This article summarizes the top 20 research studies of 2022 identified as POEMs (patient-oriented evidence that matters), excluding COVID-19. Statins for primary prevention of cardiovascular disease produce only a small absolute reduction in a person's likelihood of dying (0.6%), having a myocardial infarction (0.7%), or having a stroke (0.3%) over three to six years. Supplemental vitamin D does not reduce the risk of a fragility fracture, even in people with low baseline vitamin D levels or a previous fracture. Selective serotonin reuptake inhibitors are preferred medical therapy for panic disorder, and patients who discontinue antidepressants are more likely to relapse (number needed to harm = 6) compared with those who continue. Combination therapy using a selective serotonin reuptake inhibitor, serotonin-norepinephrine reuptake inhibitor, or tricyclic antidepressant with mirtazapine or trazodone is more effective than monotherapy for first-line treatment of acute severe depression and when monotherapy fails. Using hypnotic agents for insomnia in adults comes with a significant trade-off between effectiveness and tolerability. In patients with moderate to severe asthma, using a combination of albuterol and glucocorticoid inhalers as rescue therapy reduces exacerbations and need for systemic steroids. Observational research shows an increased risk of gastric cancer in patients taking proton pump inhibitors (number needed to harm = 1,191 over 10 years). The American College of Gastroenterology updated its guideline for gastroesophageal reflux disease, and a new guideline provides sound advice for the evaluation and management of irritable bowel syndrome. Adults older than 60 years with prediabetes are more likely to become normoglycemic than to develop diabetes mellitus or die. Treatment of prediabetes via intensive lifestyle intervention or metformin has no impact on long-term cardiovascular outcomes. Persons with painful diabetic peripheral neuropathy have similar degrees of improvement with monotherapy using amitriptyline, duloxetine, or pregabalin and greater improvement with combination therapy. When communicating with patients about disease risk, most patients prefer numbers over words because people overestimate word-based probabilities. In terms of drug therapy, the duration of an initial varenicline prescription should be 12 weeks. Many drugs can interact with cannabidiol. No important difference was found among ibuprofen, ketorolac, and diclofenac for treatment of acute nonradicular low back pain in adults.
For the past 24 years, a team of six clinicians has systematically reviewed more than 100 medical journals to find the research most likely to change and improve primary care practice. The team includes experts in family medicine, pharmacology, hospital medicine, and women's health.1,2
The goal of this process is to identify POEMs (patient-oriented evidence that matters). A POEM must report at least one patient-oriented outcome, such as improvement in symptoms, morbidity, or mortality. It should also be free of important methodologic bias, making the results valid and trustworthy. Finally, if applied in practice, the results would change what some physicians do by adopting a new practice or discontinuing an old one shown to be ineffective or harmful. Of more than 20,000 research studies published in 2022 in the journals reviewed by the POEMs team, 253 met criteria for validity, relevance, and practice change. These POEMs are emailed daily to subscribers of Essential Evidence Plus (Wiley-Blackwell, Inc.).
The Canadian Medical Association purchases a POEMs subscription, and thousands of its members receive the daily POEM. These physicians can rate each one using a validated questionnaire.3 This process is called the Information Assessment Method (https://www.mcgill.ca/iam). POEM ratings address the domains of clinical relevance, cognitive impact, use in practice, and expected health benefits. In 2022, each of the 253 daily POEMs were rated by an average of 1,087 physicians. New for 2022, readers of the daily POEM saw an “overuse alert” for POEMs that align with a Choosing Wisely recommendation.4
In this article, the 12th installment of our annual series (https://www.aafp.org/pubs/afp/content/top-poems.html), we summarize the 20 most clinically relevant POEMs of 2022 as determined by Canadian Medical Association members. Although some of the most highly rated POEMs addressed COVID-19, rapid changes in management as the pandemic has evolved make many of them less relevant in 2023. Therefore, we briefly summarize these COVID-19 POEMs, as well as highly rated practice guidelines, separately. The full POEMs discussed in this review are available at https://www.aafp.org/pubs/afp/content/top-poems/2022.html.
