Onychomycosis is a chronic fungal infection of the fingernail or toenail bed leading to brittle, discolored, and thickened nails. Onychomycosis is not just a cosmetic problem. Untreated onychomycosis can cause pain, discomfort, and physical impairment, negatively impacting quality of life. Onychomycosis should be suspected in patients with discolored nails, nail plate thickening, nail separation, and foul-smelling nails. Accurate diagnosis is important before initiating treatment because therapy is lengthy and can cause adverse effects. A potassium hydroxide preparation with confirmatory fungal culture, periodic acid–Schiff stain, or polymerase chain reaction is the preferred diagnostic approach if confirmative testing is cost prohibitive or not available. Treatment decisions should be based on severity, comorbidities, and patient preference. Oral terbinafine is preferred over topical therapy because of better effectiveness and shorter treatment duration. Patients taking terbinafine in combination with tricyclic antidepressants, selective serotonin reuptake inhibitors, atypical antipsychotics, beta blockers, or tamoxifen should be monitored for drug-drug interactions. Topical therapy, including ciclopirox 8%, efinaconazole 10%, and tavaborole 5%, is less effective than oral agents but can be used to treat mild to moderate onychomycosis, with fewer adverse effects and drug-drug interactions. Nail trimming and debridement used concurrently with pharmacologic therapy improve treatment response. Although photodynamic and plasma therapies are newer treatment options that have been explored for the treatment of onychomycosis, larger randomized trials are needed. Preventive measures such as avoiding walking barefoot in public places and disinfecting shoes and socks are thought to reduce the 25% relapse rate.
Onychomycosis, a chronic fungal infection of the fingernail or toenail bed, is commonly encountered in primary care. Onychomycosis is not just a cosmetic problem. If untreated, it can cause pain, discomfort, and physical impairment, negatively impacting quality of life. This article provides a summary of the best available patient-oriented evidence on the diagnosis and management of this condition.
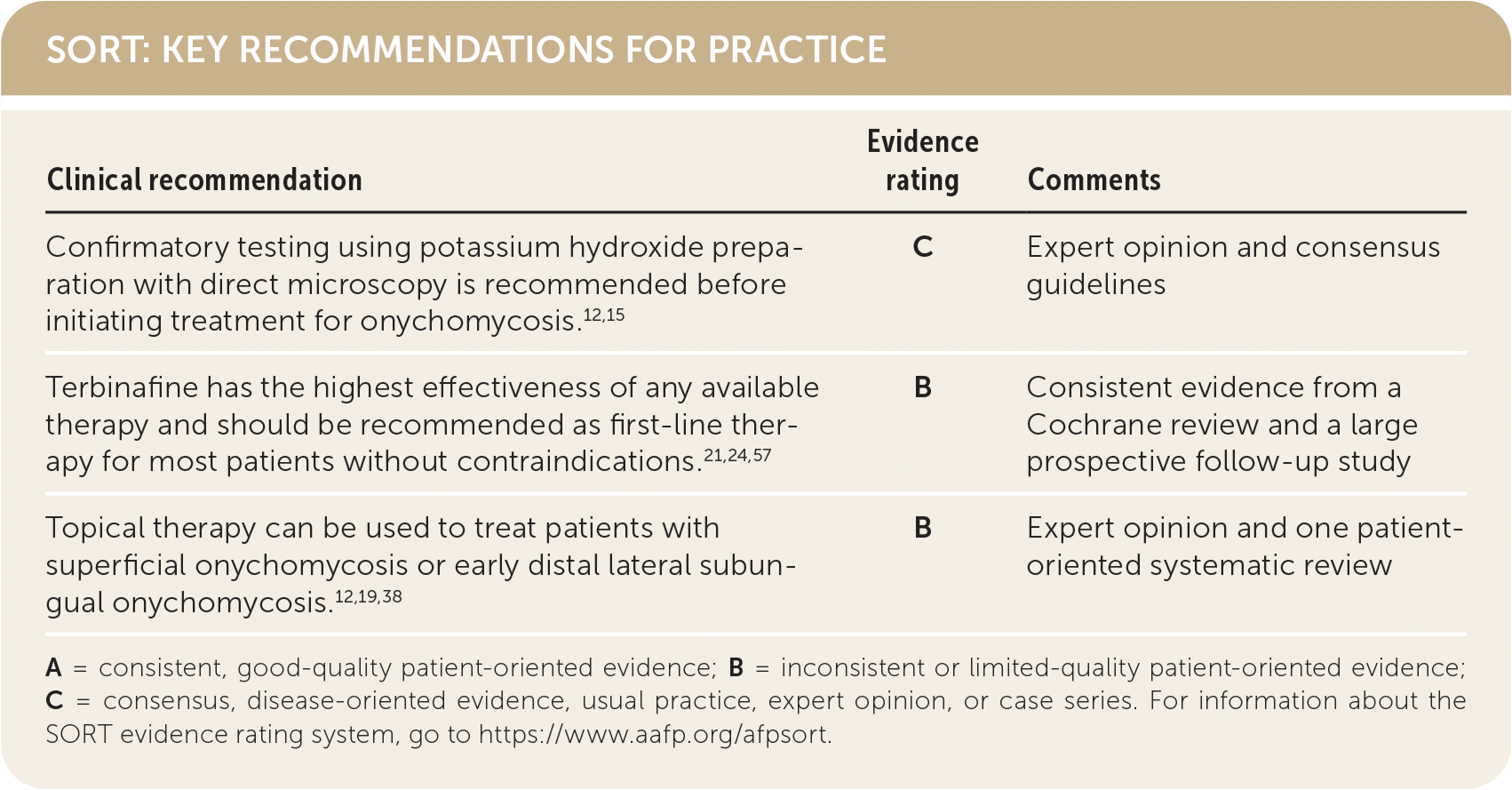
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | Comments |
|---|---|---|
| Confirmatory testing using potassium hydroxide preparation with direct microscopy is recommended before initiating treatment for onychomycosis.12,15 | C | Expert opinion and consensus guidelines |
| Terbinafine has the highest effectiveness of any available therapy and should be recommended as first-line therapy for most patients without contraindications.21,24,57 | B | Consistent evidence from a Cochrane review and a large prospective follow-up study |
| Topical therapy can be used to treat patients with superficial onychomycosis or early distal lateral subungual onychomycosis.12,19,38 | B | Expert opinion and one patient-oriented systematic review |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
BEST PRACTICES IN DERMATOLOGY

| Recommendation | Sponsoring organization |
|---|---|
| Do not prescribe oral antifungal therapy for suspected nail fungus without confirmation of fungal infection. | American Academy of Dermatology |
Source: For more information on the Choosing Wisely Campaign, see https://www.choosingwisely.org. For supporting citations and to search Choosing Wisely recommendations relevant to primary care, see https://www.aafp.org/afp/recommendations/search.htm.
