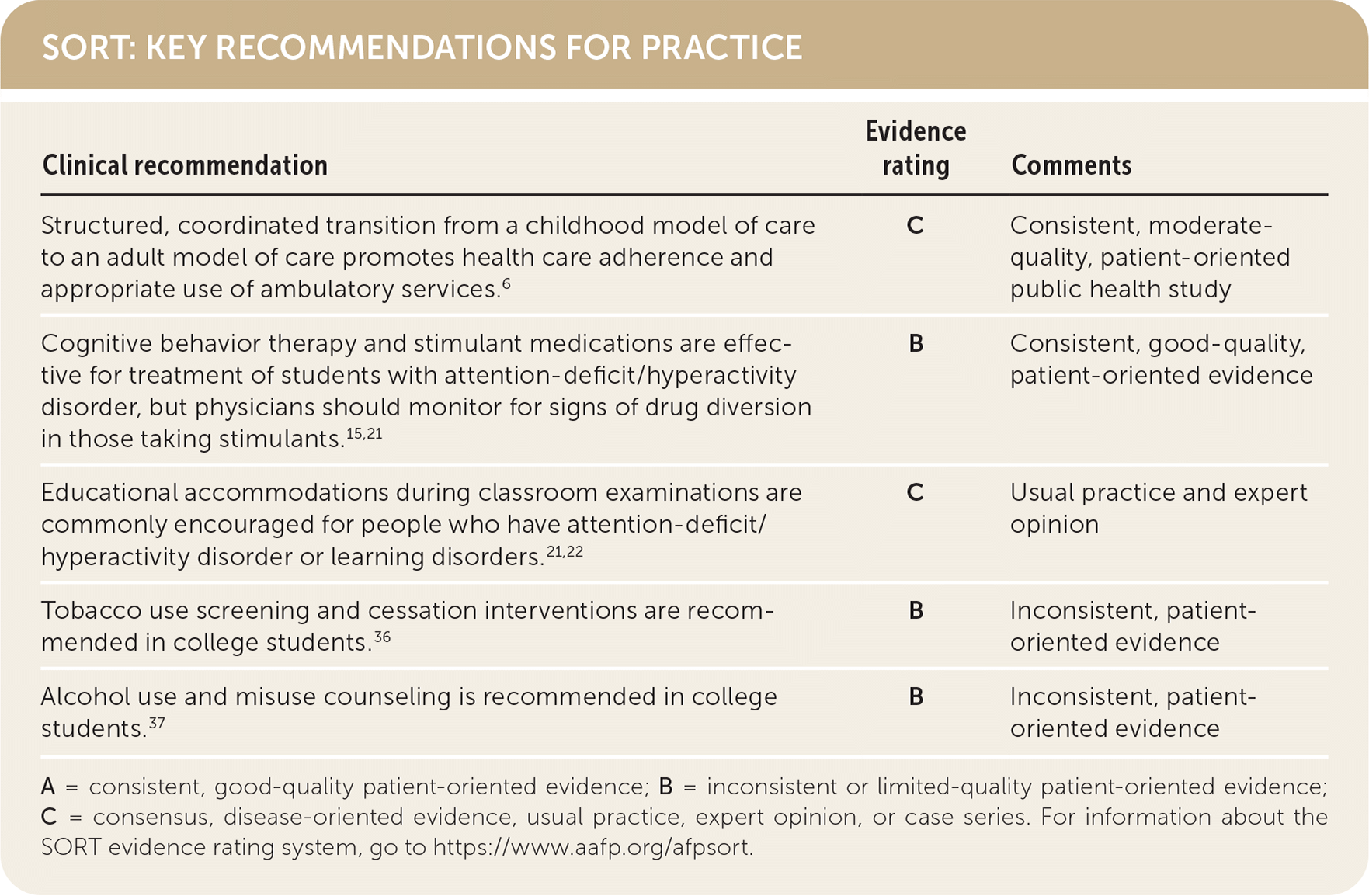
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
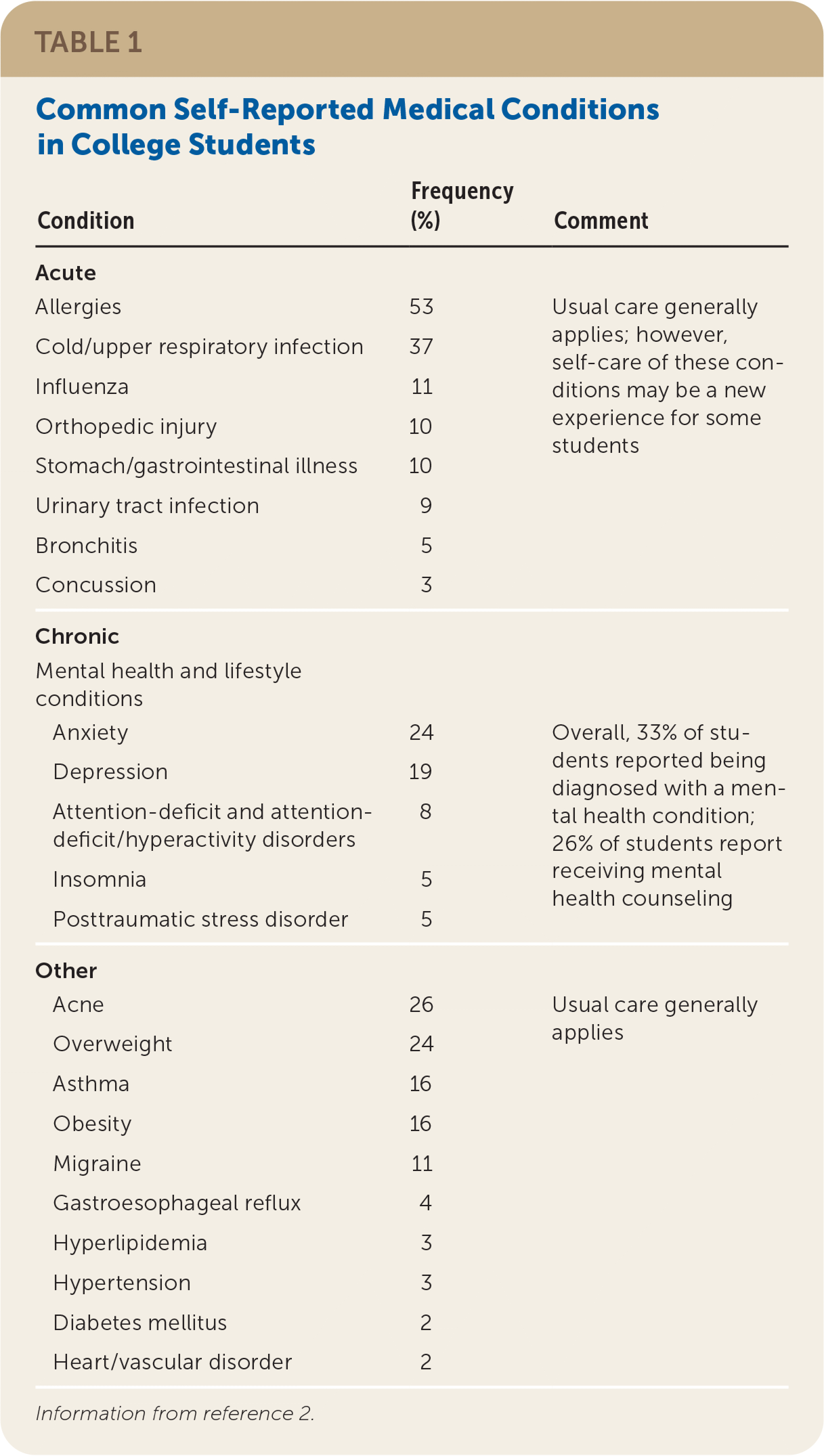
TABLE 1. Common Self-Reported Medical Conditions in College Students
| Condition | Frequency (%) | Comment |
|---|---|---|
| Acute | ||
| Allergies | 53 | Usual care generally applies; however, self-care of these conditions may be a new experience for some students |
| Cold/upper respiratory infection | 37 | |
| Influenza | 11 | |
| Orthopedic injury | 10 | |
| Stomach/gastrointestinal illness | 10 | |
| Urinary tract infection | 9 | |
| Bronchitis | 5 | |
| Concussion | 3 | |
| Chronic | ||
| Mental health and lifestyle conditions | ||
| Anxiety | 24 | Overall, 33% of students reported being diagnosed with a mental health condition; 26% of students report receiving mental health counseling |
| Depression | 19 | |
| Attention-deficit and attention deficit/hyperactivity disorders | 8 | |
| Insomnia | 5 | |
| Posttraumatic stress disorder | 5 | |
| Other | ||
| Acne | 26 | Usual care generally applies |
| Overweight | 24 | |
| Asthma | 16 | |
| Obesity | 16 | |
| Migraine | 11 | |
| Gastroesophageal reflux | 4 | |
| Hyperlipidemia | 3 | |
| Hypertension | 3 | |
| Diabetes mellitus | 2 | |
| Heart/vascular disorder | 2 |
Information from reference 2.
Transition to College
College students are often assuming responsibility for their health care for the first time; however, the transition from a childhood model of care to an adult model of care is often given a lower priority than other transitions that students are experiencing.3 Approximately 20% of U.S. youth have special health care needs.4 Although many children and adolescents have taken steps to comanage their diseases, most of these youth do not receive a structured transition to an adult care model,5 and the situation is complicated by poor care coordination.3 Students may have to reconcile recommendations from multiple sources of care, such as an ongoing childhood physician and a new clinician at college if living away from home. Physicians may perceive that youth are poorly informed regarding their own health care matters. Simultaneously, some physicians may be poorly informed about patients' childhood conditions that continue into adulthood, such as cerebral palsy and cystic fibrosis.5 Problems with this transition result in declines in treatment adherence, increased emergency department use, and increased hospitalizations.3 Improved adherence to health care, better patient experience, and increased appropriate use of ambulatory services are reported with structured health care transition visits that prepare the student for self-care and help to transfer the student to the adult model of care6 (Table 2).
