Key Points for Practice
• NSAIDs improve pain control and decrease opioid use in adults with traumatic fractures and should be used in most patients.
• NSAIDs may slightly increase the likelihood of nonunion.
• Opioid use after fracture also appears to increase the risk of nonunion.
• Intravenous ketorolac is beneficial in the acute care of adult patients with a traumatic fracture without increasing fracture nonunion.
From the AFP Editors
Opioids have been traditionally used for analgesia after orthopedic trauma because of concern that nonsteroidal anti-inflammatory drug (NSAID) use increases fracture nonunion. Because opioid misuse and abuse have risen to critical levels and opioid use has also been associated with fracture nonunion, the safety of NSAID use after orthopedic trauma is an open question. The Eastern Association for the Surgery of Trauma and the Orthopaedic Trauma Association conducted systematic reviews to publish guidelines for the use of NSAIDs after traumatic orthopedic fractures in adults with regard to acute pain control and risk of nonunion.
Risk of Nonunion
NSAIDs are recommended after fracture because the benefit of improved acute pain control outweighs the low risk of nonunion. Although NSAID use increased fracture non-union in more than 600,000 patients studied, the number needed to harm was 105 (95% CI, 47 to 1,173) compared with not using an NSAID. The risk might be slightly higher with chronic NSAID use before fracture, with indomethacin, and in patients with hip fracture.
The definition of nonunion and study results varied. Low-dose aspirin used for deep venous thrombosis prevention after fracture does not increase nonunion risk. One large claims database demonstrated that patients with chronic NSAID use before fracture were more likely to have non-union, which was similar to the risk with acute opioid use. In that same study, NSAID use for less than 30 days after fracture did not increase rates of nonunion. NSAID use for traumatic fractures does not increase rates of acute renal failure compared with other analgesic treatments.
Reduction of Opioid Use
Use of NSAIDs after traumatic fracture decreases the oral morphine equivalents used for acute pain control during hospitalization, whether the fracture is treated operatively or nonoperatively. NSAID use results in improved pain control from the first several hours through the first week after the fracture.
Specific NSAIDs
Intravenous ketorolac in the acute care setting appears to improve traumatic fracture pain and decreases opioid use without increasing nonunion. Limited study has not shown that cyclooxygenase-2 selective NSAIDs are superior to non-selective NSAIDs for fracture nonunion.