Epidemiology
- The estimated point prevalence of onychomycosis in North America is up to 13.8% for adults and 0.44% for children and adolescents younger than 18 years.1,2
- Age older than 60 years is an important risk factor because of poor peripheral circulation, suboptimal immune function, slower nail growth, and longer exposure to pathogenic fungi.3
- Other risk factors include recurrent nail trauma, tobacco use, and certain comorbidities (diabetes mellitus, obesity, psoriasis, malignancy, HIV, peripheral vascular disease, immunocompromised state).
Pathogenesis
- Dermatophytes cause 70% of onychomycosis infections in the United States, with the remaining 30% caused by nondermatophyte molds and yeasts.4
- One study showed that 39% of infections were mixed (caused by dermatophytes plus nondermatophyte mold and/or yeast), making diagnosis and treatment challenging.5
Diagnosis
DIFFERENTIAL DIAGNOSIS AND CLINICAL PRESENTATION
- With fungi causing 50% of nail dystrophies, the differential diagnosis for nail abnormalities is large (Table 1).6–10
- Common signs and symptoms of onychomycosis include nails that appear discolored (Figure 1), deformed (Figure 2), hypertrophic, or hyperkeratotic; subungual debris; separation from the nail bed; brittle nails that break easily or crumble (Figure 3); and nails that are foul smelling.
- Onychomycosis is classified into several subtypes based on the phenotypic pattern of nail invasion (Table 2).8,11,12
- Severity is classified as mild, moderate, or severe based on the Onychomycosis Severity Index. This index uses three clinical features to assess severity: area of involvement, proximity of disease to the nail matrix, and presence of dermatophytoma or subungual hyperkeratosis thickness greater than 2 mm.13
TABLE 1. Differential Diagnosis of Nail Abnormalities

| Condition | Frequency of nail involvement (%)* | Nail manifestations |
|---|---|---|
| Skin disorders | ||
| Psoriasis | 50% to 90% | Nail pitting, onycholysis, subungual hyperkeratosis, brownish discoloration (oil stains) or salmon-colored patches |
| Lichen planus | 10% to 16% | Longitudinal grooves and fissures, progressive nail thinning, dorsal pterygium |
| Chronic dermatitis | 11% | Nail pitting, Beau lines (transverse grooves) |
| Infectious conditions | ||
| Paronychia | 100% | Inflammation of the nail bed associated with erythema, edema, and pain at the proximal nail folds |
| Warts | — | Nodules cause onycholysis or longitudinal grooves in the nail plate and splinter hemorrhages |
| Herpetic whitlow | — | Hemorrhagic and purpuric nail lesions |
| Trauma | ||
| Onychodystrophy | — | Onycholysis, periungual keratosis |
| Tumors | ||
| Bowen disease | 8% | Paronychia, lack of nail growth, onycholysis |
| Melanoma | 0.2% to 7% of cutaneous melanomas | Brownish-yellow discoloration of the nail plate, subungual hyperkeratosis, onychorrhexis |
| Fibroma | — | Smooth, firm, flesh-colored lumps that emerge from the nail folds |
| Other | ||
| Trachyonychia | 100% | Longitudinal ridging; thin, brittle nails; nail pitting; usually involves all 20 nails |
| Yellow nail syndrome | 100% | Yellowish nail discoloration |
*—Data provided if available.
FIGURE 1.