TABLE 2. Clinician Checklist for Students Transitioning to College

| Meet privately with the patient for part of the visit |
| Prepare youth and family for transition by encouraging chronic condition management responsibilities (knowledge of conditions, treatments) |
| Assess readiness for transition and develop transition plan |
| Implement transition plan with provision of medical records (visits, tests, reports) to patient and family and care coordination with receiving practice |
| Anticipatory guidance |
| Awareness of counseling services |
| Chronic health conditions |
| College/occupational plans |
| Food security |
| Functional independence and community inclusion (for students with disabilities) |
| Health insurance |
| Legal matters (power of attorney, advance medical directive) |
| Medical decision-making/privacy at age of majority (state-specific) |
| Nutrition and fitness |
| Pocket card or electronic medical record of conditions, medications, and immunizations |
| Public service (voting rights, selective service) |
| Sexuality and relationships |
| Sports/athletics |
| Substance use, smoking, and vaping |
Health Care Coverage
Under the Patient Protection and Affordable Care Act (ACA), students younger than 26 years have four options for qualifying health coverage: coverage under a parent's insurance plan, school-offered health plans, marketplace plans, and Medicaid and the Children's Health Insurance Program.7 Despite these options, 72% of college students and recent college graduates indicate that finding health care coverage remains difficult, and 1.6 million students remain uninsured.8
A parent's insurance plan may be the least expensive option, but it may also limit confidentiality for the young adult because notices of service are sometimes sent to the primary enrollee. Participation in one of the other three options results in bills and explanations of benefits being sent directly to the student. Many school-offered plans do not provide coverage during summer breaks and may leave the student uninsured if other options are not pursued.
Under the ACA, all but the school-offered health plans are regulated by the Department of Health and Human Services. These plans are required to provide the following coverage without an annual or lifetime limit: ambulatory services; emergency services; hospitalization; laboratory tests; maternity and newborn care; mental health care, including substance use treatment; prescription medications; and rehabilitation services.7 Copays for these services vary widely.
