Case Scenario
My 83-year-old patient, E.P., with a history of Alzheimer disease, hypertension, hypothyroidism, and mild chronic obstructive pulmonary disease, has received care from a home health aide and family support in the home for two years. Although their comorbidities are stable, E.P. is now falling frequently, is experiencing delusions and hallucinations, has bowel and bladder incontinence, and is unable to dress and bathe properly. E.P. is no longer able to direct medical and executive affairs; however, their daughter (E.P.’s power of attorney) would like to look at options other than a long-term care facility and has asked for assistance in finding care alternatives for her parent. Financial resources are running out.
What are alternatives to long-term care facility placement? What are the critical issues I need to understand and what actions should I take to assist the patient and family in finding the most appropriate alternatives?
Commentary
The goal of care transitions for older adults is to promote the best possible safe functioning for the individual in the least restrictive environment throughout their late life. Some needs of older adults for assistance due to normal aging, medical comorbidities, or disablement may be anticipated if the physician and caretakers attend to the changing medical, psychosocial, and goals of care needs of the patient.
REASONS FOR TRANSITION
Common reasons for care transitions are listed in Table 1. The functional and behavioral problems of dementia are particularly taxing for patients and caregivers, and they often require care transitions to other environments.
TABLE 1. Reasons for Care Transitions in Adults

| Patient factors Decline in function (e.g., activities of daily living and instrumental activities of daily living such as mobility, self-care, communication) New, acute medical condition (e.g., injury, infection) Progression or exacerbation of chronic medical conditions resulting in need for external support (e.g., medication management, transportation, intravenous antibiotics, management of Foley catheter, wound care) Worsening cognitive impairment, dementia-related behavioral and psychological symptoms (e.g., aggression, agitation, delusions, hallucinations) |
| Family, caregiver, social, or environmental factors Caregiver burden or fatigue when family or caregiver cannot meet patient needs (e.g., medical, emotional, social) Environmental factors such as inadequate or unsafe housing, changes in transportation or community resources (e.g., pharmacy, grocery store) Financial limitations Loss of spouse or support group, social isolation, unbefriended older adult Physical distance between family and patient Time requirements |
| Transition from hospitalization Adapting to a new normal after hospitalization, surgery, or injury Education and management of new or progressing medical conditions Medication monitoring, adjustment, and adherence Need for therapy to improve or maintain function and independence |
| End-of-life care Hospice criteria are met* Respite services for caregivers |
*—Criteria available at https://www.cms.gov/medicare-coverage-database/view/lcd.aspx?LCDId=33393&ContrId=272&ContrVer=1&CntrctrSelected=272*1&Cntrctr=272&DocType=2.
CAREGIVER SUPPORT
Current or potential caregiver responsibilities and fatigue are essential considerations in patient transitions of care, especially if caregivers are themselves older adults or in poor health. Caregiver responsibilities can lead to adverse physical, emotional, financial, and functional outcomes for both the patient and caregiver and increased use of health and other supportive services. Caregiver fatigue and duties are powerful predictors of patient institutionalization and termination of home care.1 Caregivers should be screened for increasing burden, and their status must be considered when deciding on appropriate transitions of care.2 Early caregiver assessment and education, promotion of respite care, and discussions about advance care planning are critical responsibilities of the physician.3
EARLY PLANNING
Ideally, planning for provision of practical assistance in the home occurs years before a medical or social crisis. Aging in place is a concept that encourages older adults to create practical plans to meet future housing, financial, transportation, recreational, and health and wellness needs.4 Financial planning may include estate planning for those with substantial assets who can afford this service. Financial planning may also include consideration of long-term care insurance to facilitate more in-home care options than those covered by Medicare, such as nonskilled care or environmental modifications in the home.5
The resources available for older adult care are unique to each patient and community. Physician understanding of these resources within their community is important for answering questions about care options for older adults. Area Agencies on Aging can provide vital assistance and are accessible in all areas of the country.6 Consultation with a social worker can be invaluable in assisting the physician, patient, and family in choosing the most appropriate strategies for care.
