Key Points for Practice
• Increased physical activity may be particularly beneficial for patients with type 2 diabetes, with combined training including aerobic and resistance exercise leading to greater improvement in A1C level than either modality alone.
• High-intensity interval exercise leads to greater glycemic control in less total exercise time but increases musculoskeletal injury and transient postexercise hyperglycemia in some patients.
• People with type 2 diabetes are prone to volume depletion from hyperglycemia and more susceptible to heat injury with physical activity.
From the AFP Editors
Type 2 diabetes mellitus affects approximately one in 10 people in the United States. Lifestyle interventions, including exercise and physical activity, are often prescribed as part of a treatment plan for people at risk of or diagnosed with type 2 diabetes. The American College of Sports Medicine (ACSM) updated its original statement on physical activity for people with type 2 diabetes. Recommendations include all types of physical activity, encompassing more human movement than just planned exercise.
Impact of Physical Activity on People With Diabetes
Regular aerobic exercise improves glycemia in adults with type 2 diabetes, reducing daily hyperglycemic excursions and lowering A1C levels by at least 0.5%. Resistance training improves muscle mass and insulin sensitivity. Combined aerobic and resistance training provides a greater reduction in A1C level than either modality alone.
High-intensity interval training has gained popularity as a time-efficient exercise modality with significant health benefits. This type of exercise involves aerobic activity done between 65% and 90% of the maximum oxygen concentration or between 75% and 95% of peak heart rate for 10 seconds to four minutes with up to five minutes of active or passive recovery. High-intensity interval exercise reduces postprandial hyperglycemia and provides greater reduction of A1C level per period of activity than other forms of exercise. It also improves continuous glycemia while enhancing insulin sensitivity and pancreatic beta-cell function more than a similar energy expenditure from walking. High-intensity interval exercise has a higher risk of musculoskeletal injury than other exercise modalities. When counseling people with type 2 diabetes about performing chronic intense high-intensity interval exercise, clinicians should consider recommending monitoring for paradoxical transient postexercise hyperglycemia.
Physical activity also reduces symptoms of depression and anxiety. In one exercise study, improvements in mood were maintained for eight years following the intervention.
Physical Activity Recommendations
The physical activity recommendations for all adults are also recommended for people with or at risk of type 2 diabetes. These recommendations include at least 150 minutes per week of moderate-intensity activity or 75 minutes per week of vigorous-intensity aerobic physical activity, and resistance exercise involving all major muscle groups on two or more days per week. Flexibility and balance activities improve function, and activities such as yoga, Tai chi, Pilates, and qigong may also improve glycemic control.
Three minutes of physical activity after every 30 minutes of sedentary activity may improve glycemic control and insulin sensitivity.
Medical evaluation is not needed for people starting low- to moderate-intensity exercise. Exercise stress testing can be considered in adults with type 2 diabetes who are older than 30 years and have been sedentary and now want to participate in moderate- to high-intensity activity. Based on limited research, pre-exercise stress testing has not been proven to reduce cardiac events.
Management of Health Complications With Physical Activity
People taking insulin or insulin secretagogues can have exercise-induced hypoglycemia, especially with longer exercise duration and higher intensity, and pre-exercise dose adjustments or carbohydrate intake can reduce this risk. Conversely, exercise during periods of hyperglycemia increases the risk of volume depletion, which can occur with normoglycemia when taking sodium-glucose cotransporter-2 inhibitors. Adults with type 2 diabetes have reduced ability to thermoregulate because of impaired vasodilation and sweating that can increase the risk of heat injury, although acclimatization to heat does occur over time.
Exercise Timing
Exercise after meals leads to the best glycemic control. Performing high-intensity interval exercise in the afternoon appears more effective than in the morning for glycemic control. Self-paced walking around dinnertime controls glucose better than traditional exercise in the evening.
Dietary Considerations
Although intermittent fasting has become popular, the benefits for people with type 2 diabetes are unknown. The impact of a ketogenic diet, combined with exercise, is not clear.
Diabetes Medications
Overall, more study is needed to understand the impact of medications on the effects of physical activity on glycemia. Despite improving glycemic control with exercise, metformin may blunt exercise-enhanced peripheral insulin sensitivity and may attenuate skeletal muscle hypertrophy after weight lifting. Glucagon-like peptide-1 agonists improve glycemic control with exercise, whereas treatment with insulin appears not to affect glycemic control with exercise.
