Case Scenario
A 58-year-old man, J.D., with a history of hypertension and tobacco use comes to my office to discuss his laboratory results. J.D. had a lipid panel drawn before the visit and wants to know whether he has high cholesterol. I use the American College of Cardiology/American Heart Association (ACC/AHA) 2013 atherosclerotic cardiovascular disease (ASCVD) risk estimator to evaluate the appropriateness of statin therapy in this patient.1 Based on the calculator's components for race, I ask J.D. whether he identifies as African American, White, or Other.
J.D. is confused by the categories offered and responds that he is Puerto Rican. The patient adds, “I have relatives who are Black, and I have relatives who are Spanish.” J.D. wants to know why the clinical calculator does not include multiracial people and why race is relevant to cardiovascular health.
Commentary
The use of race in clinical decision-making is a source of controversy in U.S. modern medicine. Definitions of race are inconsistent throughout the medical literature and in medical education, and most experts in biology and social sciences agree that race has a limited biologic basis and is actually a social concept influenced by culture and politics, not genetics.2,3
However, the use of race as a descriptor persists in clinical algorithms designed to aid decision-making in patient care.4 Race is used as a variable in clinical calculators in a variety of many specialties, ranging from predictors of in-hospital heart failure mortality to the likelihood of success of a vaginal birth after a previous cesarean delivery.5,6
The reasons for inclusion of race as a variable in clinical calculators are complex. The designers of the 2013 ACC/AHA calculator described in this case used data from several community-based cohorts that included adults identified as African American or White with at least 12 years of follow-up. Data from other racial and ethnic groups were insufficient, which is why they are not included in the final calculator.1
Using calculators that force physicians to place their patients into one of several non-overlapping racial categories can significantly change clinical management. For example, if the patient in the case scenario is categorized as White, the 10-year ASCVD risk is estimated as 5.8%; if the patient is categorized as Other, it is 9.6%. If the patient is categorized as African American, the ASCVD risk jumps to 17.7%.1
It is unlikely that a professional consensus about the role of race in clinical algorithms will occur in the immediate future. It is also unlikely that researchers can immediately develop acceptable replacements for every algorithm that includes race. Therefore, because many of these calculators remain helpful to physicians, a framework for addressing these complex issues with patients is provided.
Consider Race with Caution
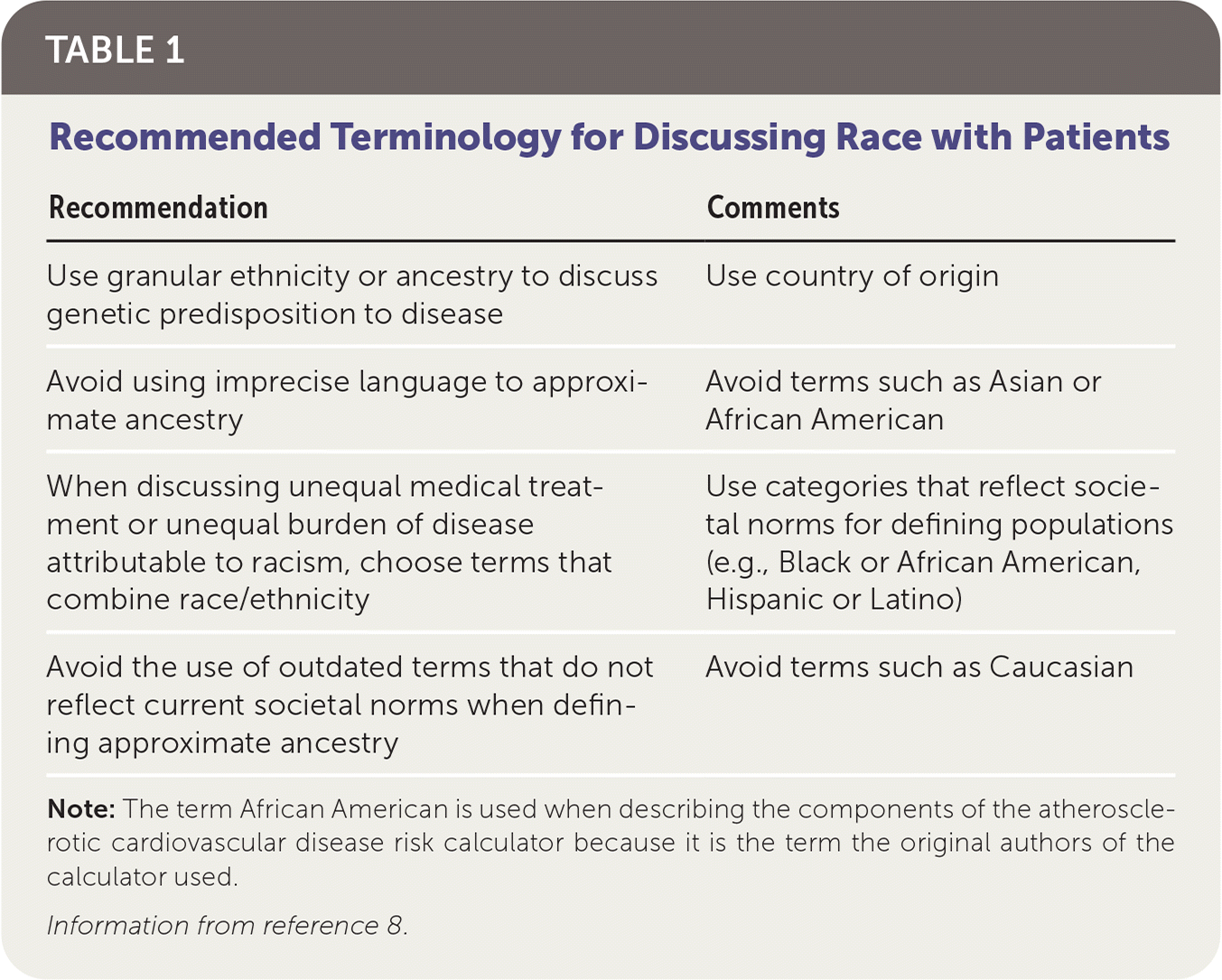
Physicians are encouraged to exercise caution when using race as a marker of genetic ancestry because no meaningful relationship may exist between the two categories. See the editorial in a previous issue of American Family Physician that addressed the dangers of practicing race-based medicine.7 Table 1 provides recommendations for terminology on discussing race with patients.8
TABLE 1. Recommended Terminology for Discussing Race with Patients
| Recommendation | Comments |
|---|---|
| Use granular ethnicity or ancestry to discuss genetic predisposition to disease | Use country of origin |
| Avoid using imprecise language to approximate ancestry | Avoid terms such as Asian or African American |
| When discussing unequal medical treatment or unequal burden of disease attributable to racism, choose terms that combine race/ethnicity | Use categories that reflect societal norms for defining populations (e.g., Black or African American, Hispanic or Latino) |
| Avoid the use of outdated terms that do not reflect current societal norms when defining approximate ancestry | Avoid terms such as Caucasian |
Note: The term African American is used when describing the components of the atherosclerotic cardiovascular disease risk calculator because it is the term the original authors of the calculator used.