Preventive Health Care
The first two POEMs relate to preventive medicine (Table 1).5,6 Many patients take statins to reduce cardiovascular events. But how large is the benefit? A meta-analysis identified 19 studies that randomized 132,763 patients to statin therapy or placebo.5 Studies were typically three to six years in duration, and statins reduced the risk of overall death by 0.8%, myocardial infarction by 1.3%, and stroke by 0.4%. When statins were used as primary prevention, the reductions were smaller: 0.6% fewer deaths, 0.7% fewer myocardial infarctions, and 0.3% fewer strokes, for an overall number needed to treat of 63 to prevent one event over three to six years. The 95% CI around all-cause mortality alone was 88 to 250 over several years of treatment as primary prevention. Not bad, but this is probably a higher number needed to treat than most of our patients believe.
TABLE 1. Preventive Health Care

| Clinical question | Bottom-line answer |
|---|---|
| 1. What is the impact of LDL cholesterol reduction on the individual risks of overall mortality, myocardial infarction, and stroke?5 | Statins for primary prevention produce modest benefit. Reducing LDL cholesterol levels with statins provides only a small absolute reduction in the person's overall likelihood of dying (0.8% reduction), having a myocardial infarction (1.3%), or having a stroke (0.4%) over three to six years. Too often we are given relative risk reductions or a bundling together of these outcomes with other lesser outcomes, which leads to an inflated sense of importance attributed to cholesterol treatment. In addition, the authors also found a small and inconsistent relationship between more intensive lowering of LDL cholesterol and these outcomes, which is contrary to what many (U.S.) guidelines would have us believe. |
| 2. Does supplemental vitamin D reduce the risk of fracture in older adults?6 | Vitamin D supplementation does not reduce fracture risk. Vitamin D level is a very good marker of ill health, but a terrible treatment target. This large study showed definitively that supplemental vitamin D does not reduce the risk of fracture, even in people with low baseline vitamin D levels or a previous fracture. |
LDL = low-density lipoprotein.
Screening for low vitamin D levels and recommending replacement in those who are deficient have become popular, although the U.S. Preventive Services Task Force (USPSTF) found insufficient evidence to recommend screening in asymptomatic individuals.7 A trial randomized 25,871 men 50 years or older and women 55 years or older to receive 2,000 IU of vitamin D or placebo daily for a median of five years.6 There was no difference between groups in any type of fracture, even in patients with low baseline vitamin D levels (hazard ratio = 1.04; 95% CI, 0.80 to 1.36) or a previous fracture.
Behavioral Health