Institutions of higher education vary with regard to testing, immunization, and prevention practice, depending on state law and exemption practices, in their health care resources and responses to the COVID-19 pandemic.9
Common Learning and Mental Health Issues
The learning and mental health needs of college students remain a growing concern. College counseling center directors report an increase in the number of students who arrive on campus already taking a psychotropic medication,10 with at least 40% of these directors reporting increases compared with the previous five years of depression and anxiety disorders, learning disorders, sexual assault, and crisis issues requiring immediate responses.11 In colleges, most health center visits (60%) are to primary care clinics, whereas a smaller proportion of these visits (13%) are to mental health clinics.11 Students in higher education are protected by the Americans with Disabilities Act and Section 504 of the Rehabilitation Act12; however, the ACA does not support costs associated with diagnosis and treatment of learning disorders.13 Students should meet with their college office of disabilities to understand school policies and resources and to self-advocate regarding insurance requirements.14
ATTENTION-DEFICIT/HYPERACTIVITY DISORDER
Approximately 8.2% of college students endorse a diagnosis of attention-deficit/hyperactivity disorder (ADHD).2 Pharmacotherapy, including amphetamines, methylphenidate (Ritalin), bupropion (Wellbutrin), and atomoxetine (Strattera), is effective in appropriately diagnosed adults. 15 Associated symptoms are identified by using the Adult ADHD Self-Report Scale (Table 32,10,11,16–20 ). Cognitive behavior therapy for adults with ADHD, particularly with symptoms of inattention, has been shown to be effective.21 Students should be counseled regarding consequences of drug diversion.
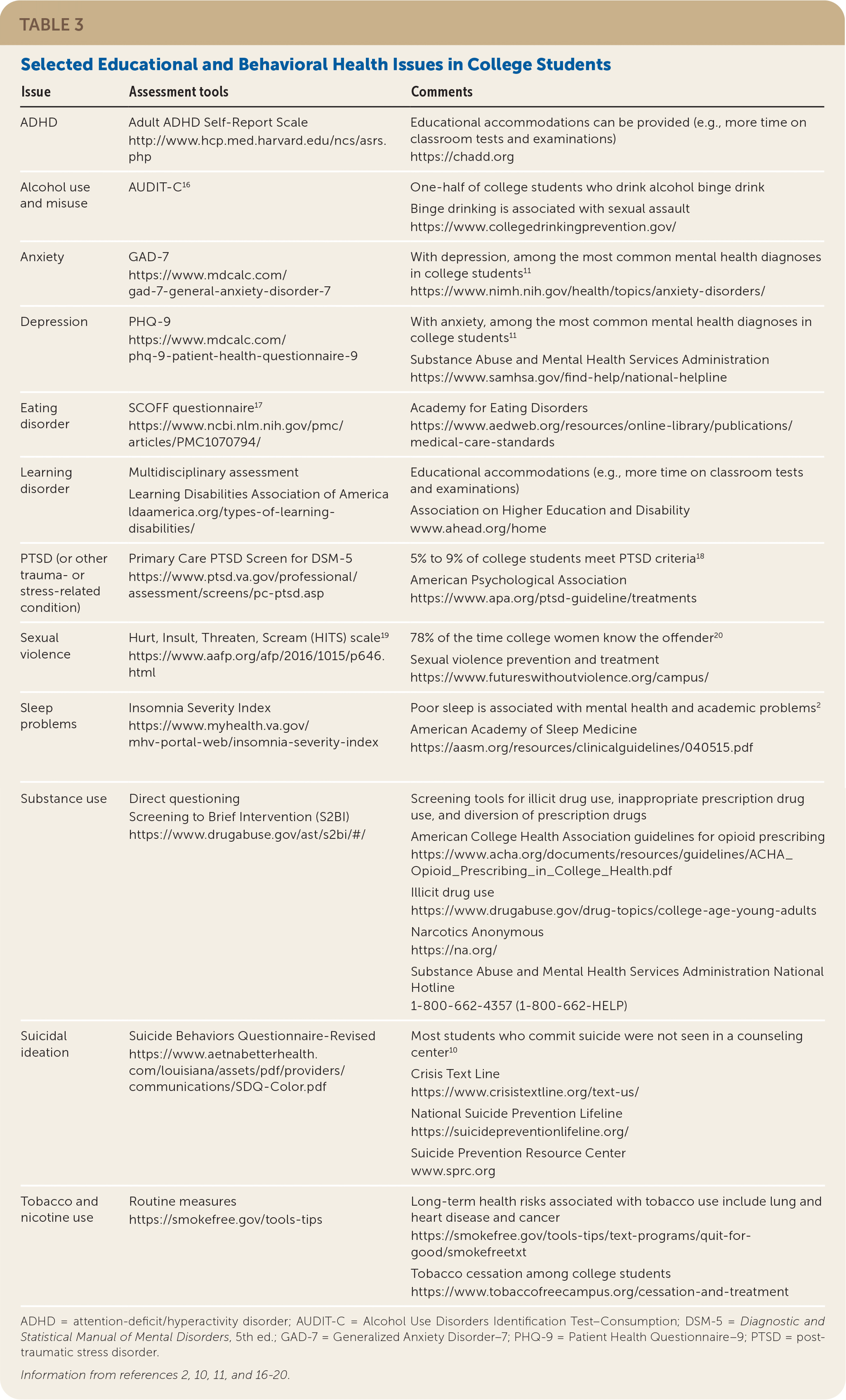
TABLE 3. Selected Educational and Behavioral Health Issues in College Students
| Issue | Assessment tools | Comments |
|---|---|---|
| ADHD | Adult ADHD Self-Report Scale http://www.hcp.med.harvard.edu/ncs/asrs.php | Educational accommodations can be provided (e.g., more time on classroom tests and examinations) https://chadd.org |
| Alcohol use and misuse | AUDIT-C16 | One-half of college students who drink alcohol binge drink Binge drinking is associated with sexual assault https://www.collegedrinkingprevention.gov/ |
| Anxiety | GAD-7 https://www.mdcalc.com/gad-7-general-anxiety-disorder-7 | With depression, among the most common mental health diagnoses in college students11 https://www.nimh.nih.gov/health/topics/anxiety-disorders/ |
| Depression | PHQ-9 https://www.mdcalc.com/phq-9-patient-health-questionnaire-9 | With anxiety, among the most common mental health diagnoses in college students11 Substance Abuse and Mental Health Services Administration https://www.samhsa.gov/find-help/national-helpline |
| Eating disorder | SCOFF questionnaire17 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1070794/ | Academy for Eating Disorders https://www.aedweb.org/resources/online-library/publications/medical-care-standards |
| Learning disorder | Multidisciplinary assessment Learning Disabilities Association of America ldaamerica.org/types-of-learning-disabilities/ | Educational accommodations (e.g., more time on classroom tests and examinations) Association on Higher Education and Disability https://www.ahead.org/home |
| PTSD (or other trauma- or stress-related condition) | Primary Care PTSD Screen for DSM-5 https://www.ptsd.va.gov/professional/assessment/screens/pc-ptsd.asp | 5% to 9% of college students meet PTSD criteria18 American Psychological Association https://www.apa.org/ptsd-guideline/treatments |
| Sexual violence | Hurt, Insult, Threaten, Scream (HITS) scale19 https://www.aafp.org/afp/2016/1015/p646.html | 78% of the time college women know the offender 20 Sexual violence prevention and treatment https://www.futureswithoutviolence.org/campus/ |