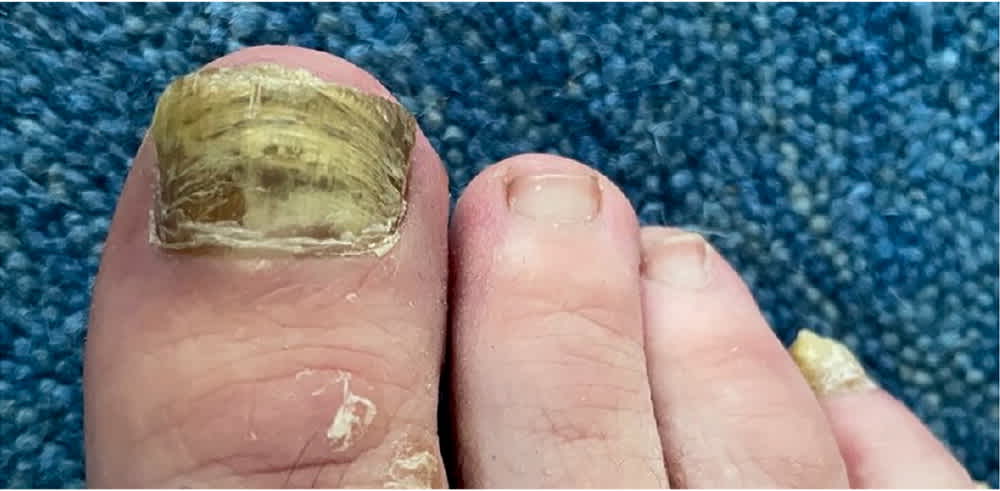
Onychomycosis of the first toenail with superimposed Pseudomonas infection. Note the greenish color of the nail plate.
FIGURE 2.
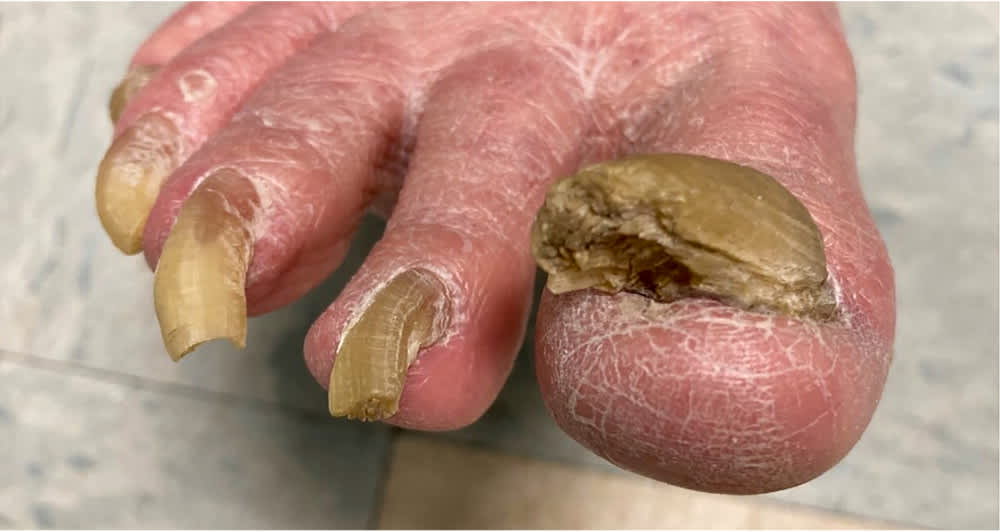
Onychogryphosis (opaque, yellow-brown thickening of the nail plate) with associated gross hyperkeratosis, elongation, and increased curvature due to lack of proper nail care.
FIGURE 3.
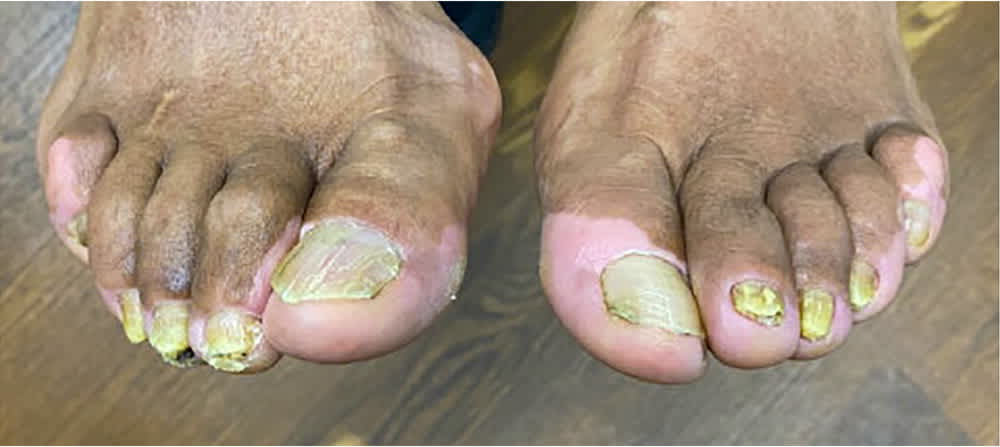
Mixed pattern onychomycosis showing distal lateral subungual onychomycosis and superficial onychomycosis with brittle second and third toenails.