The first POEM in this group provides insight into what happens when a patient discontinues an antidepressant8 (Table 28–13 ). The study included primary care patients with at least two episodes of depression who had been taking an antidepressant for at least two years.8 Patients were randomized to continue the medication or taper it over two months to placebo. After one year, the likelihood of relapse was significantly higher in the discontinuation group (56% vs. 39%; hazard ratio = 2.1; 95% CI, 1.6 to 2.7). Symptoms in the discontinuation group were also more severe.
TABLE 2. Behavioral Health
| Clinical question | Bottom-line answer |
|---|---|
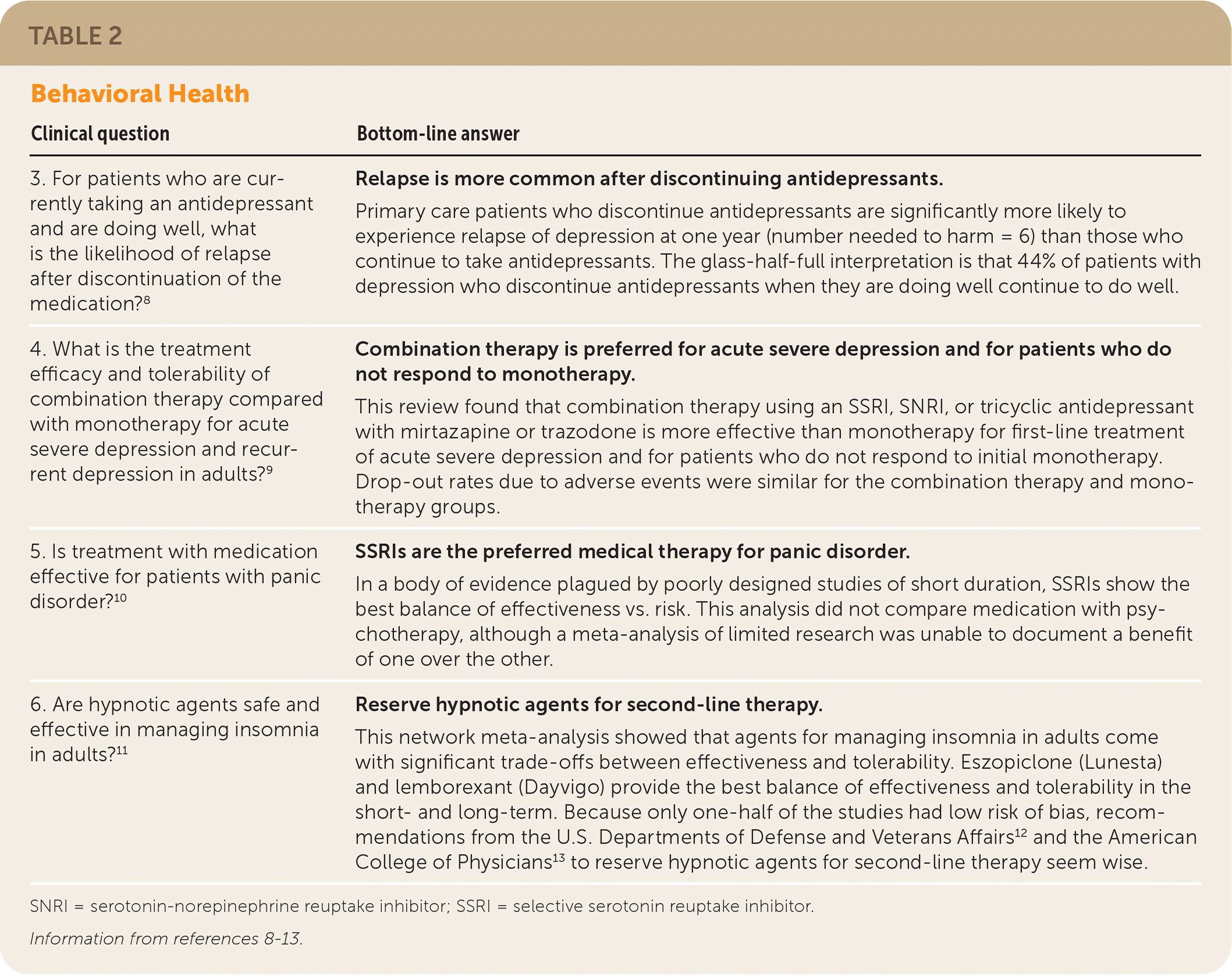
| 3. For patients who are currently taking an antidepressant and are doing well, what is the likelihood of relapse after discontinuation of the medication?8 | Relapse is more common after discontinuing antidepressants. Primary care patients who discontinue antidepressants are significantly more likely to experience relapse of depression at one year (number needed to harm = 6) than those who continue to take antidepressants. The glass-half-full interpretation is that 44% of patients with depression who discontinue antidepressants when they are doing well continue to do well. |
| 4. What is the treatment efficacy and tolerability of combination therapy compared with monotherapy for acute severe depression and recurrent depression in adults?9 | Combination therapy is preferred for acute severe depression and for patients who do not respond to monotherapy. This review found that combination therapy using an SSRI, SNRI, or tricyclic antidepressant with mirtazapine or trazodone is more effective than monotherapy for first-line treatment of acute severe depression and for patients who do not respond to initial monotherapy. Drop-out rates due to adverse events were similar for the combination therapy and monotherapy groups. |
| 5. Is treatment with medication effective for patients with panic disorder?10 | SSRIs are the preferred medical therapy for panic disorder. In a body of evidence plagued by poorly designed studies of short duration, SSRIs show the best balance of effectiveness vs. risk. This analysis did not compare medication with psychotherapy, although a meta-analysis of limited research was unable to document a benefit of one over the other. |
| 6. Are hypnotic agents safe and effective in managing insomnia in adults?11 | Reserve hypnotic agents for second-line therapy. This network meta-analysis showed that agents for managing insomnia in adults come with significant trade-offs between effectiveness and tolerability. Eszopiclone (Lunesta) and lemborexant (Dayvigo) provide the best balance of effectiveness and tolerability in the short- and long-term. Because only one-half of the studies had low risk of bias, recommendations from the U.S. Departments of Defense and Veterans Affairs12 and the American College of Physicians13 to reserve hypnotic agents for second-line therapy seem wise. |
SNRI = serotonin-norepinephrine reuptake inhibitor; SSRI = selective serotonin reuptake inhibitor.