COMMON OPTIONS FOR TRANSITIONS OF CARE
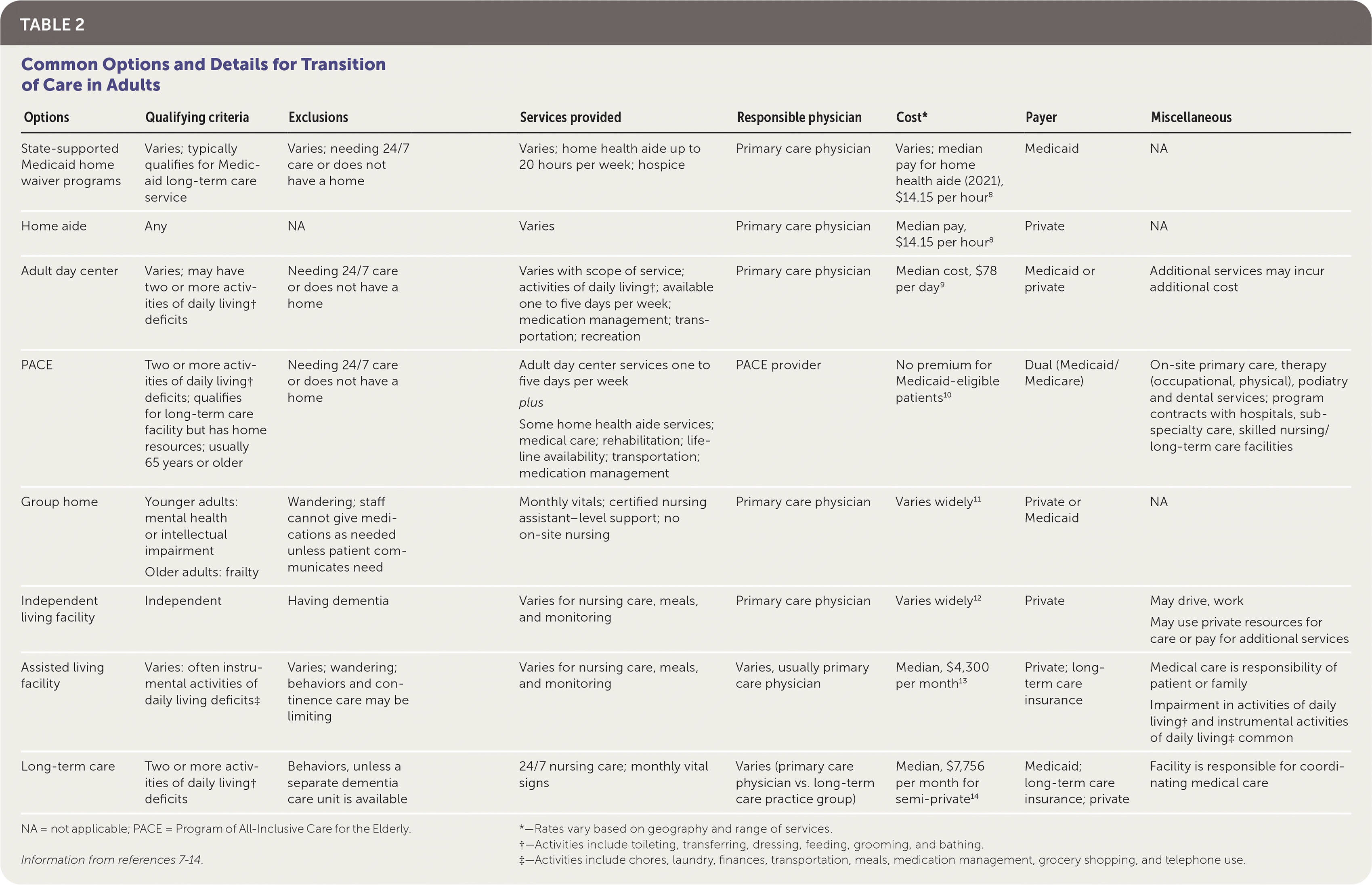
Table 2 presents transition of care options.7–14 The choice of setting is a dynamic interplay of factors, including needs, goals of care, patient preferences and capacity for directing their own affairs, caregiving support, and family and community resources. The continuum of care ranges from services in the home with aides, adult day centers, Programs of All-Inclusive Care for the Elderly (PACE), and facility-based care (ranging from group homes to long-term care facilities). Patient qualifications, scope of services, physician participation, and cost vary among the venues of care.
