Case Scenario
A 14-year-old patient with a history of obesity presents to his primary care physician for a preparticipation physical evaluation for basketball. The patient is excited for the season to start, and his mother attributes his lower body mass index and improved grades to his growing motivation to play basketball.
The patient has no family history of premature death or congenital cardiac disease and does not have chest pain, syncope, or dyspnea. The patient’s heart rate and blood pressure are normal. The examination reveals normal femoral pulses, normal heart sounds without a murmur, and no stigmata of Marfan syndrome or other disease. The physician orders an electrocardiogram (ECG). The automated interpretation suggests first-degree atrioventricular block and left ventricular hypertrophy. Initially, the patient is counseled to avoid strenuous exercise and referred to a pediatric cardiologist. During the cardiology appointment several weeks later, results of a repeat ECG and echocardiography are normal, and the patient is diagnosed with “athlete’s heart.” He is cleared for strenuous activity and joins the basketball team after missing two weeks of practice, feeling out of shape and out of sync with his teammates.
Clinical Commentary
Children and adolescents who regularly participate in sports have a lower risk of obesity, chronic disease, alcohol and drug use, and criminal activity, and have higher self-esteem compared with nonparticipants.1–3 However, only 24% of youth engage in the 60 minutes of physical activity per day recommended by national guidelines.4 Participation in structured sports has decreased from 45% to 38% in the past 10 years, and children in low-income households are one-half as likely to participate regularly in sports compared with children from higher-income households.4 The Aspen Institute found growing disparities in physical activity by income; the percentage of inactive children in households with annual incomes less than $25,000 increased from 24% in 2012 to 33% in 2018, whereas the percentage of inactive children in households earning more than $100,000 decreased from 14% to 9.9% during the same time frame.4
In the United States, 49 states and the District of Columbia require a preparticipation physical evaluation before participation in school sports (Vermont leaves the decision to screen to individual school districts).5 The major components of the preparticipation physical evaluation are a detailed family history, medical history, symptom history, and physical examination.6,7
Concern about undiagnosed cardiac disease in athletes has grown over the past several decades following high-profile cases of sudden cardiac death.8 Rates of sudden cardiac death in young athletes range from 0.4 to 4 per 100,000 athlete-years.8,9 One suggested role of the preparticipation physical evaluation is preventing these deaths through early identification of children at high risk. Recognizing that the incidence of sudden cardiac death and cardiac disease is generally highest in first-degree relatives of individuals with related cardiac disease,10 the American Heart Association (AHA), American Academy of Family Physicians, and American Academy of Pediatrics (AAP) have focused efforts on increasing the sensitivity of screening tools for affected relatives. The AHA 14-element screening tool (https://www.acc.org/latest-in-cardiology/articles/2014/09/15/14/24/acc-aha-release-recommendations-for-congenital-and-genetic-heart-disease-screenings-in-youth), which includes cardiovascular history and physical examination, is recommended.