The next study looked at the best way to treat these patients with acute severe depression. It showed that combination therapy is better than monotherapy for first-line treatment and in patients who do not respond to initial monotherapy (standardized mean difference [SMD] = 0.31; 95% CI, 0.19 to 0.44).9 An SMD of 0.31 is consistent with a small effect size. The combination of a monoamine reuptake inhibitor (selective serotonin reuptake inhibitor [SSRI], serotonin-norepinephrine reuptake inhibitor, or tricyclic antidepressant) with mirtazapine or trazodone is more effective than monotherapy for first-line treatment and for patients who do not respond to monotherapy.
Turning to anxiety disorders, a network meta-analysis of 87 randomized controlled trials with 12,800 participants evaluated 12 drug classes to treat panic disorder.10 Only one trial was at low risk of bias, and most trials were no more than three months in duration. The meta-analysis found that the most effective drugs were benzodiazepines, tricyclic antidepressants, and SSRIs, with SSRIs having the least risk of adverse effects. Sertraline and escitalopram have the best balance of high remission rates and low risk of adverse events. But remember, other studies have found that cognitive behavior therapy and mindfulness-based therapies are likely to be as effective as medications.14,15
Finally, a network meta-analysis identified 154 double-blind randomized controlled trials that compared a broad range of hypnotic agents with each other and placebo for the treatment of insomnia.11 There were 20 individual drugs and drug classes, including benzodiazepines, melatonin, trazodone, and newer short-acting hypnotics such as eszopiclone (Lunesta) and lemborexant (Dayvigo). The drugs most likely to be effective were eszopiclone and lemborexant in the long-term and eszopiclone, lemborexant, benzodiazepines, seltorexant (undergoing clinical trials in the United States), trazodone, trimipramine, zopiclone (not available in the United States), and zolpidem in the short-term. However, all drugs had relatively high rates of adverse effects (although so did placebo). The authors concluded that eszopiclone and lemborexant provide the best balance of effectiveness and tolerability in the short- and long-term.
Asthma
One POEM reported on a study of 3,132 children and adults with moderate to severe asthma who were taking long-term inhaled corticosteroids and had experienced a severe asthma exacerbation in the previous year16 (Table 316,17 ). They were randomized to two puffs each of albuterol, 90 mcg, plus budesonide, 80 mcg; albuterol, 90 mcg, plus budesonide, or albuterol alone as a rescue inhaler. In the higher-dose budesonide group, there was about 1 fewer exacerbation per 7 patients treated for one year compared with the albuterol only group, and patients also took significantly fewer systemic steroids (84 mg vs. 130 mg per year).