TABLE 2. Onychomycosis Classification
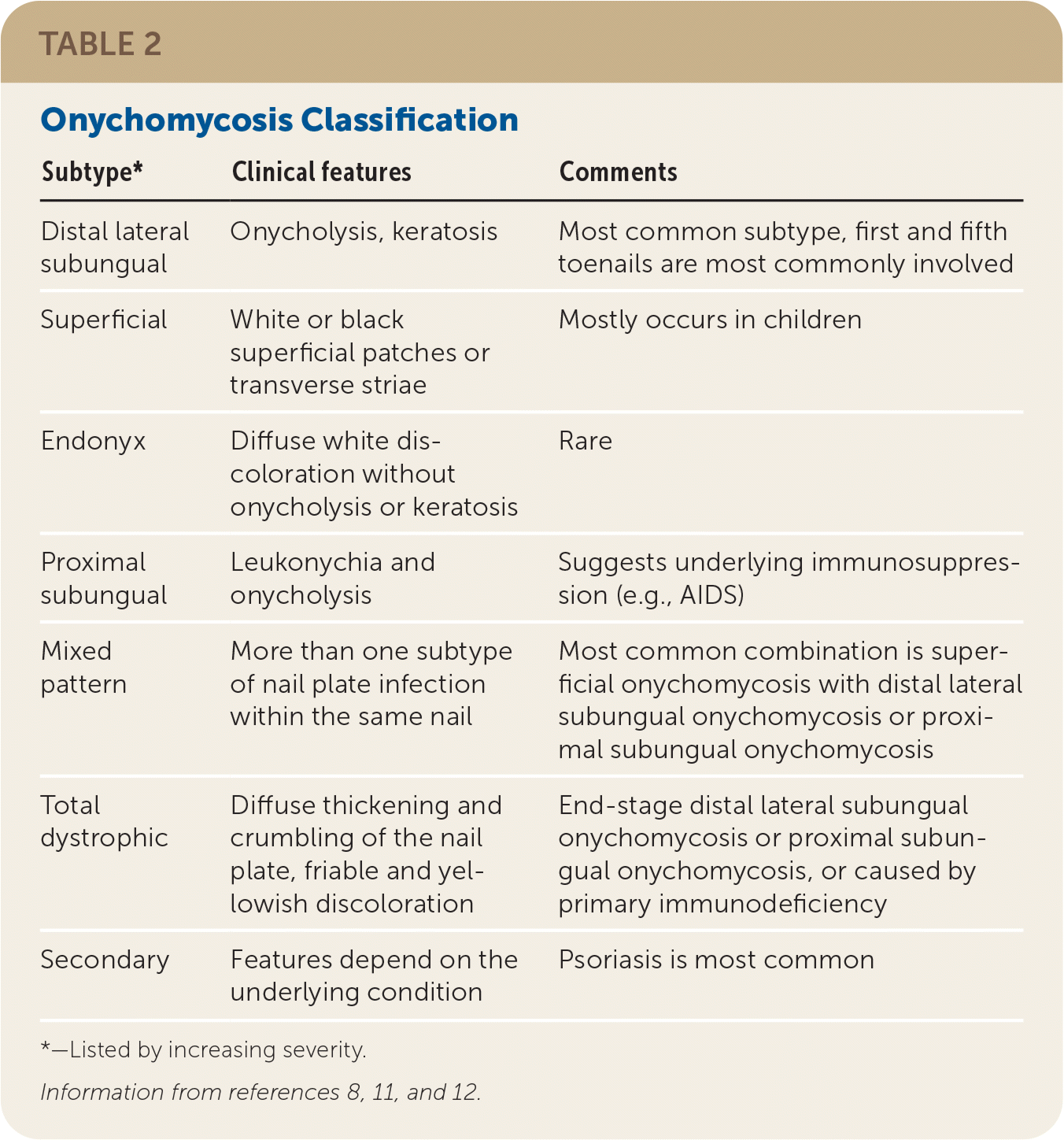
| Subtype* | Clinical features | Comments |
|---|---|---|
| Distal lateral subungual | Onycholysis, keratosis | Most common subtype, first and fifth toenails are most commonly involved |
| Superficial | White or black superficial patches or transverse striae | Mostly occurs in children |
| Endonyx | Diffuse white discoloration without onycholysis or keratosis | Rare |
| Proximal subungual | Leukonychia and onycholysis | Suggests underlying immunosuppression (e.g., AIDS) |
| Mixed pattern | More than one subtype of nail plate infection within the same nail | Most common combination is superficial onychomycosis with distal lateral subungual onychomycosis or proximal subungual onychomycosis |
| Total dystrophic | Diffuse thickening and crumbling of the nail plate, friable and yellowish discoloration | End-stage distal lateral subungual onychomycosis or proximal subungual onychomycosis, or caused by primary immunodeficiency |
| Secondary | Features depend on the underlying condition | Psoriasis is most common |
*—Listed by increasing severity.
DIAGNOSTIC TESTS
- Laboratory confirmation of nail infection is important for accurate diagnosis.14
- A potassium hydroxide (KOH) preparation with direct microscopy is the preferred diagnostic method because it is highly specific, has rapid results, and is cost-effective.12,15 Diagnosis by KOH preparation alone is sufficient for treatment initiation. However, if KOH results are negative and there is high clinical suspicion for onychomycosis, other testing may be performed to confirm the diagnosis. Table 3 includes the accuracy of diagnostic testing methods.16,17
- Fungal culture of nail clippings or subungual debris allows for species differentiation but is limited by cost and the time it takes to get results. Biopsy and periodic acid–Schiff stain of nail clippings can help assess the degree of nail plate involvement. Polymerase chain reaction can also confirm the diagnosis but is more expensive than other tests.15–17
- Because samples should be taken from the most proximal area of onycholysis (Figure 4), the nail plate may need to be trimmed to reveal this area.
