Key Points for Practice
• Because no treatments for low back pain are clearly superior, patients should be engaged in shared decision-making about whether to consider nonpharmacologic, pharmacologic, or watchful waiting approaches to managing acute or chronic low back pain.
• Cognitive behavior therapy modestly improves pain and function in chronic low back pain.
• Although medications have limited benefit in low back pain, NSAIDs and duloxetine have the strongest evidence for benefit.
• Acetaminophen does not improve pain or function in low back pain compared with placebo.
From the AFP Editors
Low back pain is one of the most frequently experienced medical conditions, affecting 84% of adults in the United States at some point. Nearly 40% of adults will have experienced this type of pain within a three-month period. Low back pain is the leading cause of disability worldwide. The U.S. Department of Veterans Affairs and U.S. Department of Defense (VA/DoD) have published guidelines on the diagnosis and treatment of low back pain.
Evaluation of Low Back Pain
Because low back pain is common, the initial evaluation focuses on identifying patients with serious underlying conditions. Red flags (Table 1) are the most reliable indicators of serious or progressive neurologic deficits and serious conditions that warrant immediate imaging.
The physical examination has limited use in evaluating back pain. The numerous special tests for nerve root compression, including the straight leg raise, Bragard, Fajersztajn, Sicard, passive neck flexion, and slump tests, have limited accuracy. Similarly, the Mekhail, Patrick, and thigh thrust tests do not reliably identify a sacroiliac source of pain.
TABLE 1. Red Flag Findings in the Evaluation of Low Back Pain
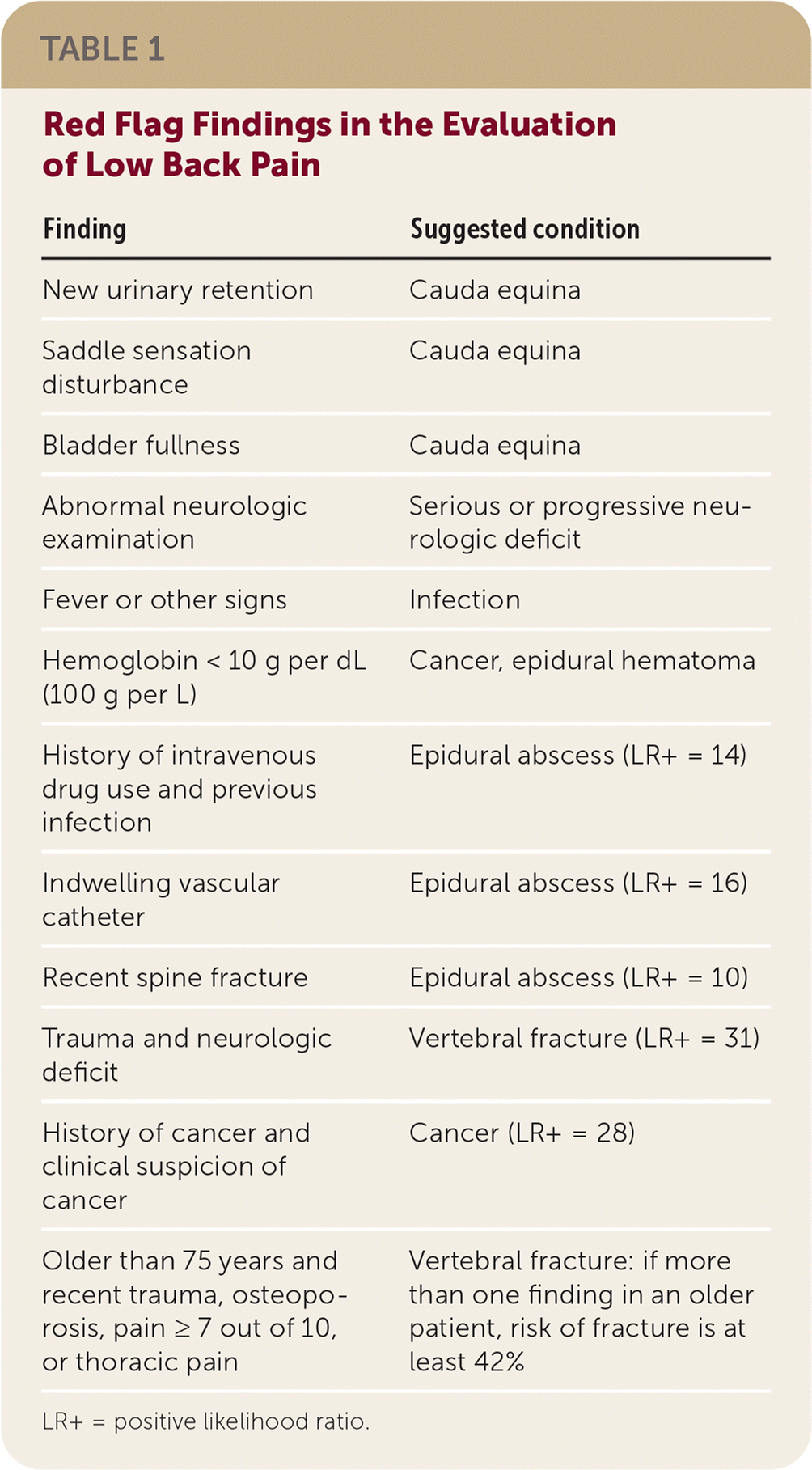
| Finding | Suggested condition |
|---|---|
| New urinary retention | Cauda equina |
| Saddle sensation disturbance | Cauda equina |
| Bladder fullness | Cauda equina |
| Abnormal neurologic examination | Serious or progressive neurologic deficit |
| Fever or other signs | Infection |
| Hemoglobin < 10 g per dL (100 g per L) | Cancer, epidural hematoma |
| History of intravenous drug use and previous infection | Epidural abscess (LR+ = 14) |
| Indwelling vascular catheter | Epidural abscess (LR+ = 16) |
| Recent spine fracture | Epidural abscess (LR+ = 10) |
| Trauma and neurologic deficit | Vertebral fracture (LR+ = 31) |
| History of cancer and clinical suspicion of cancer | Cancer (LR+ = 28) |
| Older than 75 years and recent trauma, osteoporosis, pain ≥ 7 out of 10, or thoracic pain | Vertebral fracture: if more than one finding in an older patient, risk of fracture is at least 42% |
LR+ = positive likelihood ratio.
Unless there are focal neurologic deficits or red flags, imaging does not improve outcomes. Obtaining early magnetic resonance imaging for low back pain increases the probability of surgery by 13 times. Early imaging is also associated with increased opioid use, higher cost of care, higher pain scores, and more work absence.