RATIONALE FOR INCLUDING ECGS IN PREPARTICIPATION PHYSICAL EVALUATIONS
The sensitivity of preparticipation physical evaluations for significant cardiac disease, even when they include the AHA 14-element screening tool, is low (2% to 6%), and the false-positive rate is high (31%).11,12 The most common causes of sudden cardiac death are hypertrophic cardiomyopathy, arrhythmias (e.g., long QT syndrome, Wolff-Parkinson-White syndrome), and coronary artery anomalies. Some of these causes can be identified with a screening ECG.13,14 Other diagnoses do not cause ECG changes or cause transient changes that may not be evident during a screening ECG. Initial studies show that an ECG increases the sensitivity of the preparticipation physical evaluation for identifying significant cardiac disease to 50%.11,15
In one cohort study of 1,070 Swiss athletes 14 to 35 years of age, four of the 11 athletes with cardiac disease were identified by ECG alone.16 A larger study in the Veneto region of Italy found a steady decrease in sudden cardiac death over the two decades following a 1978 law mandating preparticipation physical evaluation with an ECG, and a 79% relative reduction in sudden cardiac death after the law was implemented.17 The results of this study led the European Society of Cardiology to recommend an ECG as a standard part of the preparticipation physical evaluation and widespread adoption of this practice across Europe. Another Italian study suggested that ECGs may be more cost-effective for identifying cardiac disease than a patient history and physical examination or an echocardiogram.18
WHY ECGS SHOULD NOT BE ROUTINELY INCLUDED IN PREPARTICIPATION PHYSICAL EVALUATIONS
The results of the Veneto study have not been replicated. Israel implemented mandatory preparticipation physical evaluations with ECGs and exercise stress testing in 1997, but sudden cardiac death rates have not changed.19 When studied in the United States, preparticipation physical evaluation with or without an ECG did not significantly predict or reduce sudden cardiac death.9 Most athletes in the Football Association (England, soccer) with cardiac death had normal screening results despite mandatory preparticipation physical evaluations, ECGs, and echocardiography.20 Preparticipation physical evaluation with an ECG has a high false-positive rate (40%) and false-negative rate overall (4% to 5%), with both preparticipation evaluations and ECGs having higher false-negative rates specifically for hypertrophic cardiomyopathy (10%).11,21,22 A cost analysis showed that implementing preparticipation physical evaluations with ECGs in the United States would cost $470 per athlete per year or $51 billion to $69 billion over 20 years.23
Sudden cardiac death in an athlete is rare, totaling fewer than 100 deaths per year in the United States, at a rate of 1 in 150,000 athletes per year.8,9 In Denmark, the rate of sudden cardiac death in the general population is more than 20 times greater than the rate in teenaged and young adult athletes (0.43 to 0.47 per 100,000 athlete person-years).24 The preintervention rate in the Veneto study (4 per 100,000 athlete-years) was much higher than that observed in more contemporary studies. Considering the lower rates of sudden cardiac death in the United States, even if the benefit in the Veneto study could be replicated, the number of ECGs needed to prevent one sudden cardiac death would be 33,000 to 192,000.23
An estimated 2% of children are disqualified from sports participation through the screening process when it includes an ECG.22 Approximately 45 million children and adolescents participate in sports in the United States; therefore, 900,000 children and adolescents would be unable to participate in organized physical activity without clear evidence of benefit if universal ECG screening were recommended.25 Intensive exercise commonly causes cardiac remodeling, termed athlete’s heart, that can lead to asymptomatic bradyarrhythmia, first-degree heart block, and ventricular hypertrophy.25 ECG and echocardiogram changes can be mistaken for concerning pathology, prompting unnecessary testing. Athletes are often not aware that consenting to a preparticipation physical evaluation could disqualify them from sports participation.26 A time-intensive screening process to identify a rare diagnosis may exacerbate social and financial barriers to sports participation.
The recommendation to obtain an ECG only in patients who have a positive result using the AHA 14-element screening tool was affirmed by the 2020 AAP Choosing Wisely recommendations.27 The AAP cited the high false-positive rate, unnecessary evaluation associated with the false-positives, and a lack of evidence that screening with an ECG reduces mortality.
WHAT SHOULD CLINICIANS DO?
Although an ECG is not routinely recommended as part of the preparticipation physical evaluation, it has a role for children who are identified as having a higher-than-normal risk of cardiac disease on initial screening. Screening patients at high risk during well-child examinations may be underused, regardless of sports participation; one survey of pediatricians found that 24% had never ordered an ECG.28 Notably, rates of sudden cardiac death are equivalent or lower in athletes compared with nonathletes.12,13,23
Emergency response plans that include training staff in resuscitation and use of an automated external defibrillator are recommended and have been shown to save lives.29–31 In an eight-year follow-up study of professional soccer players who screened negative for cardiac risk, three athletes experienced cardiac arrest during competition or training, and all of them were successfully resuscitated.32
TAKE-HOME MESSAGES FOR RIGHT CARE
Screening for undiagnosed cardiac disease during well-child examinations using a validated tool such as the American Heart Association 14-element evaluation is a high-value, low-cost intervention for children and adolescents regardless of sports participation.
