Sacroiliac (SI) joint dysfunction is a common cause of low back pain and accurate diagnosis can be challenging. A complete history and physical examination are critical in differentiating other diagnoses that may have similar signs and symptoms. Positive responses to at least three physical provocation tests suggest SI joint dysfunction, and local anesthetic SI joint blocks can also be useful for confirming the SI joint as the source of pain. Conservative treatment consists of a multimodal program combining patient education, pelvic girdle stabilization with focused stretching, and manipulative therapy. These programs can be performed by physical therapists or clinicians trained in manipulative therapy. Pelvic belts may be beneficial in affected postpartum patients. Patients with symptoms that do not improve with conservative management may benefit from interventional treatment options including intra-articular corticosteroid injections, cooled radiofrequency ablation, or SI joint fusion.
The prevalence of sacroiliac (SI) joint dysfunction is approximately 25% in adult patients with chronic low back pain.1 Pain can be unilateral or bilateral but usually not midline.2 Women are more likely to present with SI joint dysfunction than men.3 The SI joint in women is more mobile compared with the SI joint in men, resulting in larger stress, load, and pelvic ligament strain.4 SI joint dysfunction is common in pregnant and postpartum patients.5
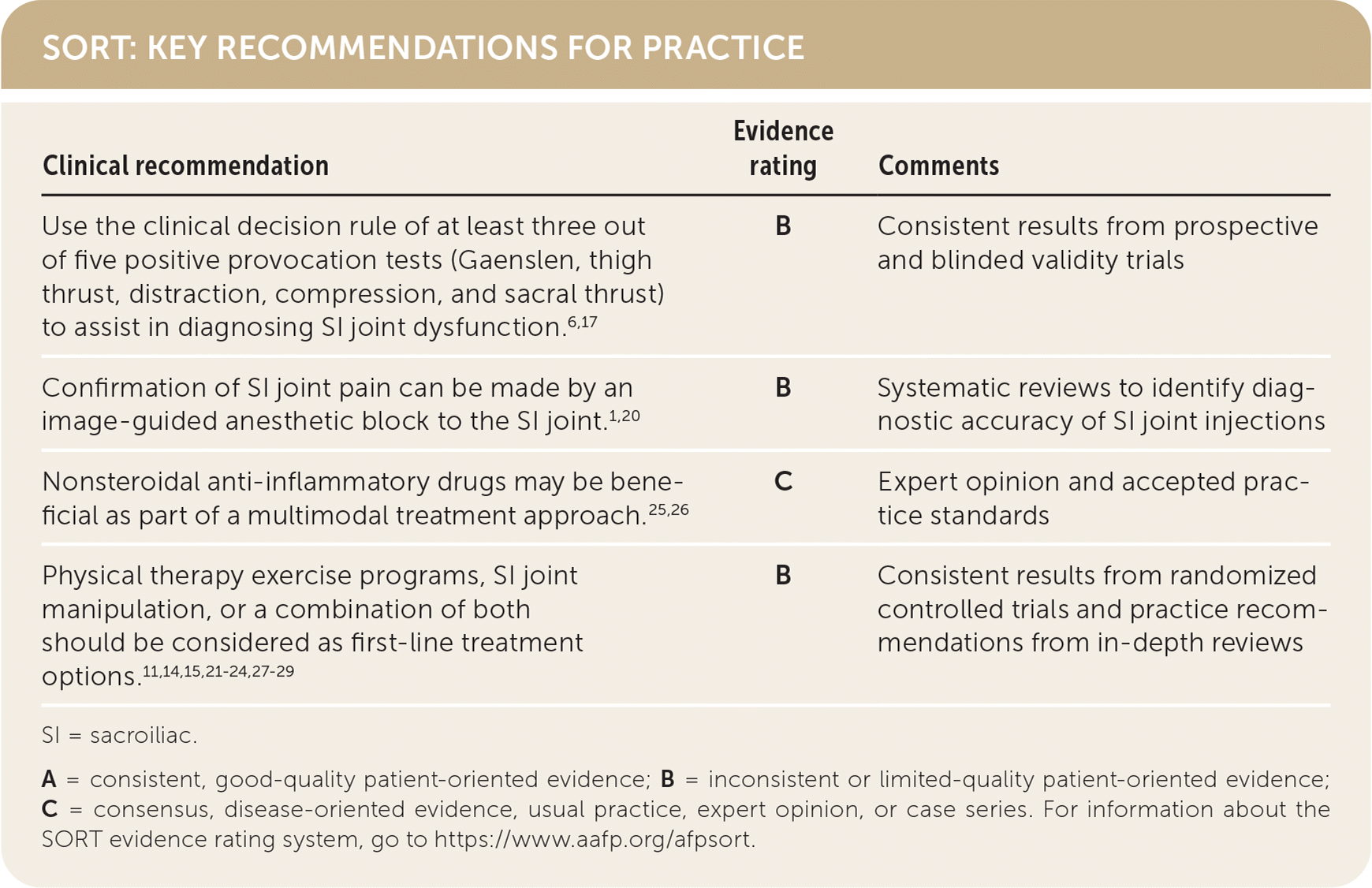
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | Comments |
|---|---|---|
| Use the clinical decision rule of at least three out of five positive provocation tests (Gaenslen, thigh thrust, distraction, compression, and sacral thrust) to assist in diagnosing SI joint dysfunction.6,17 | B | Consistent results from prospective and blinded validity trials |