- Diagnostic testing is generally recommended before initiating treatment, but empiric treatment with terbinafine can be considered if testing is cost prohibitive.18
TABLE 3. Accuracy of Diagnostic Testing for Onychomycosis
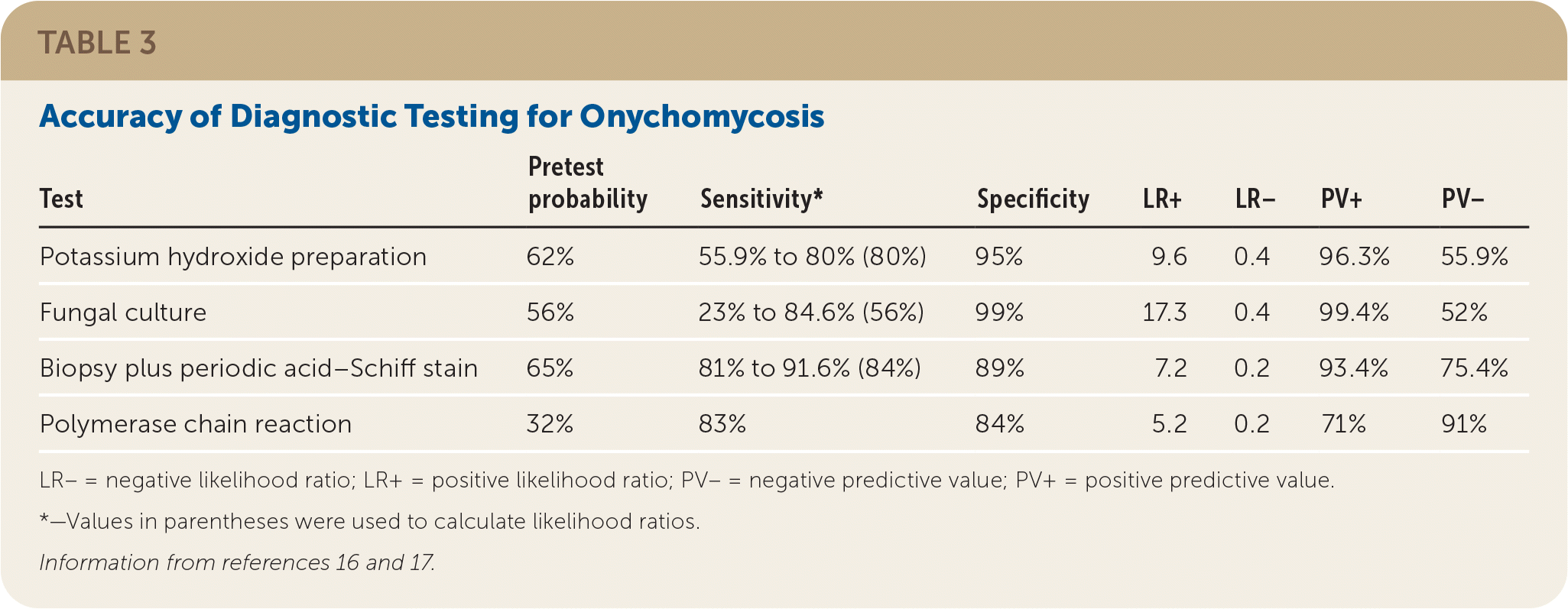
| Test | Pretest probability | Sensitivity* | Specificity | LR+ | LR− | PV+ | PV− |
|---|---|---|---|---|---|---|---|
| Potassium hydroxide preparation | 62% | 55.9% to 80% (80%) | 95% | 9.6 | 0.4 | 96.3% | 55.9% |
| Fungal culture | 56% | 23% to 84.6% (56%) | 99% | 17.3 | 0.4 | 99.4% | 52% |
| Biopsy plus periodic acid–Schiff stain | 65% | 81% to 91.6% (84%) | 89% | 7.2 | 0.2 | 93.4% | 75.4% |
| Polymerase chain reaction | 32% | 83% | 84% | 5.2 | 0.2 | 71% | 91% |
LR− = negative likelihood ratio; LR+ = positive likelihood ratio; PV− = negative predictive value; PV+ = positive predictive value.
*—Values in parentheses were used to calculate likelihood ratios.
FIGURE 4.
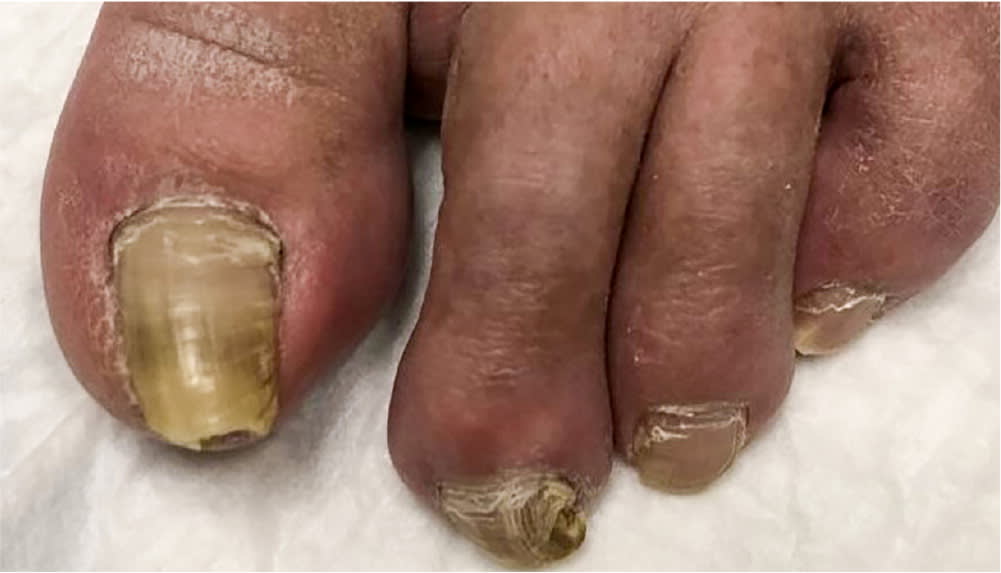
Onycholysis of the first toenail.