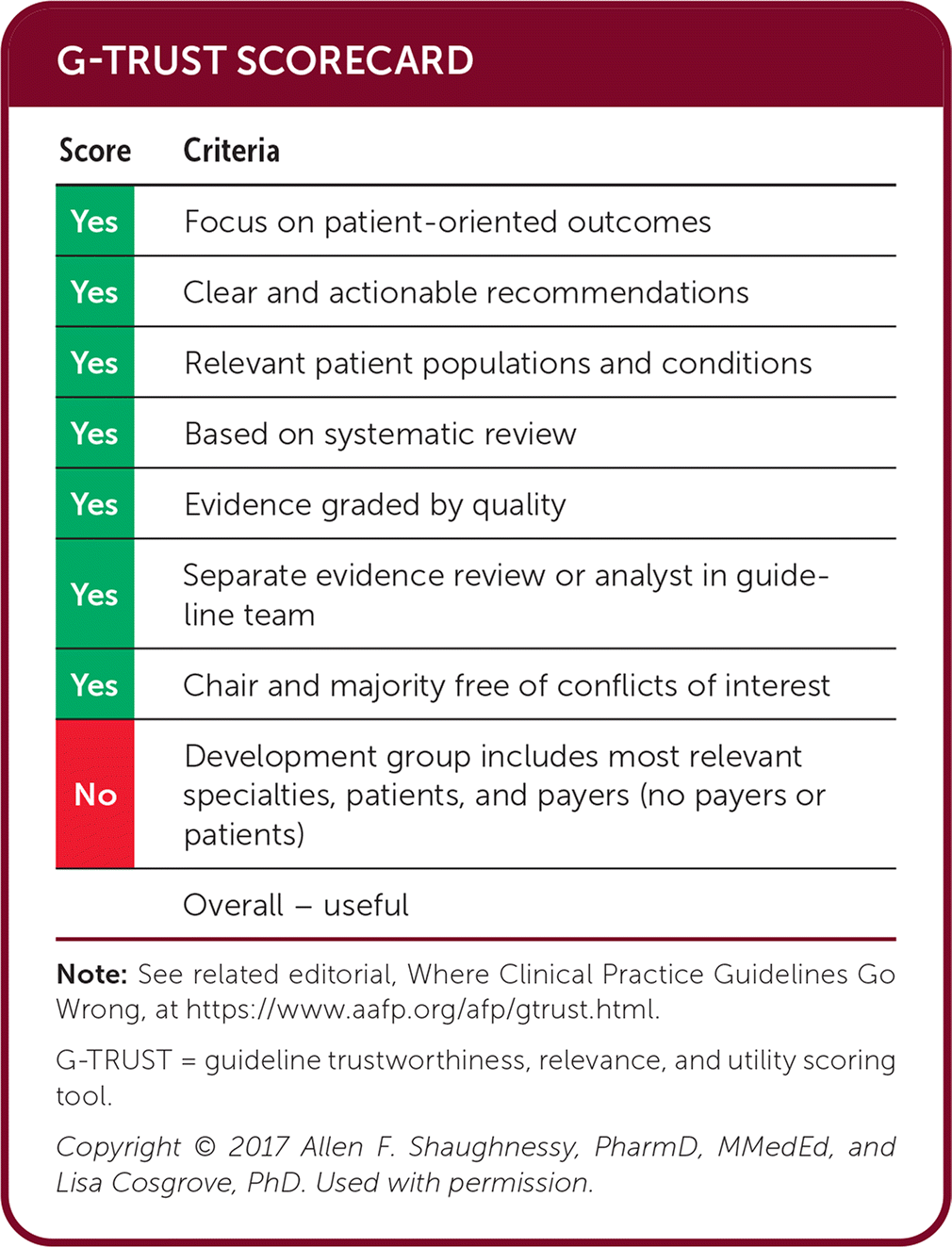
G-TRUST SCORECARD
| Score | Criteria |
|---|---|
| Yes | Focus on patient-oriented outcomes |
| Yes | Clear and actionable recommendations |
| Yes | Relevant patient populations and conditions |
| Yes | Based on systematic review |
| Yes | Evidence graded by quality |
| Yes | Separate evidence review or analyst in guideline team |
| Yes | Chair and majority free of conflicts of interest |
| No | Development group includes most relevant specialties, patients, and payers (no payers or patients) |
| Overall – useful |
Note: See related editorial, Where Clinical Practice Guidelines Go Wrong, at https://www.aafp.org/afp/gtrust.html.
G-TRUST = guideline trustworthiness, relevance, and utility scoring tool.
Copyright © 2017 Allen F. Shaughnessy, PharmD, MMedEd, and Lisa Cosgrove, PhD. Used with permission.
Editor's Note: The number needed to harm reported in the Practice Guideline was calculated by the authors based on raw data provided in the original guideline.
This guideline is important because it finally questions something many of us have been taught by orthopedists in medical school and residency—avoid NSAIDs with fracture because they delay healing and lead to nonunion. These two orthopedic trauma societies looked at the evidence and found several interesting things despite limited evidence: (1) there is an increased risk of nonunion with NSAID use, but it is small; (2) the nonunion risk is highest in patients with previous chronic NSAID use and with longer courses and may not occur with less than 30 days of use; and (3) opioid use also seems to increase the risk of nonunion, so switching to opioids does not eliminate risk. That is the kind of evidence we can use to make better decisions.—Michael J. Arnold, MD, Assistant Medical Editor
The views expressed are those of the author and do not necessarily reflect the official policy or position of the Uniformed Services University of the Health Sciences, U.S. Air Force, U.S. Department of Defense, or U.S. government.
Guideline source: Eastern Association for the Surgery of Trauma and the Orthopaedic Trauma Association
Published source: Murphy PB, Kasotakis G, Haut ER, et al. Efficacy and safety of non-steroidal anti-inflammatory drugs (NSAIDs) for the treatment of acute pain after orthopedic trauma: a practice management guideline from the Eastern Association for the Surgery of Trauma and the Orthopedic Trauma Association. Trauma Surg Acute Care Open. 2023;8(1):e001056.