| Confirmation of SI joint pain can be made by an image-guided anesthetic block to the SI joint.1,20 | B | Systematic reviews to identify diagnostic accuracy of SI joint injections |
| Nonsteroidal anti-inflammatory drugs may be beneficial as part of a multimodal treatment approach.25,26 | C | Expert opinion and accepted practice standards |
| Physical therapy exercise programs, SI joint manipulation, or a combination of both should be considered as first-line treatment options.11,14,15,21–24,27–29 | B | Consistent results from randomized controlled trials and practice recommendations from in-depth reviews |
SI = sacroiliac.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Etiology and Differential Diagnosis
The SI joint serves as a shock absorber and transfers vertical loads from the lumbar spine to the lower extremities during bending movements. The etiology of SI joint dysfunction is not well understood. The SI joint may be the primary source of pain, or dysfunction at the joint or surrounding structures may affect the joint’s load transfer function and produce a painful stimulus.6
SI joint dysfunction can be associated with osteoarthritis or inflammatory conditions such as ankylosing spondylitis, posttraumatic arthritis, and other spondyloarthropathies.7 Similarly, mechanical faults at the pubic symphysis or SI joint can result in pelvic asymmetry or joint instability. Nonoptimal load transfer is seen in patients with SI joint stiffness (hypomobility) and patients with insufficient pelvic girdle stability (hypermobility).8 Table 1 presents the differential diagnoses of conditions with similar or overlapping signs and symptoms of SI joint dysfunction.9–11
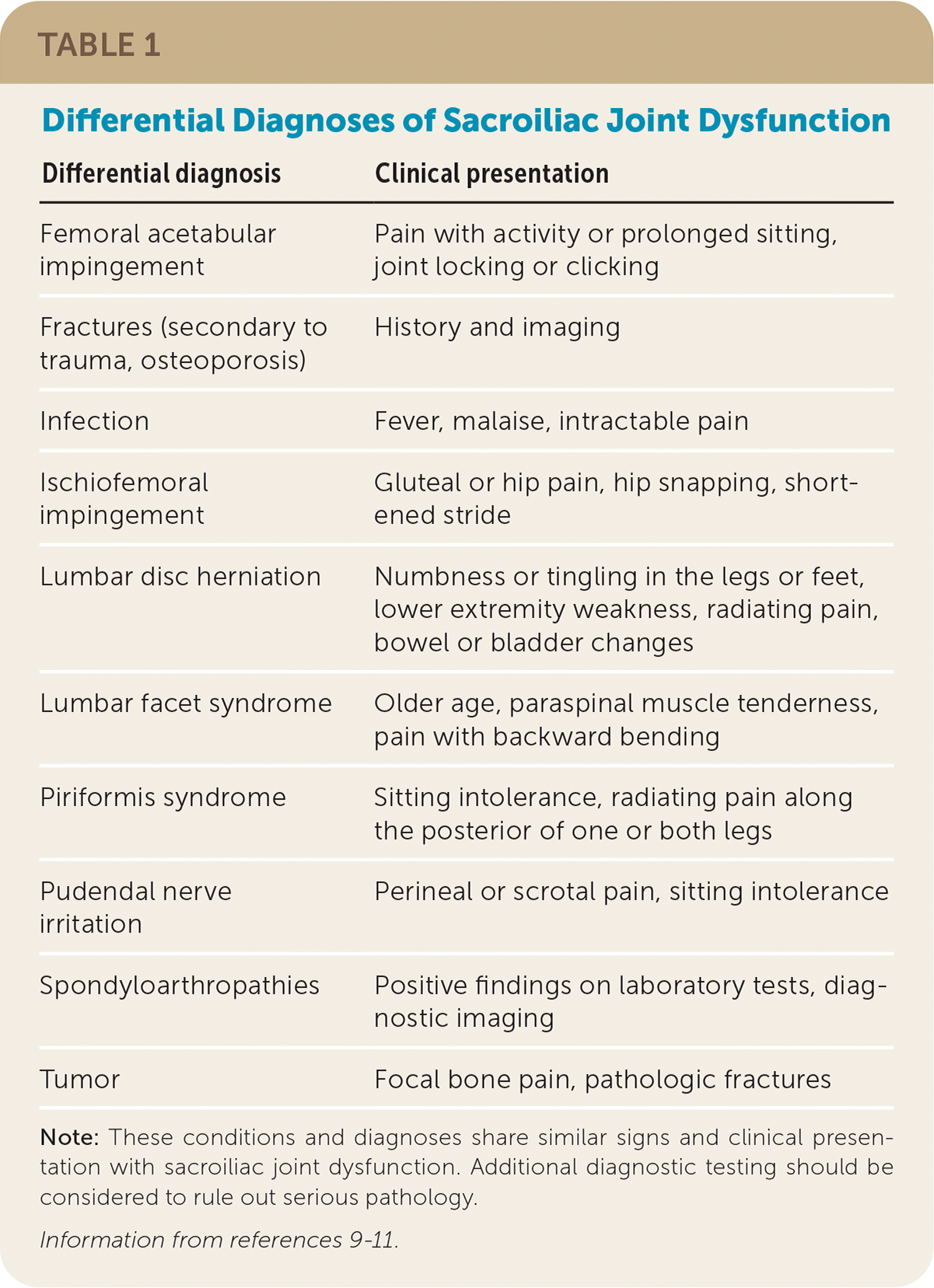
TABLE 1. Differential Diagnoses of Sacroiliac Joint Dysfunction
| Differential diagnosis | Clinical presentation |
|---|---|
| Femoral acetabular impingement | Pain with activity or prolonged sitting, joint locking or clicking |
| Fractures (secondary to trauma, osteoporosis) | History and imaging |
