Diverticulitis should be suspected in patients with isolated left lower quadrant pain, abdominal distention or rigidity, fever, and leukocytosis. Initial laboratory workup includes a complete blood count, basic metabolic panel, urinalysis, and C-reactive protein measurement. Computed tomography with intravenous contrast is the preferred imaging modality, if needed to confirm diagnosis and assess for complications of diverticulitis. Treatment decisions are based on the categorization of disease as complicated vs. uncomplicated. Selected patients with uncomplicated diverticulitis may be treated without antibiotics. Complicated diverticulitis is treated in the hospital with modified diet or bowel rest, antibiotics, and pain control. Abscesses that are 3 cm or larger should be treated with percutaneous drainage. Emergent surgery is reserved for when percutaneous drainage fails or the patient's clinical condition worsens despite adequate therapy. Colonoscopy should not be performed during the flare-up, but should be considered six weeks after resolution of symptoms in patients with complicated diverticulitis who have not had a high-quality colonoscopy in the past year. Diverticulitis prevention measures include consuming a vegetarian diet or high-quality diet (high in fruits, vegetables, whole grains, and legumes), limiting red meat and sweets, achieving or maintaining a body mass index of 18 to 25 kg per m2, being physically active, and avoiding tobacco and long-term nonsteroidal anti-inflammatory drugs. Partial colectomy is not routinely recommended for diverticulitis prevention and should be reserved for patients with more than three recurrences or abscess formation requiring percutaneous drainage.
A diverticulum is a protrusion through the intestinal wall, and diverticulosis is the presence of multiple diverticula. Acute diverticulitis is inflammation of diverticula. Possible causes include abnormal colonic motility, colonic wall resistance, intraluminal pressures, and colonic wall defects.1,2 Diverticular bleeding, the most common cause of lower gastrointestinal tract bleeding in adults, was reviewed previously in American Family Physician (https://www.aafp.org/afp/2009/1101/p977.html). The current article provides a summary of the best evidence on diagnosis and management of diverticular disease.