Sudden cardiac death is rare, and the unintended consequences of ordering nonindicated electrocardiograms include additional testing and cost, and unnecessary barriers to sports participation.
Children and adolescents who screen positive on the American Heart Association 14-element tool should be evaluated with an electrocardiogram
COVID-19
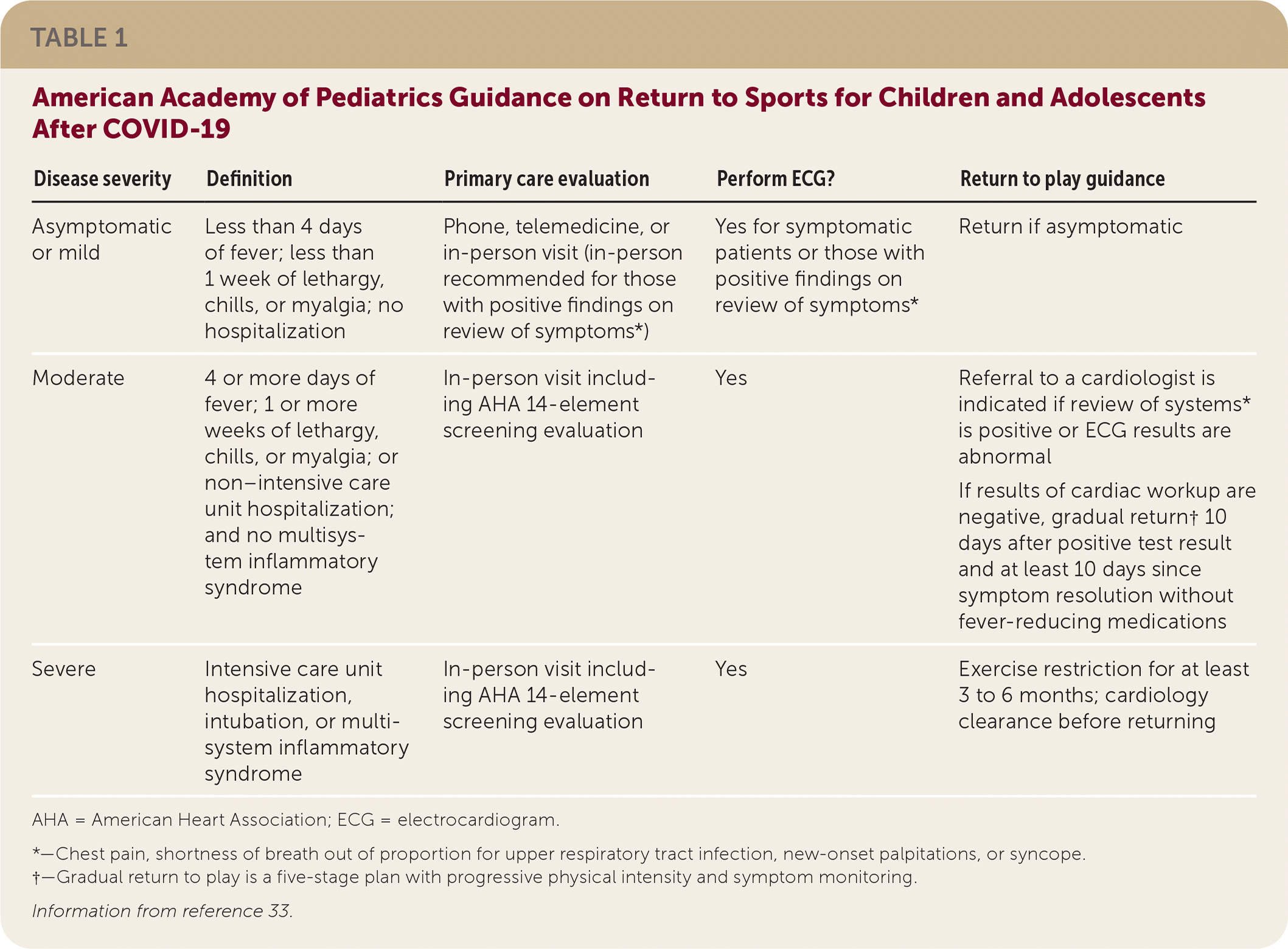
The COVID-19 pandemic has raised concerns about the additional risk of cardiac disease in children and adolescents.33,34 The AAP recommends that all children who test positive for COVID-19 rest and avoid exercise for a minimum of 14 days from diagnosis or becoming asymptomatic and seek clearance from their primary care physician before returning to sports33,34 (Table 133 ). Children who are asymptomatic or have mild symptoms can return to play once a review of symptoms is negative. In children with moderate symptoms, an ECG is recommended before a gradual return to play. Children with severe COVID-19 requiring intensive care or intubation and children diagnosed with multisystem inflammatory syndrome should avoid physical activity for at least three to six months and obtain clearance from a cardiologist before returning to play.33,34 These recommendations are mainly based on expert opinion and are likely to evolve as new data emerge.
