Key Points for Practice
• Annual LDCT screening of current smokers and those who quit within 15 years of screening between 50 and 80 years of age reduces mortality with a number needed to screen ranging, based on baseline, from 161 to 5,276 to prevent one death over 10 years.
• Risks of LDCT screening include unnecessary additional procedures and procedure complications, including an NNH of 2,500 for death after procedures and an estimated NNH of 2,500 for death caused by radiation exposure from annual screening examinations.
• In patients with multiple comorbidities, the balance between benefit and harm can shift dramatically because benefits are less likely, procedural risks increase, and overdiagnosis becomes more likely.
• Successful LDCT screening programs require multidisciplinary teams to respond to abnormal results using established algorithms.
From the AFP Editors
Lung cancer screening with low-dose computed tomography (LDCT) involves a mix of risks and benefits to individual patients despite consistent evidence of population-level benefit. The American College of Chest Physicians published guidelines for lung cancer screening based on a systematic review.
Mortality Benefit of Screening
LDCT screening reduces lung cancer–related mortality in people 50 to 80 years of age with a 20-pack-year history who continue to smoke or have quit within 15 years of screening. For the highest-risk people in this group, LDCT has a number needed to screen of 161 to prevent one death from lung cancer over 10 years due to two screening examinations compared with usual care. For this group, the number needed to screen is 354 compared with annual chest radiography. The benefits of LDCT screening are dependent on underlying clinical risk because the 20% of patients eligible for screening with lowest risk have a number needed to screen of 5,276 over 10 years.
Lung cancer mortality decreases when screening starts at 50 years of age, whereas benefits are not certain when screening starts at 55 or 60 years of age. Similarly, lung cancer mortality improvements are clear only when screening continues to at least 75 years of age. Annual and biennial screening decrease lung cancer mortality. Although men have clearer evidence of reduced mortality, the absolute benefit may be higher in women. Current smokers and recent smokers who quit within 15 years of screening appear to have similar benefits from screening.
Harms of Screening
The major harm from LDCT screening is the identification of nonmalignant nodules, which will be found in up to 40% of screening examinations and lead to invasive procedures in 3% of patients screened. About one-third of patients who undergo biopsy are found to have benign disease. Screening leads to a number needed to harm (NNH) of 213 for surgeries resulting in benign disease. For death after invasive procedures due to LDCT screening, the approximate NNH is 2,500, and for procedural adverse events, the NNH is 323.
An additional harm of annual LDCT screening is ionizing radiation exposure from repeated scans, which leads to an estimated NNH of 2,500 for one additional death caused by radiation exposure from screening based on protocols used in early trials. Current protocols reduce radiation exposure by 40%, leading to one radiation-induced cancer for every 108 lung cancers detected over 10 years.
Limited evidence does not suggest psychosocial harm from the detection of lung nodules. Indeterminate results on LDCT do not appear to increase short- or long-term anxiety compared with negative results.
Overdiagnosis
Overdiagnosis in lung cancer screening is best defined as the detection, with subsequent treatment, of lung cancer that would not have otherwise impacted well-being or mortality. Nearly one in five tumors found in the largest screening trial was estimated to have been overdiagnosed, resulting in more than one overdiagnosed lung cancer for every lung cancer death averted. Patients with limited life expectancy have increased risk of harm from procedures for overdiagnosed cancers. Because the five-year survival rate for people who meet Medicare eligibility for LDCT screening is 9% less than those eligible for the LDCT trial, overdiagnosis may be more prevalent in the general LDCT-eligible population.
Cost-effectiveness
Although LDCT screening is considered cost-effective, estimates range from $28,000 to $243,000 per quality-adjusted life-year gained.
Risk Calculators
The U.S. Preventive Services Task Force (USPSTF) recommends screening adults 50 to 80 years of age with a 20-pack-year history of smoking. This is estimated to reduce mortality with a number needed to screen of 820 compared with the previous USPSTF criteria of 55 to 75 years of age and 30-pack-year smoking history, but at the cost of nearly doubling the populations who are eligible for screening. Because of this, several risk calculators have been developed to add clarity to screening decisions.
