Key Points for Practice
• Treat older patients who have nonvalvular atrial fibrillation or venous thromboembolism with direct oral anticoagulants, including apixaban and dabigatran, instead of rivaroxaban. Use apixaban in patients with reduced kidney function. Warfarin should be avoided as initial therapy.
• In older adults, sodium-glucose cotransporter-2 inhibitors may be used, but patients should be monitored for urogenital infections and euglycemic diabetic ketoacidosis.
• Avoid combining three or more medications that act on the central nervous system or two or more medications with strong anticholinergic properties.
From the AFP Editors
The Beers criteria for potentially inappropriate medication use in older adults are currently managed by the American Geriatrics Society and have been updated seven times since their introduction in 1991. The criteria suggest medications that should be avoided in most older patients and in certain situations and combinations. These recommendations do not apply to patients in hospice or end-of-life care.
Although medication costs were not factored into risk decisions, the panel understands that costs may be important in shared decision-making.
Antithrombotic Medications
Antithrombotic medications dominated the panel's attention because of new evidence of risk in older adults with nonvalvular atrial fibrillation and venous thromboembolism.
The criteria recommend direct oral anticoagulants for initial treatment, particularly apixaban (Eliquis) or dabigatran (Pradaxa). Rivaroxaban (Xarelto), which has a higher risk of major bleeding and gastrointestinal bleeding and is not preferred, can be considered because of its once-daily dosing. For patients with reduced kidney function, only apixaban is recommended.
The panel recommends not using warfarin as initial therapy because of even higher bleeding risk, although continuation of warfarin in long-term users with well-controlled international normalized ratio levels is recommended.
Aspirin should be avoided for primary prevention of cardiovascular disease in older adults, which is consistent with the U.S. Preventive Services Task Force recommendation (https://www.uspreventiveservicestaskforce.org/uspstf/recommendation/aspirin-to-prevent-cardiovascular-disease-preventive-medication). Ticagrelor (Brilinta) and prasugrel (Effient) increase the risk of major bleeding in older adults compared with clopidogrel, and this risk should be compared with cardiac benefit.
Estrogen
Oral and transdermal estrogen products should be avoided in older patients. Topical vaginal estrogen is appropriate for vaginal atrophy and urinary tract infection prophylaxis.
Diabetes Medications
