Case Scenario
My 81-year-old patient, E.P., has a history of hypertension, hypothyroidism, and mild chronic obstructive pulmonary disease, but I have not seen them since the initial COVID-19 shutdown. The county Adult Protective Services agency has requested a medical assessment because of concerns for E.P.’s safety and possible self-neglect following reports of E.P. appearing confused and wandering in the neighborhood. As a family physician, what are my responsibilities to the patient and to Adult Protective Services in this situation? What is the best clinical approach to addressing the concerns for E.P.’s welfare?
Commentary
Elder abuse (in this Curbside Consultation, “elder” refers to a person 60 years or older) affects at least one in 10 older adults but is often undetected and underreported, even compared with any other form of abuse.1 Elder abuse can take several forms, including neglect and physical, emotional, financial, or sexual maltreatment. Adult self-neglect is the most common form of elder abuse2 (Table 12–4 ). Most of these adults live in private residences; approximately 10% of reports to Adult Protective Services involve older adults who are living in residential care facilities.2 Many states use a centralized or combined local and state hotline model to report allegations of maltreatment. Nationally, the Eldercare Locator (1-800-677-1116) can direct people to individual state resources. Approximately 60% of reports come from professionals such as police, social services, or visiting nurses or aides; other reporters include relatives, nonprofessionals (e.g., neighbors), caregivers, and the individual involved (self-report).2 Physicians and medical personnel are mandated reporters.2
TABLE 1. Types and Prevalence of Elder Abuse

| Abuse Emotional (10%): inflicting mental pain, anguish, or distress through verbal or nonverbal acts (e.g., humiliating, intimidating, threatening) Physical (8%): inflicting physical pain or injury (e.g., slapping, bruising, restraining by physical or chemical means) Sexual (0.7%): nonconsensual sexual contact of any kind |
| Exploitation Financial or material exploitation (16.5%): illegal taking, misuse, or concealment of funds, property, or assets of an older adult for someone else’s benefit |
| Neglect Neglect (14%) and abandonment (0.3%): failure by those responsible to provide food, shelter, health care, or protection for a vulnerable elder adult; desertion of a vulnerable elder adult by anyone who has assumed the responsibility for care or custody of that person Self-neglect (65%): a form of maltreatment resulting from an individual’s inability (mental or physical) to perform essential self-care tasks. These include obtaining essential food, clothing, shelter, and medical care; obtaining goods or services necessary to maintain health and general safety; managing financial affairs; paying attention to hygiene and environment; accepting services that reasonably improve quality of life; and avoiding self-endangerment through unsafe behaviors |
Adult Protective Services first screens any report of potential abuse for eligibility and authority to investigate based on state laws. Initial caseworker involvement includes prioritizing risk and contacting the client. The caseworker may assess emergency needs, general physical and mental health, medication adherence, nutritional status, financial affairs, cognitive abilities, substance and alcohol use, and overall environment and support systems. Emergency protective action is taken when urgent action is needed. Supervisors of the caseworker, other experts (law enforcement, legal services), and Adult Protective Services team members review the collected information and evidence (e.g., photos, financial records, interviews) to decide next steps, including health and service needs, safeguarding the patient’s rights and monitoring to ensure long-term safety and satisfactory fulfillment of care goals. If a perpetrator is involved, associated risks will be addressed by making the appropriate referrals to regulatory agencies, law enforcement, or perpetrator registries.
