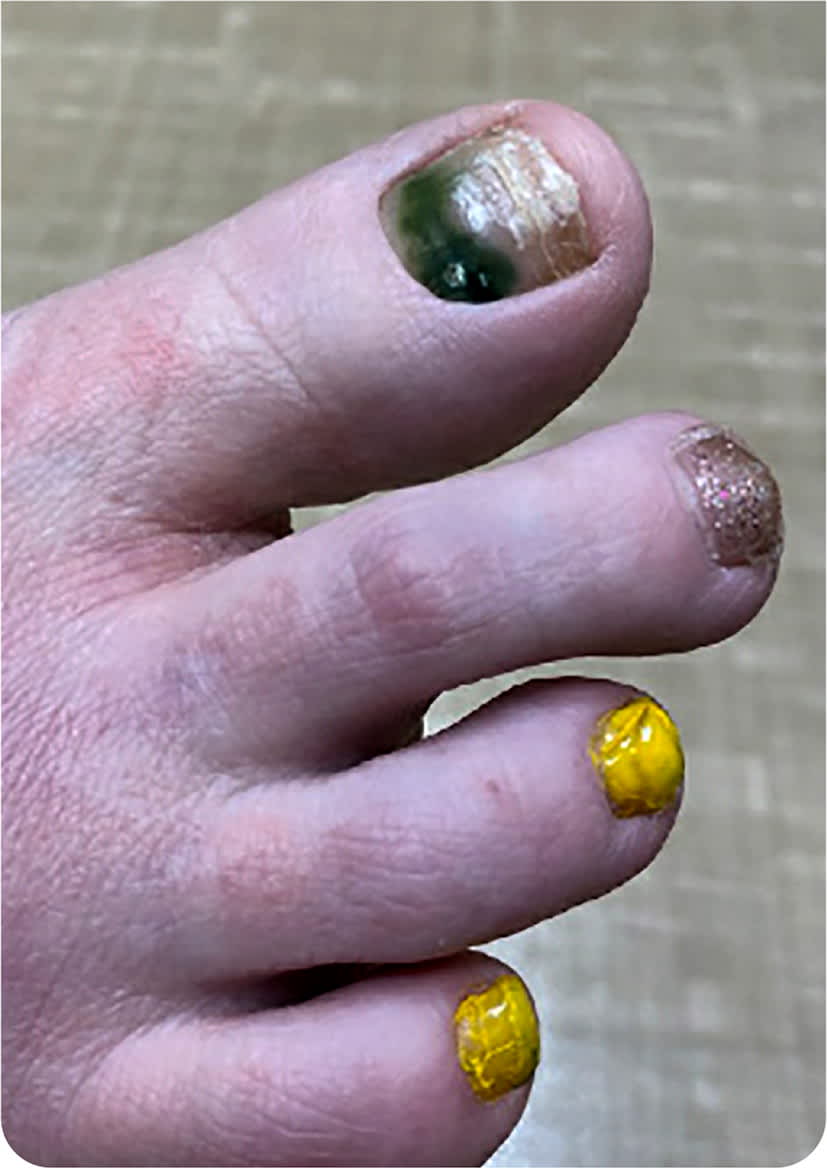
A 37-year-old woman with a history of hypertension presented with green discoloration of her right first toenail (Figure 1). She noticed the color change two days earlier when an artificial nail fell off. She had nail polish and artificial nails on all of her toenails. She had no toe pain, trauma to the area, or associated rash, swelling, or drainage. She was not a runner.
FIGURE 1
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
- A. Acral-lentiginous melanoma.
- B. Melanonychia striata.
- C. Onychomycosis.
- D. Pseudomonas infection.
- E. Subungual hematoma.
Discussion
The answer is D: Pseudomonas infection, or green nail syndrome. A cutaneous Pseudomonas aeruginosa infection results in blue-green biofilm on the surface of the nail. Predisposing factors for green nail syndrome include chronic paronychia, onycholysis, and onychomycosis. These disorders can alter the nail plate, exposing the nail bed to pathogens such as Pseudomonas or Candida.
Occupational history is important because green nail syndrome is common in homemakers, barbers, nail salon technicians, dishwashers, janitors, bakers, and medical personnel because of water or chemical exposure.1 The use of artificial nails and nail polishes may increase the risk of infection, but there is little evidence to confirm this.
Diagnosis of green nail syndrome is based on clinical findings. Additional studies are typically unnecessary. However, if other conditions are suspected, nail culture or biopsy may be indicated. Treatment varies depending on the severity and duration of the condition. The risk of systemic Pseudomonas infection is low in people who are not immunocompromised.2
Treatment consists of trimming the nails, keeping nails dry, and avoiding trauma to the area. Home treatments such as vinegar (acetic acid) soaks or diluted chlorine bleach solutions are often tried by the patient before presentation for medical care, but the effectiveness of these remedies has not been reported.1 Topical antibiotics such as fluoroquinolones or aminoglycosides can be applied to the nail bed. Occasionally, the nail may need to be removed if conservative treatment fails. Oral antibiotics can be used for more severe infections. For this patient, two drops of topical ciprofloxacin were applied twice per day. The green nail discoloration improved after four weeks of topical antibiotics.