All sulfonylurea medications should be avoided because of a higher risk of hypoglycemia, cardiovascular events, and all-cause mortalities compared with other treatments. Although the criteria caution against using sodium-glucose cotransporter-2 inhibitors because of increased risk of urogenital infections and euglycemic diabetic ketoacidosis, the panel acknowledges the value of these medications and recommends monitoring during early treatment.
Combinations to Avoid
Several medication combinations should be avoided in older patients:
- Three or more medications that act on the central nervous system (e.g., antiepileptics, antidepressants, antipsychotics, opioids, benzodiazepines)
- Renin-angiotensin system inhibitor (e.g., angiotensin-converting enzyme inhibitor, angiotensin receptor blocker) with another renin-angiotensin system inhibitor, a potassium-sparing diuretic, or lithium
- Warfarin with amiodarone, selective serotonin reuptake inhibitors, or certain antibiotics (e.g., ciprofloxacin, macrolides, trimethoprim/sulfamethoxazole)
- Two or more medications with strong anticholinergic properties (Table 1)
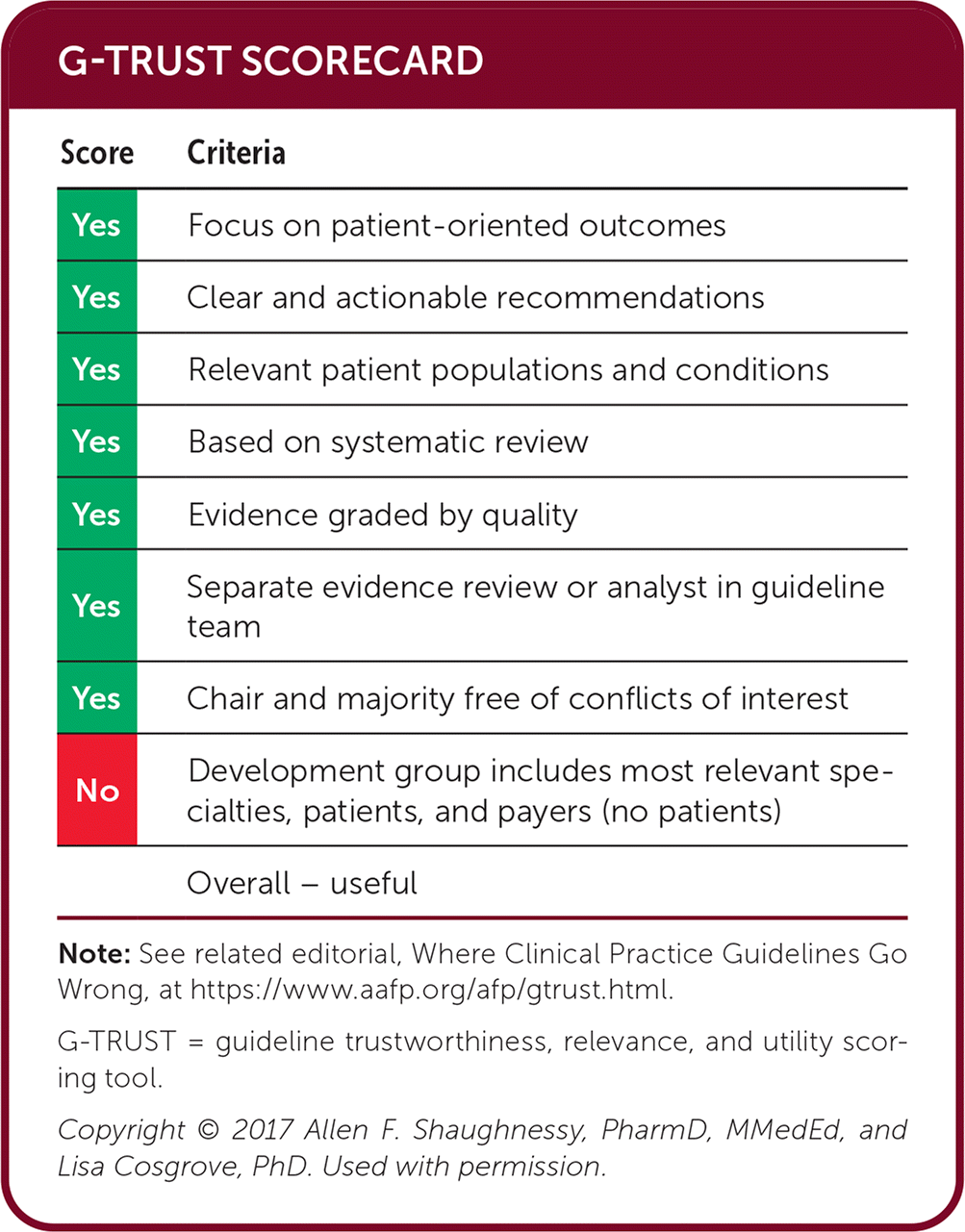
G-TRUST SCORECARD
| Score | Criteria |
|---|---|
| Yes | Focus on patient-oriented outcomes |
| Yes | Clear and actionable recommendations |
| Yes | Relevant patient populations and conditions |
| Yes | Based on systematic review |
| Yes | Evidence graded by quality |
| Yes | Separate evidence review or analyst in guideline team |
| Yes | Chair and majority free of conflicts of interest |
| No | Development group includes most relevant specialties, patients, and payers (no patients) |
| Overall – useful |
Note: See related editorial, Where Clinical Practice Guidelines Go Wrong, at https://www.aafp.org/afp/gtrust.html.
G-TRUST = guideline trustworthiness, relevance, and utility scoring tool.
Copyright © 2017 Allen F. Shaughnessy, PharmD, MMedEd, and Lisa Cosgrove, PhD. Used with permission.
Editor's Note: Updates to the Beers criteria provide an overview of the major evidence for medications that are most likely to harm older adults. The risk for antithrombotic medications are the most substantial part of the update. Although the actual medication lists are best integrated into the pharmacy module of the electronic health records, the latest updates offer insight into recent evidence for older adults. The American Geriatrics Soceity offers a mobile app with the Beers criteria for $9.99 annually to members and nonmembers.—Michael J. Arnold, MD, Assistant Medical Editor
The views expressed are those of the author and do not necessarily reflect the official policy or position of the Naval Undersea Medical Institute, Uniformed Services University of the Health Sciences, U.S. Navy, U.S. Department of Defense, or U.S. government.
Guideline source: American Geriatrics Society
Published source: American Geriatrics Society 2023 updated AGS Beers criteria for potentially inappropriate medication use in older adults. J Am Geriatr Soc. 2023;71(7):2052–2081