| Sleep problems | Insomnia Severity Index https://www.myhealth.va.gov/mhv-portal-web/insomnia-severity-index | Poor sleep is associated with mental health and academic problems2 American Academy of Sleep Medicine https://aasm.org/resources/clinicalguidelines/040515.pdf |
| Substance use | Direct questioning Screening to Brief Intervention (S2BI) https://www.drugabuse.gov/ast/s2bi/#/ | Screening tools for illicit drug use, inappropriate prescription drug use, and diversion of prescription drugs American College Health Association guidelines for opioid prescribing https://www.acha.org/documents/resources/guidelines/ACHA_Opioid_Prescribing_in_College_Health.pdf Illicit drug use https://www.drugabuse.gov/drug-topics/college-age-young-adults Narcotics Anonymous https://na.org/ Substance Abuse and Mental Health Services Administration National Hotline 1-800-662-4357 (1-800-662-HELP) |
| Suicidal ideation | Suicide Behaviors Questionnaire-Revised https://www.aetnabetterhealth.com/louisiana/assets/pdf/providers/communications/SDQ-Color.pdf | Most students who commit suicide were not seen in a counseling center10 Crisis Text Line https://www.crisistextline.org/text-us/ National Suicide Prevention Lifeline https://suicidepreventionlifeline.org/ Suicide Prevention Resource Center https://www.sprc.org/ |
| Tobacco and nicotine use | Routine measures https://smokefree.gov/tools-tips | Long-term health risks associated with tobacco use include lung and heart disease and cancer https://smokefree.gov/tools-tips/text-programs/quit-for-good/smokefreetxt Tobacco cessation among college students https://www.tobaccofreecampus.org/cessation-and-treatment |
ADHD = attention-deficit/hyperactivity disorder; AUDIT-C = Alcohol Use Disorders Identification Test–Consumption; DSM-5 = Diagnostic and Statistical Manual of Mental Disorders, 5th ed.; GAD-7 = Generalized Anxiety Disorder–7; PHQ-9 = Patient Health Questionnaire–9; PTSD = posttraumatic stress disorder.
LEARNING DISORDERS
Physicians may identify a learning disorder when considering other conditions (e.g., depression, sleep problems, thyroid dysfunction). An estimated 3.6% to 11% of college students self-report a learning disorder.2 Learning disorders may manifest as difficulty listening, thinking, speaking, reading, writing, spelling, or completing mathematical calculations.22 Among those who self-identify with a learning disorder, only 33% reported using accommodations.22 Interventions include neuropsychologic evaluation, assistive technologies (e.g., text-to-speech or speech-to-text), direct assistance (e.g., tutoring and remediation), coursework or testing modifications, strategy instruction (i.e., showing students how to learn the content or skills needed), and comprehensive support (e.g., group and individual instructions).23 It remains unclear whether accommodations result in better academic performance or satisfaction with school22 (Table 32,10,11,16–20 ).
Selected Mental Health and Behavioral Health Issues
ANXIETY AND DEPRESSION
Anxiety and depression are the most common mental health diagnoses among college students.11 Risk factors for depression among college students are associated with being female, entering college with depression, a pattern of negative thinking or rumination, dysfunctional attitudes, history of childhood abuse or sexual abuse, or stressful life events.24 Prevention programs can decrease the prevalence of anxiety and depression on college campuses.25 Interventions commonly used to treat depression and generalized anxiety disorder, such as pharmacotherapy, cognitive behavior therapy, and mindfulness, work well in collegiate populations, although there is less evidence of success compared with other anxiety disorders (e.g., panic disorder, social phobia, specific phobia).26
SUICIDE
An estimated 13.3% of college students reported seriously considering suicide, and 2.4% reported attempting suicide in the past 12 months.2 Among those presenting to a mental health clinic, there has been a 12.7% increase in the number of college students presenting with serious suicidal ideation over the past nine years.27 Family physicians may have a role in identifying these students because most college students (86%) who commit suicide had not sought services in a counseling center.10