The Lung Cancer Death Risk Assessment Tool (https://analysistools.cancer.gov/lungCancerRiskAssessment/#/) has the best evidence for targeting screening. Using an assessment tool threshold of 1.4% risk of death instead of the previous USPSTF criteria results in screening the same number of people while including 15% more people who have the potential to benefit from screening. Because these calculators note increased risk in older people, the risk should be balanced with considerations of life expectancy.
Minimizing Disparities
Black people have elevated lung cancer mortality and greater potential benefit from screening. LDCT screening is underused overall, with even lower rates of screening in minority populations, people with lower socioeconomic status, and those with lower education levels. These disparities appear to be worsened by restrictive screening criteria. Expanding the smoking eligibility criteria to 20 pack-years from 30 pack-years and the age eligibility to 50 years of age from 55 years may partially correct these disparities.
Comorbidities
In addition to their effect on life expectancy, patient comorbidities affect the harms and benefits of screening. Patients with more comorbidities have greater harms from LDCT screening because mortality from surgical resection increases. The benefits of screening vary depending on the comorbidity. Yet, when screening continues to 80 years of age instead of 75 years, lung cancer mortality improves by 10% at the cost of increased screening. Although comorbidities influence the benefits and risks of screening, continuing screening into older age improves mortality.
Pulmonary comorbidities decrease the benefits of screening. In patients with two or more pulmonary conditions, LDCT screening is less beneficial. Chronic obstructive pulmonary disease confers a higher risk of lung cancer while also increasing overall mortality and surgical risks. With poor functional status, LDCT screening may not be beneficial.
Screening Programs
Successful screening requires two elements: adequate shared decision-making before screening and organized multidisciplinary programs to evaluate abnormal results.
Shared decision-making is required by Medicare, including determination of eligibility, review of benefits and harms, next steps, and smoking cessation. Benefit and harm discussions should include false-positive rates, possible subsequent evaluations, radiation exposure, and repeat screening.
