A 53-year-old man presented with concerns about swelling in his scrotum. The swelling appeared approximately three years earlier and had been increasing in size. It was painless and did not affect his walking, urination, erections, or ejaculation. He had no urethral discharge.
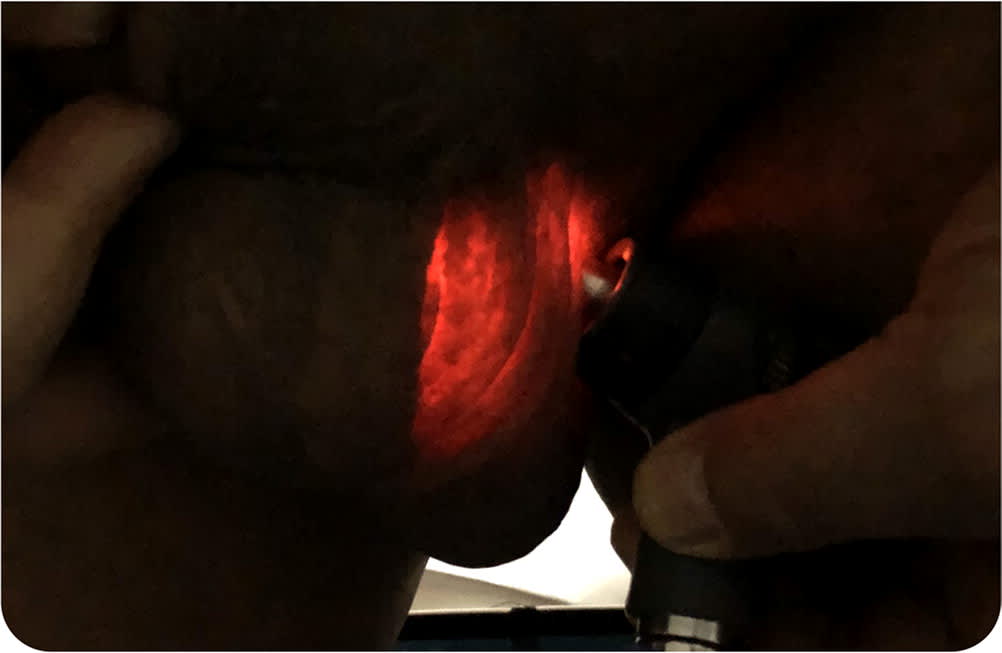
Physical examination revealed a left-sided scrotal mass (Figure 1) that was mobile, spongy, and ovoid. It was superior to the testicle and roughly twice the size. With the room lights turned off, an otoscope shined on the mass showed transillumination (Figure 2).
FIGURE 1

FIGURE 2
Question
Based on the patient’s history and physical examination findings, which one of the following is the most likely diagnosis?
- A. Epidermoid cyst.
- B. Hydrocele.
- C. Inguinal hernia.
- D. Testicular cancer.
- E. Varicocele.
Discussion
The answer is B: hydrocele. Hydroceles are benign masses that gradually form in the scrotum. They present as ovoid, nontender, mobile scrotal masses located superior or adjacent to the testicle. They consist of a persistent section of the processus vaginalis or tunica vaginalis and contain clear fluid. Hydroceles may appear at any age but are common in newborns, resolving in the first year of life. They are usually unilateral and appear insidiously. Hydroceles that form from a persistent processus vaginalis are situated superior to the testicle, and those that develop from the tunica vaginalis may overlap and obscure the adjacent testicle. In adults, hydroceles may result from conditions that cause lymphatic obstruction, including filariasis in tropical regions.1
Transillumination can aid in the diagnosis. Hydroceles transilluminate, whereas solid scrotal masses do not. Ultrasonography is needed to confirm the diagnosis and rule out other conditions.1
A hydrocele can be treated conservatively because it typically does not damage surrounding structures or cause pain. Larger hydroceles may be removed surgically.1
Epidermoid cysts, also called sebaceous cysts or epidermal inclusion cysts, are asymptomatic, slow-growing, firm, round nodules near the skin surface in areas with hair. They are commonly found on the scalp, neck, and torso, but smaller cysts are sometimes found on the scrotum. Epidermoid cysts do not transilluminate. They usually form from a ruptured pilosebaceous follicle when duct obstruction causes keratin and lipids to accumulate. If the cyst is expressed or ruptures, the discharge smells foul and looks like cottage cheese. These cysts are occasionally excised because of pain or recurrent infection.2