Treatment
INDICATIONS FOR MEDICAL THERAPY
- Indications for oral and topical therapy are listed in Table 4.12,19 Shared decision-making based on disease severity, length of treatment, cost, comorbidities, risk of drug-drug interactions, adverse effects, and patient preference should be used before initiating treatment. The type of treatment depends on clinical features and the degree of nail involvement.
- Onychomycosis can have a significant impact on quality of life and will progress if left untreated.20
TABLE 4. Indications for Topical vs. Oral Treatment of Onychomycosis

| Topical |
| Superficial onychomycosis |
| Distal lateral subungual onychomycosis affecting < 50% of the nail plate surface area without matrix involvement |
| Three or fewer nails affected |
| Prevention of recurrence or reinfection |
| Oral |
| Proximal subungual onychomycosis, total dystrophic onychomycosis, or presence of dermatophytoma |
| Distal lateral subungual onychomycosis affecting ≥50% of the nail plate surface area with matrix involvement |
| More than three nails affected |
| No response to topical treatment after six months |
ORAL THERAPY
- Oral therapy is the most effective treatment for onychomycosis of any severity.21 Oral antifungals have higher cure rates and shorter treatment periods than topical therapy (Table 5).19,22–31
- Terbinafine is the most effective oral agent based on its high clinical cure rate (complete nail clearance) and mycologic cure rate (negative microscopy and culture results) and should be recommended as first-line therapy.21–24 Terbinafine is less expensive than topical agents. Chronic or active liver disease is the main contraindication to terbinafine use because of reports of mild and severe liver injuries. The U.S. Food and Drug Administration (FDA) recommends transaminase testing before initiating terbinafine therapy. Subsequent laboratory monitoring is not necessary for immunocompetent patients.32
- Drugs that may interact with concomitant terbinafine therapy include tricyclic antidepressants, selective serotonin reuptake inhibitors, tamoxifen, atypical antipsychotics, and beta blockers.
- Continuous itraconazole (Sporanox) therapy is FDA approved for toenail onychomycosis, and a pulse-dosing regimen (i.e., interval treatment cycles) is approved for fingernail onychomycosis. According to a five-year double-blind prospective study with 144 patients, mycologic and clinical relapse rates are significantly higher with itraconazole than with terbinafine in patients who have severe disease (53% vs. 23% and 48% vs. 21%, respectively; P < .001).24
- A systematic review and network meta-analysis of 22 trials (n = 4,205) using oral antifungal agents for toenail onychomycosis showed that terbinafine is likely more effective than itraconazole in achieving complete cure.33
- Fluconazole (Diflucan), 150 mg weekly for at least six months for fingernails and toenails, may be used as an off-label alternative treatment if the patient is unable to tolerate terbinafine or itraconazole.27,28,31
- Griseofulvin is rarely used because of long treatment duration, higher risk of adverse events, and lower cure rates compared with other medications.34
- A systematic review comparing continuous or pulse-dosing oral antifungal regimens for the treatment of toenail onychomycosis found no significant differences in effectiveness and safety.33
- There are no systemic therapies approved by the FDA for the treatment of onychomycosis in children, although terbinafine and itraconazole are considered off-label treatments.35 Topical therapy can be used in children if there are three or fewer nails involved, less than 50% of the nail plate surface area is affected with no matrix involvement, or oral therapy is contraindicated.36