WHAT'S NEW ON THIS TOPIC

SORT: KEY RECOMMENDATIONS FOR PRACTICE
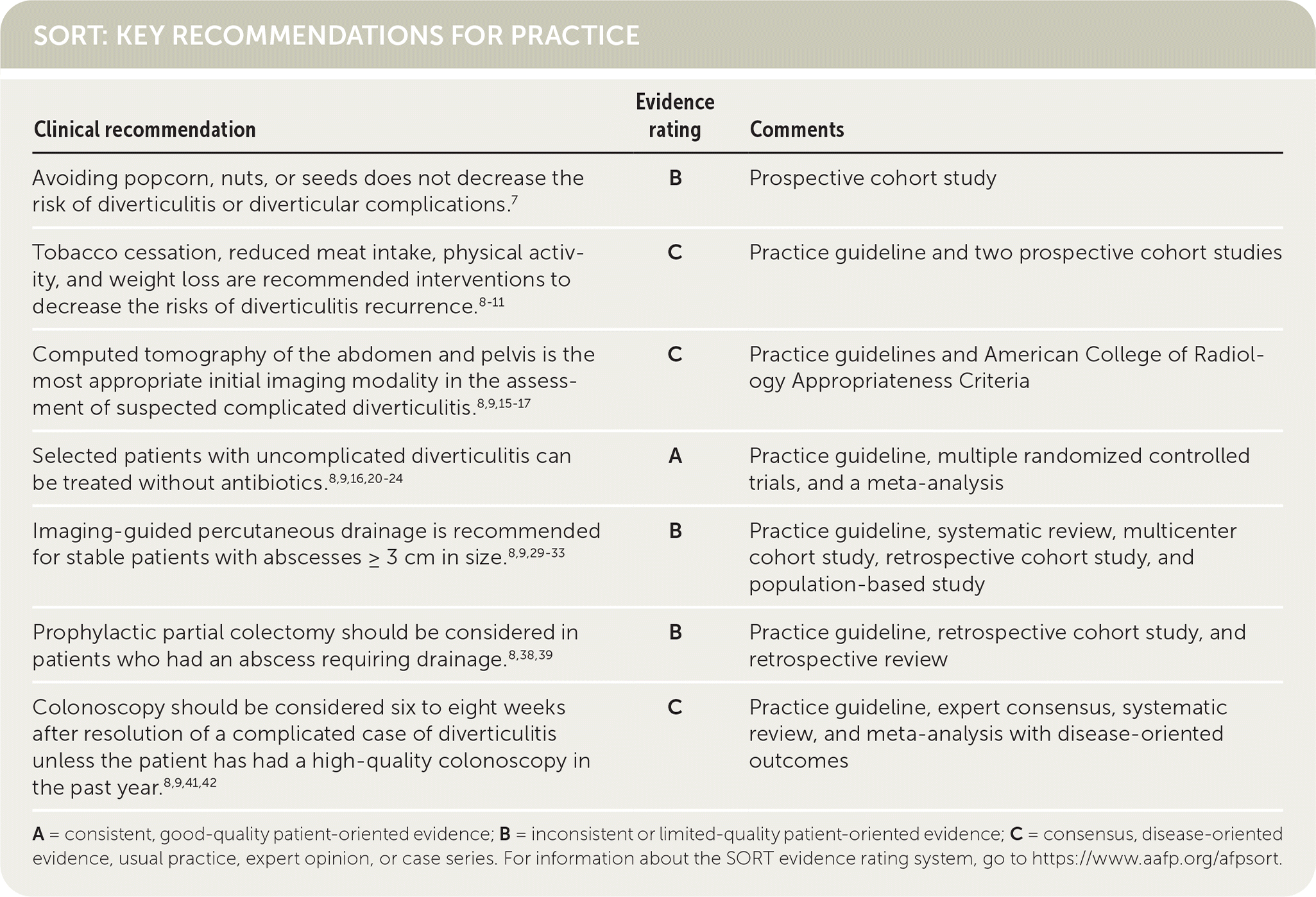
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Epidemiology
- Incidence of diverticulitis is increasing. From 1980 to 2007, the incidence increased from 115 per 100,000 person-years to 188 per 100,000 person-years.3
- Prevalence of diverticular disease is less than 10% in people 40 years vs. 80% in those older than 85 years.1,2 [corrected]
- Only 1% to 4% of patients with diverticular disease will develop diverticulitis in their lifetime.4
- Risk factors for diverticular disease include increasing age, constipation, low-fiber diet, smoking, red meat consumption, obesity, weight gain, lack of exercise, genetic susceptibility, and nonsteroidal anti-inflammatory drug and aspirin use.1,5,6
- Consumption of popcorn, nuts, and seeds is not a risk factor for developing diverticulitis.7
Screening and Prevention
- Screening for diverticular disease is not recommended. It is often found incidentally on screening colonoscopy or imaging studies performed for other reasons.
- Measures for preventing recurrence of diverticulitis include consuming a vegetarian diet or high-quality diet (high in fruits, vegetables, whole grains, and legumes), limiting red meats and sweets, achieving or maintaining a body mass index of 18 to 25 kg per m2, being physically active, and avoiding tobacco and long-term nonsteroidal anti-inflammatory drugs.8–11
- A high-fiber diet is associated with a lower incidence of diverticular disease, but evidence regarding whether it prevents the recurrence of diverticulitis is lacking.12
Diagnosis
SIGNS AND SYMPTOMS
- Tenderness to palpation located only in the left lower quadrant of the abdomen is the most specific finding for diverticulitis (likelihood ratio [LR] = 10.4). Tenderness in the left lower quadrant plus other locations is less useful (LR = 3.4).13
- History of left lower quadrant tenderness (LR = 3.3), fever (LR = 1.4), and absence of vomiting (LR = 1.4) also support the diagnosis13 (Table 11 ).