TABLE 3. Asthma
| Clinical question | Bottom-line answer |
|---|---|
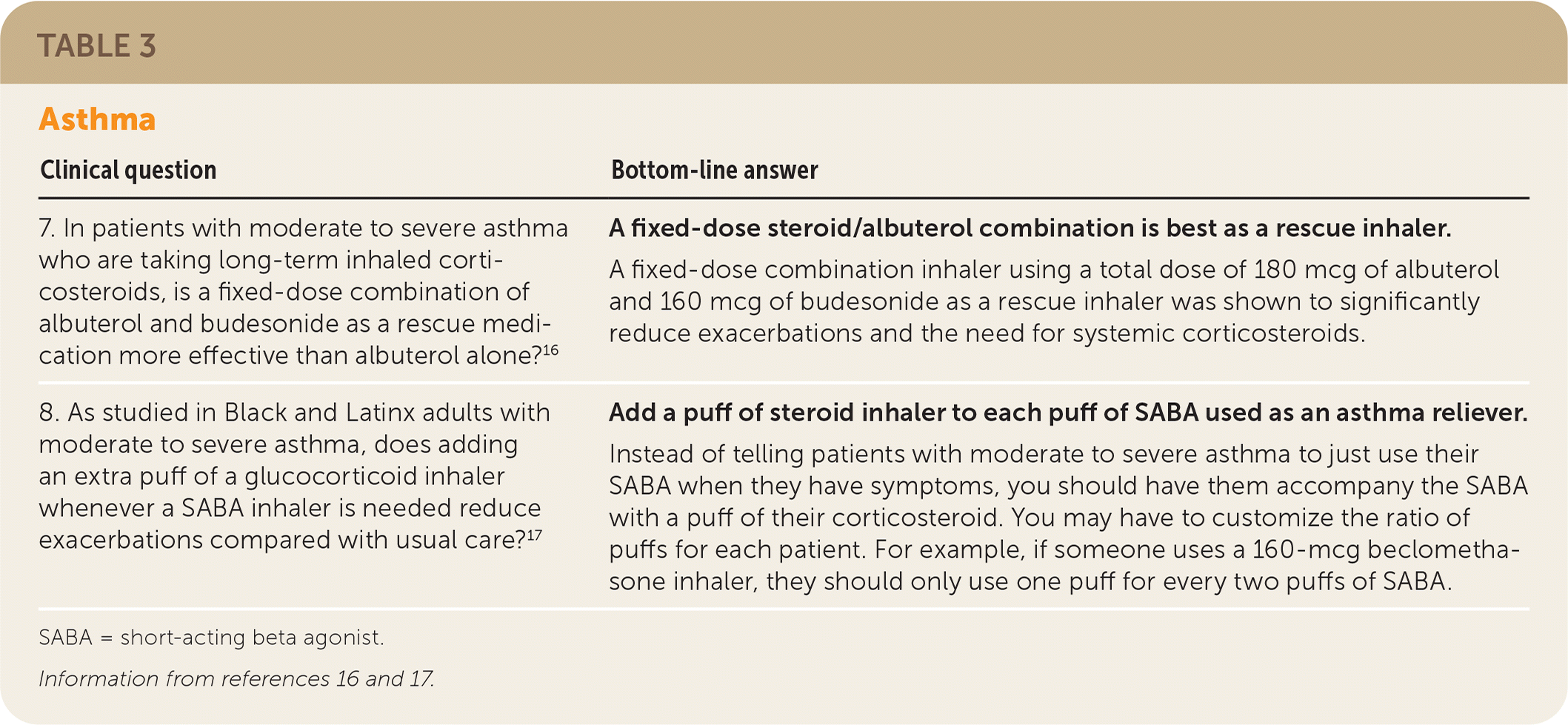
| 7. In patients with moderate to severe asthma who are taking long-term inhaled corticosteroids, is a fixed-dose combination of albuterol and budesonide as a rescue medication more effective than albuterol alone?16 | A fixed-dose steroid/albuterol combination is best as a rescue inhaler. A fixed-dose combination inhaler using a total dose of 180 mcg of albuterol and 160 mcg of budesonide as a rescue inhaler was shown to significantly reduce exacerbations and the need for systemic corticosteroids. |
| 8. As studied in Black and Latinx adults with moderate to severe asthma, does adding an extra puff of a glucocorticoid inhaler whenever a SABA inhaler is needed reduce exacerbations compared with usual care?17 | Add a puff of steroid inhaler to each puff of SABA used as an asthma reliever. Instead of telling patients with moderate to severe asthma to just use their SABA when they have symptoms, you should have them accompany the SABA with a puff of their corticosteroid. You may have to customize the ratio of puffs for each patient. For example, if someone uses a 160-mcg beclomethasone inhaler, they should only use one puff for every two puffs of SABA. |
SABA = short-acting beta agonist.
The second POEM in this group adds to the same evidence base as the first but in a more diverse population. Asthma disproportionately affects Black and Latinx patients, yet these groups have been underrepresented in research. This study randomized 1,201 self-identified Black and Latinx adults with moderate to severe asthma to a short-acting beta agonist (SABA) inhaler alone as reliever therapy or to a SABA plus a puff of a beclomethasone, 80 mcg, inhaler for every puff of the SABA.17 There was approximately 1 fewer asthma exacerbation for every 8 patients in the combined therapy group compared with SABA alone over one year. Asthma control scores also improved, but the change was not clinically significant. Minority representation in studies is critical to addressing health disparities.18
Gastroenterology
The first of three POEMs on gastroenterology topics (Table 419–22 ) summarized an observational study of the following question: Is there an association between gastric cancer and the use of proton pump inhibitors (PPIs)? Answer: Patients taking PPIs have a small increased risk of gastric cancer (number needed to harm = 1,191 over 10 years).19 But, remember, association is not causation. That said, physicians initiating antacid therapy should begin with a histamine H2 blocker. If physicians are prescribing a PPI, the lowest dose and duration possible should be used. Choosing Wisely Canada provides a toolkit for helping to deprescribe PPIs (available at https://choosingwiselycanada.org/toolkit/bye-bye-ppi).
