Case Scenario
My 85-year-old patient, E.P., with a history of Alzheimer disease, hypertension, hypothyroidism, and mild chronic obstructive pulmonary disease, has been receiving adult day center support and family care for their Alzheimer disease. E.P. is now wheelchair walking, experiencing delusions and hallucinations, has bowel and bladder incontinence, and is dependent in all activities of daily living. E.P. has not been able to direct their medical and executive affairs for a few years. The adult care center cannot continue to provide services for E.P., and the family is unable to provide further assistance. A family member (E.P.’s guardian) is asking for help with placing E.P. in a long-term care facility. E.P. currently receives Medicaid support. What critical steps do I need to understand and take to assist the patient and their family in transitioning E.P. into a long-term care facility? What information and documentation does the facility need from me to effectively manage this transition?
Commentary
Part 1 of this Curbside Consultation, published in the November 2022 issue of American Family Physician, discussed the importance of planning for long-term care support and services, including strategies for aging in place, alternatives to long-term care facilities, long-term care insurance, and Medicaid requirements.1 In the case stated here, these alternatives have been exhausted, and the patient now requires care in a long-term facility.
This patient’s experience is a common one. In the United States, approximately 1.3 million people live in 15,600 long-term care facilities; 90% of these individuals are 65 years and older.2 About 60% use Medicaid as a payer source.2 Nearly 50% of patients in long-term care facilities have dementia, and the majority experience impairments in activities of daily living.2
Selection of a long-term care facility is influenced by many factors, including social and cultural norms, timing of placement (e.g., from hospital vs. from home), language, and family dynamics. Selection is most heavily influenced by location, with the usual goal of being close to family and friends. Secondary factors include facility resources and cost, staffing, racial and language concordance (e.g., Spanish-speaking staff), patient experiences, and the patient’s and family’s overall sense of comfort and confidence in the facility.3,4 The Alzheimer’s Association (https://www.alz.org) and community Area Agencies on Aging can be valuable resources. The U.S. Centers for Medicare and Medicaid Services collects quality data on long-term care facilities and hosts a website for consumers to compare facilities within a community. The site provides information on facilities’ health inspection results, staffing ratios, and quality measures.5 Patients and families should be shown and encouraged to use available resources to guide facility selection.
Long-term care facility placement is likely to result in a transition of medical practice. Only 10% of primary care physicians provide long-term care, and numbers continue to decline.6,7 Care of adults who are frail and who have medical complexities is increasingly provided by nurse practitioners and physician assistants dedicated to care in a long-term care environment.6,7 Long-term care facility staff utilize an interdisciplinary team approach to attend to the physical, medical, nutritional, functional, recreational, emotional, social, and environmental needs of residents. Poor communication of the patient’s medical, functional, cognitive, emotional, and social function will result in concomitantly poor transitional care, which increases the risk of medical errors, inappropriate care, adverse outcomes, and patient and family dissatisfaction.8