- Other nonspecific signs and symptoms may include abdominal rigidity, anorexia, dysuria, hypoactive bowel sounds, rectal bleeding, or tenderness on rectal examination.1,13
- Fecaluria, pneumaturia, pyuria, and stool per vagina should raise suspicion for fistula formation.8
- Studies have found that right-sided diverticulitis is more common in Asian countries.14
- The differential diagnosis of diverticulitis is shown in Table 2.1
TABLE 1. Accuracy of Signs and Symptoms for the Diagnosis of Acute Diverticulitis
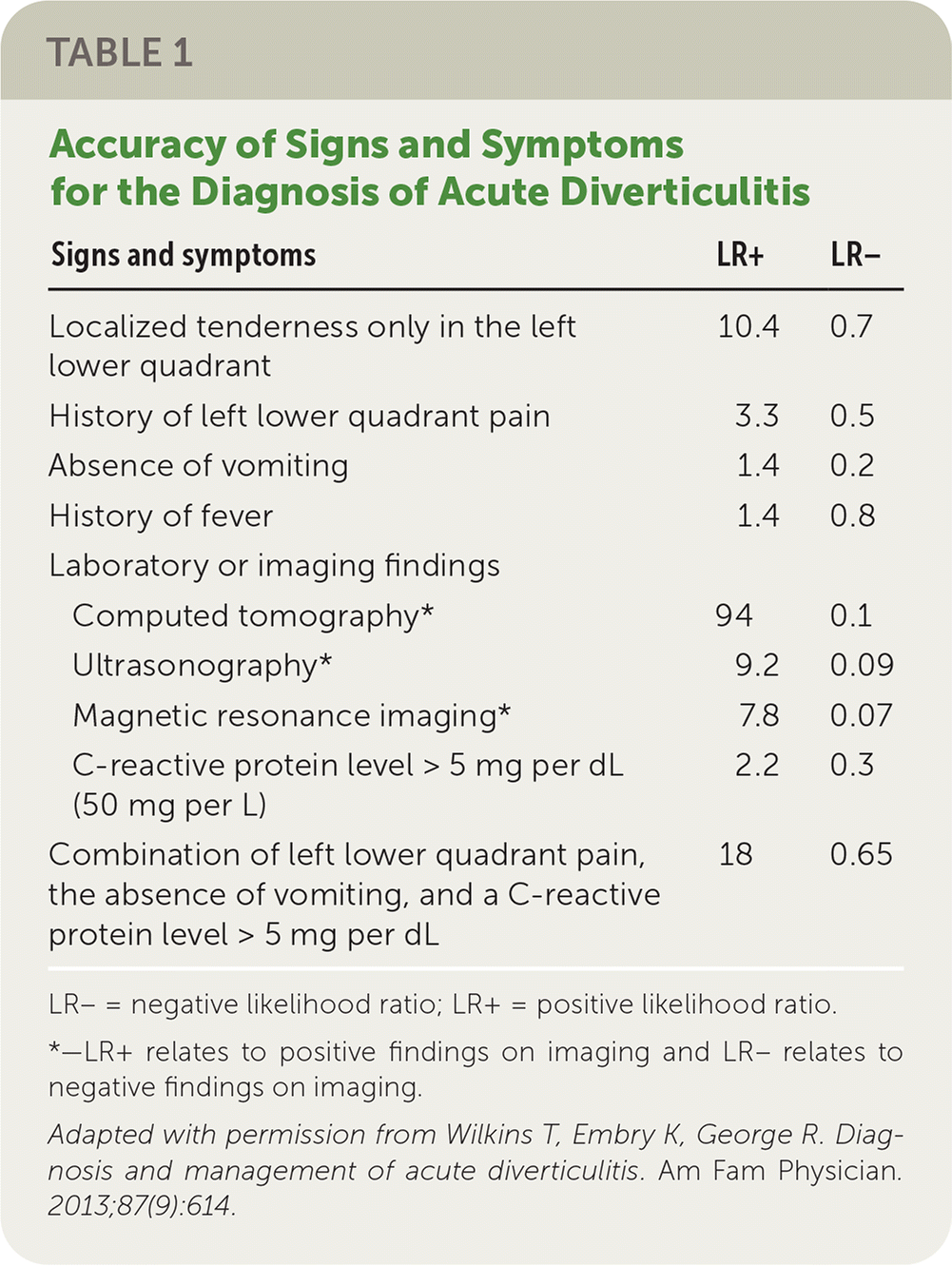
| Signs and symptoms | LR+ | LR− |
|---|---|---|
| Localized tenderness only in the left lower quadrant | 10.4 | 0.7 |
| History of left lower quadrant pain | 3.3 | 0.5 |
| Absence of vomiting | 1.4 | 0.2 |
| History of fever | 1.4 | 0.8 |
| Laboratory or imaging findings | ||
| Computed tomography* | 94 | 0.1 |
| Ultrasonography* | 9.2 | 0.09 |
| Magnetic resonance imaging* | 7.8 | 0.07 |
| C-reactive protein level > 5 mg per dL (50 mg per L) | 2.2 | 0.3 |
| Combination of left lower quadrant pain, the absence of vomiting, and a C-reactive protein level > 5 mg per dL | 18 | 0.65 |
LR− = negative likelihood ratio; LR+ = positive likelihood ratio.
