Key Points for Practice
• Perform physical and ultrasound examinations in patients with abdominal trauma to identify patients who need immediate surgical exploration.
• Perform serial abdominal examinations in patients who have experienced abdominal trauma because missed bowel injuries are common.
• Do not rely on CT to exclude bowel injury in abdominal trauma because CT misses up to 28% of bowel injuries.
From the AFP Editors
Traumatic bowel injury, including mesenteric injury, affects 1 in 5 cases of penetrating abdominal trauma and 1 in 100 cases of blunt abdominal trauma. Bowel and mesenteric injuries are challenging to identify in the context of multiple injuries; however, they need to be treated promptly to prevent significant consequences. The World Society of Emergency Surgery published guidelines for identifying and treating bowel injuries.
Assessment After Abdominal Trauma
Rapid assessment is essential in abdominal trauma because mortality increases by 1% for every three minutes in the emergency department. Initial assessment after trauma involves a primary survey for life-threatening injuries and a focused assessment with sonography for trauma (FAST) evaluation. Immediate surgical consultation is recommended if the FAST evaluation finds intra-abdominal fluid, especially in hemodynamically unstable patients. Peritoneal lavage, the withdrawal of abdominal fluid to assess for blood, has a lower positive predictive value than the FAST evaluation and results in unnecessary laparotomies.
The importance of abdominal examination findings depends on the mechanism of injury and the presence of distracting injuries that may reduce examination accuracy.
Although blunt abdominal injuries often lack external signs of injury, the seat belt sign (i.e., bruising where the seat belt restrained a patient involved in a motor vehicle incident) represents a 12% risk of bowel or splenic injury. Similarly, children with abdominal bruising from bicycle handlebars are at increased risk of multiple abdominal organ injury including bowel injury.
After bowel injury, signs of peritoneal irritation may be delayed for several hours. Serial abdominal examinations can decrease missed abdominal injuries in patients who do not require immediate surgery. Failure when attempting enteral feeding can indicate a missed bowel injury.
A serum procalcitonin level is more accurate than other liver or bowel injury biomarkers but can take hours to days to indicate injury. Serial procalcitonin monitoring should be considered for patients admitted to the hospital.
Role of Computed Tomography
Computed tomography (CT) has limited accuracy in identifying bowel injuries. Bowel wall hematomas, bowel wall discontinuities, oral contrast media extravasation, and intra-abdominal free air indicate the need for immediate surgical exploration. Although free fluid, bowel wall thickening, and mesenteric stranding suggest bowel injury, none are specific enough to require surgery.
CT can miss up to 20% of bowel injuries in blunt trauma and up to 28% in penetrating trauma. However, for penetrating trauma with entry wounds on the posterior or flank, CT is the test of choice. In addition to CT findings suggesting bowel injury, metallic fragments within the bowel wall or lumen warrant immediate surgical consultation.
When CT is used, intravenous contrast media alone is comparable to adding oral and rectal contrast media. Repeat CT should be considered after six hours for patients at risk of bowel injury despite initial negative CT results.
Surgical Options
Laparotomy is the safest option for exploration, hemostasis, and repair of abdominal trauma and is recommended when patients are hemodynamically unstable or have peritonitis. Primary bowel repair and anastomosis are preferred unless the complication risk is high because of patient instability. If the complication risk is high, an ostomy or initial damage control surgery with delayed anastomosis should be performed. Damage control surgery can involve an anastomosis, ostomy, or bowel resection with the ends left separated for a second surgery to evaluate or complete the repair. The complication risk increases with time to definitive repair. Stomas can also be formed, but reversal increases the complication risk.
Diagnostic or therapeutic laparoscopy is less invasive than laparotomy and is increasingly used for hemodynamically stable patients in certain clinical situations. Laparoscopy can be used to diagnose and treat peritoneal and diaphragmatic injuries in penetrating trauma. Diagnostic laparoscopy misses up to 45% of bowel injuries; therefore, observation is required after a negative laparoscopy. Laparoscopic repair of bowel injury is technically challenging and requires more equipment and longer surgeries than open repair.
Wound exploration, in which a wound is probed under local or general anesthesia to visualize whether the peritoneum has been pierced, can be used to evaluate penetrating abdominal wounds. Visualization often requires surgical wound extension during exploration.
Missed Bowel Injury
In blunt trauma, bowel injuries are often missed due to insidious presentation, the unreliable nature of physical examination in multiple-trauma patients, and initial nonspecific imaging findings. Morbidity and mortality increase when surgical intervention is delayed more than five hours from the initial presentation. In addition to a high index of suspicion, serial examinations and repeat imaging are strongly recommended if nonoperative management is pursued in patients with blunt abdominal trauma.