| Infection | Fever, malaise, intractable pain |
| Ischiofemoral impingement | Gluteal or hip pain, hip snapping, shortened stride |
| Lumbar disc herniation | Numbness or tingling in the legs or feet, lower extremity weakness, radiating pain, bowel or bladder changes |
| Lumbar facet syndrome | Older age, paraspinal muscle tenderness, pain with backward bending |
| Piriformis syndrome | Sitting intolerance, radiating pain along the posterior of one or both legs |
| Pudendal nerve irritation | Perineal or scrotal pain, sitting intolerance |
| Spondyloarthropathies | Positive findings on laboratory tests, diagnostic imaging |
| Tumor | Focal bone pain, pathologic fractures |
Note: These conditions and diagnoses share similar signs and clinical presentation with sacroiliac joint dysfunction. Additional diagnostic testing should be considered to rule out serious pathology.
History and Physical Examination
Differentiating SI joint dysfunction from other diagnoses presenting with low back pain requires a complete history and physical examination of the spine, pelvic girdle, and hips as well as a review of other systems to rule out red flags such as history of trauma, unexplained weight loss, fever, bowel and bladder changes, cancer, and night pain.6,12,13
Patients with SI joint dysfunction may present with pain that is localized to the area at or just inferomedial to the posterior superior iliac spine as demonstrated in a Fortin finger test (Figure 1) or along the gluteal area, lateral hip, lower extremities, and groin.2,12 Potential aggravating factors and activities that may exacerbate pain from SI joint dysfunction are described in Table 2.3,12
FIGURE 1.
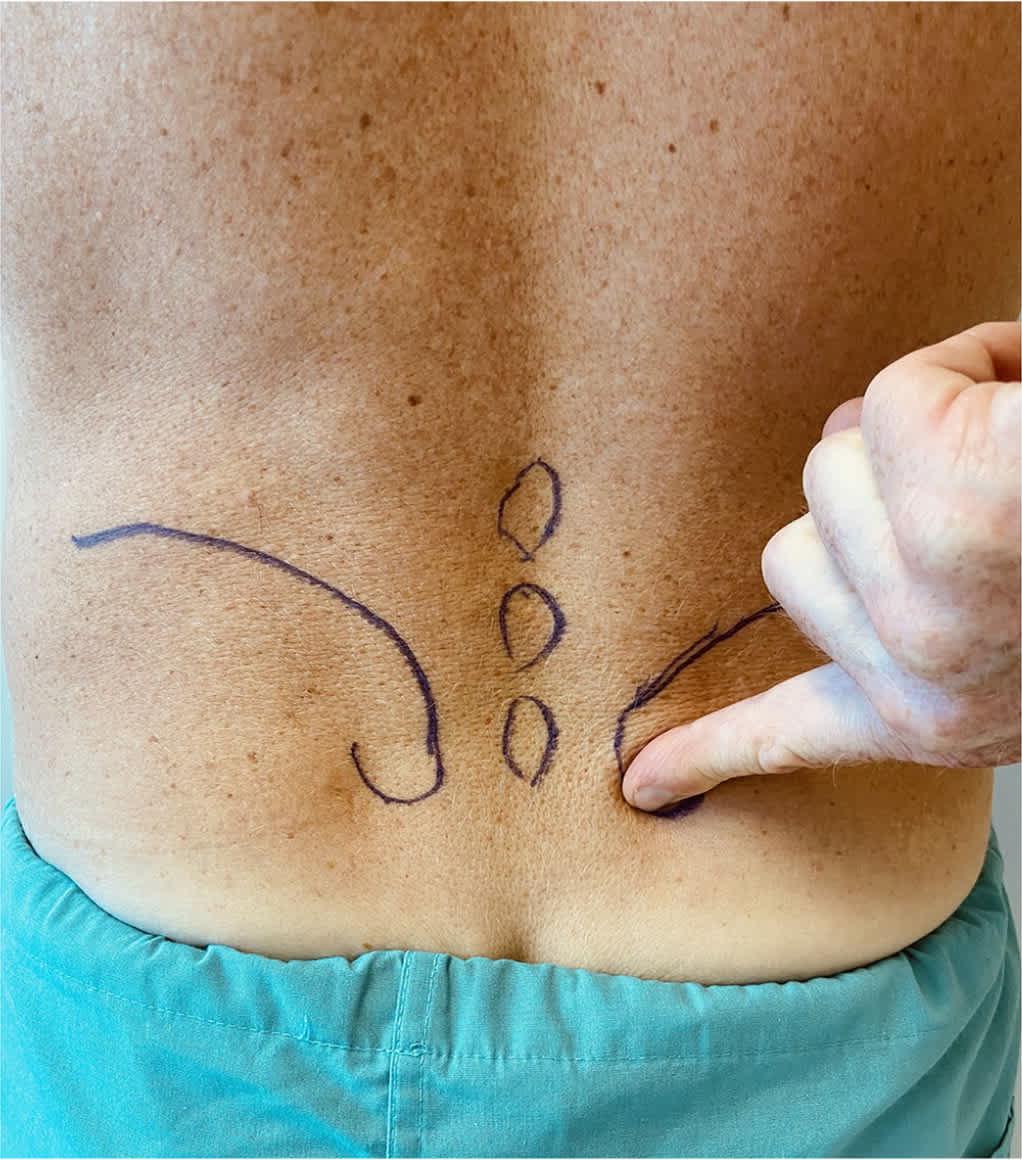
Fortin finger test. The patient points to the area of pain with one finger. The test is positive if the site of pain is within 1 cm of the posterior superior iliac spine. Usually, the pain is inferomedial to the posterior superior iliac spine on the affected side.