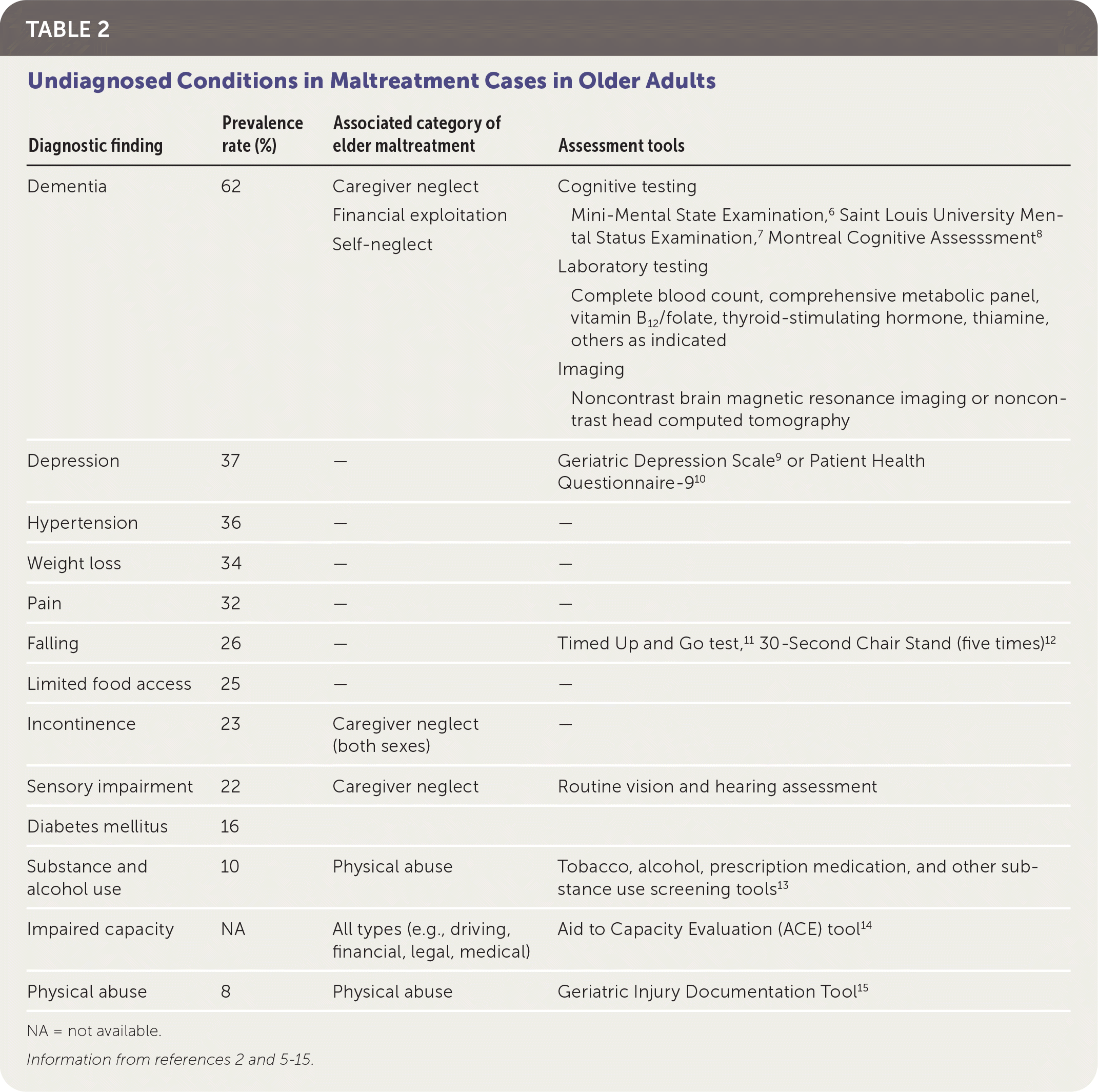
As part of the investigation, Adult Protective Services may request information from the patient’s physician, including medication review, physical and cognitive function assessment, anticipated prognosis, and recommendations for health care. Because patients experiencing mal-treatment commonly have undiagnosed medical conditions,5 physicians should be alert for and address the conditions listed in Table 2.2,5–15 Family physicians should also consider the possibility of patient maltreatment when an older patient presents with any of the conditions identified in Table 2.2,5–15
TABLE 2. Undiagnosed Conditions in Maltreatment Cases in Older Adults
| Diagnostic finding | Prevalence rate (%) | Associated category of elder maltreatment | Assessment tools |
|---|---|---|---|
| Dementia | 62 | Caregiver neglect Financial exploitation Self-neglect | Cognitive testing Mini-Mental State Examination,6 Saint Louis University Mental Status Examination,7 Montreal Cognitive Assesssment8 Laboratory testing Complete blood count, comprehensive metabolic panel, vitamin B12/folate, thyroid-stimulating hormone, thiamine, others as indicated Imaging Noncontrast brain magnetic resonance imaging or noncontrast head computed tomography |
| Depression | 37 | — | Geriatric Depression Scale9 or Patient Health Questionnaire-910 |
| Hypertension | 36 | — | — |
| Weight loss | 34 | — | — |
| Pain | 32 | — | — |
| Falling | 26 | — | Timed Up and Go test,11 30-Second Chair Stand (five times)12 |
| Limited food access | 25 | — | — |
| Incontinence | 23 | Caregiver neglect (both sexes) | — |
| Sensory impairment | 22 | Caregiver neglect | Routine vision and hearing assessment |
| Diabetes mellitus | 16 | ||
| Substance and alcohol use | 10 | Physical abuse | Tobacco, alcohol, prescription medication, and other substance use screening tools13 |
| Impaired capacity | NA | All types (e.g., driving, financial, legal, medical) | Aid to Capacity Evaluation (ACE) tool14 |
| Physical abuse | 8 | Physical abuse | Geriatric Injury Documentation Tool15 |
NA = not available.