G-TRUST GUIDELINE SCORECARD
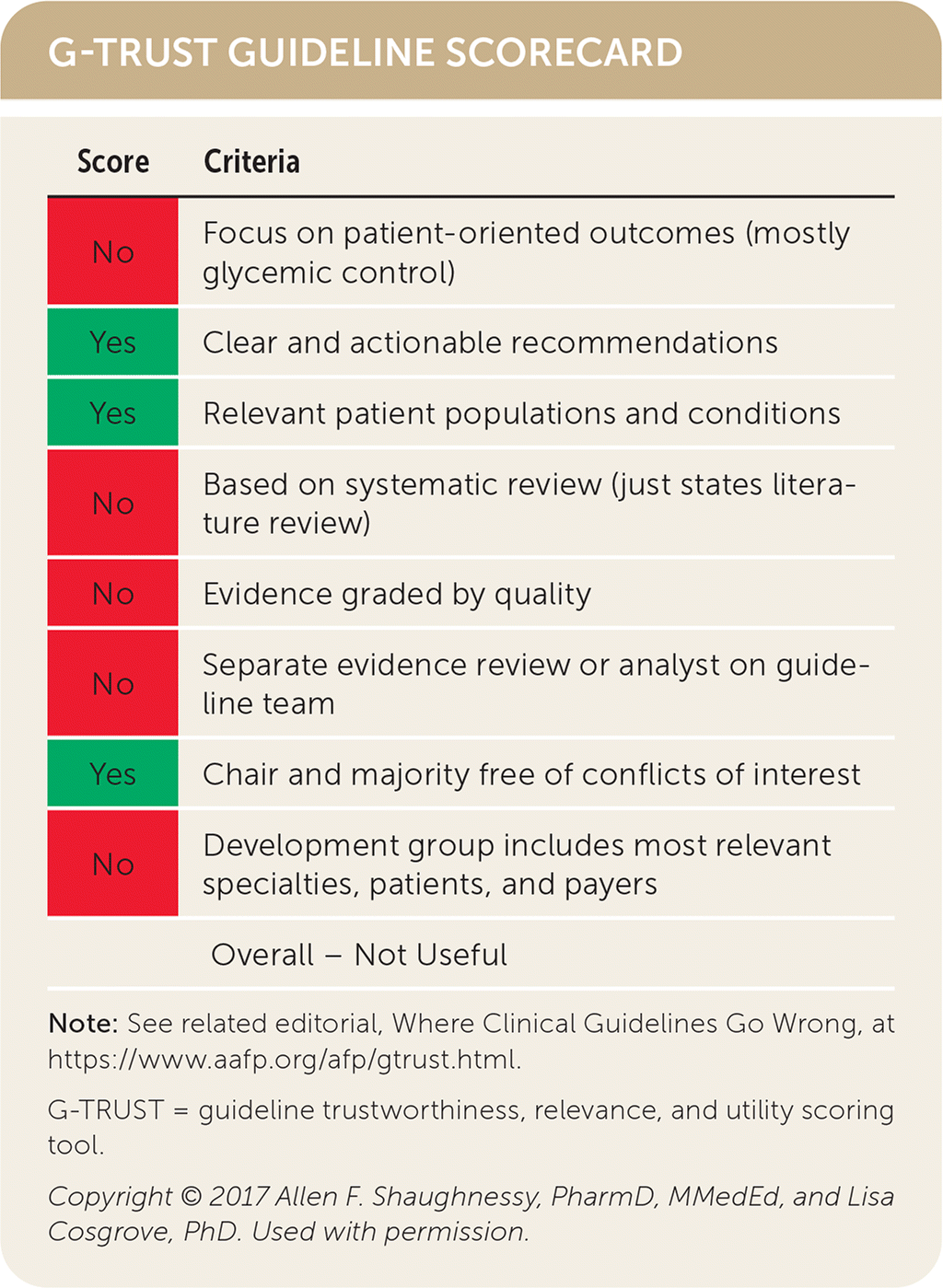
| Score | Criteria |
|---|---|
| No | Focus on patient-oriented outcomes (mostly glycemic control) |
| Yes | Clear and actionable recommendations |
| Yes | Relevant patient populations and conditions |
| No | Based on systematic review (just states literature review) |
| No | Evidence graded by quality |
| No | Separate evidence review or analyst on guideline team |
| Yes | Chair and majority free of conflicts of interest |
| No | Development group includes most relevant specialties, patients, and payers |
| Overall – Not Useful |
Note: See related editorial, Where Clinical Guidelines Go Wrong, at https://www.aafp.org/afp/gtrust.html.
G-TRUST = guideline trustworthiness, relevance, and utility scoring tool.
Copyright © 2017 Allen F. Shaughnessy, PharmD, MMedEd, and Lisa Cosgrove, PhD. Used with permission.
The views expressed in this article are those of the author alone and do not reflect the policy, views, or opinions of Naval Medical Center Camp Lejeune, the U.S. Navy, the U.S. Defense Health Agency, or the U.S. Department of Defense.
Editor's Note: I often struggle to give specific exercise recommendations to my patients with diabetes without nagging or giving them trite exhortations to exercise more. I am disappointed that the research remains limited regarding the role of exercise and how it affects glycemia and prevents long-term harms from type 2 diabetes. These guidelines, based on a consensus statement of sports medicine specialists, do not score well for relevance and validity using the G-TRUST scorecard but do give us some guidance until better information is developed. The evidence for high-intensity interval exercise adds a new option to recommend to busy patients. Although the evidence surrounding risks in patients with poor glycemic control is limited, it provides a foundation on which to tailor recommendations.—Michael J. Arnold, MD, Contributing Editor
Guideline source: American College of Sports Medicine
Published source: Med Sci Sports Exerc. February 1, 2022;54(2):353–368