TABLE 2. Activities That May Aggravate Pain Associated With Sacroiliac Joint Dysfunction
SI joint dysfunction may be attributed to a variety of causes.12 Traumatic onset commonly occurs with heavy lifting, a fall onto the buttocks, and motor vehicle collisions. A more insidious onset can be caused by recreational activities with repeated weight bearing and shear or torsional forces experienced during sports such as football, gymnastics, and golfing.
A physical examination should include gait analysis (i.e., reporting of pain with walking, shortened stride length, antalgic gait), range of motion, provocation testing, strength, flexibility, and palpation assessments (Table 3).2,3,12,14–16 Lower extremity neurologic screening (i.e., reflexes, sensation, strength, straight leg raise) is helpful when considering differential diagnoses.
TABLE 3. Physical Examination Findings Suggestive of Sacroiliac Joint Dysfunction

| Component | Findings or physical examination response |
|---|---|
| Observation | Asymmetric iliac crest height |
| Asymmetric weight-bearing when standing | |
| Gait | Painful catching or increased pain ipsilaterally during stance phase |
| Decreased hip extension resulting in shortened contralateral stride length | |
| Provocation tests | Three of five positive tests suggest sacroiliac joint dysfunction (Figures 2 through 6) |
| Strength testing | Gluteus medius weakness |
| Flexibility | Iliopsoas tightness |
| Piriformis tightness | |
| Hamstring tightness with gluteal weakness | |
| Palpation | Reported pain at or inferomedial to the posterior superior iliac spine |
Motion and provocation tests can assess the SI joint for dysfunction and pain reproduction6,17 (Figure 2, Figure 3, Figure 4, Figure 5, and Figure 6). A video demonstration is available at https://www.youtube.com/watch?v=8biQsdgdyzA.
FIGURE 2.