Standardized criteria, currently represented by the Lung-RADS criteria, guide evaluation of findings by nodule size and characteristics to inform subsequent analysis. Smoking cessation counseling with lung cancer screening leads to slightly increased quit rates.
Lung cancer screening follow-up often involves primary care physicians, pulmonologists, radiologists, thoracic surgeons, medical and radiation oncologists, nursing staff, information technology experts, schedulers, and administrative staff. Structured reports should include evidence-based management recommendations or centralized management of pulmonary and nonpulmonary findings.
G-TRUST GUIDELINE SCORECARD
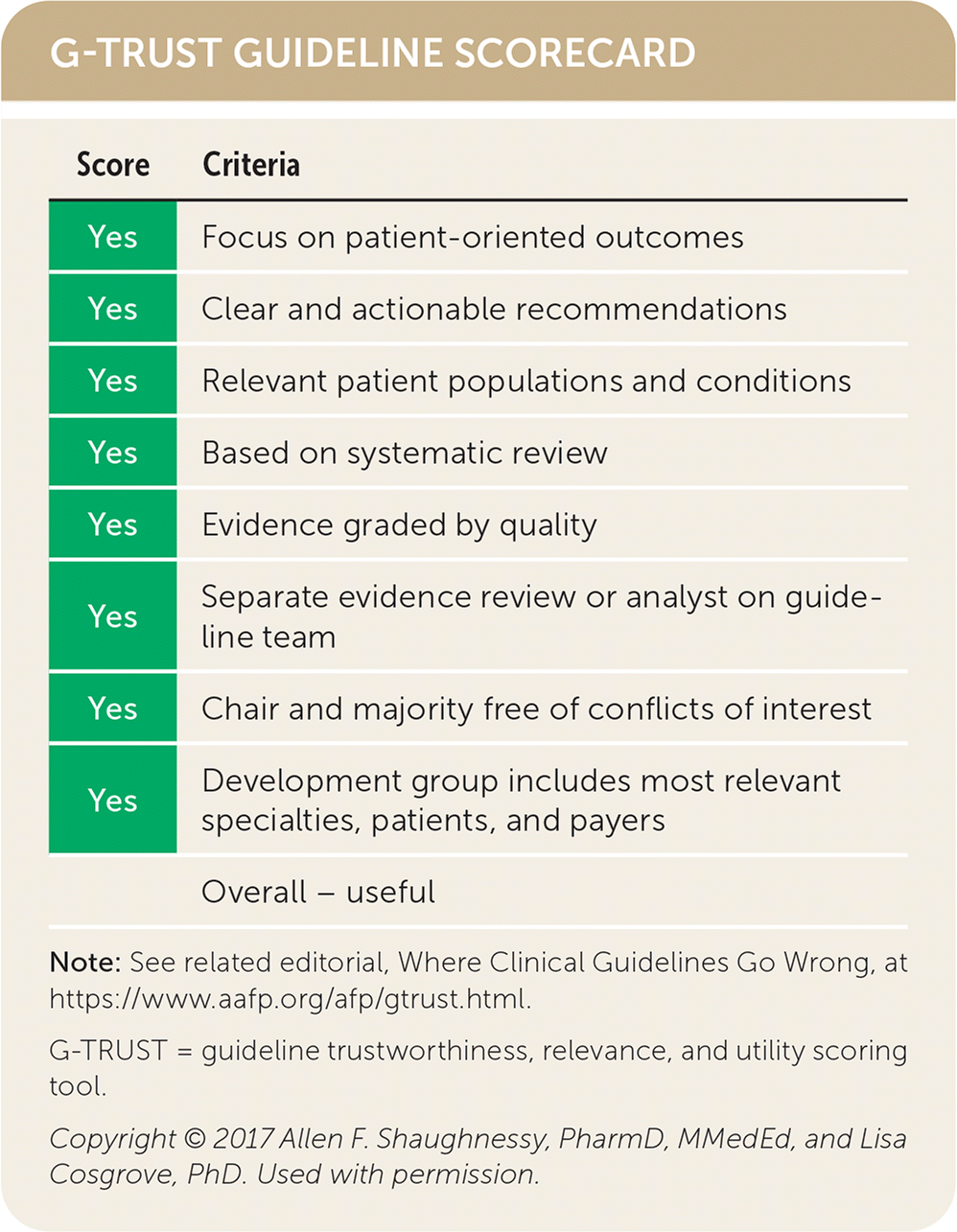
| Score | Criteria |
|---|---|
| Yes | Focus on patient-oriented outcomes |
| Yes | Clear and actionable recommendations |
| Yes | Relevant patient populations and conditions |
| Yes | Based on systematic review |
| Yes | Evidence graded by quality |
| Yes | Separate evidence review or analyst on guideline team |
| Yes | Chair and majority free of conflicts of interest |
| Yes | Development group includes most relevant specialties, patients, and payers |
| Overall – useful |
Note: See related editorial, Where Clinical Guidelines Go Wrong, at https://www.aafp.org/afp/gtrust.html.
G-TRUST = guideline trustworthiness, relevance, and utility scoring tool.
Copyright © 2017 Allen F. Shaughnessy, PharmD, MMedEd, and Lisa Cosgrove, PhD. Used with permission.
The views expressed in this article are those of the authors and do not necessarily reflect the official policy or position of the U.S. Navy, Uniformed Services University of the Health Sciences, U.S. Department of Defense, or the U.S. government.
Editor's Note: The numbers needed to screen and NNH were calculated by the authors based on data provided in the guidelines.
These guidelines echo the current USPSTF recommendations while providing nuance for screening that we as a community are struggling to implement. They highlight the challenge of considering life expectancy and false positives while providing a path for shared decision-making. The call for programs to manage the frequent pulmonary and nonpulmonary abnormalities from screening may be most important for meeting the goal of increasing screening.—Michael J. Arnold, MD, Contributing Editor
Guideline source: American College of Chest Physicians
Published source: Chest. November 2021;160(5):e427–e494