- It is important for clinicians to counsel patients about realistic expectations for complete cure because fingernails typically take three to six months to completely regrow and toenails can take up to 18 months.
TABLE 5. Onychomycosis Treatment Options and Clinical Cure Rates
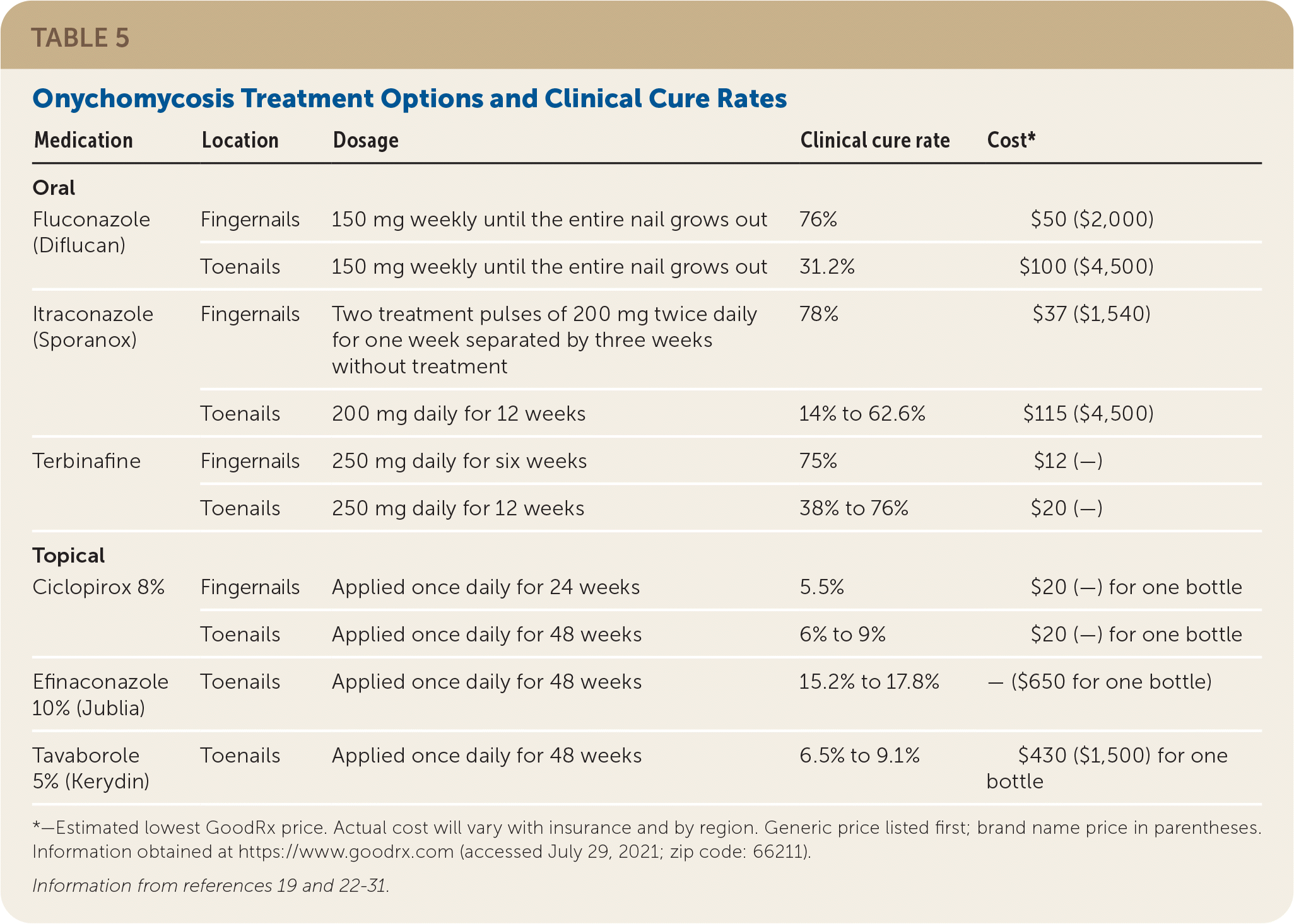
| Medication | Location | Dosage | Clinical cure rate | Cost* |
|---|---|---|---|---|
| Oral | ||||
| Fluconazole (Diflucan) | Fingernails | 150 mg weekly until the entire nail grows out | 76% | $50 ($2,000) |
| Toenails | 150 mg weekly until the entire nail grows out | 31.2% | $100 ($4,500) | |
| Itraconazole (Sporanox) | Fingernails | Two treatment pulses of 200 mg twice daily for one week separated by three weeks without treatment | 78% | $37 ($1,540) |
| Toenails | 200 mg daily for 12 weeks | 14% to 62.6% | $115 ($4,500) | |
| Terbinafine | Fingernails | 250 mg daily for six weeks | 75% | $12 (—) |
| Toenails | 250 mg daily for 12 weeks | 38% to 76% | $20 (—) | |
| Topical | ||||
| Ciclopirox 8% | Fingernails | Applied once daily for 24 weeks | 5.5% | $20 (—) for one bottle |
| Toenails | Applied once daily for 48 weeks | 6% to 9% | $20 (—) for one bottle | |
| Efinaconazole 10% (Jublia) | Toenails | Applied once daily for 48 weeks | 15.2% to 17.8% | — ($650 for one bottle) |
| Tavaborole 5% (Kerydin) | Toenails | Applied once daily for 48 weeks | 6.5% to 9.1% | $430 ($1,500) for one bottle |
*—Estimated lowest GoodRx price. Actual cost will vary with insurance and by region. Generic price listed first; brand name price in parentheses. Information obtained at https://www.goodrx.com (accessed July 29, 2021; zip code: 66211).
TOPICAL THERAPY
- Although topical therapy is less effective and more expensive than oral therapy, it can be used as an alternative first-line treatment in patients with superficial onychomycosis or early distal lateral subungual onychomycosis because of low risks of adverse effects and minimal drug-drug interactions.19,37,38 The recommended duration of topical therapy is 24 weeks for fingernails and 48 weeks for toenails.12 Adverse effects are generally limited to exfoliation, erythema, burning, and dermatitis at the application site.39
- Ciclopirox 8% topical solution is FDA approved for mild to moderate fingernail and toenail onychomycosis. Two randomized controlled trials (RCTs) including 460 total patients showed that compared with vehicle, ciclopirox 8% is better at achieving complete cure at 48 weeks, although only the second study was statistically significant (study 1: 5.5% vs. 0.9%; P = .059 and study 2: 8.5% vs. 0%; P = .001).29
- Once-daily treatment with efinaconazole 10% (Jublia) is an option for mild to moderate onychomycosis. In two phase 3 randomized studies including 1,655 total patients with moderate disease, complete cure rates were higher with efinaconazole 10% compared with vehicle (17.8% vs. 3.3%; P < .001; number needed to treat [NNT] = 7 in study 1 and 15.2% vs. 5.5%; P < .001; NNT = 10 in study 2).40
- In two phase 2 randomized studies including a total of 1,198 patients with moderate disease, tavaborole 5% (Kerydin) had favorable effectiveness compared with ciclopirox, although, again, absolute treatment benefit is low. Complete cure rates compared with vehicle were 6.5% vs. 0.5% (P < .001; NNT = 17) in study 1 and 9.1% vs. 1.5% (P < .001; NNT = 13) in study 2. 41
- Amorolfine 5% lacquer (not available in the United States) can be used for onychomycosis without matrix involvement and for mild distal lateral subungual onychomycosis (Figure 5) that affects up to two nails. A small RCT with 24 patients showed a mycologic cure rate of 8% (P < .001) with once-weekly treatment for nine months.42
FIGURE 5.