TABLE 4. Gastroenterology

| Clinical question | Bottom-line answer |
|---|---|
| 9. Is there an association between gastric cancer and the use of PPIs?19 | PPIs are associated with a small increased risk of gastric cancer. This is the strongest evidence to date that there is a small but clinically significant increase in the risk of gastric cancer for patients taking a PPI (number needed to harm = 1,191 over 10 years). Antacid therapy should begin with a histamine H2 blocker. If a PPI is prescribed, the lowest dose and duration possible should be used. Another recent study using data from a Korean registry produced similar findings.20 |
| 10. How should clinicians evaluate and manage patients with suspected gastroesophageal reflux disease?21 | Diagnosis and management of gastroesophageal reflux disease The American College of Gastroenterology has updated its guideline for the diagnosis and management of gastroesophageal reflux disease. The guideline includes several tables and algorithms that may be useful to primary care clinicians. In patients who are treatment naive and have classic symptoms and no alarm symptoms, clinicians should attempt to discontinue PPIs after a successful eight-week trial. |
| 11. What is the best way to manage IBS?22 | Diagnosis and management of IBS This high-quality, evidence-based guideline from the British Society of Gastroenterology provides sound advice for the evaluation and management of IBS in primary care. Colonoscopy is recommended only for patients with alarm signs and symptoms or those at risk of microscopic colitis. First-line therapy includes exercise and gradually increasing doses of soluble fiber (e.g., psyllium). |
IBS = irritable bowel syndrome; PPI = proton pump inhibitor.
How should clinicians evaluate and manage patients with suspected gastroesophageal reflux disease? The American College of Gastroenterology guideline panel recognizes that some patients require long-term PPI therapy, and the benefits outweigh the theoretical risks in these patients. In patients who are treatment naive and have classic symptoms and no alarm symptoms, clinicians should attempt to discontinue PPIs after a successful eight-week trial. Therefore, initial prescriptions should generally be limited to a duration of eight weeks.21
Informed by systematic reviews, the British Society of Gastroenterology published updated recommendations for the diagnosis of irritable bowel syndrome (defined as at least six months of abdominal pain or discomfort and altered bowel habits).22 Colonoscopy is recommended only for patients with alarm signs and symptoms or those at risk of microscopic colitis. First-line therapy includes exercise and gradually increasing doses of soluble fiber (e.g., psyllium). Recommendations for other first- and second-line treatments are summarized in the POEM.
Prediabetes/Diabetes Mellitus
The natural history of prediabetes in adults older than 60 years is the topic of the first POEM in this category (Table 523–26 ). This English study included more than 2,000 adults without diabetes mellitus at baseline.23 The average age of participants was 70.6 years, and 55% were women. Over eight years of follow-up, older people with prediabetes were more likely to become normoglycemic than to develop diabetes or die. Perhaps it is time to retire the term “prediabetes” when talking with older people.
TABLE 5. Prediabetes/Diabetes Mellitus

| Clinical question | Bottom-line answer |
|---|---|
| 12. What is the natural history of prediabetes in adults older than 60 years?23 | Most older adults with prediabetes never develop diabetes. In this cohort study, older people with prediabetes were more likely to become normoglycemic than to develop diabetes or die. |
| 13. What is the long-term impact of treating prediabetes on mortality and cardiovascular outcomes?24 | Treatment of prediabetes does not impact long-term outcomes. In patients with prediabetes, neither an intensive lifestyle intervention nor metformin has any impact on the long-term risk of cardiovascular outcomes. |
| 14. How frequent is hypoglycemia among older institutionalized adults with type 2 diabetes?25 | Drug-induced hypoglycemia is common in frail older adults living in nursing homes. In this small study, more than 75% of older adults with type 2 diabetes who were living in nursing homes had at least one hypoglycemic event during two weeks of monitoring, and nearly 50% experienced severe hypoglycemia. A lower A1C level was associated with more frequent events and a longer time spent in a hypoglycemic state. |
| 15. Are amitriptyline, duloxetine (Cymbalta), and pregabalin (Lyrica) effective in decreasing pain in adults with diabetic peripheral neuropathy?26 | Combination therapy is better than monotherapy for diabetic neuropathy pain. In this study, adults with painful diabetic peripheral neuropathy had similar degrees of improvement with monotherapy using amitriptyline, duloxetine, or pregabalin. However, there was greater improvement with subsequent combination therapy, regardless of initial medication choice. |
The next POEM reports on the long-term cardiovascular outcomes for participants in the original Diabetes Prevention Program trial.24 In this trial, participants were randomized to receive metformin, 850 mg twice daily; an intensive exercise program; or placebo, and were then followed for three years. At the conclusion of the study, all patients were invited to participate in a long-term open-label follow-up study, and 86% agreed. The bottom line: In patients with prediabetes, neither an intensive lifestyle intervention nor metformin had an impact on the long-term risk of cardiovascular outcomes.