An inguinal hernia forms when abdominal contents pass through the inguinal canal into the scrotum. It presents as a soft, polypoid mass with a sensation of fullness, pressure, or pain in the scrotum or inguinal canal. The hernia is reducible and may descend on Valsalva maneuver. Bowel sounds may be auscultated with a stethoscope directly over the swelling. Inguinal hernias typically develop from a persistent processus vaginalis, allowing the tissue to follow it like a canal. These do not transilluminate.1
Testicular cancer presents as a firm mass in the center of the testicle or on its border. It can be painful or painless and does not transilluminate. Ultrasonography and laboratory testing for alpha fetoprotein, lactate dehydrogenase, and beta human chorionic gonadotropin are required to assist in diagnosis and staging. Urgent referral to urology for orchiectomy is recommended. Testicular masses are the most common malignant tumors in men 25 to 35 years of age.3
A varicocele is a collection of dilated veins from the venous plexus arising from the spermatic cord. On palpation, a varicocele feels like “a bag of worms.” It is benign and generally does not require treatment since the veins do not damage surrounding structures. Varicoceles can cause pain and may contribute to low sperm counts. Surgical treatment may be considered for infertility. Varicoceles are more common in individuals who are tall and thin. They generally occur on the left side of the scrotum and decrease in size when the patient is supine. Ultrasonography is needed to confirm the diagnosis. Varicoceles do not transilluminate.1
SUMMARY TABLE
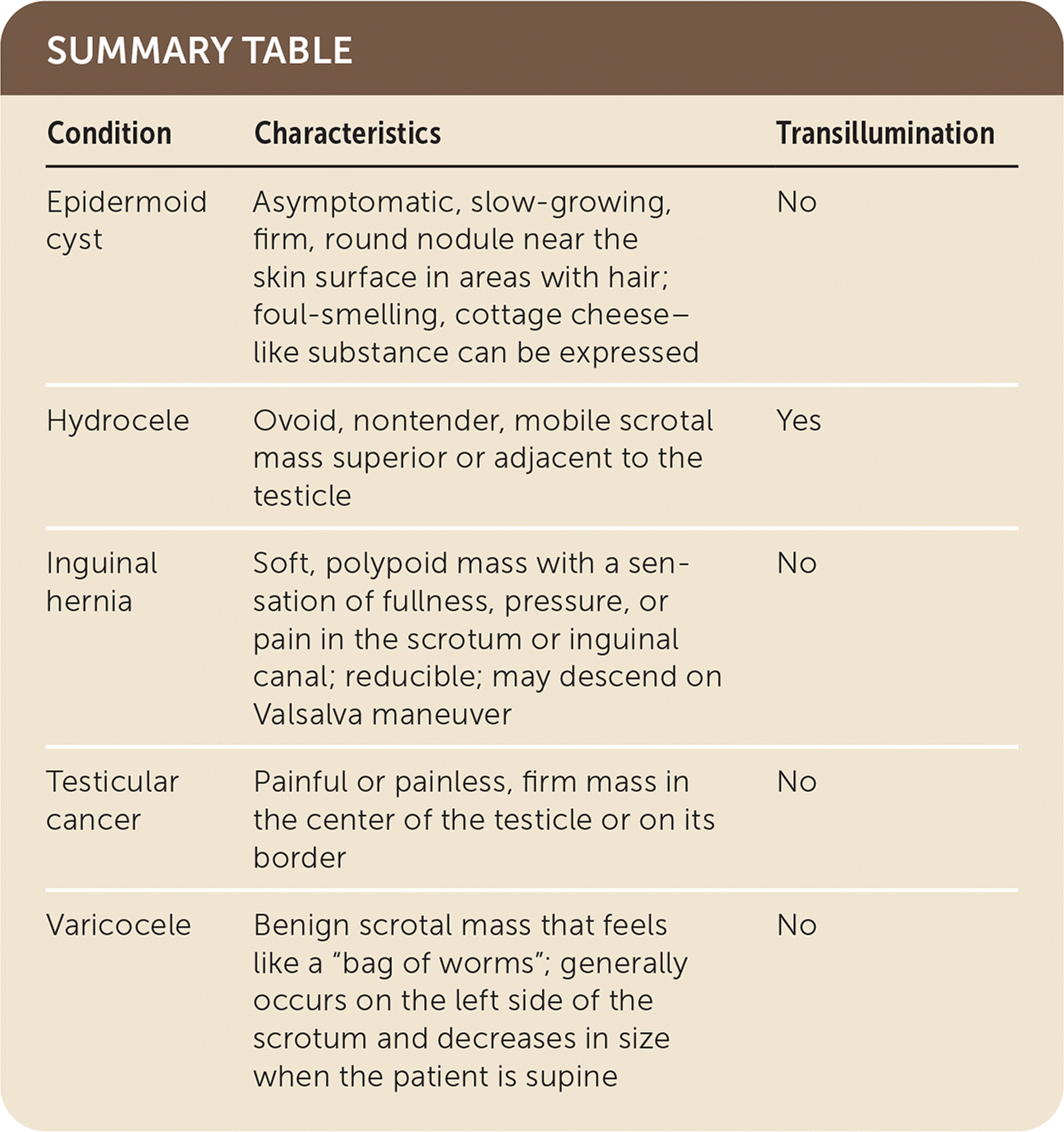
| Condition | Characteristics | Transillumination |
|---|---|---|
| Epidermoid cyst | Asymptomatic, slow-growing, firm, round nodule near the skin surface in areas with hair; foul-smelling, cottage cheese–like substance can be expressed | No |
| Hydrocele | Ovoid, nontender, mobile scrotal mass superior or adjacent to the testicle | Yes |
| Inguinal hernia | Soft, polypoid mass with a sensation of fullness, pressure, or pain in the scrotum or inguinal canal; reducible; may descend on Valsalva maneuver | No |
| Testicular cancer | Painful or painless, firm mass in the center of the testicle or on its border | No |
| Varicocele | Benign scrotal mass that feels like a “bag of worms”; generally occurs on the left side of the scrotum and decreases in size when the patient is supine | No |