*—LR+ relates to positive findings on imaging and LR− relates to negative findings on imaging.
Adapted with permission from Wilkins T, Embry K, George R. Diagnosis and management of acute diverticulitis. Am Fam Physician. 2013;87(9):614.
TABLE 2. Differential Diagnosis of Diverticulitis

| Gastrointestinal Bowel obstruction Colitis (infectious and ischemic) Colon cancer Inflammatory bowel disease Irritable bowel syndrome Perforation | Gynecologic Ectopic pregnancy Endometriosis Ovarian cyst Pelvic inflammatory disease Torsion Tubo-ovarian abscess | Urinary Nephrolithiasis Urinary tract infection |
Information from reference 1.
DIAGNOSTIC EVALUATION
- Initial tests include complete blood count (white blood cell count may be normal in 45% of patients), basic metabolic panel to evaluate electrolyte and renal status, urinalysis to rule out urinary tract infection, and C-reactive protein (level greater than 20 mg per dL [200 mg per L] is suggestive of perforation).13
- Other tests to consider in selected patients include a beta-human chorionic gonadotropin test to rule out ectopic pregnancy and if surgery is needed in a patient who could become pregnant, and a lipase test to rule out acute pancreatitis (mild elevation of lipase may occur with perforation).
- Imaging should be considered if the diagnosis is uncertain or there is concern for complicated diverticulitis.
- If imaging is performed, computed tomography with contrast is the diagnostic test of choice because of its availability and high sensitivity (94%) and specificity (99%).8,9,15,16
- Magnetic resonance imaging has good diagnostic accuracy and avoids radiation exposure but may not be as readily available as computed tomography.8,17
- Ultrasonography can be effective in the diagnosis of diverticulitis, but operator experience affects accuracy. Its ability to assess for free air or the extent of large abscesses is limited.8,17
CLINICAL PREDICTION RULES
- The combination of a C-reactive protein level greater than 5 mg per dL (50 mg per L), isolated left lower quadrant tenderness, and absence of vomiting has a positive LR of 5.3 to 18 for diverticulitis (sensitivity = 36% to 37%; specificity = 93% to 98%).13,18
- A clinical prediction rule that includes abdominal guarding, white blood cell count, and C-reactive protein level can be used to predict the likelihood of complicated diverticulitis.19
Treatment
UNCOMPLICATED ACUTE DIVERTICULITIS
- For patients who have normal vital signs, are able to maintain oral intake, and have no signs of complications (e.g., peritonitis, fever), outpatient management is appropriate.
- Antibiotics should not be used routinely in the treatment of uncomplicated diverticulitis.8,9,16,20–24 A meta-analysis of nine randomized controlled trials with 2,505 patients showed that those treated without antibiotics had shorter hospital stays than those treated with antibiotics, and there was no difference in complication or readmission rates.20
- If symptoms do not improve after 48 to 72 hours, a broad-spectrum antibiotic against anaerobic and gram-negative rods should be initiated and typically continued for seven to 10 days (Table 325,26 ).