TABLE 2. Common Options and Details for Transition of Care in Adults
| Options | Qualifying criteria | Exclusions | Services provided | Responsible physician | Cost* | Payer | Miscellaneous |
|---|---|---|---|---|---|---|---|
| State-supported Medicaid home waiver programs | Varies; typically qualifies for Medicaid long-term care service | Varies; needing 24/7 care or does not have a home | Varies; home health aide up to 20 hours per week; hospice | Primary care physician | Varies; median pay for home health aide (2021), $14.15 per hour8 | Medicaid | NA |
| Home aide | Any | NA | Varies | Primary care physician | Median pay, $14.15 per hour8 | Private | NA |
| Adult day center | Varies; may have two or more activities of daily living† deficits | Needing 24/7 care or does not have a home | Varies with scope of service; activities of daily living†; available one to five days per week; medication management; transportation; recreation | Primary care physician | Median cost, $78 per day9 | Medicaid or private | Additional services may incur additional cost |
| PACE | Two or more activities of daily living† deficits; qualifies for long-term care facility but has home resources; usually 65 years or older | Needing 24/7 care or does not have a home | Adult day center services one to five days per week plus Some home health aide services; medical care; rehabilitation; life-line availability; transportation; medication management | PACE provider | No premium for Medicaid-eligible patients10 | Dual (Medicaid/Medicare) | On-site primary care, therapy (occupational, physical), podiatry and dental services; program contracts with hospitals, subspecialty care, skilled nursing/long-term care facilities |
| Group home | Younger adults: mental health or intellectual impairment Older adults: frailty | Wandering; staff cannot give medications as needed unless patient communicates need | Monthly vitals; certified nursing assistant–level support; no on-site nursing | Primary care physician | Varies widely11 | Private or Medicaid | NA |
| Independent living facility | Independent | Having dementia | Varies for nursing care, meals, and monitoring | Primary care physician | Varies widely12 | Private | May drive, work May use private resources for care or pay for additional services |
| Assisted living facility | Varies: often instrumental activities of daily living deficits‡ | Varies; wandering; behaviors and continence care may be limiting | Varies for nursing care, meals, and monitoring | Varies, usually primary care physician | Median, $4,300 per month13 | Private; long-term care insurance | Medical care is responsibility of patient or family Impairment in activities of daily living† and instrumental activities of daily living‡ common |
| Long-term care | Two or more activities of daily living† deficits | Behaviors, unless a separate dementia care unit is available | 24/7 nursing care; monthly vital signs | Varies (primary care physician vs. long-term care practice group) | Median, $7,756 per month for semi-private14 | Medicaid; long-term care insurance; private | Facility is responsible for coordinating medical care |
NA = not applicable; PACE = Program of All-Inclusive Care for the Elderly.
Information from references 7–14.
*—Rates vary based on geography and range of services.
†—Activities include toileting, transferring, dressing, feeding, grooming, and bathing.
‡—Activities include chores, laundry, finances, transportation, meals, medication management, grocery shopping, and telephone use.
FINANCIAL CONSIDERATIONS
For patients with private insurance, long-term care insurance, and/or financial resources, continuing care retirement communities may be an option. Additionally, assisted living facilities and memory support units may be available to support patients who do not require long-term care services.
If financial constraints are present, choices may be limited to programs with Medicaid payment options. Medicaid is the primary payer source for long-term and community-based care services, so planning is important before health deteriorates or an urgent or emergent situation occurs.15 Patients and families make better decisions when not stressed; anticipatory planning can be presented as integral to prudent, thoughtful prospective care. Often the need for Medicaid services arises in a crisis when the patient and caregivers cannot safely sustain the current living environment. Community-based care and aging in place are usually preferred. Understanding of Medicaid benefits promotes in-home care to manage the current situation and facilitates planning for long-term care placement if needed. Medicaid guidelines for long-term care and community services vary from state to state, making resources more accessible in some states than others.16
Families often hold the misconception that Medicare will provide additional support in the home for activities of daily living and instrumental activities of daily living, such as bathing and meal preparation. Medicare covers only up to 100 days per year of inpatient skilled nursing facility services and does not pay for unskilled home-based care.5 As a result, many individuals struggle with meeting care needs and must exhaust almost all their financial resources until they qualify for Medicaid. Encouraging early Medicaid enrollment for qualifying patients fosters timely delivery of care.
A best practice is to refer patients and caregivers to local Medicaid offices for information on specific guidelines and available resources. The universal requirements for Medicaid services include meeting state-specific residency, citizenship, age, and disability requirements.17 Medicaid long-term care waivers require disclosure of individual and spousal income and assets, with the threshold amount for eligibility being different in each state. Financial eligibility can be modified by factors such as spousal protection, burial needs and plans, and nonsalable property. States require a person to meet “nursing home level of care” (i.e., that the individual has a physical and/or mental condition requiring skilled nursing care and/or assistance with several activities of daily living). Screening tools such as Universal Assessment Instruments are used to determine medical and functional eligibility.18 An individual must meet both disability and financial requirements to qualify for Medicaid-funded services in the community.19 Physician input may be helpful in clarifying issues that arise regarding disability or medical necessity assessments performed by state agencies.
Case Resolution
E.P.’s comorbidities of hypothyroidism, hypertension, and mild chronic obstructive pulmonary disease are stable and require only maintenance care, and E.P.’s dementia is progressive. The predictable behavioral and functional components of decline need to be continuously addressed. The patient and family do not have financial resources for enrollment in an assisted living facility or memory support unit. Clinical social work consultation or referral to local Area Agencies on Aging should assist the patient’s family in completing the Universal Assessment Instrument and applying for Medicaid benefits. Informational materials should be provided to the family about community resources, including the community adult day center and the local PACE program, with encouragement to tour both facilities. A goal of care for the patient and family members is to continue their relationships with the patient’s primary physician. The adult day center does not require changing responsibility of primary care to the PACE program’s health care personnel. The physician should assist the family in completing any clinical documents needed for day facility enrollment. Regular follow-up visits to address the patient’s evolving status should be scheduled, and physicians should work closely with the family to determine a potential future change in care environment.