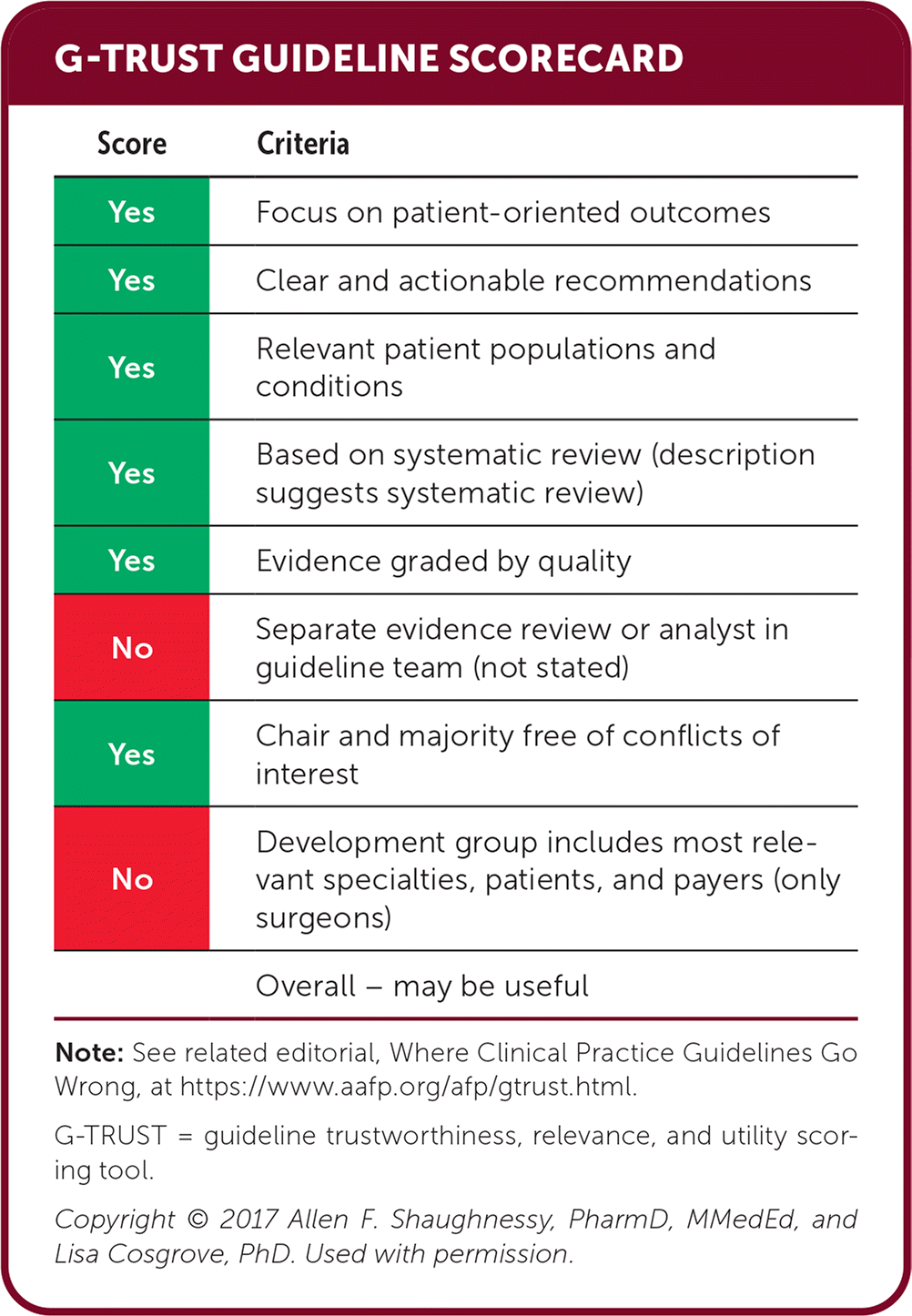
G-TRUST GUIDELINE SCORECARD
| Score | Criteria |
|---|---|
| Yes | Focus on patient-oriented outcomes |
| Yes | Clear and actionable recommendations |
| Yes | Relevant patient populations and conditions |
| Yes | Based on systematic review (description suggests systematic review) |
| Yes | Evidence graded by quality |
| No | Separate evidence review or analyst in guideline team (not stated) |
| Yes | Chair and majority free of conflicts of interest |
| No | Development group includes most relevant specialties, patients, and payers (only surgeons) |
| Overall – may be useful |
Note: See related editorial, Where Clinical Practice Guidelines Go Wrong, at https://www.aafp.org/afp/gtrust.html.
G-TRUST = guideline trustworthiness, relevance, and utility scoring tool.
Copyright © 2017 Allen F. Shaughnessy, PharmD, MMedEd, and Lisa Cosgrove, PhD. Used with permission.
Editor's Note: As mass shootings using high-velocity weapons previously limited to areas of conflict have become common, this guideline is sadly more relevant to our specialty. However, few of us have the time to pursue Advanced Trauma Life Support certification. There are many interesting elements of this guideline, such as the elevated risk demonstrated by abdominal bruising from seat belts or handlebars in blunt trauma, the limited accuracy of CT and laparoscopy in finding subtler bowel injury, and the resulting importance of serial abdominal examinations and the surgical options of wound exploration and laparoscopy.—Michael J. Arnold, MD, Assistant Medical Editor
The views expressed in this article are those of the authors alone and do not reflect the policy, views, or opinions of the U.S. Navy, Defense Health Agency, U.S. Department of Defense, or the U.S. government.
Guideline source: World Society of Emergency Surgery
Published source: World J of Emerg Surg. March 4, 2022;17(1):13.