Melanonychia striata present as horizontal or longitudinal pigmented bands of the nail, sometimes involving the entire nail plate.3 The causes of melanonychia are extensive, and most are benign. Longitudinal nail bands must be differentiated from subungual or acral-lentiginous melanoma, which can present with a dark pigmented patch or longitudinal band subungually or periungually, with or without nail dystrophy. Melanoma may have darker discolorations, and a green color is less common. Suspicion for melanoma of the nail requires urgent dermatology referral.4
Onychomycosis is an infection of the nail caused by dermatophytes, yeast, or nondermatophyte molds. The nail is thickened and dystrophic. Nail plate destruction can occur if untreated.5 Although topical treatment is available, it is minimally effective, and oral antifungal treatment is usually needed for resolution.
Subungual hematoma is caused by bleeding in the underlying vascular nail bed due to trauma. This is common in the toenails of distance runners and is therefore also referred to as runner's nails. Treatment is generally supportive, although evacuation or nail removal may be required for symptom relief.
SUMMARY TABLE
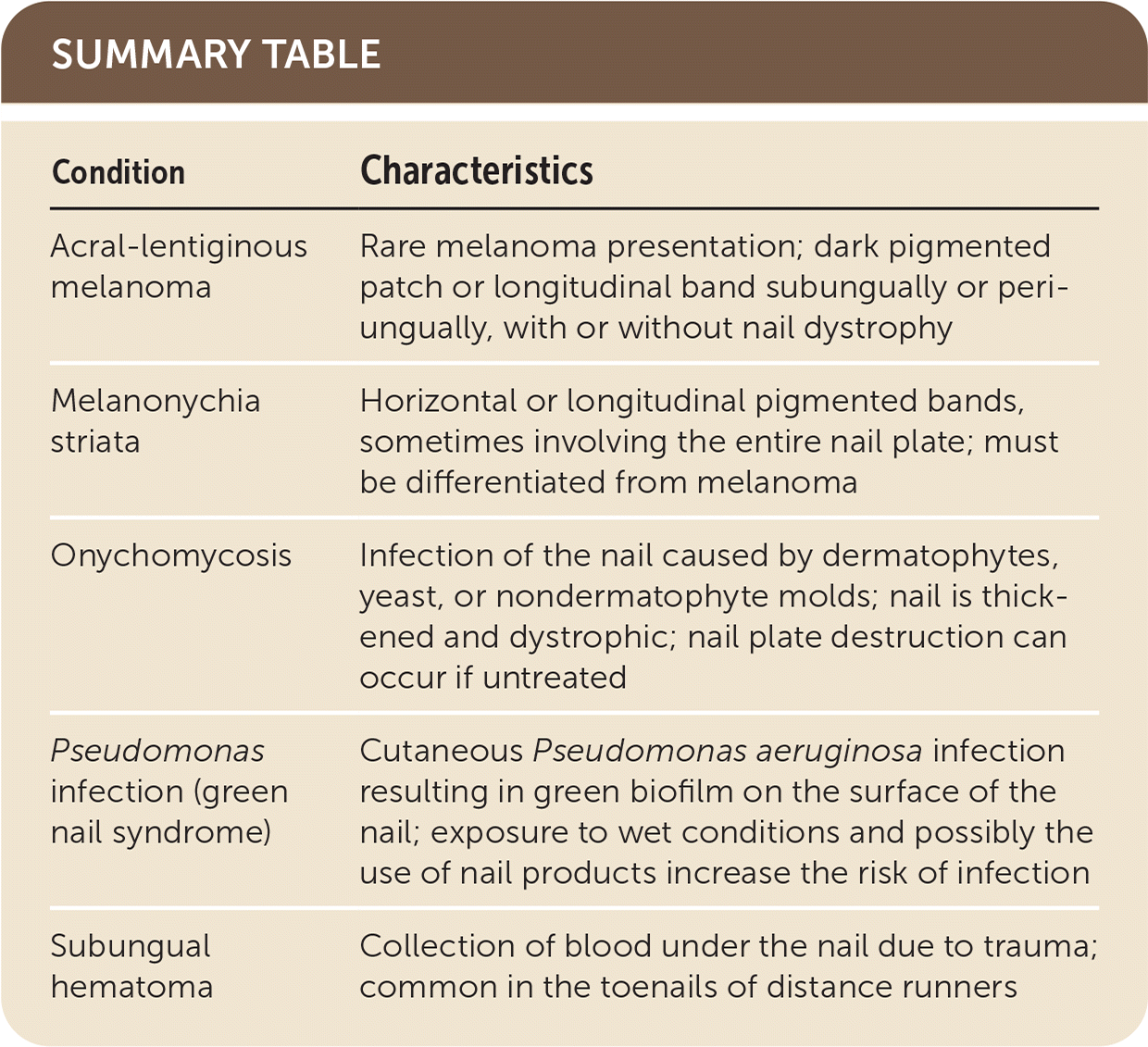
| Condition | Characteristics |
|---|---|
| Acral-lentiginous melanoma | Rare melanoma presentation; dark pigmented patch or longitudinal band subungually or periungually, with or without nail dystrophy |
| Melanonychia striata | Horizontal or longitudinal pigmented bands, sometimes involving the entire nail plate; must be differentiated from melanoma |
| Onychomycosis | Infection of the nail caused by dermatophytes, yeast, or nondermatophyte molds; nail is thickened and dystrophic; nail plate destruction can occur if untreated |
| Pseudomonas infection (green nail syndrome) | Cutaneous Pseudomonas aeruginosa infection resulting in green biofilm on the surface of the nail; exposure to wet conditions and possibly the use of nail products increase the risk of infection |
| Subungual hematoma | Collection of blood under the nail due to trauma; common in the toenails of distance runners |

