A 32-year-old woman presented with a one-month history of pain in her right foot, under the fourth toe at the base of the proximal phalanx. About one month before presentation, she stepped on broken glass. She thought she removed all glass fragments at the time but noticed worsening pain since then. Walking intermittently caused sharp, localized pain. She had no additional symptoms, including fever, chills, or rash. She did not have skin changes, lumps, or discoloration in the painful area. She had no relevant family, medical, or social history.
Physical examination revealed a faint, circular, sharply demarcated nodule approximately 6 mm to 7 mm in diameter. It was light gray with no surrounding erythema, firm, and moderately tender on palpation. Radiography was performed (Figure 1).
FIGURE 1
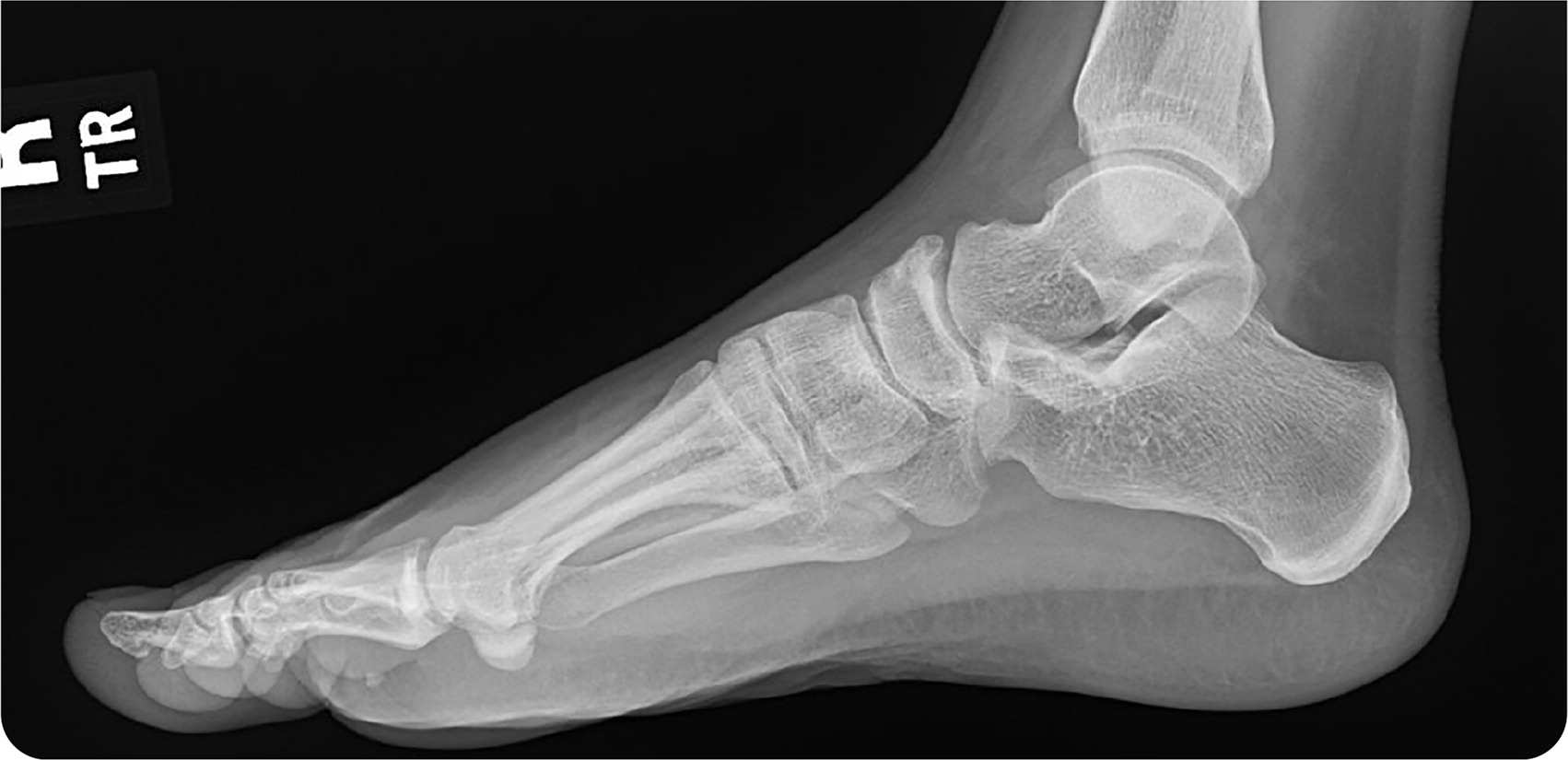
Question
Based on the patient's history, physical examination, and radiography findings, which one of the following is the most likely diagnosis?
- A. Foreign body.
- B. Morton neuroma.
- C. Osteomyelitis.
- D. Osteophyte.
