Clinical Question
How accurate are history and physical examination in diagnosing testicular torsion?
Evidence Summary
Testicular torsion has an annual incidence of approximately 1 in 4,000 males younger than 25 years.1 It is more common in children and adolescents, and delayed repair can result in the loss of the testis.1 Therefore, prompt and accurate diagnosis is important when patients present with acute scrotal or testicular pain.
Testicular torsion typically presents with unilateral scrotal pain that begins suddenly. Individual clinical findings that best predict testicular torsion include nausea and vomiting, past trauma, a tender testicle, an abnormal testicular lie (i.e., elevated or transverse), and an absent cremasteric reflex.2,3 This reflex is triggered by gently scraping the medial thigh adjacent to the testis and looking for the testicle to retract. The patient must be comfortable and the examination room should be warm for this finding to be observed.
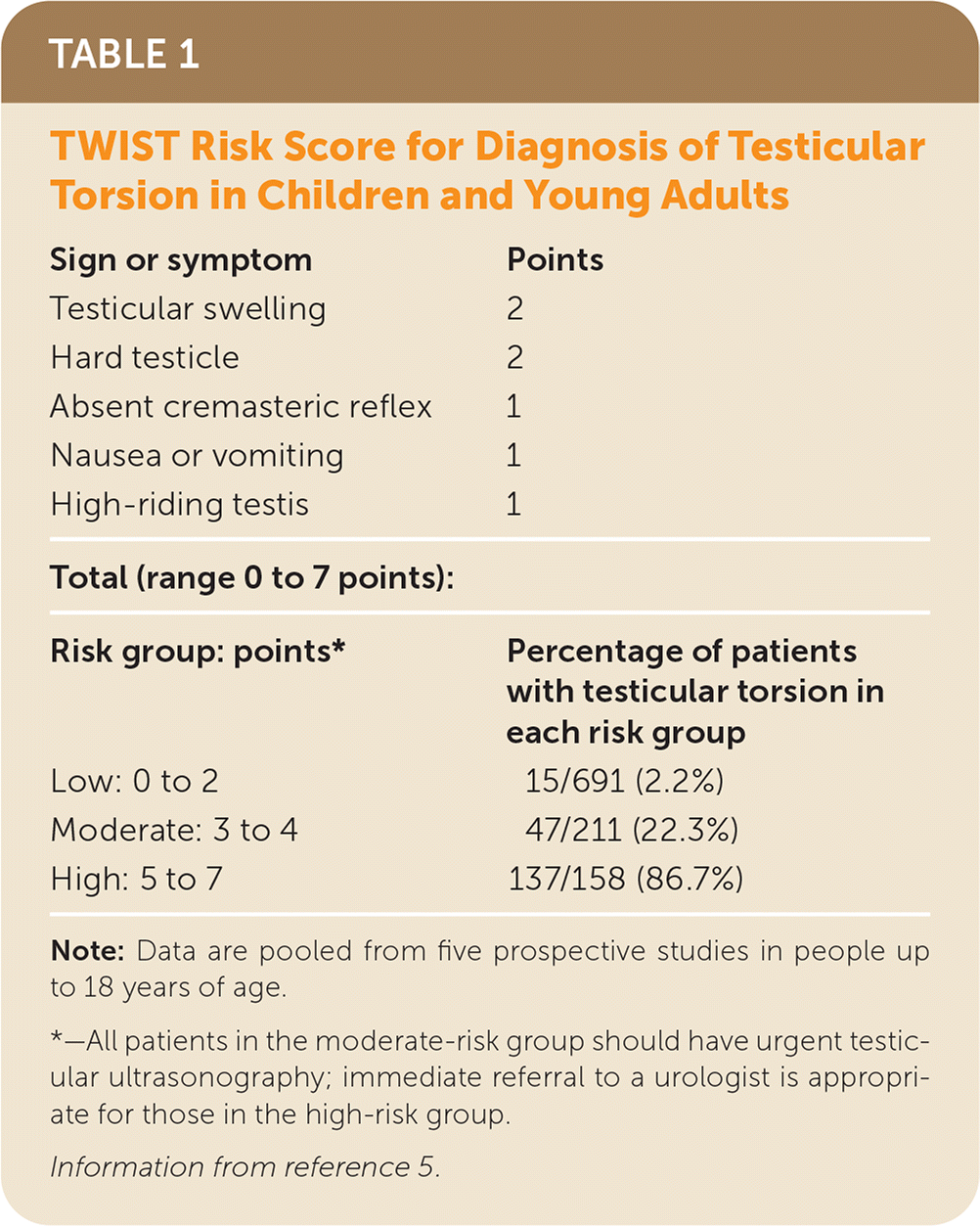
In 2013, a simple risk score for the diagnosis of testicular torsion was developed by Barbosa and colleagues.4 The authors called it the Testicular Workup for Ischemia and Suspected Torsion, or TWIST, score. It included five signs or symptoms and divided patients into low-, moderate-, and high-risk groups (Table 15 ). A systematic review and meta-analysis identified 13 studies that evaluated the accuracy of the TWIST score. Eight studies gathered data prospectively, and five gathered data prospectively in populations 18 years and younger.5 Limiting the reporting to prospective studies is appropriate because documentation of signs and symptoms can be inconsistent in the electronic health record. All studies used scrotal ultrasonography as the reference standard.
TABLE 1. TWIST Risk Score for Diagnosis of Testicular Torsion in Children and Young Adults
| Sign or symptom | Points |
| Testicular swelling | 2 |
| Hard testicle | 2 |
| Absent cremasteric reflex | 1 |
| Nausea or vomiting | 1 |
| High-riding testis | 1 |
| Total (range 0 to 7 points): | |
| Risk group: points* | Percentage of patients with testicular torsion in each risk group |
| Low: 0 to 2 | 15/691 (2.2%) |
| Moderate: 3 to 4 | 47/211 (22.3%) |
| High: 5 to 7 | 137/158 (86.7%) |
Note: Data are pooled from five prospective studies in people up to 18 years of age.
*—All patients in the moderate-risk group should have urgent testicular ultrasonography; immediate referral to a urologist is appropriate for those in the high-risk group.
Information from reference 5.
Pooled data from the five prospective studies in children and adolescents showed that the TWIST score is accurate. The low-risk group included 691 patients, and 2.2% were diagnosed with testicular torsion; the moderate-risk group included 211 patients, and 22.3% were diagnosed; and the high-risk group included 158 patients, and 86.7% were diagnosed. All 50 patients with a score of 7 had testicular torsion, whereas only four of 392 (1.0%) patients with a score of 0 or 1 had it. The area under the receiver operating characteristic curve was 0.924, which indicates that the TWIST score is highly accurate.
There are fewer studies about the accuracy of the TWIST score in adults. In a prospective study that enrolled 68 adult men (i.e., 16 years and older if postpubertal) presenting with acute scrotal pain, one-half were diagnosed with testicular torsion.6 The score performed well: zero of 23 in the low-risk group (0 to 2 points) had testicular torsion compared with seven of 15 in the moderate-risk group (3 to 4 points) and 27 of 30 in the high-risk group (5 to 7 points). Eighteen patients had a score of 6 or 7, and all were diagnosed with testicular torsion.
Applying the Evidence
A 12-year-old boy presents with acute onset of testicular pain. On examination, the testicle is not hard but is swollen and high riding. The cremasteric reflex is absent. He denies nausea or vomiting. He has a TWIST score of 4 points and is at moderate risk for testicular torsion, with a 22% probability. You refer him for urgent ultrasonography.