Approach to Care
Because there is no single treatment that is clearly effective, low back pain care is based on a patient-centered, holistic approach based on comorbidities. Because care is commonly self-directed, success depends on the communication between physician and patient. The limited evidence for many of the common treatments emphasizes the importance of shared decision-making.
Noninvasive Treatments
PSYCHOTHERAPY
Cognitive Behavior Therapy. Cognitive behavior therapy leads to small improvements in pain and functional status in patients with chronic low back pain after four to 12 visits. This type of therapy often uses relaxation, behavioral activation, and exposure to improve quality of life and reduce the functional impact of pain.
Mindfulness-based Stress Reduction. Mindfulness-based stress reduction does not appear as helpful, with similar pain and functional outcomes vs. usual care. Another systematic review of very low-quality evidence suggests mindfulness-based interventions may be as effective as cognitive behavior therapy at reducing pain intensity.
EXERCISE AND MOBILIZATION
Many types of clinician-directed, structured exercise programs improve pain, disability, and function in patients with low back pain. Beneficial exercise programs include aerobic exercise, aquatic exercise, mechanical diagnosis and therapy, mobility, motor control, Pilates, strength training, structured walking programs, and tai chi. Nearly every activity is beneficial.
Yoga and qi gong do not consistently improve outcomes over other types of activity. Yoga does not improve disability, quality of life, or pain more than physical therapy or strength training. The benefits of qi gong are less certain.
Lumbar supports and mechanical traction do not improve pain or function.
COMPLEMENTARY THERAPIES
Although demonstrated to be beneficial in patients with chronic low back pain, there is not enough research to support a recommendation for or against spinal manipulation and mobilization for patients with acute low back pain.
Acupuncture appears to be effective for chronic low back pain, with reduced pain up to one year but no benefit at two years. Acupuncture has not been adequately studied in acute low back pain. Cupping, laser therapy, transcutaneous electrical nerve stimulation, and ultrasound therapy do not improve pain or disability in low back pain.
Medications for Low Back Pain
BENEFICIAL MEDICATIONS
Duloxetine. In patients with chronic low back pain, one additional patient will experience at least a 30% reduction in pain with duloxetine (Cymbalta) compared with patients who receive placebo (number needed to treat = 9; 95% CI, 6 to 16). However, many patients will not find a clinically relevant decrease in pain with treatment. Discontinuation is common with duloxetine because of adverse effects including nausea, insomnia, dry mouth, constipation, and fatigue.