POSTTRAUMATIC STRESS DISORDER
Lifetime prevalence of posttraumatic stress disorder (PTSD) among college students ranges from 5% to 9%, which is similar to that of the general U.S. population.18 PTSD is associated with other significant mental health problems among college students, including risky alcohol use, medication misuse, disordered eating, and depression.18 Sources of trauma among college students are diverse and warrant screening.11,18 Student veterans and student veterans with PTSD are more likely to engage in high-risk drinking and fighting.28
Eating and Lifestyle
EATING DISORDERS
Risk factors for eating disorders include frequent dieting, weight concerns, body dissatisfaction, and drive for thinness. College-based programs for preventing and treating eating disorders can be effective.29 Most of these programs are based on cognitive behavior therapy principles or dissonance-based techniques (i.e., learning to act in a way that is contrary to an existing attitude).29 Treatment focuses on medical stabilization, nutritional rehabilitation, normalization of eating behavior, and psychosocial stabilization.30
SLEEP DISORDERS
Poor sleep is associated with other mental health problems, including ADHD, anxiety, depression, and suicidal thoughts and behaviors. As many as 62% of college students experience poor sleep quality.31 Sleep difficulties negatively impacted class performance or delayed progress toward a degree among 22.4% of students.2 Proper treatment of sleep-related problems is based on structured assessment.32
Selected Substance Use and Misuse
MEDICATION MISUSE AND DIVERSION
The prevalence of nonmedical use of controlled medications among college students within the past year ranged from 1.9% to 21.4%.33 Lifetime rates of diversion range from 16% to 29% among students with stimulant prescriptions.34 Greater risk of nonmedical use of stimulants is associated with being 18 to 25 years of age, being male, being White, having a college grade point average below 3.5, being in a fraternity or sorority, self-reporting more severe ADHD symptoms, and other substance use disorders.35
TOBACCO AND NICOTINE USE
As many as 33.8% of college students have ever used tobacco or a nicotine-delivery product (e.g., vaping, electronic cigarettes), and 65% of these students have used these products at least once within the past three months.2 Physician-directed interventions and institutional efforts are effective in reducing tobacco use in this population.36
ALCOHOL USE AND MISUSE
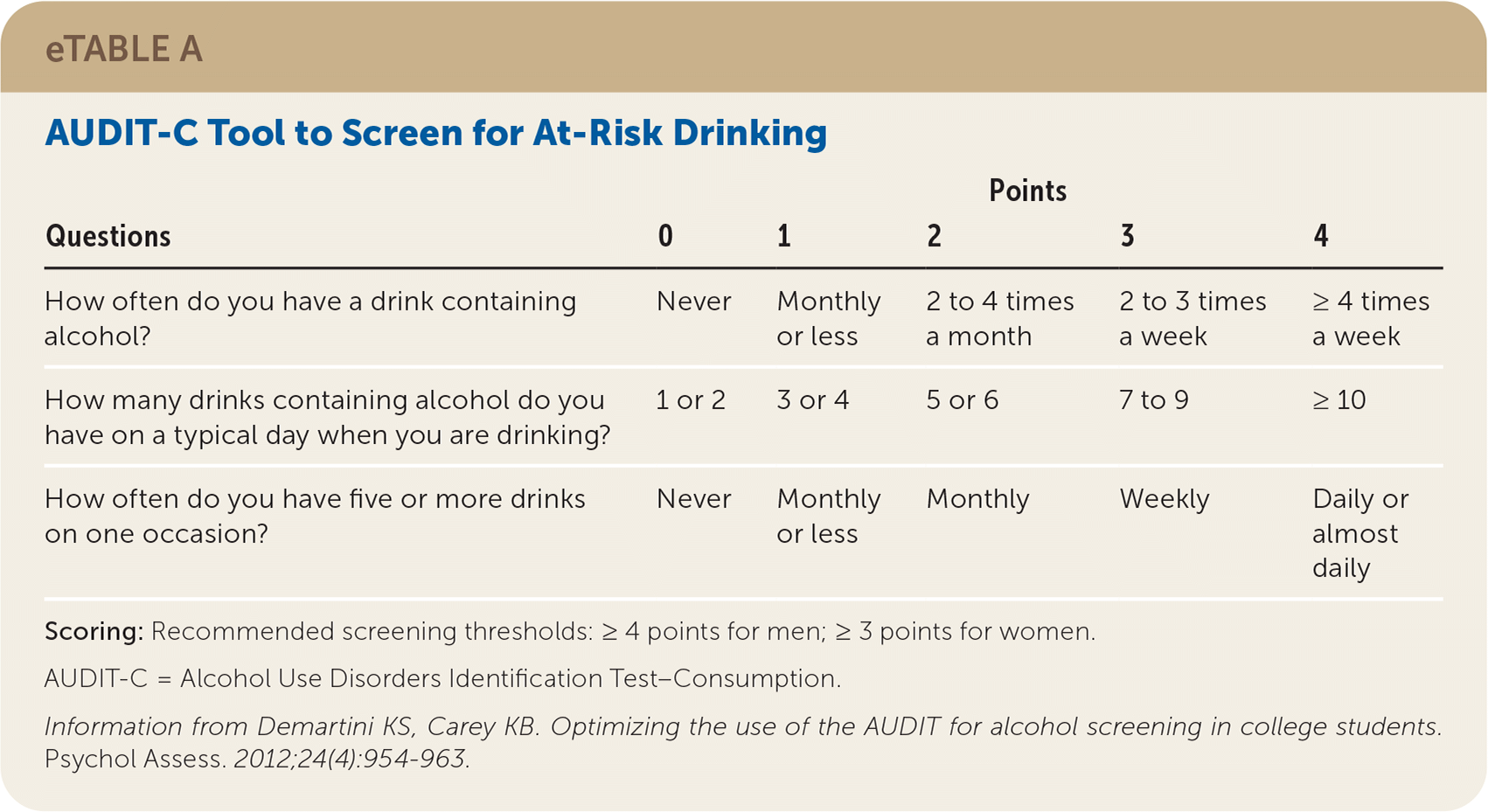
In the prior two weeks, 24% of college students endorsed binge drinking (i.e., five or more drinks per sitting), and 22% indicated that within the past 12 months they did something they later regretted after drinking alcohol.2 Brief interventions using motivational enhancement or motivational interview strategies are effective for reducing alcohol use among college students who drink.37 Physicians can screen for problematic alcohol use with the Alcohol Use Disorders Identification Test–Consumption (AUDIT-C; eTable A). Scores of 5 or above for women and 7 or above for men indicate possible problem drinking in college populations.38
eTABLE A AUDIT-C Tool to Screen for At-Risk Drinking
| Questions | Points | ||||
|---|---|---|---|---|---|
| 0 | 1 | 2 | 3 | 4 | |
| How often do you have a drink containing alcohol? | Never | Monthly or less | 2 to 4 times a month | 2 to 3 times a week | ≥ 4 times a week |
| How many drinks containing alcohol do you have on a typical day when you are drinking? | 1 or 2 | 3 or 4 | 5 or 6 | 7 to 9 | ≥ 10 |
| How often do you have five or more drinks on one occasion? | Never | Monthly or less | Monthly | Weekly | Daily or almost daily |
Scoring: Recommended screening thresholds: ≥ 4 points for men; ≥ 3 points for women.
AUDIT-C = Alcohol Use Disorders Identification Test–Consumption.
Information from Demartini KS, Carey KB. Optimizing the use of the AUDIT for alcohol screening in college students. Psychol Assess. 2012;24(4):954–963.