Information from reference 8.
Self-reported race is a complex phenomenon that typically relies on the subjective interpretation of a combination of information, including behavioral, cultural, and societal norms. Cases have been reported of self-identified Black patients who were found to have evidence of European ancestry, and some self-identified White patients who identify as being of European ancestry have evidence of mixed African ancestry.9
In reinforcing the false idea of race as a fixed genetic category, the use of race in clinical algorithms may further propagate racism and bias. Critics also argue that the use of race in many widely employed clinical algorithms may exacerbate racial disparities. For example, the use of race correction in the calculation of glomerular filtration rate may systematically underestimate that measurement in Black patients, leading to delayed treatment or decreased likelihood of kidney transplant.10
Using race as a blunt—and often inaccurate—proxy for genetic ancestry is inadequate, and finding more specific genetic markers for risk of cardiovascular disease (CVD) is an area of ongoing research. CVD is complex; however, it is rarely monogenic. Currently, the use of genetic testing to predict primary cardiovascular events is still investigational and offers little benefit over the evaluation of traditional risk factors, such as those factors included in the ACC/AHA calculator.11
Consider Alternative Factors to Evaluate Risk
There are alternatives to using the 2013 ACC/AHA ASCVD calculator to evaluate the risk of a primary cardiovascular event, but each has strengths and weaknesses. Considering these alternative approaches to risk stratification may be particularly useful for individuals from cohorts that were not studied in the original data sets that contributed to the development of the calculator, including people of Hispanic or Asian descent.
Physicians are encouraged to use their clinical judgment and shared decision-making around pharmacologic prevention of coronary artery disease. In discussions with patients, physicians can address the following risk factors to evaluate those who are at higher risk of cardiovascular events. Some, but not all, of these variables are included in the existing ASCVD calculator.
- Older age
- Cisgender male sex
- Comorbidities, including hypertension, abnormal cholesterol levels, and diabetes mellitus
- Lifestyle factors, including smoking status, obesity, diet, and physical inactivity
The ACC/AHA endorses the use of coronary artery calcium scoring in its 2018 guidelines as a tool for risk stratification of patients with intermediate or borderline risk of CVD based on the ASCVD calculator.12 Some authors have proposed including aortic pulse-wave velocity, carotid ultrasonography, and ankle-brachial index evaluation, especially in patients with a family history of early-onset peripheral arterial disease.13
However, the U.S. Preventive Services Task Force (USPSTF) found insufficient evidence to support coronary artery calcium scoring and ankle-brachial index assessment and recommended against the use of carotid ultrasonography for this purpose.14,15 The USPSTF does not weigh in on the use of aortic pulse-wave velocity as a screening modality for CVD. Family physicians should watch for changing evidence and guideline recommendations.
Use Social Determinants of Health as an Alternative to Demographics
Some proponents of including race in clinical algorithms argue that taking a patient's race into account helps identify individuals at risk of disease and encourages physicians to address that risk appropriately.16 Race may serve as a useful proxy for other risk factors of disease that have a biologic basis. For example, scholars theorize that the experience of racism can lead to chronic stress, which in turn may increase the chances of developing a variety of diseases.17,18
Instead of race, some authors have proposed using a social determinants of health score to estimate the risk of developing CVD.19 There is biologic plausibility that social determinants of health contribute to the risk of developing CVD through a variety of mechanisms, including exposure to chronic stress, access to heart-healthy foods, and access to green spaces for regular exercise.20
Although use of a social determinants of health calculator has not been validated, physicians may help reduce their patients' risk of CVD by inquiring about these determinants and working with interprofessional teams (i.e., social workers, nutritionists, mental health professionals) to help address social risk factors.
Case Resolution
The patient's question about the use of the ASCVD calculator offers an opportunity for shared decision-making. The physician in the case scenario can provide a rationale for skepticism about the use of race in clinical algorithms and offer the patient an alternative risk evaluation based on select elements of the ASCVD calculator that have a more established link to coronary artery disease. The physician can also include social determinants of health in the assessment because these have a significant impact on patient morbidity and mortality.