- In one study, patients were given four days of ertapenem (Invanz) for uncomplicated acute diverticulitis. If symptoms improved, they were randomized to three additional days of treatment or no further antibiotics. The cure rate was 98% in both groups.27
- Although bowel rest is typically recommended, there is no evidence to support it over a modified diet (e.g., a clear liquid or soft mechanical diet as tolerated) for uncomplicated disease.28
- Follow-up is recommended two or three days after diagnosis to assess improvement.
TABLE 3. Antibiotic Treatment Guidelines for Diverticulitis
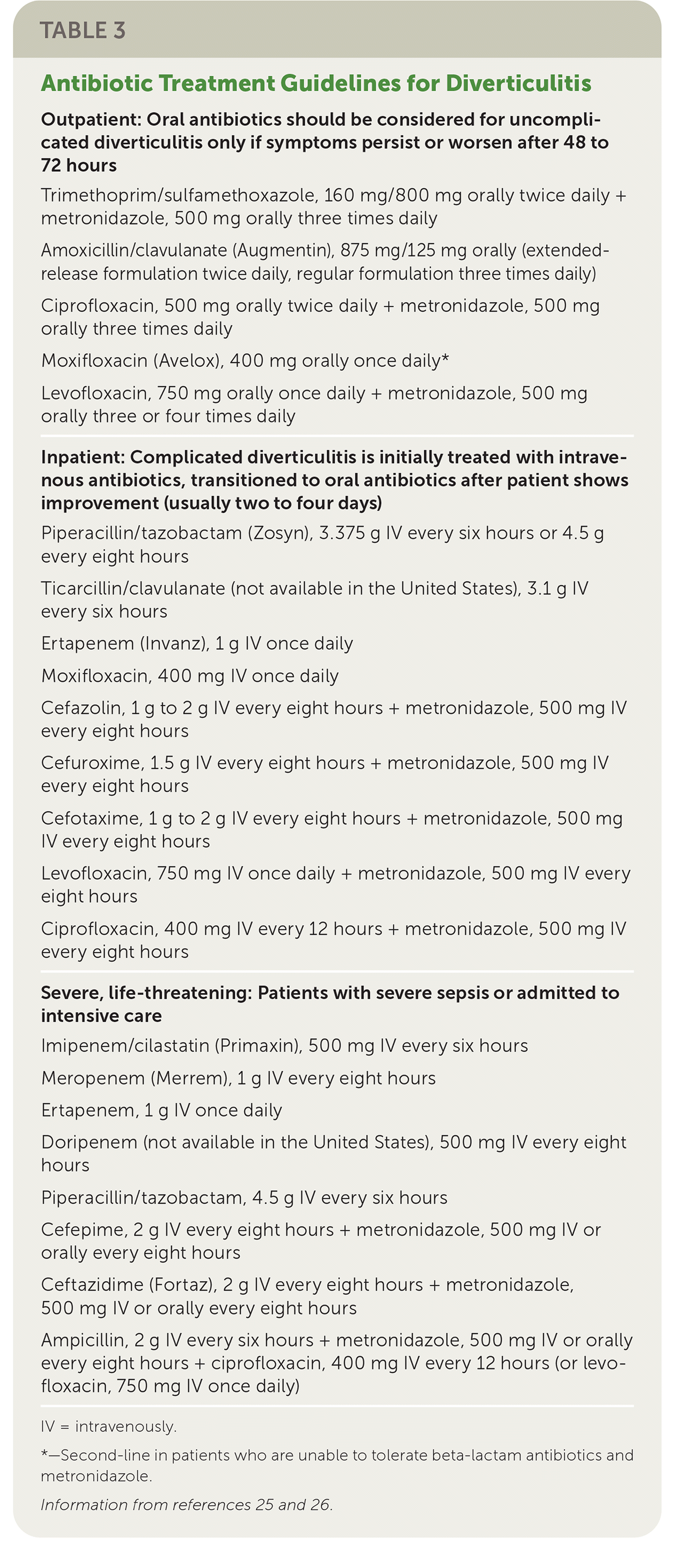
| Outpatient: Oral antibiotics should be considered for uncomplicated diverticulitis only if symptoms persist or worsen after 48 to 72 hours |
| Trimethoprim/sulfamethoxazole, 160 mg/800 mg orally twice daily + metronidazole, 500 mg orally three times daily |
| Amoxicillin/clavulanate (Augmentin), 875 mg/125 mg orally (extended-release formulation twice daily, regular formulation three times daily) |
| Ciprofloxacin, 500 mg orally twice daily + metronidazole, 500 mg orally three times daily |
| Moxifloxacin (Avelox), 400 mg orally once daily* |
| Levofloxacin, 750 mg orally once daily + metronidazole, 500 mg orally three or four times daily |
| Inpatient: Complicated diverticulitis is initially treated with intravenous antibiotics, transitioned to oral antibiotics after patient shows improvement (usually two to four days) |
| Piperacillin/tazobactam (Zosyn), 3.375 g IV every six hours or 4.5 g every eight hours |
| Ticarcillin/clavulanate (not available in the United States), 3.1 g IV every six hours |
| Ertapenem (Invanz), 1 g IV once daily |
| Moxifloxacin, 400 mg IV once daily |
| Cefazolin, 1 g to 2 g IV every eight hours + metronidazole, 500 mg IV every eight hours |
| Cefuroxime, 1.5 g IV every eight hours + metronidazole, 500 mg IV every eight hours |
| Cefotaxime, 1 g to 2 g IV every eight hours + metronidazole, 500 mg IV every eight hours |
| Levofloxacin, 750 mg IV once daily + metronidazole, 500 mg IV every eight hours |