ILLICIT DRUG USE
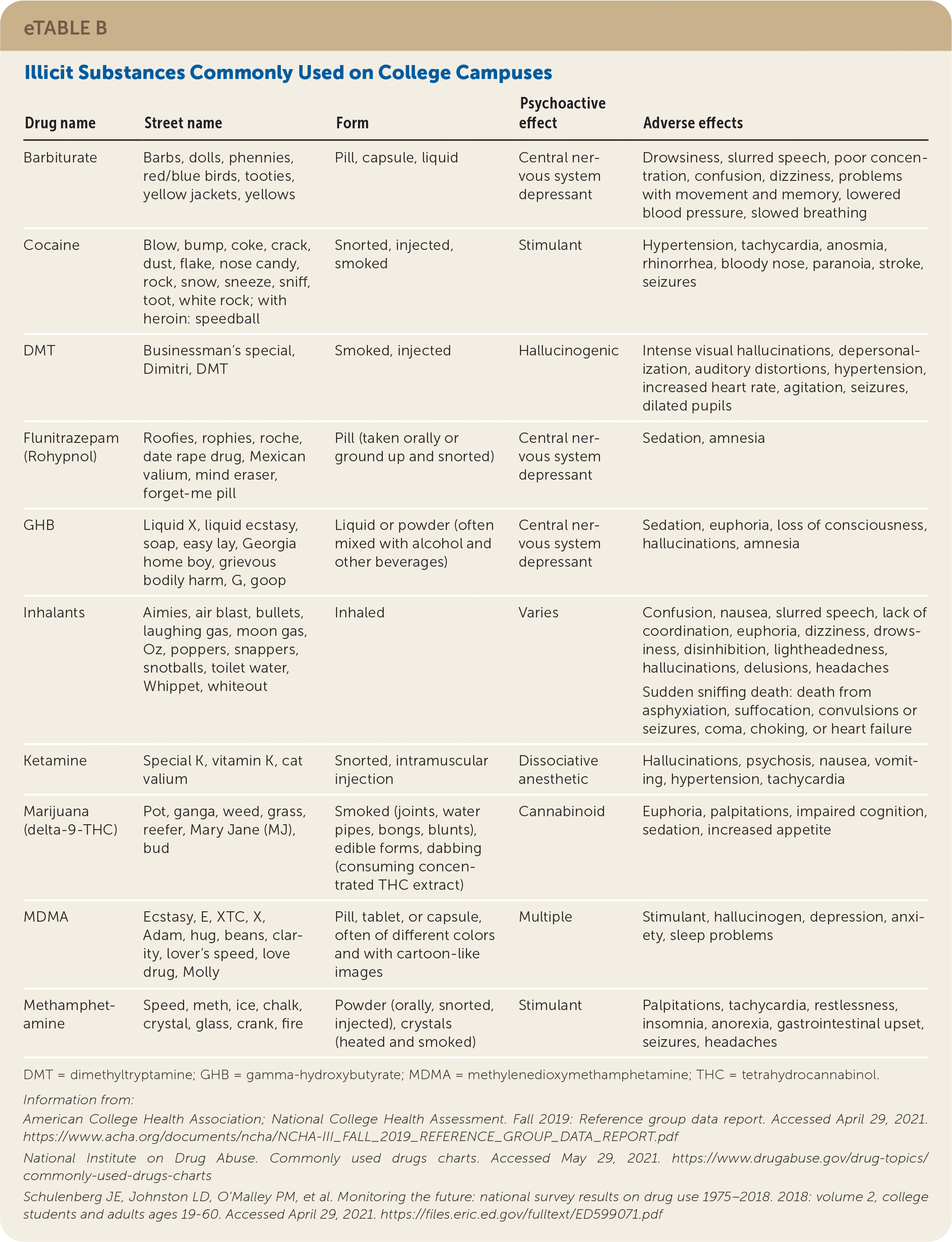
Annual prevalence of using any illicit drug (45%) and any illicit drug other than marijuana (18%) was similar between college students and their noncollege peers.39 College students tend to use MDMA (3,4-methylenedioxymethamphetamine; 4.4%), amphetamines (8.5%; without a doctor's prescription), and cocaine (5.3%) at higher rates than their noncollege peers.39 eTable B summarizes common illicit drugs, their common street names, and related effects.
eTABLE B Illicit Substances Commonly Used on College Campuses
| Drug name | Street name | Form | Psychoactive effect | Adverse effects |
|---|---|---|---|---|
| Barbiturate | Barbs, dolls, phennies, red/blue birds, tooties, yellow jackets, yellows | Pill, capsule, liquid | Central nervous system depressant | Drowsiness, slurred speech, poor concentration, confusion, dizziness, problems with movement and memory, lowered blood pressure, slowed breathing |
| Cocaine | Blow, bump, coke, crack, dust, flake, nose candy, rock, snow, sneeze, sniff, toot, white rock; with heroin: speedball | Snorted, injected, smoked | Stimulant | Hypertension, tachycardia, anosmia, rhinorrhea, bloody nose, paranoia, stroke, seizures |
| DMT | Businessman's special, Dimitri, DMT | Smoked, injected | Hallucinogenic | Intense visual hallucinations, depersonalization, auditory distortions, hypertension, increased heart rate, agitation, seizures, dilated pupils |
| Flunitrazepam (Rohypnol) | Roofies, rophies, roche, date rape drug, Mexican valium, mind eraser, forget-me pill | Pill (taken orally or ground up and snorted) | Central nervous system depressant | Sedation, amnesia |
| GHB | Liquid X, liquid ecstasy, soap, easy lay, Georgia home boy, grievous bodily harm, G, goop | Liquid or powder (often mixed with alcohol and other beverages) | Central nervous system depressant | Sedation, euphoria, loss of consciousness, hallucinations, amnesia |
| Inhalants | Aimies, air blast, bullets, laughing gas, moon gas, Oz, poppers, snappers, snotballs, toilet water, Whippet, whiteout | Inhaled | Varies | Confusion, nausea, slurred speech, lack of coordination, euphoria, dizziness, drowsiness, disinhibition, lightheadedness, hallucinations, delusions, headaches Sudden sniffing death: death from asphyxiation, suffocation, convulsions or seizures, coma, choking, or heart failure |
| Ketamine | Special K, vitamin K, cat valium | Snorted, intramuscular injection | Dissociative anesthetic | Hallucinations, psychosis, nausea, vomiting, hypertension, tachycardia |
| Marijuana (delta-9-THC) | Pot, ganga, weed, grass, reefer, Mary Jane (MJ), bud | Smoked (joints, water pipes, bongs, blunts), edible forms, dabbing (consuming concentrated THC extract) | Cannabinoid | Euphoria, palpitations, impaired cognition, sedation, increased appetite |
| MDMA | Ecstasy, E, XTC, X, Adam, hug, beans, clarity, lover's speed, love drug, Molly | Pill, tablet, or capsule, often of different colors and with cartoon-like images | Multiple | Stimulant, hallucinogen, depression, anxiety, sleep problems |
| Methamphetamine | Speed, meth, ice, chalk, crystal, glass, crank, fire | Powder (orally, snorted, injected), crystals (heated and smoked) | Stimulant | Palpitations, tachycardia, restlessness, insomnia, anorexia, gastrointestinal upset, seizures, headaches |
DMT = dimethyltryptamine; GHB = gamma-hydroxybutyrate; MDMA = methylenedioxymethamphetamine; THC = tetrahydrocannabinol.