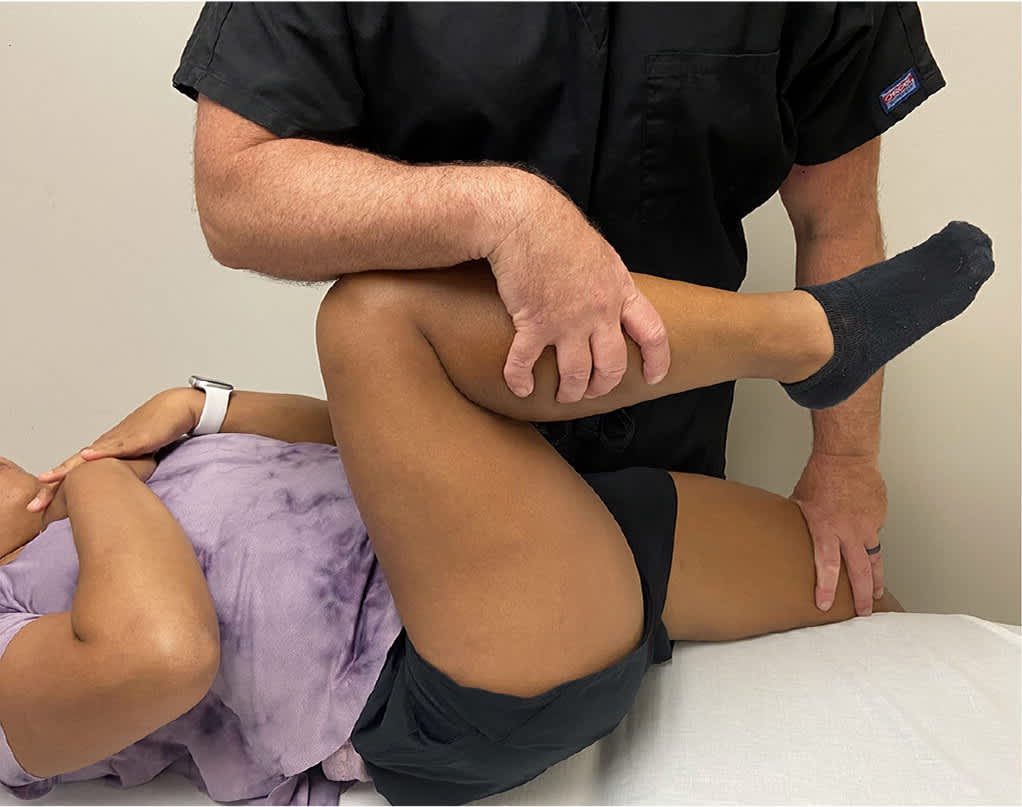
Gaenslen test. The pelvis is loaded by a superior or posterior force applied to the cephalad knee and a posteriorly directed force applied to the caudal knee. The test is positive if pain is reproduced. In this example, the right side is being tested.
FIGURE 3.
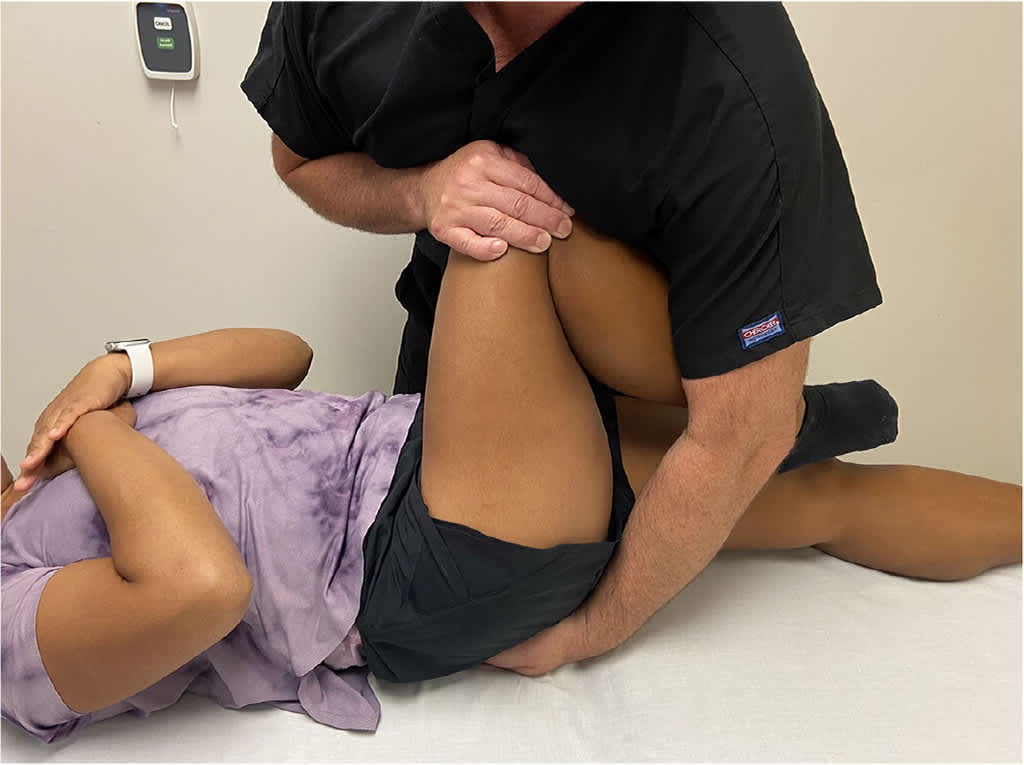
Thigh thrust test. The sacrum is fixated against the table with the caudal hand, and a force is applied through the axis of the femur with the cephalad hand, producing a shear force. The test is positive if pain is reproduced on the side being tested.