Discussion
The answer is A: foreign body. Most foreign bodies are introduced into the skin through lacerations and soft tissue wounds. Complications include chronic pain and neurovascular impairment. Assessment should include radiography or ultrasonography before removal.1 Contraindications for removal include the foreign body is close to a vital structure or cannot be located, or the patient is unable to tolerate removal.1
In this patient, plain radiography showed a foreign body present under the fourth phalanx (Figure 2A). A glass fragment was extracted through a linear incision at the base of the right foot under the phalanx after adequate anesthetic use (Figure 2B).
FIGURE 2.
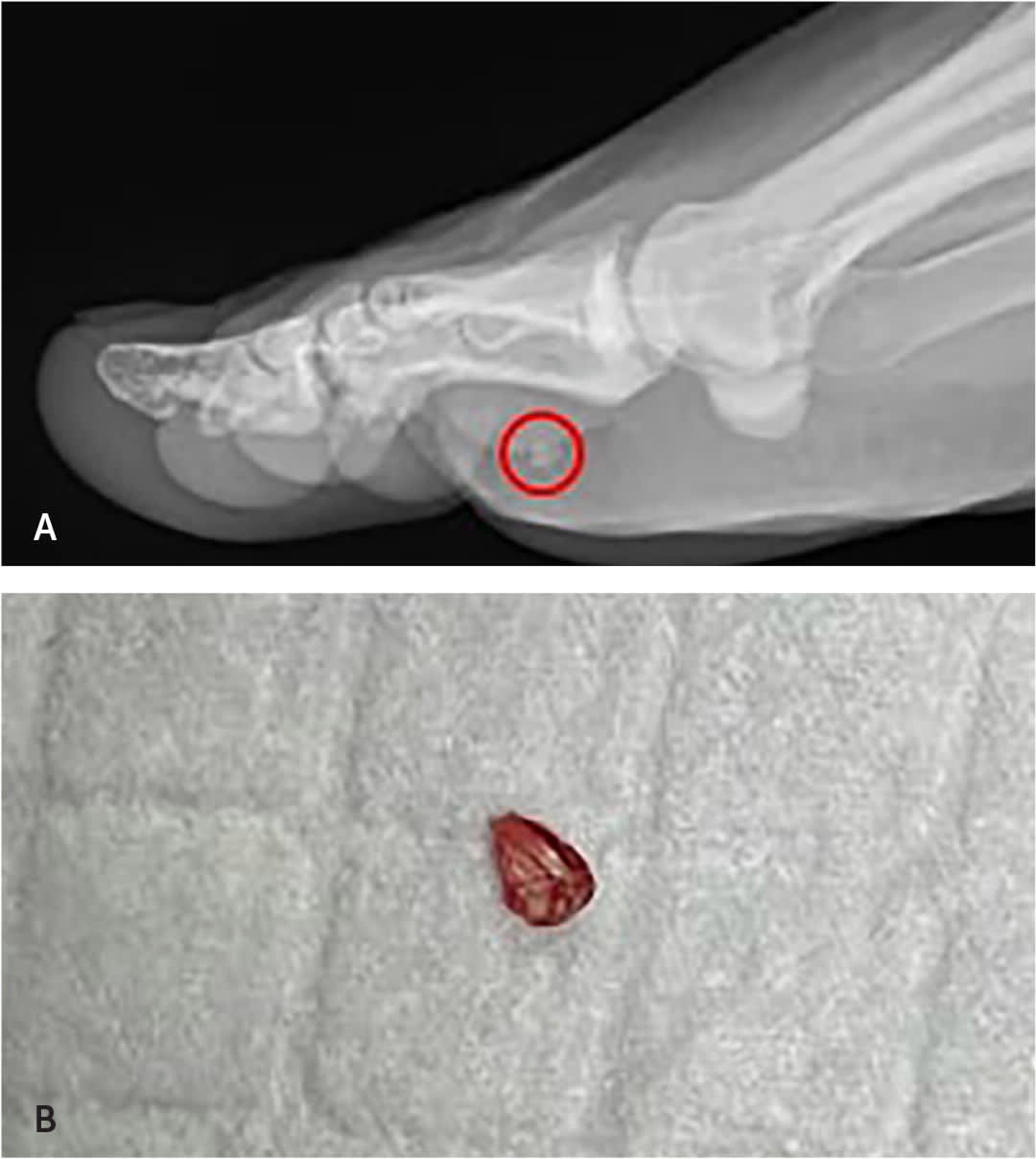
(A) Foreign body shown on plain radiography. (B) The glass fragment was extracted through a linear incision at the base of the right foot under the phalanx after adequate anesthetic use.
Morton neuroma is a nonneoplastic, perineural, fibrous proliferation involving a plantar digital nerve in the second or third intermetatarsal space. It is caused by pressure or repetitive irritation. The most common clinical signs are burning-like pain, altered sensation, and the feeling of a pebble in the shoe. Treatment options include orthotics, steroid injections, and surgical excision.2
Osteomyelitis is associated with inflammatory bone changes caused by pathogenic bacteria. Clinical features include fever, chills, and malaise. The most common symptom is pain at the site of infection.3 The condition is diagnosed using radiography or magnetic resonance imaging.