In the nursing home setting, a cohort of 42 older adults with type 2 diabetes were evaluated for the frequency and persistence of hypoglycemia. All participants were taking medications capable of inducing hypoglycemia (e.g., sulfonylureas, repaglinide, insulin). The study showed that seven people (17%) spent more than 20% of an entire day in a hypoglycemic state. Severe hypoglycemia occurred in 19 people (45%). A lower A1C level was associated with more frequent events and a longer time spent in a hypoglycemic state.25 We should allow A1C results to be higher in frail older patients.
The last POEM in this group summarized the findings of a crossover trial that compared three drugs for decreasing pain in adults with diabetic peripheral neuropathy.26 Similar degrees of improvement were reported with monotherapy using amitriptyline, duloxetine (Cymbalta), or pregabalin (Lyrica). Greater improvement was reported with subsequent combination therapy, regardless of initial choice of medication. This POEM included a table summarizing the adverse effects associated with three combinations of these drugs. Dizziness was more common with duloxetine plus pregabalin, nausea with pregabalin plus amitriptyline, and dry mouth with amitriptyline plus pregabalin.
Miscellaneous
Five top POEMs do not fall easily into a single category (Table 627–31 ). With regard to health information, understanding should clearly precede decision-making. However, when we say “rare” or “high risk,” what are we implying, and what do these terms mean to patients? A systematic review of 33 studies found significant variability in the presentation of probabilities and their subsequent interpretation by patients. This POEM also showed that most patients prefer numbers rather than word-based estimates of risk.27
TABLE 6. Miscellaneous

| Clinical question | Bottom-line answer |
|---|---|
| 16. How do patients interpret word-based and number-based probability estimates, and how do they prefer to receive estimates of risk?27 | When physicians are communicating risk, most patients prefer numbers over words. In general, people grossly overestimate probabilities conveyed by the words we use. People translate “rare” as 10%, on average, which is about 100-fold higher than its typical intended meaning when used for medication risk labeling. The interpretation of “common” (an average of 59%) is closer to “almost always” than the accepted definition of 1% to 10%. Patients may prefer hearing the actual numbers if you can provide them. |
| 17. Is there any benefit to extending varenicline (Chantix) therapy beyond 12 weeks or combining varenicline with nicotine replacement therapy for increasing smoking cessation?28 | Use 12 weeks of varenicline therapy for smoking cessation. This study found no additional benefit with varenicline treatment for 24 weeks vs. 12 weeks for increasing smoking cessation rates. There was also no additional benefit with varenicline plus nicotine replacement therapy vs. varenicline monotherapy. Results were not affected by patient sex, race, treatment site, or level of tobacco dependence. |
| 18. What common medications have serious interactions with CBD?29 | Many drugs can interact with CBD. The nonintoxicating phytocannabinoid CBD is widely available and may interact with other medications. Although interactions have been documented, their likelihood and impact have not been adequately described. Consider asking patients about their CBD use before prescribing another psychoactive medicine, and ask if they have experienced any unexpected adverse effects with other medications. |
| 19. How do ibuprofen, ketorolac, and diclofenac compare for the treatment of acute nonradicular low back pain in adults?30 | Nonsteroidal anti-inflammatory drugs have a class effect for analgesia in patients with acute low back pain. This study found no differences among ibuprofen, ketorolac, and diclofenac in the primary outcome of overall clinical improvement at five days in adults presenting to the emergency department with acute nonradicular low back pain. Some of the secondary outcomes favored ketorolac, however, leaving open the possibility that ketorolac is superior. |
| 20. What is the best topical treatment for patients with mild to moderate acne vulgaris?31 | Best options for first-line treatment of acne vulgaris For patients with mild to moderate acne, this network meta-analysis suggests starting with adapalene/benzoyl peroxide, clindamycin/benzoyl peroxide, or adapalene alone. Patients who do not tolerate either benzoyl peroxide combination are likely to better tolerate adapalene alone. |
CBD = cannabidiol.