Nonsteroidal Anti-inflammatory Drugs (NSAIDs). In patients with chronic low back pain, treatment with NSAIDs reduces pain by at least 30% compared with placebo, with a number needed to treat of 6 over four to 12 weeks. Studies of NSAIDs used for more than 12 weeks show results that are equivalent to placebo. Adverse events are similar between NSAIDs and placebo for up to 12 weeks.
MEDICATIONS WITH UNCERTAIN EVIDENCE OF BENEFIT
Tricyclic Antidepressants. Tricyclic antidepressants may not be effective for low back pain, because pain and function are similar compared with placebo and the muscle relaxant benztropine at three months or more. Tricyclic antidepressants should be used with caution in patients with cardiovascular risk factors.
Gabapentin and Pregabalin. Very low-quality evidence suggests that pregabalin (Lyrica) leads to a moderate improvement in pain and function in low back pain. Gabapentin does not improve pain or function in low back pain compared with placebo. Gabapentin and pregabalin are associated with significant adverse effects and have the potential for misuse.
Nonbenzodiazepine Muscle Relaxants. The benefits of muscle relaxants in acute low back pain are uncertain. In a small systematic review, skeletal muscle relaxants moderately improved pain and function for the first several days after treatment. Adding cyclobenzaprine to naproxen for acute low back pain does not improve pain or function compared with naproxen alone one week later. Nonbenzodiazepine muscle relaxants are no better than placebo for chronic low back pain.
Systemic Corticosteroids. Use of systemic corticosteroids does not improve pain in acute or chronic low back pain. There may be a slight improvement in disability in acute back pain. In a small study of acute lumbar radiculopathy, a 15-day corticosteroid taper led to a slightly greater improvement in disability than placebo for up to one year.
Topical Medications. Topical preparations for low back pain have not been adequately studied.
Diet and Supplements. No specific diet or supplement has evidence of benefit in low back pain. Vitamin D supplementation does not improve outcomes in low back pain.
MEDICATIONS TO AVOID
Acetaminophen. Acetaminophen is not beneficial in low back pain. A large systematic review comparing acetaminophen with placebo for acute low back pain found no difference in pain, disability, quality of life, or function through 12 weeks. Because of the hepatotoxicity risk and unproven benefit, the VA/DoD recommend against using acetaminophen for back pain.
Opioids. Opioids improve pain and function in chronic low back pain for up to four months, but the long-term risks are high without any proven benefit. A recent study suggests that tramadol may not improve pain or function. Another study suggests that extended-release oxycodone does not improve function.
Benzodiazepines. Avoid benzodiazepines for patients with low back pain. In acute low back pain, adding diazepam to naproxen does not improve pain or function compared with naproxen alone. For chronic low back pain, a systematic review did not find a benefit of diazepam over placebo.
Nonsurgical Treatments
Few interventional procedures are beneficial for low back pain. Radiofrequency ablation of the lumbar medial branch or sacral lateral branch nerves improves pain for up to 36 months without clinically improving disability or quality of life. Epidural corticosteroid injections improve pain by an average of 0.75 points on a 10-point scale, which may not be clinically relevant, but they do not improve function. Intra-articular facet joint corticosteroid injections are not beneficial compared with placebo injections. The benefit of sacroiliac joint injections is uncertain. Spinal cord stimulation does not meaningfully improve back pain, leg pain, or health-related quality of life.
Orthobiologics, including platelet-rich plasma and stem cells, have limited evidence of benefit. Platelet-rich plasma injections may slightly improve pain based on a study of fewer than 100 patients.