| Ciprofloxacin, 400 mg IV every 12 hours + metronidazole, 500 mg IV every eight hours |
| Severe, life-threatening: Patients with severe sepsis or admitted to intensive care |
| Imipenem/cilastatin (Primaxin), 500 mg IV every six hours |
| Meropenem (Merrem), 1 g IV every eight hours |
| Ertapenem, 1 g IV once daily |
| Doripenem (not available in the United States), 500 mg IV every eight hours |
| Piperacillin/tazobactam, 4.5 g IV every six hours |
| Cefepime, 2 g IV every eight hours + metronidazole, 500 mg IV or orally every eight hours |
| Ceftazidime (Fortaz), 2 g IV every eight hours + metronidazole, 500 mg IV or orally every eight hours |
| Ampicillin, 2 g IV every six hours + metronidazole, 500 mg IV or orally every eight hours + ciprofloxacin, 400 mg IV every 12 hours (or levofloxacin, 750 mg IV once daily) |
IV = intravenously.
*—Second-line in patients who are unable to tolerate beta-lactam antibiotics and metronidazole.
COMPLICATED ACUTE DIVERTICULITIS
- Diverticulitis is considered complicated in patients with abnormal vital signs, signs of perforation with or without abscess, fistula or obstruction, or the inability to maintain oral intake.
- Patients with complicated acute diverticulitis should be admitted to the hospital. Computed tomography with intravenous contrast should be obtained for patients with vital sign abnormalities or if there is a concern for abscess, perforation, or fistula.8,9,17
- Intravenous antibiotics should be initiated (Table 325,26 ).
- Bowel rest or clear liquid diet is recommended if the patient is able to tolerate oral intake, nothing by mouth if not.
- Abscesses smaller than 3 cm should be treated with intravenous antibiotics, and reevaluation if there is clinical deterioration. Imaging-guided percutaneous drainage is recommended for abscesses that are 3 cm or larger, with surgical consultation if needed. Surgical consultation is required for management of bowel perforation (Table 4).8,9,29–33
- The patient may be discharged home when vital signs normalize, pain is resolved or improving and can be controlled with oral medications, and the patient can tolerate oral intake.