FIGURE 4.
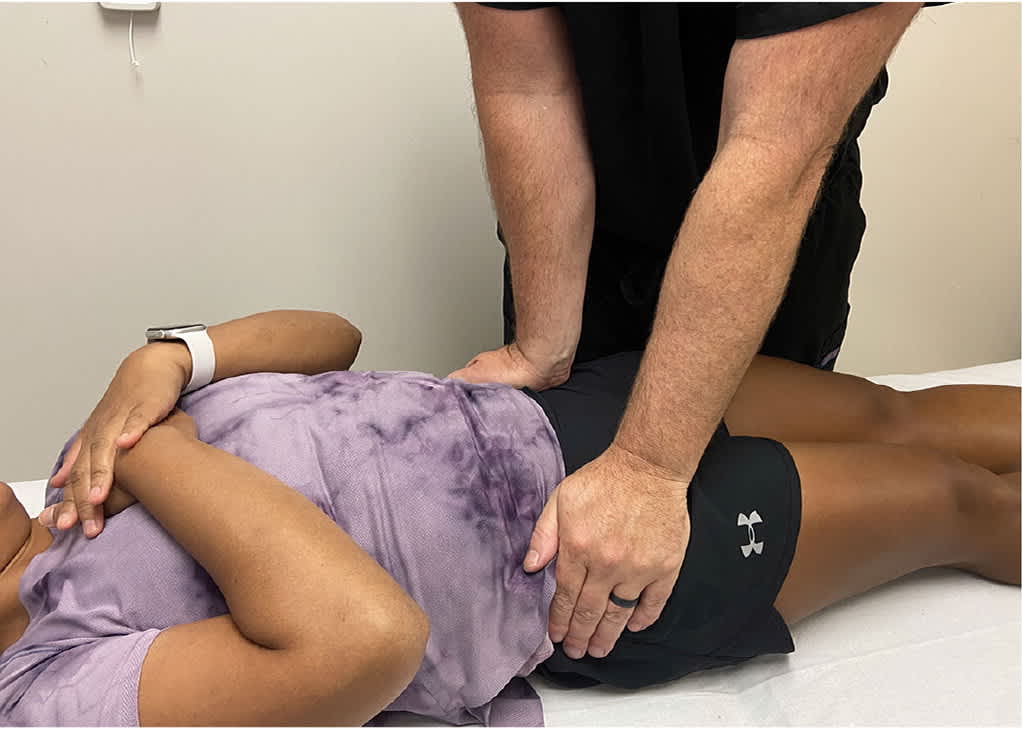
Distraction (gapping) test. A posteriorly directed force is applied to the anterior superior iliac spine thereby distracting the sacroiliac joints. The test is positive if pain is reproduced on the affected side.
FIGURE 5.
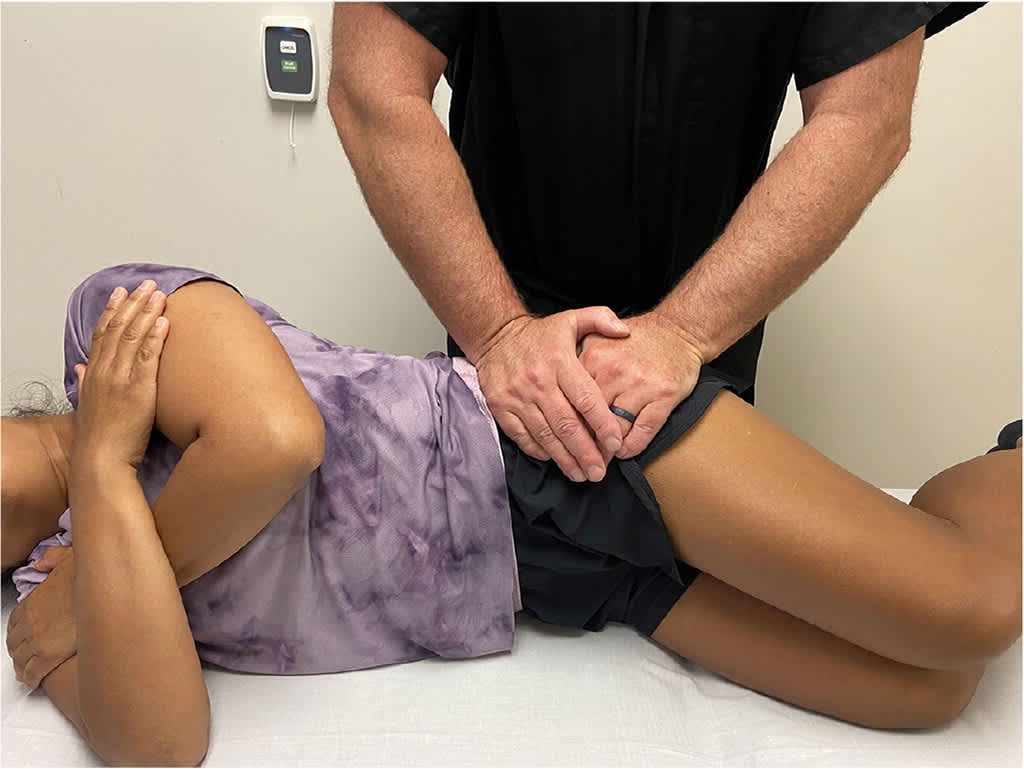
Compression test. A posteriorly directed force is applied to the iliac crest, thereby compressing the sacroiliac joint. The test is positive if pain is reproduced on the affected side.