G-TRUST GUIDELINE SCORECARD
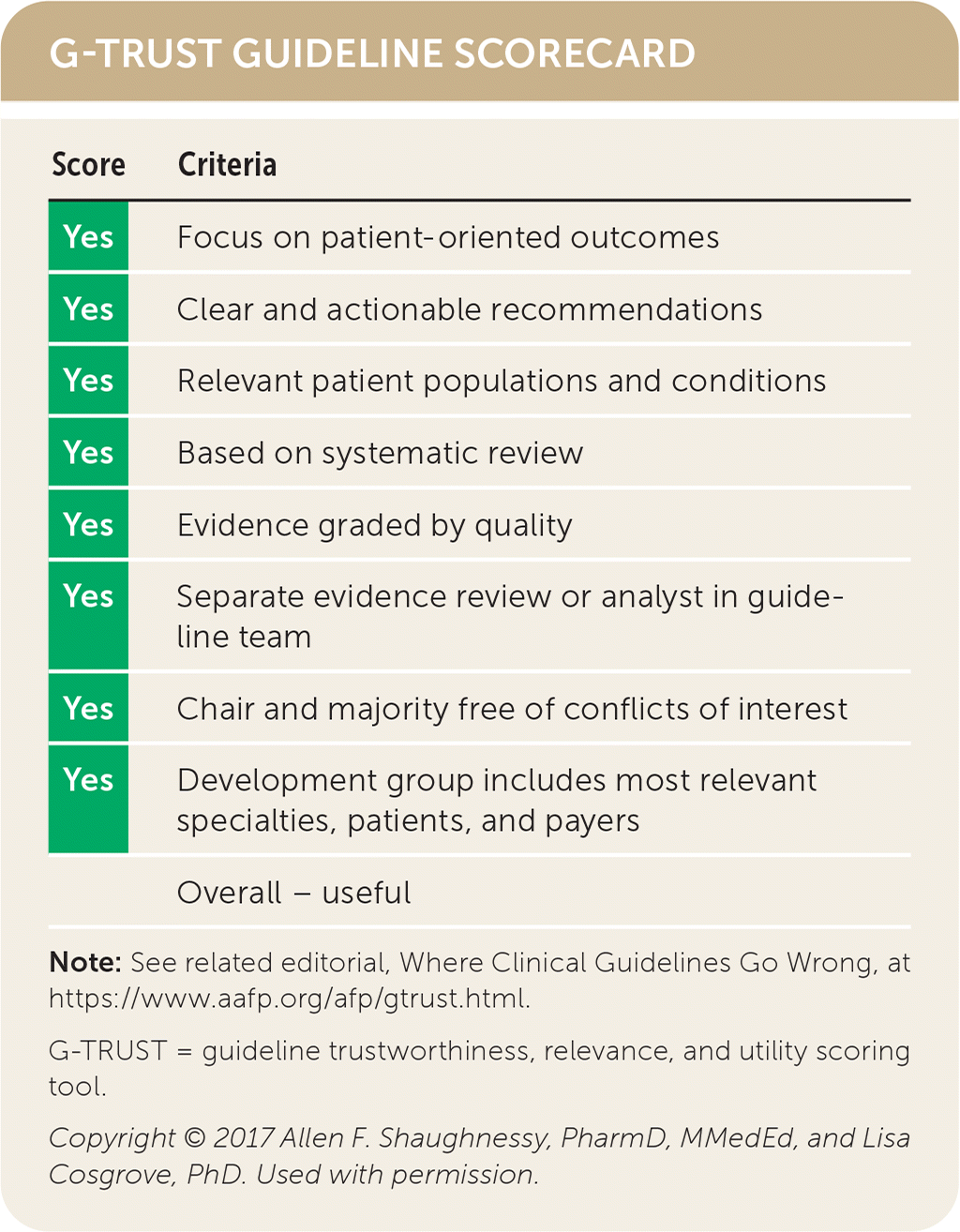
| Score | Criteria |
|---|---|
| Yes | Focus on patient-oriented outcomes |
| Yes | Clear and actionable recommendations |
| Yes | Relevant patient populations and conditions |
| Yes | Based on systematic review |
| Yes | Evidence graded by quality |
| Yes | Separate evidence review or analyst in guideline team |
| Yes | Chair and majority free of conflicts of interest |
| Yes | Development group includes most relevant specialties, patients, and payers |
| Overall – useful |
Note: See related editorial, Where Clinical Guidelines Go Wrong, at https://www.aafp.org/afp/gtrust.html.
G-TRUST = guideline trustworthiness, relevance, and utility scoring tool.
Copyright © 2017 Allen F. Shaughnessy, PharmD, MMedEd, and Lisa Cosgrove, PhD. Used with permission.
Editor's Note: The numbers needed to treat reported in this Practice Guideline were calculated by the author based on raw data provided in the original guideline.
Despite the ubiquity of low back pain in clinical practice, there are few recent guidelines that review treatment, and none are as extensive as this guideline. Unfortunately, the primary message is that no medication or intervention is very effective. Yet, this frees us to allow our patients to choose from the most effective options that suit their needs best.— Michael J. Arnold, MD, Contributing Editor
The views expressed are those of the authors and do not necessarily reflect the official policy or position of the U.S. Department of the Navy, U.S. Department of the Air Force, U.S. Department of the Army, Uniformed Services University of the Health Sciences, U.S. Department of Defense, U.S. Department of Veterans Affairs, or the U.S. government.
Guideline source: U.S. Department of Veterans Affairs and U.S. Department of Defense
Available at: https://www.healthquality.va.gov/guidelines/Pain/lbp/