TABLE 1. American Academy of Pediatrics Guidance on Return to Sports for Children and Adolescents After COVID-19
| Disease severity | Definition | Primary care evaluation | Perform ECG? | Return to play guidance |
|---|---|---|---|---|
| Asymptomatic or mild | Less than 4 days of fever; less than 1 week of lethargy, chills, or myalgia; no hospitalization | Phone, telemedicine, or in-person visit (in-person recommended for those with positive findings on review of symptoms*) | Yes for symptomatic patients or those with positive findings on review of symptoms* | Return if asymptomatic |
| Moderate | 4 or more days of fever; 1 or more weeks of lethargy, chills, or myalgia; or non–intensive care unit hospitalization; and no multisystem inflammatory syndrome | In-person visit including AHA 14-element screening evaluation | Yes | Referral to a cardiologist is indicated if review of systems* is positive or ECG results are abnormal If results of cardiac workup are negative, gradual return† 10 days after positive test result and at least 10 days since symptom resolution without fever-reducing medications |
| Severe | Intensive care unit hospitalization, intubation, or multi-system inflammatory syndrome | In-person visit including AHA 14-element screening evaluation | Yes | Exercise restriction for at least 3 to 6 months; cardiology clearance before returning |
AHA = American Heart Association; ECG = electrocardiogram.
*—Chest pain, shortness of breath out of proportion for upper respiratory tract infection, new-onset palpitations, or syncope.
†—Gradual return to play is a five-stage plan with progressive physical intensity and symptom monitoring.
Information from reference 33.
Patient Perspective
The sports preparticipation physical evaluation can be a double-edged sword for parents and children. Although most parents would surely want to know if their child has a concerning cardiovascular condition, these conditions are rare, and an abnormality on an ECG can delay or restrict a child’s participation in sports even if it is later deemed insignificant. The problem with any screening test is that it assesses health at a point in time that may shift with circumstances. For example, intense, ongoing exercise in a hot climate may induce electrolyte disturbances. This, coupled with a low-potassium diet, may cause hypokalemia and prolonged QT interval.35 This risk is increased in the 15% of people of African descent who carry the SCN5A 1103Y missense variant.36
As parents, we have been concerned that the tendency to demand more of young competitive athletes may lead to an increased risk of cardiac events, especially in the context of rising global temperatures. The widely publicized association of COVID-19 with myocarditis has also raised the overall level of anxiety around young people’s heart health. The complexity of screening criteria, especially concerning COVID-19, may confuse some parents. Because of the conflicting evidence on the usefulness of ECGs, there is room for shared decision-making. The added expense of an ECG is likely to be a concern for families who may already be struggling with the expense of competitive sports. Parents can look to their child’s primary care physician to explain the potential benefits and harms, including the impact of false-positives, with a jargon-free description of recommendations from expert groups. However, it may be that accessible automated external defibrillators backed up by a good emergency plan are the wisest allocation of resources to prevent sudden cardiac death in young athletes.
Resolution of Case
The patient, now age 15, returns to his primary care physician for a preparticipation physical evaluation before his next basketball season. He completes the AHA 14-element screening tool. His screening result is negative, and he has no concerning findings on his physical examination. As a result, he does not undergo an ECG and can participate on the first day of practice.