FIGURE 6.
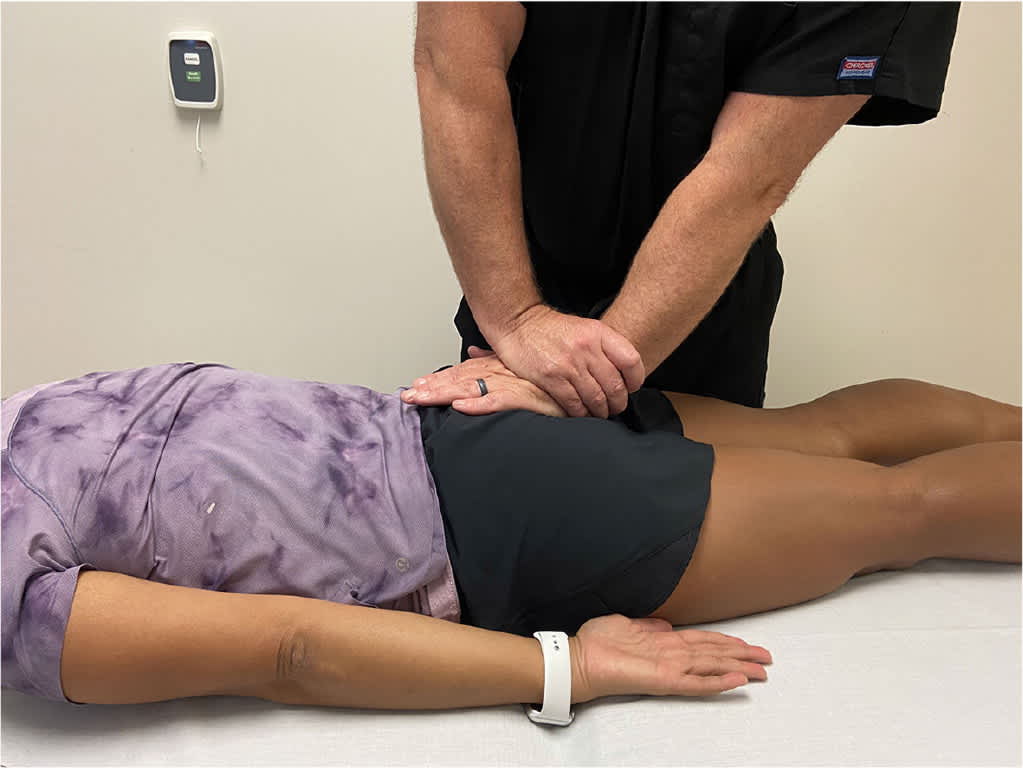
Sacral thrust test. Force is applied vertically and anteriorly to the apex of the curve of the sacrum, producing a shear force at the sacroiliac joints. The test is positive if pain is reproduced on the affected side.
When individual provocation tests for SI joint dysfunction are used in isolation, they have poor sensitivity and specificity.17 However, if three or more of the tests described in Figure 2, Figure 3, Figure 4, Figure 5, and Figure 6 reproduce pain, the clinician can reasonably conclude SI joint dysfunction is present (sensitivity = 94%; specificity = 78%; and positive likelihood ratio = 4.3 using three or more positive tests as the reference standard).17 Training and experience in provocation testing are critical for diagnosing SI joint dysfunction.
