Clinical Question
Are educational, supportive, behavioral, or mixed intervention strategies effective at increasing compliance with continuous positive airway pressure (CPAP) in patients with obstructive sleep apnea (OSA)?
Evidence-Based Answer
Behavioral interventions increase CPAP use (mean difference [MD] = 1.31 hours per night; 95% CI, 0.95 to 1.66) compared with usual care. These interventions also increase CPAP adherence, measured by participants using their machine four or more hours per night, from 371 to 501 per 1,000 patients (number needed to treat [NNT] = 8; 95% CI, 5 to 23). Supportive interventions may slightly increase CPAP use (MD = 0.70 hours per night; 95% CI, 0.36 to 1.05) vs. usual care, and they increase CPAP adherence from 601 to 717 per 1,000 patients (NNT = 9; 95% CI, 5 to 56). The benefits of educational and mixed interventions are unclear because of low-quality evidence.1 (Strength of Recommendation: A, based on consistent, good-quality patient-oriented evidence.)
Practice Pointers
OSA causes sleep fragmentation and can lead to excessive daytime sleepiness, mood changes, and impairments in cognition, memory, and driving competence. OSA increases the risk of cardiovascular, cerebrovascular, and metabolic morbidity.2 CPAP is first-line treatment for OSA, and consistent use can improve sleep quality and associated symptoms.3 A large systematic review and meta-analysis showed that CPAP had no effect on cardiovascular outcomes in patients with OSA; however, in most randomized controlled trials, patients used CPAP less than four hours per night.4 The effectiveness of CPAP on OSA symptoms directly correlates to duration of compliance, with more than four hours of adherence to therapy demonstrating improvements in sleep quality, daytime sleepiness, fatigue, and depressive symptoms.5
This Cochrane review included 41 studies with 9,005 participants.1 It evaluated the effectiveness of educational, supportive, behavioral, and mixed interventions on CPAP compliance compared with usual care, which was defined as providing background information and general instructions for CPAP use.1 Most participants were CPAP naive. Educational interventions aimed to improve patient knowledge and understanding of OSA in general or CPAP treatment specifically and were delivered in various formats (written, group, video, in-person). Supportive interventions used automated feedback from the CPAP machine that triggered a clinician intervention or scheduled a follow-up visit to encourage CPAP use. Behavioral interventions included motivational enhancement therapy, social cognitive theory, transtheoretical/stages of change model, and cognitive behavior therapy to improve compliance. Mixed interventions were any combination of the previous interventions. The authors used total CPAP hours per night and total number of participants who used the machine four or more hours per night to measure CPAP compliance. Patient-oriented outcomes of daytime sleepiness and quality of life could not be evaluated because of inconsistency in measurement among studies.
Based on high-certainty evidence, behavioral interventions demonstrated a significant benefit (MD = 1.31 more hours per night of CPAP use compared with usual care; 95% CI, 0.95 to 1.66). They also increased the number of participants adhering to therapy, assessed by using their machine for four or more hours per night, from 371 to 501 per 1,000 (NNT = 8; 95% CI, 5 to 23). Patients using behavioral interventions were less likely to withdraw from therapy based on a decrease in study withdrawals from 146 to 101 per 1,000 (NNT = 22; 95% CI, 13 to 33).