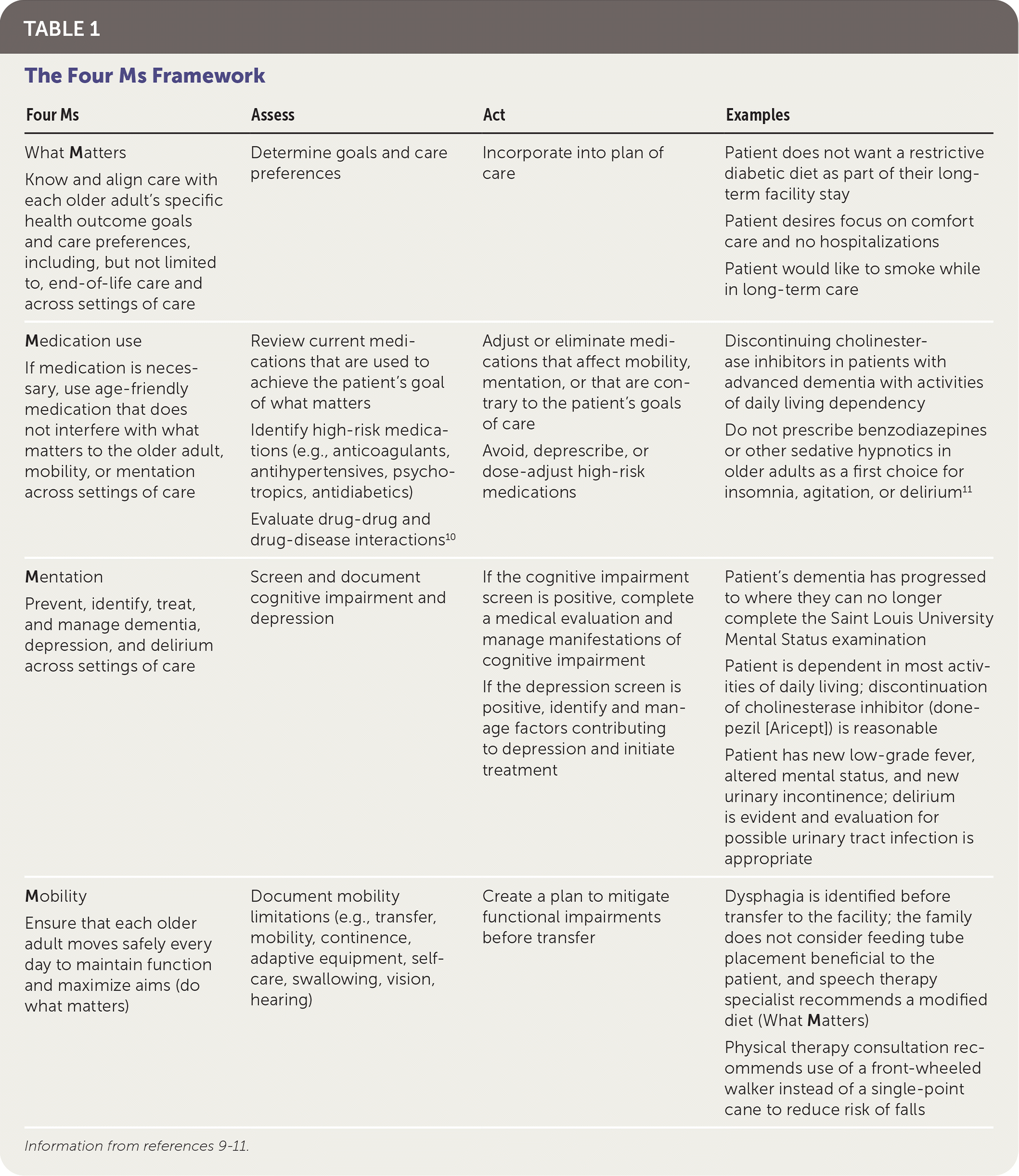
The physician’s focus in transitioning the patient to a long-term care facility is captured in the 4Ms framework described by the Institute for Healthcare Improvement.9 Before the move to the facility, the physician should explore the 4Ms: what Matters to the patient and family for future care, Medication use, Mentation, and Mobility (Table 19–11 ). Multimorbidity is often considered a fifth M in this care paradigm because these patients commonly have dementia, depression, hypertension, diabetes mellitus, chronic obstructive pulmonary disease, chronic kidney disease, vascular disease, and/or gastroesophageal reflux disease.12,13
TABLE 1. The Four Ms Framework
| Four Ms | Assess | Act | Examples |
|---|---|---|---|
| What Matters Know and align care with each older adult’s specific health outcome goals and care preferences, including, but not limited to, end-of-life care and across settings of care | Determine goals and care preferences | Incorporate into plan of care | Patient does not want a restrictive diabetic diet as part of their long-term facility stay Patient desires focus on comfort care and no hospitalizations Patient would like to smoke while in long-term care |
| Medication use If medication is necessary, use age-friendly medication that does not interfere with what matters to the older adult, mobility, or mentation across settings of care | Review current medications that are used to achieve the patient’s goal of what matters Identify high-risk medications (e.g., anticoagulants, antihypertensives, psychotropics, antidiabetics) Evaluate drug-drug and drug-disease interactions10 | Adjust or eliminate medications that affect mobility, mentation, or that are contrary to the patient’s goals of care Avoid, deprescribe, or dose-adjust high-risk medications | Discontinuing cholinesterase inhibitors in patients with advanced dementia with activities of daily living dependency Do not prescribe benzodiazepines or other sedative hypnotics in older adults as a first choice for insomnia, agitation, or delirium11 |
| Mentation Prevent, identify, treat, and manage dementia, depression, and delirium across settings of care | Screen and document cognitive impairment and depression | If the cognitive impairment screen is positive, complete a medical evaluation and manage manifestations of cognitive impairment If the depression screen is positive, identify and manage factors contributing to depression and initiate treatment | Patient’s dementia has progressed to where they can no longer complete the Saint Louis University Mental Status examination Patient is dependent in most activities of daily living; discontinuation of cholinesterase inhibitor (donepezil [Aricept]) is reasonable Patient has new low-grade fever, altered mental status, and new urinary incontinence; delirium is evident and evaluation for possible urinary tract infection is appropriate |
| Mobility Ensure that each older adult moves safely every day to maintain function and maximize aims (do what matters) | Document mobility limitations (e.g., transfer, mobility, continence, adaptive equipment, self-care, swallowing, vision, hearing) | Create a plan to mitigate functional impairments before transfer | Dysphagia is identified before transfer to the facility; the family does not consider feeding tube placement beneficial to the patient, and speech therapy specialist recommends a modified diet (What Matters) Physical therapy consultation recommends use of a front-wheeled walker instead of a single-point cane to reduce risk of falls |
WHAT MATTERS?