Gathering further information to evaluate the presence and severity of maltreatment can present multiple challenges, even in the setting of a referral from Adult Protective Services. When a patient is reluctant to provide information or appears to downplay disabilities or injuries, self-neglect or abuse should be suspected. Undiagnosed cognitive impairment may present as a lack of concern for personal hygiene or adequate nutrition; it may also manifest as unsafe driving or disregard for personal safety or social conventions. Observational information from a family member, neighbor, or close friend can clarify a patient’s ability to perform activities of daily living, such as dressing, toileting, feeding, and instrumental activities of daily living that include shopping, housekeeping, and food preparation. This information may also provide a timeline of the progression of any cognitive impairment or neglect. The IQCODE (Informant Questionnaire on Cognitive Decline in the Elderly) is a useful tool for gathering information about how well the patient is functioning at home.16 A physician house call or a home health referral can also provide a basic home-based evaluation of the patient to assess cognition, safety, and ability to perform activities of daily living and instrumental activities of daily living.
Once the historical information is collected, the physician should continue with a comprehensive geriatric assessment, focusing on medication review, mobility impairments, and any additional cognitive and mood disorders that may impair a patient’s function.17 With this information, the physician should be able to objectively document appropriate individualized diagnoses, treatment, and prognostic recommendations for care. Treatment recommendations could include a need for supervision or assistance in the home or recommendations for care transition, for example, to adult day care, assisted living facilities, Area Agencies on Aging, memory support units, or long-term care.
Adult Protective Services often requests that the physician address a patient’s capacity to make decisions and to manage their affairs. This could include maintaining control of medications and finances, living independently, making medical decisions, appointing a medical and financial power of attorney, and completing an advance directive. The capacity to make such decisions is defined as the ability to understand the risks and benefits of treatments/decisions and alternatives, to demonstrate appreciation of risks and benefits of proposed treatments vs. harms of declining treatments/options, to demonstrate logical reasoning for making choices, and to effectively communicate choices.18 Should the physician believe the patient is incapable of making safe and appropriate decisions about the independent management of health or finances, Adult Protective Services will ask the physician to provide a written statement documenting the domains of a patient’s incapacity. With this information, Adult Protective Services can help the patient and family obtain resources and appoint medical or financial powers of attorney or guardians to assume decision-making within the specified domain. Physicians tend to underdiagnose lack of capacity, possibly because of concerns about insufficient expertise or reluctance to restrict patient autonomy.18 Nevertheless, a physician who has a close and knowledgeable long-term relationship with a patient should be able to make these determinations and recommendations to promote the health and safety of the patient appropriately.
Case Resolution
Adult Protective Services should identify a family member, friend, or neighbor close to E.P. who has concerns about E.P.’s ability to care for themselves at home. If possible, that person may be encouraged to take E.P. to the physician’s office for assessment. An extensive evaluation of E.P.’s medical conditions and medications, including adverse effects and adherence, should be performed to determine the causes of cognitive decline. The physician could order (or independently perform) a home health assessment, which may demonstrate significant cognitive impairments resulting in the patient’s inability to remember to eat or take medications. Appropriate screening for dementia should be performed. E.P.’s adult children should be contacted to act as the medical and financial powers of attorney and find help at home for E.P. Ideally, they should accompany E.P. in person or virtually to all future doctors’ appointments.