Magnetic resonance imaging, computed tomography, and bone scans do not reliably determine the source of pain with SI joint dysfunction,18 but they may be beneficial in ruling out other diagnoses with symptoms that mimic SI joint dysfunction.12,19,20 Laboratory tests to rule out other conditions include rheumatoid factor and human leukocyte antigen B27, which may be elevated or positive in inflammatory arthropathies.3 A contrast-enhanced intra-articular injection with local anesthetic can assist in confirming the SI joint as the source of pain for patients who have not benefited from conservative management or before considering interventional procedures.1,20
Treatment for SI Joint Dysfunction
If SI joint dysfunction is suspected or confirmed by the physical evaluation, initial treatment should consist of a nonsteroidal anti-inflammatory drug (NSAID) and referral to a physical therapist or a physician trained in osteopathic manipulative therapy.11,21–24 A multimodal rehabilitation program is recommended to correct the biomechanical faults with manipulative therapy combined with an exercise program to strengthen the pelvic girdle and lengthen tight muscles.12,14
If sacroiliitis or other spondyloarthropathies are suspected, referral to an orthopedist, interventional radiologist, or pain physician to provide an intra-articular corticosteroid injection may be appropriate.3 Physicians who specialize in the treatment of chronic pain can also provide other interventional treatments.
CONSERVATIVE TREATMENT
Medications. Although there are no studies comparing the use of NSAIDs to other treatments for SI joint dysfunction, NSAIDs are effective for acute and chronic low back pain. They may be especially effective in patients with sacroiliitis.25,26
Physical Therapy. Physical therapy exercise programs have demonstrated intermediate and long-term benefits.15,21 Family physicians can facilitate the use of these programs by providing education on iliopsoas and piriformis stretching.11 Additional muscles that should be addressed by a physical therapist and treated in the presence of muscle weakness include the abdominals, pelvic floor, ipsilateral gluteal muscles, and contralateral latissimus muscles.23,24
Thoracolumbar fascia tightness is often present in patients with SI joint dysfunction.8,24 Tightness of the thoracolumbar fascia can be assessed by having the patient forward flex the lumbar spine. If flexion is limited by the sensation of diffuse tightness along the lower back and sacrum, the patient can be taught self-mobilization techniques or referred to physical therapy or a massage therapist. Treatment options to address tight thoracolumbar fascia include foam rolling and deep tissue mobilization.
Manipulation Combined With Exercise Programs. SI joint manipulation provides short-term benefits,14,21,27 whereas the combination of manipulation with exercise programs achieves longer-term results compared with exercise programs alone.28 Two sessions of manipulative therapy to the SI joint over a two-week period resulted in more patients achieving improved pain and health status outcomes (i.e., physical functioning, social functioning, role limitations, and mental, emotional, and general health) compared with a six-week stretching and lumbar and pelvic floor strengthening program in patients with SI joint–related leg pain.27 SI joint manipulation and pelvic girdle stretching and strengthening exercises were more effective in reducing pain and improving function compared with SI joint manipulation and lumbar-focused exercises at three months.28 SI joint manipulation is also effective in treating generalized low back pain, suggesting that the SI joint influences loading of the lumbar spine.29 Exercise programs play an important role in long-term benefits; therefore, combining both treatment modalities should be considered.26
Pelvic Belt. Pelvic belts may assist in stabilizing SI joint motion and reducing ligament strain for peripartum patients with SI joint dysfunction.30
INTERVENTIONAL AND SURGICAL TREATMENT
Image-Guided Interventions. Intra-articular and periarticular corticosteroid injections or radiofrequency ablation may provide short- and long-term relief in refractory SI joint dysfunction.31,32 Corticosteroid injections are beneficial in treating sacroiliitis or other inflammatory conditions.33,34 Radiofrequency ablation involves the application of radiofrequency energy to cause a thermal lesion to the nerve that interrupts the pain signal. Cooled radiofrequency ablation of the L4 and L5 medial branch and lateral sacral branches is beneficial in patients with a positive response to a diagnostic SI joint block.31,32,35 Referral to a pain physician for consideration for these procedures should be made when other conservative or less invasive measures are not successful.
SI Joint Fusion. Patients who do not report improvement in pain symptoms after conservative and less invasive interventions (i.e., intra-articular corticosteroid injections and radiofrequency ablation) may benefit from surgical fusion of the SI joint.36
Data Sources: A PubMed search was completed in Clinical Queries using the following key search terms paired with sacroiliac joint dysfunction, including: medications, nonsteroidals, injection, radiofrequency neurotomy, fusion, physical therapy, rehabilitation, belts, and manipulation. The search was filtered first with a narrow scope and then a broad scope. The search included meta-analyses, randomized controlled trials, clinical trials, reviews, and case series. Also searched were the Cochrane Database of Systematic Reviews, CINHAL Database, Essential Evidence Plus, POEMS, and Ovid Database. Search dates: May 2021 and June 2021.
The views expressed in this article are those of the authors and do not reflect the official policy or position of the Department of the Army, Department of Defense, or the U.S. government.


