Case Scenario
One of my practice partners noted in the electronic health record that our older colleague, M.C., recently prescribed a questionable medication to a patient. During discussions with other physicians in the practice, we recalled several conversations with M.C. in which he has talked about outdated treatments. My colleagues and I are unsure about whether M.C. is just not staying current with updated guidelines or whether he might have some cognitive issues. M.C. is well past traditional retirement age, and he has asserted that he will never retire. What are our professional obligations in this situation? Do we handle this ourselves, or do we turn to others? Who determines when a physician is no longer able to practice safely?
Commentary
There are many reasons why a physician's competence to practice medicine may decline over time. Optimal retirement age varies by person, and most medical practices do not have built-in retirement mandates. Age-related decline in cognitive function among physicians, even to the point of overt dementia, may become increasingly common as the U.S. physician population ages. Current estimates are that over the next 10 years, more than 40% of practicing physicians will be 65 years or older,1 an age group in which 11.7% of individuals self-report cognitive decline. 2 Although cognitive impairment is less common among highly educated individuals (such as physicians),3 population data indicate that as many as one in five physicians older than 70 years may have mild cognitive impairment, and about one in 15 may have some form of dementia.4
For other physicians, declining professional competency may simply be a matter of failing to stay current with evolving guidelines and advances in medicine. It has been long known that the more years a physician is in practice, the more likely the physician will have declining knowledge about current standards of care.5 Nearly two-thirds of physicians across multiple specialties report spending insufficient time keeping current in their area of practice.6 This problem is reflected in data showing that 4% to 13% of physicians in varying specialties fail their recertification examinations,7 and nearly 6% of family physicians do not even attempt recertification.8
Clinical performance can also be impaired by multiple stressors unrelated to age or cognitive impairment, such as family or financial problems and personal medical conditions, including mental health issues and substance use.
Physician colleagues or patients are the people most likely to express concerns about a physician who may not be practicing at the optimal standard of care. The nature of the concern and the circumstances can help determine the best course of action.
Some concerns can be handled within the practice and easily resolved. For example, a colleague may appear to be outdated in one area of practice but is otherwise performing well. This may be remedied by self-assessment through continuing education activities and peer monitoring with direct observation and chart reviews.9,10 Some health care systems even offer formal peer-monitoring programs. Other possibilities include limiting scope of practice to areas in which the physician's competence is not in question or reassignment to alternative duties such as administrative work rather than clinical practice. These reassignments can allow physicians to continue to contribute within their level of competence. However, this approach is appropriate only if there are minor concerns about the physician's practice and there are no threats to patient safety.
If an underperforming physician refuses to accept peer feedback or alternative responsibilities or if more serious concerns that involve potential threats to patient safety arise, it then becomes appropriate for colleagues (or students or residents working with the physician) to bring lapses in patient care to the attention of an appropriate supervisor (e.g., clinic director, department chair, hospital or health system credentialing committee) or, in many cases, to report those concerns to the state medical board.
The Federation of State Medical Boards, which represents all medical boards in the United States, has a guideline stating that physicians have a duty to report to their state medical board “anytime there is evidence or information that appears to show that a physician is incompetent, guilty of negligence, guilty of a violation of the medical practice act, engaging in inappropriate relationships with patients, is mentally or physically unable to practice safely, or has an alcohol or drug abuse problem.”11 Similarly, the American Medical Association Code of Medical Ethics states that physicians have an “obligation to report incompetent or unethical conduct that may put patients at risk.”12