The next POEM was a randomized trial evaluating whether extending varenicline (Chantix) treatment beyond 12 weeks is beneficial for increasing the likelihood of smoking cessation. At 52 weeks of follow-up, there was no difference in quit rates between those taking varenicline for 12 weeks vs. 24 weeks.28 Also, combining varenicline with nicotine replacement therapy produced no additional benefit. Therefore, initial varenicline prescriptions should specify a duration of 12 weeks. Using varenicline for longer than 12 weeks may be appropriate for a select group of patients who want a longer treatment course.32
Drug interactions between cannabidiol (CBD) and commonly used medications is the topic of the next POEM. This study showed that CBD may increase serum levels of SSRIs, tricyclic antidepressants, antipsychotics, beta blockers, and opioids.29 CBD increases levels of lamotrigine, but other anti-convulsants decrease levels of CBD. Although this reminds us of the potential for drug-drug interactions with CBD, we also need to know more about the severity of these interactions for better clinical decision-making.
The next POEM addresses the treatment of acute nonradicular low back pain. A randomized controlled trial of 198 adults 18 to 65 years of age presenting to the emergency department found no difference among ibuprofen, ketorolac, and diclofenac for the outcome of clinical improvement at five days.30 Thus, although some nonsteroidal anti-inflammatory drugs may have a reputation of being a better analgesic, there seems to be a class effect with these drugs.
Our final top POEM identified the best topical therapy for mild to moderate acne vulgaris. The authors of this network meta-analysis of randomized controlled trials began by asking patients what was most important to them in terms of the outcome of acne treatment. Thus, the primary outcomes of this study were effectiveness, the proportion of patients who reported at least moderate improvement, tolerability, and the proportion who withdrew from the study or stopped using the medication due to adverse events. The bottom line: For a condition such as acne that has many treatment choices, good options include adapalene/benzoyl peroxide (Epiduo), followed by clindamycin/benzoyl peroxide and then adapalene alone.31
COVID-19 and Practice Guidelines
As noted earlier, studies of COVID-19 vaccines were among the most highly rated for relevance. The uniform message across these studies was that vaccines and boosters are highly effective, especially at preventing hospitalizations and in older patients.33–37 They are also very safe. Although there is a small increase in the risk of myocarditis, especially in younger men (about 2 to 6 cases per 100,000 vaccinated men 18 to 39 years of age), the risk of myocarditis and other complications associated with COVID-19 infection and the lower risk of cardiac arrest or death in vaccinated people support the importance of vaccination.38
Several guidelines were also highly rated. The USPSTF no longer recommends initiating aspirin therapy for primary prevention in patients 60 years or older based on newer studies showing no net benefit. The USPSTF continues to recommend statins for adults 40 to 75 years of age who have one or more cardiovascular risk factors and an estimated 10-year cardiovascular event risk of at least 10%, with shared decision-making for those with a 10-year event risk of 7.5% to 9.9%.39
The National Institute for Health and Care Excellence updated guidelines for two important conditions. Although metformin remains the cornerstone of oral drug therapy for type 2 diabetes, increased use of sodium-glucose cotrans-porter-2 inhibitors is encouraged, especially for patients with chronic heart or renal disease.40 The updated guideline includes a helpful decision tree (see https://www.bmj.com/content/377/bmj.o775/infographic). The National Institute for Health and Care Excellence updated guidelines for depression highlight the importance of an ongoing patient-physician relationship and for management of less severe depression to begin with various nondrug treatment options, such as guided self-help. For more severe depression, treatment should begin with cognitive behavior therapy, medication, or both.41
Editor's Note: This article was cowritten by Dr. Mark Ebell, deputy editor for evidence-based medicine for AFP and cofounder and editor-in-chief of Essential Evidence Plus, published by Wiley-Blackwell, Inc. Because of Dr. Ebell’s dual roles and ties to Essential Evidence Plus, the concept for this article was independently reviewed and approved by a group of AFP’s medical editors. In addition, the article underwent peer review and editing by four of AFP’s medical editors. Dr. Ebell was not involved in the editorial decision-making process.—Sumi Sexton, MD, Editor-in-Chief
The authors thank Wiley-Blackwell, Inc., for giving permission to excerpt the POEMs; Drs. Allen Shaughnessy, Henry Barry, David Slawson, Nita Kulkarni, and Linda Speer for selecting and writing the original POEMs; the academic family medicine fellows and faculty of the University of Missouri–Columbia for their work as peer reviewers; CMA Joule for supporting the POEMs CME program in Canada; Pierre Pluye, PhD, for codeveloping the Information Assessment Method; and Maria Vlasak for her assistance with copyediting the POEMs.

