
Fam Pract Manag. 1999;6(9):17-18
Financial crisis to hit Calif. medical groups, says CMA
Ninety percent of medical groups and IPAs in the state of California are “on the verge of collapse” due to financial troubles, according to a Sept. 2 report, “The Coming Medical Group Failure Epidemic,” from the California Medical Association (CMA). Citing data from the Price-WaterhouseCoopers accounting firm, the CMA projects that at least 34 medical groups or IPAs in the state will close or go bankrupt before the end of the year.
The report blames the financial turmoil, in part, on capitation rates that do not cover the cost of care. The CMA argues that if medical groups are to survive, health plans must negotiate fairly with physicians and must stop forcing groups to absorb the plans' excessive administrative costs.
Are your patients telling the whole truth?
In the struggle to avoid adverse drug reactions in their patients, physicians have a big obstacle: More than one-third of adult patients do not always provide their physicians with complete information regarding the prescription and over-the-counter medications they are taking, according to a recent survey of 1,000 patients.
The most problematic group of patients were 18- to 24-year-olds, of whom only 45 percent provided complete information. Women patients and older patients were the most truthful of all groups.
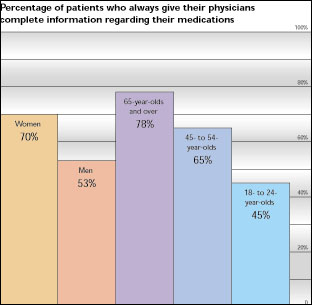
Source: Schwarz Pharma Inc., Pulse Beat Survey, 1999.
Health plan to begin dispatching ambulances
This fall, Kaiser Permanente becomes the first health care insurer to compete with 911. The health plan has signed a $600 million deal with American Medical Response (AMR), which will handle Kaiser's urgent calls from patients nationwide and will dispatch ambulances to them as needed. Supporters of the program say it will help reduce overuse of emergency services and will help patients receive appropriate medical care when they choose to call for nurse advice rather than 911.
However, critics worry that the new program will confuse patients about which number they should call in an emergency situation. “This puts fear into people that if they call 911, insurers won't pay for it,” said George Burke, spokesman for the International Association of Firefighters, in the Aug. 24 USA Today.
More health care insurers are expected to adopt programs similar to Kaiser's. The program is currently being tested by two other insurers.
Nation meets 15 percent of health goals
The latest report card on Americans' health shows that the nation has met 15 percent of the government's “Healthy People 2000” goals and is on track for another 44 percent. But for 20 percent of the objectives, the data are moving away from the targets. For the remainder, the data are inconclusive or show no change.
Positive findings include the following:
Cancer death rates are below the year 2000 target, due partly to a drop in the death rates for breast and colorectal cancer.
Infant and child mortality rates are down, dropping 50 percent and 40 percent, respectively, since 1979, thanks to efforts to decrease drownings, motor-vehicle-related deaths and fire-related deaths.
Life expectancy has increased, reflecting a continuing drop in deaths from heart disease and stroke.
The 44 percent of goals that are on schedule to be met include those related to childhood immunizations, breast-feeding, mammography screening and nutrition. Areas in which progress is not being made include obesity, childhood asthma and diabetes.
The annual report cards include more than 300 measures of Americans' health. The Healthy People initiative began in 1979.
Nonadherence named ‘major health threat’
The American Heart Association (AHA) has identified patient nonadherence as “a major hidden health threat” and estimates that the United States spends $100 billion annually as a result of patients not following appropriate treatment recommendations.
“The cost, in terms of human lives and money, is shocking,” says Martha Hill, PhD, RN, former AHA president. “It is particularly frustrating when effective strategies, identified more than 20 years ago, are not being used to fight this problem.”
The AHA reports that more than half of Americans with chronic diseases do not follow their physicians' medication and lifestyle guidance; nine out of 10 take their medications incorrectly; and two-thirds fail to take all their prescriptions.
Earlier this year, the AHA held its first Scientific Conference on Compliance in Healthcare and Research, part of a two-year effort to educate physicians, providers, health care organizations and patients about nonadherence and how to combat it.
Glossary
Benchmarking: The process of comparing your medical practice's performance (in areas such as mammography, childhood immunizations and patient satisfaction) with an acknowledged standard in order to improve the quality of care.
Value purchasing: A strategy that health care purchasers (e.g., employers) use to select managed care plans based on a combination of price and quality rather than price alone.
AAFP, AMIA offer guidance on physician-patient e-mail
In response to growing concerns about confidentiality and legal liability in physician-patient e-mail communication, the AAFP recently published “The Doctor Will E-mail You Now.” The 13-page monograph includes the American Medical Informatics Association's (AMIA) “Guidelines for the Clinical Use of Electronic Mail With Patients,” which were endorsed last year by the AAFP. The guidelines advise physicians to obtain patients' informed consent for use of e-mail, to file all e-mail messages in patients' charts and, when available, to use encryption technology.
For more information about the AMIA guidelines, contact the organization at 301-657-1291, or visit their Web site at www.amia.org. For a copy of the AAFP monograph, contact the order department at 800-944-0000, and ask for item A711.
Quote. End quote.
“The Piñata Syndrome [or the feeling that everyone is taking a whack at you] is manifested by physician-lounge grumbling, griping and grousing; sniping at medical and administrative leadership; resistance to examining best practices; refusal to hold colleagues responsible for their behavior; and general melancholy.”
Thomas J. Marr, MD, in the July/August 1998 Physician Executive, describing a physician disorder that he believes can lead to professional death.
Survey looks at health plan denials
Almost nine out of 10 physicians say their patients have experienced a denial of coverage for health care services in the last two years, according to a recent survey conducted by the Kaiser Family Foundation and Harvard University's School of Public Health. The survey, which included the responses of 601 physicians, also found that, across all types of services, between one-third and two-thirds of physicians say health plan denials have resulted in “somewhat serious” or “very serious” declines in their patients' health status.
The American Association of Health Plans (AAHP) has criticized the survey, saying it reports the percentage of physicians whose patients have experienced denials of coverage but does not report the percentage of services that are actually denied, a percentage it believes is low. The AAHP has also argued that many health plan denials are legitimate, the result of inappropriate medical care or incomplete paperwork.