Supportive interventions increased CPAP use (MD = 0.70 hours per night; 95% CI, 0.36 to 1.05) and increased adherence to therapy from 601 to 717 per 1,000 participants (NNT = 9; 95% CI, 5 to 56) compared with usual care, although these results were based on moderate- and low-certainty evidence, respectively. The benefits of educational and mixed interventions to improve CPAP compliance were uncertain due to low-quality evidence.
This Cochrane review supports the use of behavioral interventions to improve CPAP compliance. Although the studies used various behavioral intervention techniques, the key concept is to engage or interact with the patient in some way. The American Academy of Sleep Medicine strongly recommends educational interventions and conditionally recommends behavioral and troubleshooting (similar to supportive) interventions.3 The Department of Veterans Affairs/Department of Defense clinical practice guideline also includes recommendations for educational, behavioral, and supportive interventions to improve adherence to CPAP therapy in patients with OSA.6 Both guidelines recommend using these interventions during the initiation phase of CPAP therapy.3,6
SUMMARY TABLE
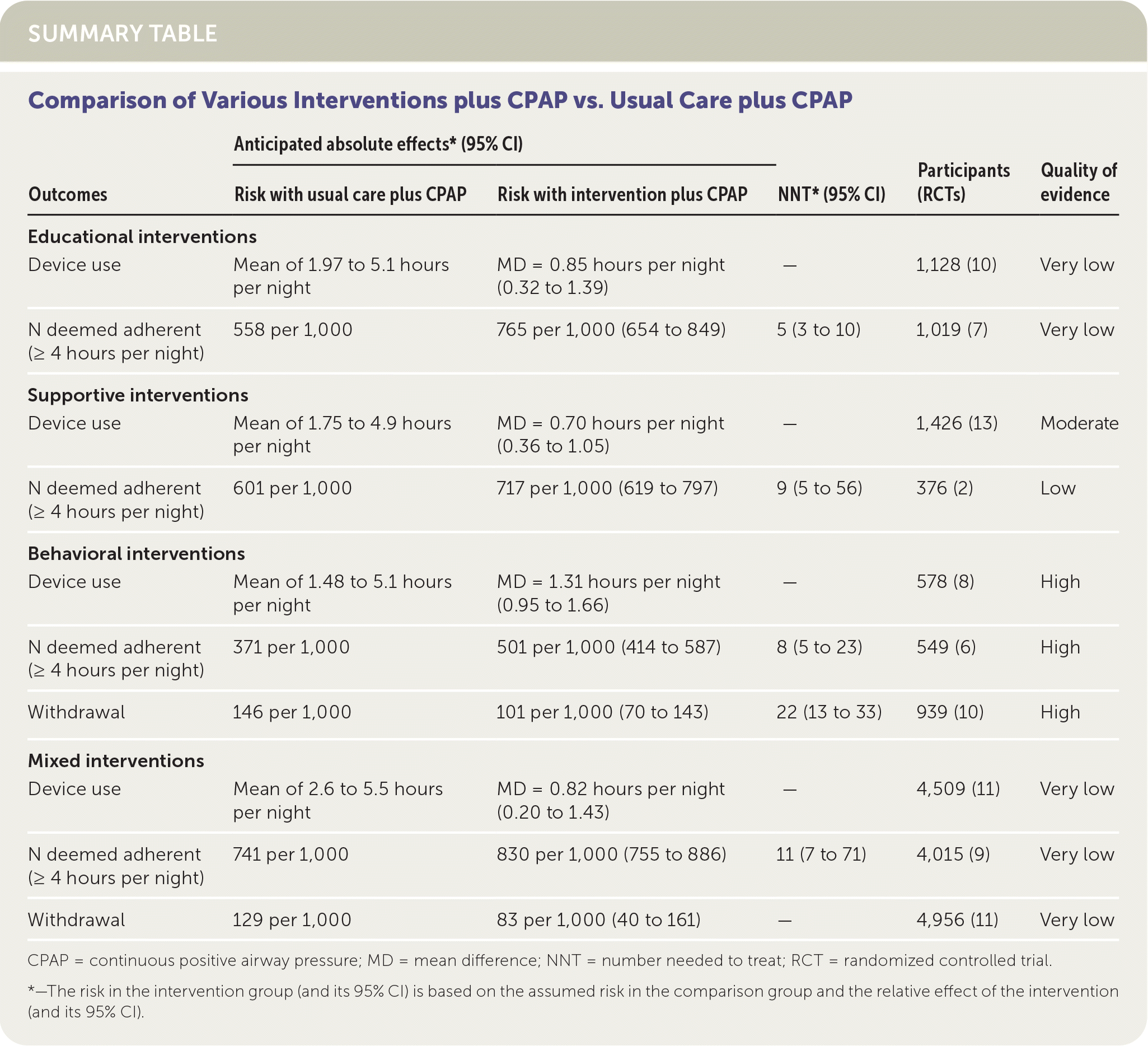
| Outcomes | Anticipated absolute effects* (95% CI) | NNT* (95% CI) | Participants (RCTs) | Quality of evidence | |
|---|---|---|---|---|---|
| Risk with usual care plus CPAP | Risk with intervention plus CPAP | ||||
| Educational interventions | |||||
| Device use | Mean of 1.97 to 5.1 hours per night | MD = 0.85 hours per night (0.32 to 1.39) | — | 1,128 (10) | Very low |
| N deemed adherent (≥ 4 hours per night) | 558 per 1,000 | 765 per 1,000 (654 to 849) | 5 (3 to 10) | 1,019 (7) | Very low |
| Supportive interventions | |||||
| Device use | Mean of 1.75 to 4.9 hours per night | MD = 0.70 hours per night (0.36 to 1.05) | — | 1,426 (13) | Moderate |
| N deemed adherent (≥ 4 hours per night) | 601 per 1,000 | 717 per 1,000 (619 to 797) | 9 (5 to 56) | 376 (2) | Low |
| Behavioral interventions | |||||
| Device use | Mean of 1.48 to 5.1 hours per night | MD = 1.31 hours per night (0.95 to 1.66) | — | 578 (8) | High |
| N deemed adherent (≥ 4 hours per night) | 371 per 1,000 | 501 per 1,000 (414 to 587) | 8 (5 to 23) | 549 (6) | High |
| Withdrawal | 146 per 1,000 | 101 per 1,000 (70 to 143) | 22 (13 to 33) | 939 (10) | High |
| Mixed interventions | |||||
| Device use | Mean of 2.6 to 5.5 hours per night | MD = 0.82 hours per night (0.20 to 1.43) | — | 4,509 (11) | Very low |
| N deemed adherent (≥ 4 hours per night) | 741 per 1,000 | 830 per 1,000 (755 to 886) | 11 (7 to 71) | 4,015 (9) | Very low |
| Withdrawal | 129 per 1,000 | 83 per 1,000 (40 to 161) | — | 4,956 (11) | Very low |
CPAP = continuous positive airway pressure; MD = mean difference; NNT = number needed to treat; RCT = randomized controlled trial.
*—The risk in the intervention group (and its 95% CI) is based on the assumed risk in the comparison group and the relative effect of the intervention (and its 95% CI).
The practice recommendations in this activity are available at http://www.cochrane.org/CD007736.
Editor's Note: The NNTs and CIs reported in this Cochrane for Clinicians were calculated by the authors based on raw data provided in the original Cochrane review.
The views expressed in this article are those of the authors and do not necessarily reflect the official policy or position of the Department of the Navy, the Department of Defense, or the U.S. government.
I am a military service member. This work was prepared as part of my official duties. Title 17 U.S.C. 105 provides that “Copyright protection under this title is not available for any work of the United States Government.” Title 17 U.S.C. 101 defines U.S. government work as a work prepared by a military service member or employee of the U.S. government as part of that person's official duties.