Osteophytes are bony outgrowths, which are radiologic signs of osteoarthritis. Osteoarthritis has varying presentations and is more common in patients older than 50 years. Risk factors include obesity, excessive joint loading, history of injury or trauma, and family history. Most cases have an insidious onset, and they are rarely acute.4
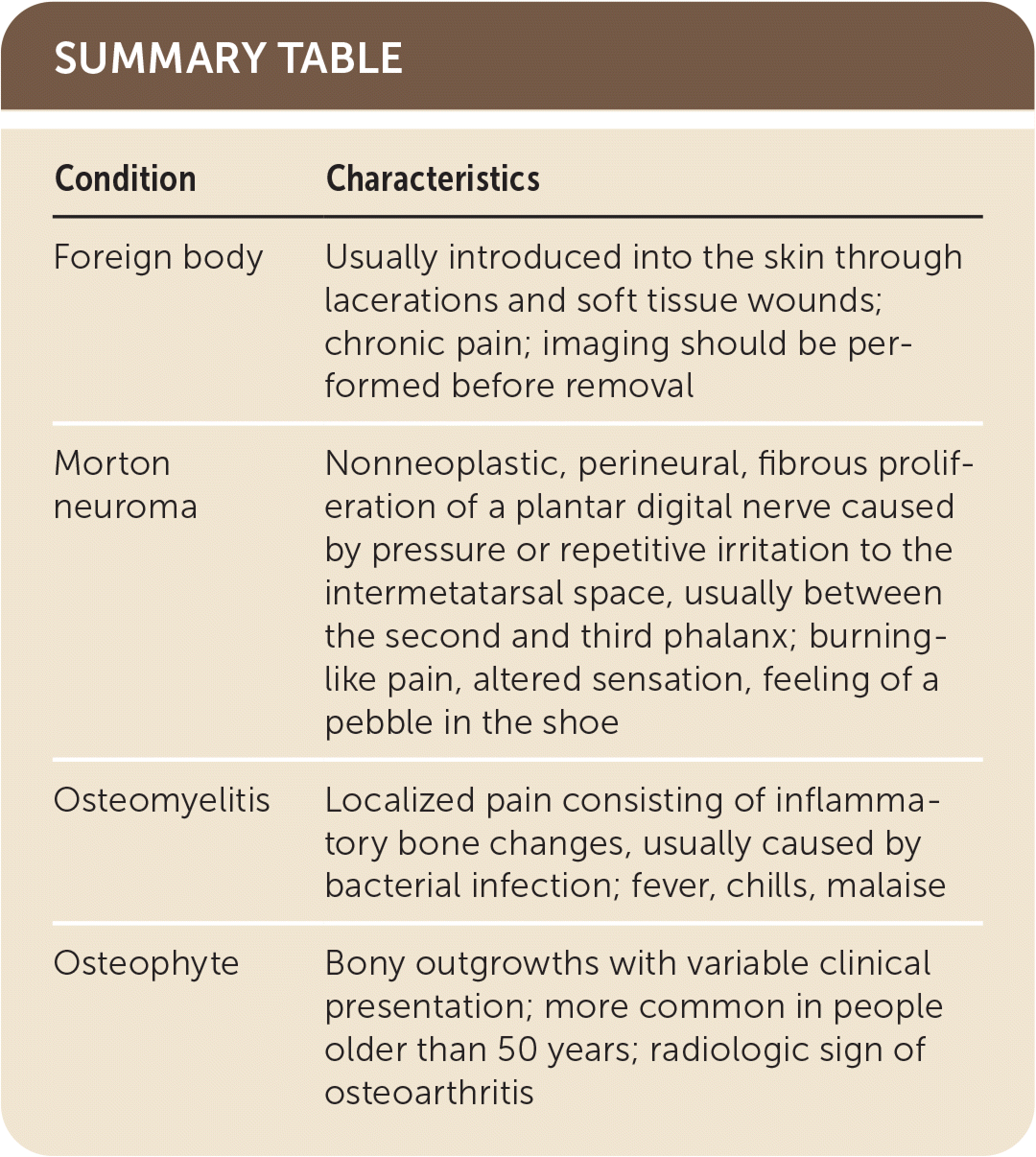
SUMMARY TABLE
| Condition | Characteristics |
|---|---|
| Foreign body | Usually introduced into the skin through lacerations and soft tissue wounds; chronic pain; imaging should be performed before removal |
| Morton neuroma | Nonneoplastic, perineural, fibrous proliferation of a plantar digital nerve caused by pressure or repetitive irritation to the intermetatarsal space, usually between the second and third phalanx; burning-like pain, altered sensation, feeling of a pebble in the shoe |
| Osteomyelitis | Localized pain consisting of inflammatory bone changes, usually caused by bacterial infection; fever, chills, malaise |
| Osteophyte | Bony outgrowths with variable clinical presentation; more common in people older than 50 years; radiologic sign of osteoarthritis |