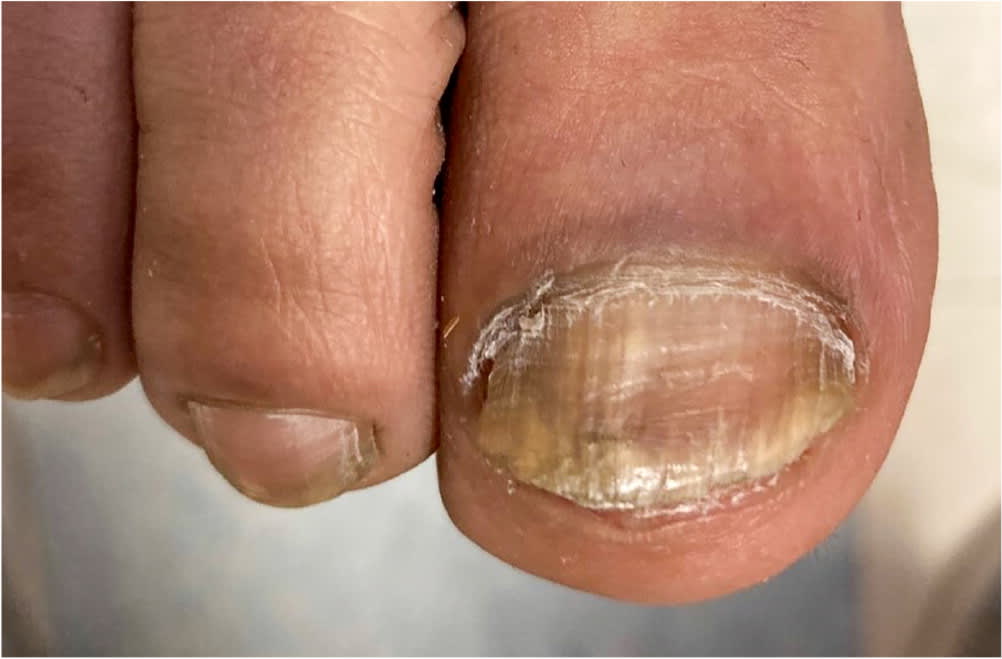
Distal lateral subungual onychomycosis.
SURGICAL THERAPY
- Nail trimming and debridement can be used with oral or topical pharmacologic therapy to increase treatment effectiveness. Surgical and nonsurgical nail removal may be indicated for severe infection or when medical therapy fails.
- Dual-wavelength infrared and fractional carbon-dioxide laser therapy are FDA approved for temporary cosmetic improvement of nails based on low-level evidence and small RCTs.43,44 Combining laser therapy with topical therapy increases overall treatment effectiveness.45
INTEGRATIVE MEDICINE
- Tea tree oil, oregano, vitamin E, oil of bitter orange, vinegar sock soaks, and menthol-camphor ointment (Vicks VapoRub) have demonstrated antifungal activity in small-scale studies.46–49 More robust studies are needed to evaluate the effectiveness of these essential oils against onychomycosis.50,51
NEW TREATMENT OPTIONS
- Although photodynamic and plasma therapies have been explored for the treatment of onychomycosis, larger randomized trials are needed to determine their effectiveness and feasibility for use in the clinical setting.4
- Plasma therapy creates air using pulses of strong electric field that ionize air molecules, generating ozone, hydroxyl radicals, and nitric oxide, which have antifungal properties. A pilot study of 19 participants without a control group showed an overall clinical cure rate of 53.8%.52
- Photodynamic therapy is a noninvasive treatment that combines light-based modalities with photosensitizers. It has been used as an off-label treatment for onychomycosis. A double-dummy RCT including 80 participants with confirmed fungal toenail onychomycosis compared biweekly photodynamic therapy with once-weekly fluconazole, 300 mg, for 24 weeks. Although response to treatment at 24 weeks was greater with photodynamic therapy (90% vs. 40%; P = .002; NNT = 2), this was not a blinded study.53
Prognosis
Prevention
- Based on expert opinion, avoiding walking barefoot in public places may help prevent recurrence.55 Patients should disinfect shoes and socks, keep feet cool and dry, and recognize the early signs of recurrence and reinfection.56
- Immediate treatment of tinea pedis can also delay onychomycosis recurrence because the infected skin can act as a reservoir of infection.57
- Compared with no prophylaxis, twice-weekly prophylaxis with a topical antifungal following terbinafine treatment has been shown to decrease the rate of recurrence (33% vs. 76%; P < .001).58
This article updates previous articles on this topic by Westerberg and Voyack8 and Rodgers and Bassler.59
Data Sources: A PubMed search was completed in Clinical Queries using the key terms onychomycosis, tinea unguium, and nail fungus. The search included meta-analyses, randomized controlled trials, clinical trials, and reviews. Also searched were the Cochrane database, DynaMed, and Essential Evidence Plus. Search dates: November 13, 2020, and August 15, 2021.