TABLE 4. Management of Diverticulitis Complications
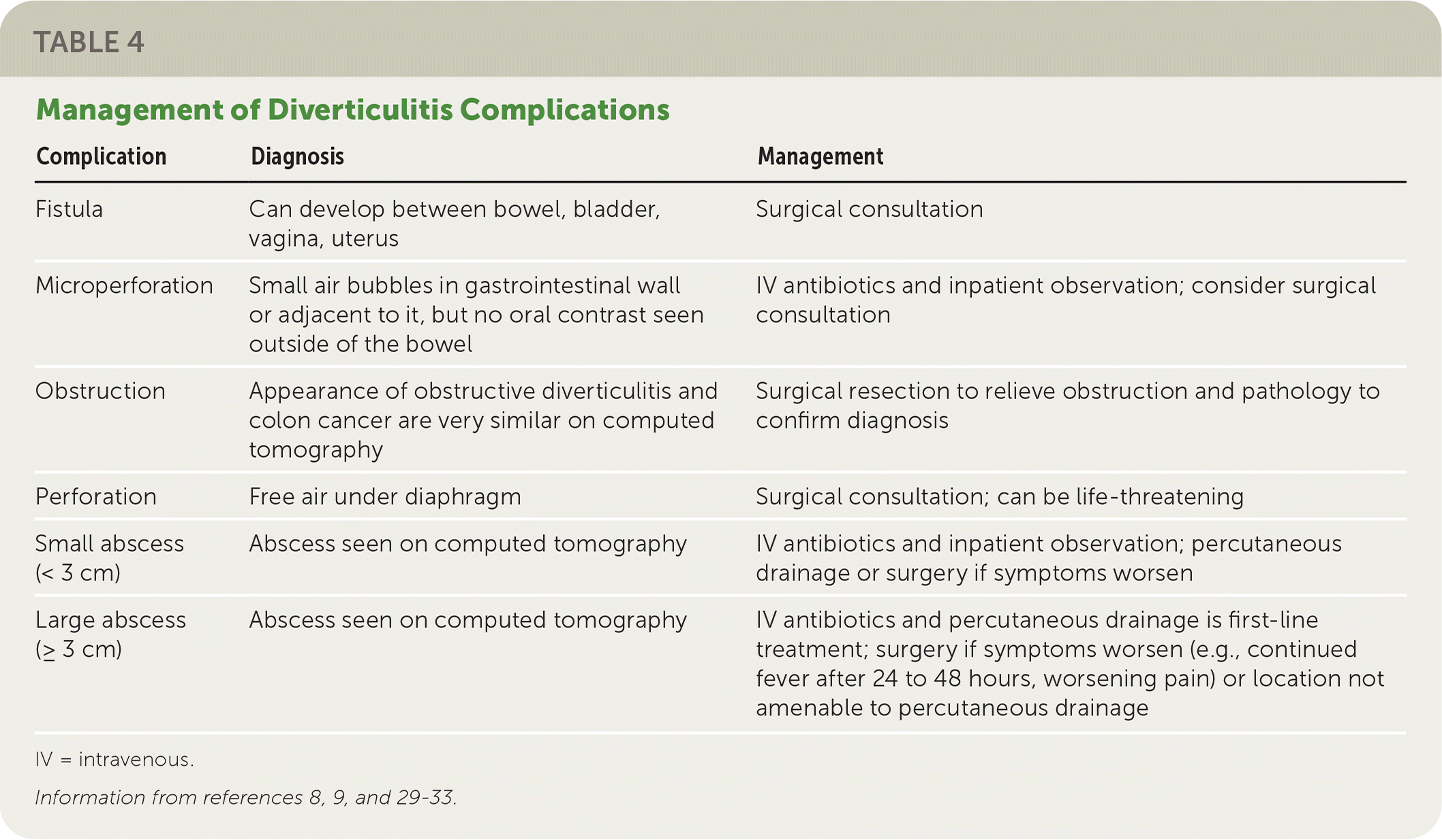
| Complication | Diagnosis | Management |
|---|---|---|
| Fistula | Can develop between bowel, bladder, vagina, uterus | Surgical consultation |
| Microperforation | Small air bubbles in gastrointestinal wall or adjacent to it, but no oral contrast seen outside of the bowel | IV antibiotics and inpatient observation; consider surgical consultation |
| Obstruction | Appearance of obstructive diverticulitis and colon cancer are very similar on computed tomography | Surgical resection to relieve obstruction and pathology to confirm diagnosis |
| Perforation | Free air under diaphragm | Surgical consultation; can be life-threatening |
| Small abscess (< 3 cm) | Abscess seen on computed tomography | IV antibiotics and inpatient observation; percutaneous drainage or surgery if symptoms worsen |
| Large abscess (≥ 3 cm) | Abscess seen on computed tomography | IV antibiotics and percutaneous drainage is first-line treatment; surgery if symptoms worsen (e.g., continued fever after 24 to 48 hours, worsening pain) or location not amenable to percutaneous drainage |
IV = intravenous.