Information from:
American College Health Association; National College Health Assessment. Fall 2019: Reference group data report. Accessed April 29, 2021. https://www.acha.org/documents/ncha/NCHA-III_FALL_2019_REFERENCE_GROUP_DATA_REPORT.pdf
National Institute on Drug Abuse. Commonly used drugs charts. Accessed May 29, 2021. https://www.drugabuse.gov/drug-topics/commonly-used-drugs-charts
Schulenberg JE, Johnston LD, O'Malley PM, et al. Monitoring the future: national survey results on drug use 1975–2018. 2018: volume 2, college students and adults ages 19–60. Accessed April 29, 2021. https://files.eric.ed.gov/fulltext/ED599071.pdf
Preventive Care
Most colleges require current immunizations before entry. Vaccination guidelines for COVID-19 vary state by state and by individual institution. A second booster dose of meningococcal ACWY vaccine should be given at 16 years of age to prevent the effects of meningitis in the vulnerable college-aged population. Two-dose coverage has been as low as 28.5% in patients who are 17 years of age.40 Immunization for meningococcus B serotype can be separately administered for patients at increased risk and based on shared decision-making.40,41 Annual influenza immunization is important in the dorm-dwelling college-aged population. Immunization for pertussis is important, especially in high-risk populations. Human papillomavirus vaccination status should be verified before or after starting college; it is approved, regardless of sex.42 Table 4 lists other U.S. Preventive Services Task Force (USPSTF) recommendations.43 Public health departments may provide low- or no-cost immunizations for eligible students.
TABLE 4. Selected USPSTF Recommendations for Preventive Care in Nonpregnant Adults

| A Recommendation: offer or provide this service Cervical cancer: screen patients 21 to 29 years of age every 3 years with cervical cytology alone Folic acid: folic acid should be taken for the prevention of neural tube defects for all who are planning or capable of pregnancy: 0.4 to 0.8 mg (400 to 800 mcg) of folic acid daily HIV infection: screen people 15 to 65 years of age and those at increased risk HIV PrEP: offer PrEP to people at high risk of acquiring HIV Hypertension: screen adults 18 years and older and suggest home monitoring; measurements outside the clinical setting are advised for diagnostic confirmation Syphilis infection: screen asymptomatic, nonpregnant adults and adolescents at risk Tobacco smoking cessation: ask all adults about tobacco use, advise them to stop using tobacco, and provide behavioral interventions and U.S. Food and Drug Administration–approved pharmacotherapy for cessation to adults who use tobacco |
| B Recommendation: offer or provide this service BRCA 1/2: assess people with a personal history of BRCA 1 and 2 gene mutations with an appropriate brief familial risk assessment tool; a positive assessment should result in receiving genetic counseling and, if indicated after counseling, genetic testing Chlamydia: screen sexually active women 24 years and younger and older women who are at increased risk of infection Depression (adolescents 12 to 18 years of age): screen for major mood disorders; screening should be implemented with adequate systems in place to ensure accurate diagnosis, effective treatment, and appropriate follow-up Depression (general adult population): screen in the general adult population, including pregnant and postpartum patients; screening should be implemented with adequate systems in place to ensure accurate diagnosis, effective treatment, and appropriate follow-up Gonorrhea: screen sexually active women 24 years and younger and older women who are at increased risk of infection Healthful diet and physical activity for CVD disease prevention in adults with cardiovascular risk factors: offer or refer adults with CVD risk factors to behavioral counseling interventions to promote a healthful diet and physical activity Hepatitis B virus: screen adolescents and adults at high risk of infection Hepatitis C virus: screen adults 18 to 79 years of age Intimate partner violence, elder abuse, and abuse of vulnerable adults: screen women of reproductive age and, in those who screen positive, provide or refer to ongoing support services Latent tuberculosis infection: screen populations at increased risk Sexually transmitted infections: provide behavioral counseling for all sexually active adolescents and for adults who are at increased risk of sexually transmitted infections Skin cancer prevention: counsel young adults, adolescents, children, and parents of young children about minimizing exposure to ultraviolet radiation in people 6 months to 24 years of age with fair skin types to reduce their risk of skin cancer Unhealthy alcohol use: screen adults 18 years and older in primary care settings and provide people engaged in risky or hazardous drinking with brief behavioral counseling interventions to reduce unhealthy alcohol use Unhealthy drug use: screen adults 18 years and older by asking questions about unhealthy drug use; screening should be implemented when services for accurate diagnosis, effective treatment, and appropriate care can be offered or referred (screening refers to asking questions about unhealthy drug use, not testing biologic specimens) Weight loss to prevent obesity-related morbidity and mortality: offer or refer adults with a body mass index of 30 kg per m2 or higher to intensive, multicomponent behavioral interventions |
| C Recommendation: offer or provide this service only if other considerations support the offering |
| Healthful diet and physical activity for CVD prevention in adults without known risk factors: individualize the decision to offer or refer adults without obesity who do not have hypertension, dyslipidemia, abnormal blood glucose levels, or diabetes mellitus to behavioral counseling to promote a healthful diet and physical activity; existing evidence indicates a positive but small benefit of behavioral counseling for the prevention of CVD in this population; people who are interested and ready to make behavioral changes may be most likely to benefit from behavioral counseling |
| D Recommendation: not recommended Cervical cancer: recommends against screening for cervical cancer in patients younger than 21 years Genital herpes infection: recommends against routine serologic screening for genital herpes simplex virus infection in asymptomatic adolescents and adults, including those who are pregnant Testicular cancer: recommends against screening for testicular cancer in adolescents or adults |