Ideally, the competent patient should transition to the facility with an advance directive and medical and financial powers of attorney in place to guide care and manage executive affairs in the event of a medical crisis. Transitioning an incompetent patient to a facility requires collaborating with the patient’s designated responsible party. The patient’s advance medical directive should be reviewed and updated accordingly if the patient’s wishes change before transfer to the facility. When appropriate, do not resuscitate (DNR) orders or physician orders for scope of treatment (POST) discussions and other orders should be completed before the transition by the trusted physician who has known the patient and/or family. Addressing what matters helps align medical therapies (e.g., de-escalating medications, artificial nutrition) with the goals of care.
MEDICATION USE
The medication list (ideally, a “brown-bag review” of actual medications on hand) should be reviewed in detail with the patient and/or family before transfer to a long-term care facility. More than one-half of patients in long-term care facilities take six or more medications.14 The goal of this review is not only to reduce drug-drug and drug-disease interactions but also to ensure that the medical therapies align with goals of care.10,11 For example, the review could identify unreported use of over-the-counter sedatives or highly anticholinergic medications that may contribute to confusion. For the purposes of transfer, scheduled medications are generally preferred over as-needed medications because patients in long-term care facilities may not be able to communicate their needs for treatment.
In addition, the transferring physician should communicate all relevant medical and social history, especially concerning multimorbidities (i.e., the fifth M) and address pertinent infectious disease screening requirements. Screening requirements for communicable diseases vary by facility and communities. Screening for tuberculosis is performed because of the risk of exposure to tuberculosis and the risk of progression from latent tuberculosis infection to tuberculosis disease.15
MENTATION
Before transition to a long-term care facility, patients should be assessed for cognitive impairment using validated tools (e.g., the Montreal Cognitive Assessment, the Saint Louis University Mental Status examination).16,17 The mentation evaluation should include an assessment of the patient’s capacity to manage their medical and executive affairs, as well as to formulate advance directives or name a surrogate decision maker. In addition to cognition, screening for depression using validated tools (e.g., Geriatric Depression Scale, Patient Health Questionnaire-9) is recommended.18,19 Management plans for any dementia-related behaviors and psychiatric symptoms should be reported in the transfer documentation.
MOBILITY
Communicating the mobility (functional) abilities and needs of the patient can foster a smoother transition to the facility by ensuring that adaptive equipment and/or nursing support is available to promote safe patient mobility and self-care. This functional assessment focuses on advanced activities of daily living (e.g., recreation, hobbies), instrumental activities of daily living (e.g., chores, medication management), and activities of daily living (e.g., toileting, dressing).
Case Resolution
The patient and family do not appear to have financial resources for an assisted living/memory support unit, and community-based care has been exhausted. Long-term care facility placement is needed to support the patient and family. Physician consultation with a clinical social worker can assist the patient’s family in discerning long-term care facility selection within the community. The practice does not support the primary care physician serving as a long-term facility attending physician; therefore, the patient’s care is transferred to the practice group supporting the chosen facility. The primary care physician should then assist the family in completing any clinical assessments (including required tuberculosis and communicable disease screening and immunization updates) and administrative actions needed for facility enrollment. A Universal Transfer Form is available to provide to the family and facility (https://www.aafp.org/pubs/afp/issues/2010/0515/p1219.html#afp20100515p1219-f1a). The primary care physician should be available to members of the clinical team at the facility for any questions that arise during their assumption of care.