SURGICAL MANAGEMENT: ACUTE MANAGEMENT
- The Hinchey classification can be used to guide acute surgical management.34,35
- Stage 1 (pericolic or mesenteric abscess) or stage 2 (walled-off pelvic abscess) is initially managed nonoperatively. If the patient does not improve, surgical intervention should be considered.
- For stages 3 or 4 (generalized purulent or feculent peritonitis), surgical consultation is needed if hemodynamically stable.
- Surgical approaches vary based on intraoperative findings and surgeon preference.9,36
SURGICAL MANAGEMENT: PREVENTION OF RECURRENCE
- Surgical intervention is based on recurrence risk and the patient's overall health status. Considerations for surgical referral include severity of pain or symptoms, complicated disease, potential for poor outcome, and the medical needs of the patient.8,9
- Surgical referral for partial colectomy after the third reoccurrence appears to be most cost-effective.37
- Abscess formation requiring drainage increases the risk of recurrence, and prophylactic partial colectomy should be considered.8,38,39
- Risk factors for recurrence include age older than 50 years, tobacco use, obstruction, peritonitis, and fistula formation.8,38
- Elective partial colectomy is no longer recommended in patients younger than 50 years at first occurrence of diverticulitis.40
AFTERCARE
- Colonoscopy should be considered six to eight weeks after symptom resolution in patients with complicated diverticulitis unless the patient has had a high-quality colonoscopy in the past year (colorectal cancer risk is 1.3% in uncomplicated diverticulitis and 7.9% in complicated diverticulitis).8,9,41,42
- If a patient with a history of diverticulitis has persistent pain, fecal calprotectin measurement (or C-reactive protein if unavailable), colonoscopy, or imaging should be considered to evaluate for ongoing inflammation.8,9,43
- Fecal calprotectin measurement may be useful for differentiating chronic inflammation from visceral hypersensitivity. One endoscopically confirmed case-control study (n = 48) showed 100% of patients with irritable bowel syndrome had a fecal calprotectin level less than 15 mcg per g, whereas 90% of patients with chronic diverticular inflammation had elevated fecal calprotectin (15 to 60 mcg per g).44
- Mesalamine has not shown benefit in the prevention of inflammation or diverticulitis recurrence and should not be used prophylactically.9,45
- Irritable bowel syndrome should be diagnosed in patients with persistent symptoms and a workup negative for chronic inflammation.9,46
Prognosis
- Most cases of diverticula are asymptomatic. The incidence is 0.46 per 1,000 person-years for diverticular bleeding and 1.5 to 6 per 1,000 person-years for diverticulitis.47
- Most cases of diverticulitis/diverticular disease will be uncomplicated (88%), and 12% will be complicated (abscess formation, fistula, obstruction).3,47
- After an initial episode of diverticulitis, the risk of having a second flare-up is 22% at 10 years. If a patient has a second occurrence, they have a 55% chance of a third occurrence in the next 10 years.3,9
- The overall risk of developing a complicated flare-up does not increase with subsequent flare-ups.9
This article updates previous articles on this topic by Wilkins, et al.,1 and Salzman and Lillie.48
Data Sources: A PubMed search was completed in Clinical Queries using the key terms diverticulitis and diagnosis, medical and surgical treatment, and prevention. The search was limited to meta-analyses, randomized controlled trials, clinical trials, reviews, and clinical guidelines. We also searched Essential Evidence Plus, the Agency for Healthcare Research and Quality evidence reports, Clinical Evidence, the Cochrane database, and DynaMed. Search dates: July 2021 and April 2022.