| I Statement: insufficient evidence Chlamydia and gonorrhea (sexually active men): current evidence is insufficient to assess the balance of benefits and harms of screening for chlamydia and gonorrhea in men Gynecologic conditions: current evidence is insufficient to assess the balance of benefits and harms of performing screening pelvic examinations in asymptomatic patients who are not at increased risk of any specific gynecologic condition for the early detection and treatment of a range of gynecologic conditions Illicit drug use in children, adolescents, and young adults: current evidence is insufficient to assess the balance of benefits and harms of primary care–based behavioral counseling interventions to prevent illicit drug use, including nonmedical use of prescription drugs, in children, adolescents, and young adults Intimate partner violence, elder abuse, and abuse of vulnerable adults: current evidence is insufficient to assess the balance of benefits and harms of screening for abuse and neglect in older or vulnerable adults Skin cancer in asymptomatic adults: current evidence is insufficient to assess the balance of benefits and harms of visual skin examination by a clinician to screen for skin cancer in asymptomatic adults Skin cancer prevention: current evidence is insufficient to assess the balance of benefits and harms of counseling adults about skin self-examination to prevent skin cancer Suicide risk: current evidence is insufficient to assess the balance of benefits and harms of screening for suicide risk in adolescents, adults, and older adults in primary care Tobacco smoking cessation: the current evidence is insufficient to assess the balance of benefits and harms of electronic cigarettes for tobacco cessation in adults; the USPSTF recommends that clinicians direct patients who smoke tobacco to other cessation interventions with established effectiveness and safety |
CVD = cardiovascular disease; PrEP = pre-exposure prophylaxis; USPSTF = U.S. Preventive Services Task Force.
Information from reference 43.
Sexual Health
The USPSTF has issued several evidence-based screening guidelines applicable to college-aged students, which are also supported by the American Academy of Family Physicians.44 Cervical cytology screening should not be performed until 21 years of age and should then occur every three years until 29 years of age.45 Of note, the American Cancer Society recommends screening with primary human papillomavirus testing (with co-testing or cytology alone as a back-up option) beginning at 25 years of age.46 See the article in American Family Physician on health maintenance for women for more information.47 Screening for chlamydia and gonorrhea is recommended for sexually active women 24 years and younger48; this recommendation is currently being updated to also offer screening for women 25 years and older who are at increased risk of infection.49 Screening for HIV is recommended for adolescents 15 years and older, and hepatitis C screening is recommended for all adults 18 to 79 years of age.50,51
The USPSTF recommends intensive behavioral and contraceptive counseling for all sexually active adolescents and adults at an increased risk of sexually transmitted infections.52 The USPSTF and the American College Health Association (ACHA) also recommend offering pre-exposure prophylaxis with effective antiretroviral therapy to people at high risk of HIV acquisition.53,54 The ACHA has extensive guidelines around best practices for sexual health promotion and the avoidance of sexual and relationship violence.55,56 Physicians start this process by creating a welcoming and inclusive clinic environment for students that considers different sexual orientations and ensures confidentiality. The guidelines recommend first assessing preferred gender identity, followed by assigned sex at birth, and then sexual orientation to determine next steps in preventive health measures.55
Studies have found that 0.5% to 8.4% of college women and 0.6% to 0.7% of college men have been raped and that 1.8% to 34% of college women (most studies found more than 20%) and 4.8% to 31% of college men have had unwanted sexual contact.57 Physicians asking about violence increases the likelihood that students will be willing to report violent relationships.58
The 2019 ACHA survey notes that 82% of students describe themselves as heterosexual. Other students identify as asexual (0.7%), bisexual (8.8%), gay (2%), lesbian (1.3%), pansexual (1.6%), queer (1.2%), and questioning (1.9%).2 Table 5 lists some available resources for physicians who care for these students.
TABLE 5. Resources for Clinicians Who Care for College Students

| Caring for LGBTQ patients GLMA: Health Professionals Advancing LGBTQ Equality http://www.glma.org/index.cfm?nodeid=1 LGBT National Help Center: LGBT national hotline https://www.glbthotline.org/national-hotline.html The Trevor Project https://www.thetrevorproject.org/ Immunization schedules American Academy of Family Physicians https://www.aafp.org/patient-care/public-health/immunizations/schedules.html Centers for Disease Control and Prevention: Advisory Committee on Immunization Practices https://www.cdc.gov/vaccines/schedules/hcp/index.html Meningococcal ACWY Vaccine https://www.immunize.org/catg.d/p2018.pdf | Transition to college (from childhood model to adult model) American College Health Association: COVID-19 resources https://www.acha.org/ACHA/Resources/Topics/2019_Novel_Coronavirus_2019-nCoV.aspx Centers for Disease Control and Prevention: tips for college health and safety https://www.cdc.gov/healthequity/features/college/index.html Food finder https://foodfinder.us Got transition: youth and young adults https://www.gottransition.org/ NCAA: 2020–21 NCAA banned substances http://www.ncaa.org/sport-science-institute/topics/2019-20-ncaa-banned-substances Veterans Student Veterans of America http://www.studentveterans.org |
LGBTQ = lesbian, gay, bisexual, transgender, queer; NCAA = National Collegiate Athletic Association.
This article updates a previous article on this topic by Unwin, et al.59
Data Sources: Specific evidence-based research on college students is relatively limited. PubMed was used as the primary literature search engine. Key words were college student and university student, plus selected content (e.g., alcohol, tobacco). Key sources of data: American College Health Association, review articles in American Family Physician, and federal reports on selected content. Search dates: May, August, and December 2020; May 29, 2021.
The opinions and assertions contained herein are the private views of the authors and are not to be construed as official or as reflecting the views of the U.S. Army, Navy, or Air Force Medical Departments; the U.S. Army, Navy, Air Force, or Public Health Service; or Carilion Clinic.