Thirty-four U.S. states and territories have specific laws requiring physicians to personally report to their licensing board any peers whose practice or behaviors put patients at risk (Table 1).13 Many states also have requirements that hospitals, malpractice insurance companies, and other entities report such concerns.14
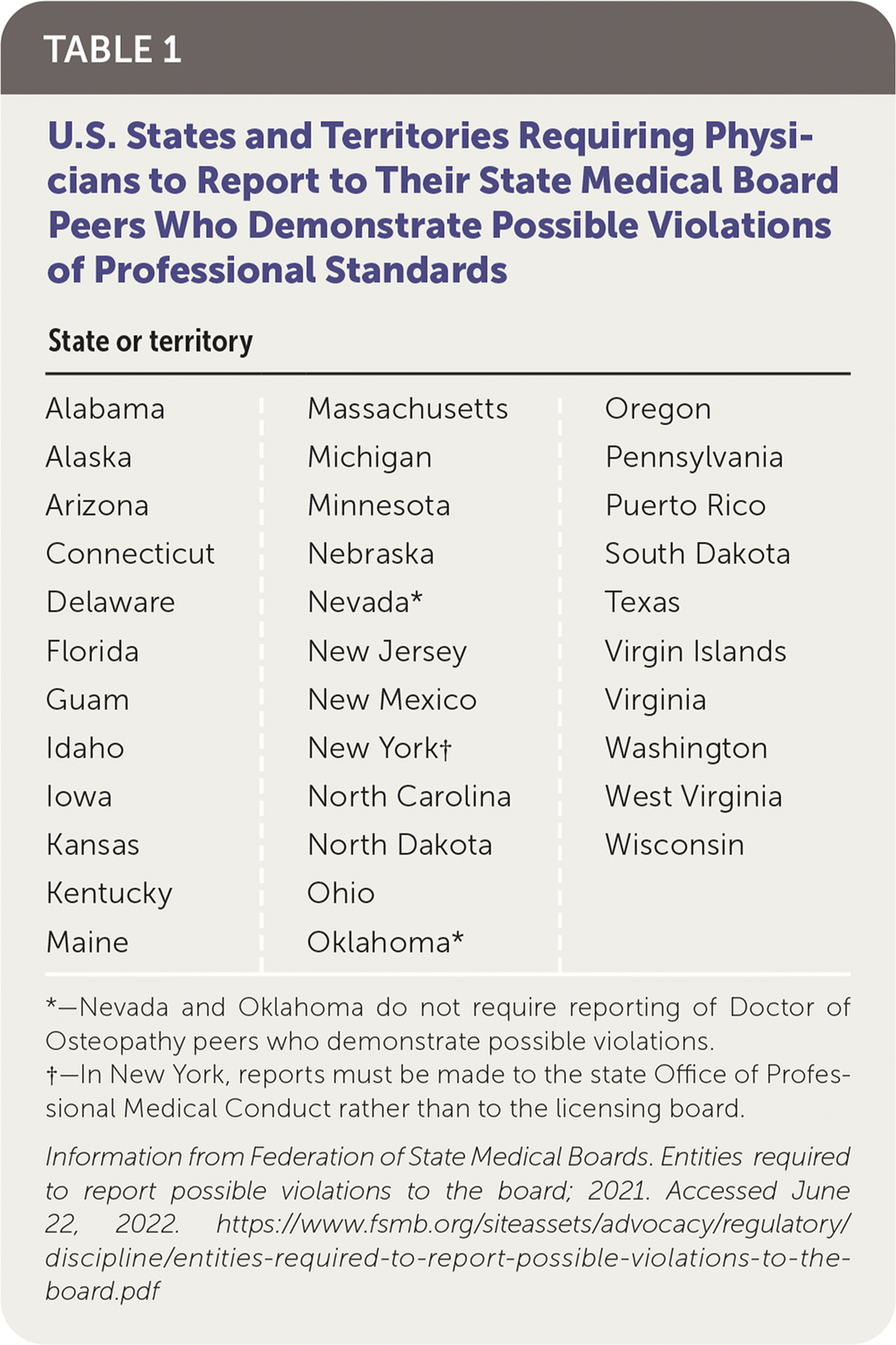
TABLE 1. U.S. States and Territories Requiring Physicians to Report to Their State Medical Board Peers Who Demonstrate Possible Violations of Professional Standards
| State or territory | ||
|---|---|---|
| Alabama Alaska Arizona Connecticut Delaware Florida Guam Idaho Iowa Kansas Kentucky Maine | Massachusetts Michigan Minnesota Nebraska Nevada* New Jersey New Mexico New York† North Carolina North Dakota Ohio Oklahoma* | Oregon Pennsylvania Puerto Rico South Dakota Texas Virgin Islands Virginia Washington West Virginia Wisconsin |
*—Nevada and Oklahoma do not require reporting of Doctor of Osteopathy peers who demonstrate possible violations.
†—In New York, reports must be made to the state Office of Professional Medical Conduct rather than to the licensing board.
Information from Federation of State Medical Boards. Entities required to report possible violations to the board; 2021. Accessed June 22, 2022. https://www.fsmb.org/siteassets/advocacy/regulatory/discipline/entities-required-to-report-possible-violations-to-the-board.pdf
State medical boards can be a resource for evaluating and managing concerns about professional competency. Medical boards review all complaints against physicians. When they receive complaints or reports from patients, peer physicians, hospitals, or other sources, the board's physician investigators and often outside consultants conduct a detailed review of all relevant medical records and may also interview the involved physician and patients. These investigative reports and other pertinent case records are reviewed by the board at their meetings, at which time the physician under investigation has the opportunity to respond to concerns raised in the investigation. The board then decides on what, if any, action should be taken.
ILLUSTRATIVE CASE FROM A STATE MEDICAL BOARD
A patient's family filed a complaint with their state medical board because the patient's physician made a serious and obvious error in managing the patient's condition, which created a question of physician competence. On review of the case records and other aspects of the physician's practice, it became apparent that this physician was not meeting minimal standards of medical care. Most of the physician's diagnostic and treatment plans were inappropriate.
The physician was given the opportunity to address the concerns raised by the board's investigators and consultants; however, during the interview, the physician was obviously confused and disoriented and demonstrated numerous signs of cognitive impairment. All members of the board, along with the board's investigators and consultants, agreed that the physician was a danger to patients if allowed to continue practicing. The physician's license was revoked.
The state in this case, similar to several others (Table 113 ), requires that physicians shall “report to the board any information that appears to show that a doctor of medicine is or may be medically incompetent.”14 Further board review of this case revealed that the physician's partners had already recognized his professional incompetence, but because of his status as senior partner and practice owner, they were not comfortable confronting him about his quality of care. The medical board disciplined and fined all the practice partners for failure to report to the board a physician who was incompetent to practice medicine.
Case Scenario Resolution
The concerned physicians in the case scenario should confer with M.C. and share their concerns in a caring and collegial manner. If M.C. appropriately recognizes that his current approach to providing medical care puts patients at risk and no alternative administrative or supervised role to obviate that risk is available or feasible, the next step is to strongly encourage M.C. to stop practicing. If M.C. insists on continuing to practice, you and your colleagues have an ethical responsibility, and in many states a legal responsibility, to report him to the state medical board.
Editor's Note: Dr. Weiss is an associate medical editor for American Family Physician.

