
Fam Pract Manag. 2000;7(2):22-24
NPs rival MDs in primary care, says study
A study published in the Jan. 5 Journal of the American Medical Association has attempted to answer the often-debated question of whether independent nurse practitioners can provide the same quality of care as primary care physicians. The study, involving 1,316 patients randomly assigned to either physicians or independent nurse practitioners, found no significant differences in patients' health status or service utilization and only small differences in patient satisfaction.
But evidence that primary care physicians and nurse practitioners are interchangeable is “far from convincing,” wrote internist Harold C. Sox, MD, in an editorial in the same issue of JAMA. “It would have been useful to know how well the physicians and nurse practitioners compared in performing activities that are the hallmark of independent primary care practice,” such as making accurate diagnoses and caring for patients with multiple complex problems. “Equal skill in these diverse tasks would give a measure of confidence that a person who chose a nurse practitioner to be his or her long-term primary care caregiver would experience the same long-term outcomes as if he or she had chosen a physician,” wrote Sox.
Other weaknesses of the survey, wrote Sox, were its six-month time period, too short to test providers' competence across the broad spectrum of primary care, and its atypical patient mix, mostly Hispanic women in their 40s.
The AAFP has echoed similar concerns but acknowledged that the study “demonstrates again that primary care makes a positive difference in the health of patients.”
Health plans need consent to access patient records
The 4th District Court of Appeals has upheld a lower court's ruling that insurers cannot access medical records without patients' consent. The issue originated with a 1997 case in which Humana Medical Plan of Florida terminated its contract with Charles Fischman, MD, and requested the charts of his Humana patients. Because the health plan could not present patient consent forms, Fischman refused to release the records, which prompted Humana to file suit against him.
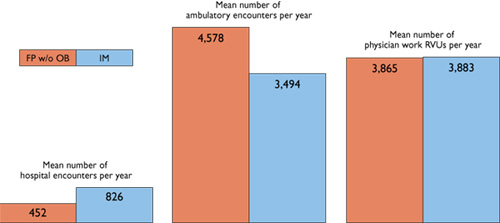
Physician productivity: How FPs, IMs compare
Physician productivity is never easy to gauge. It is a combination of both the number and complexity of patient encounters. One way of measuring complexity involves using relative value units (RVUs), developed by the Health Care Financing Administration to help determine Medicare reimbursement rates. According to a Medical Group Management Association survey, family physicians and internists are nearly even in terms of RVUs, although their mix of patient encounters are dissimilar.
Study shows effects of Medicare HMO withdrawals
A “substantial share” of Medicare beneficiaries were negatively affected when their managed care plans withdrew from Medicare, according to a recent study of 1,830 involuntarily disenrolled beneficiaries.
Thirty-five percent saw a decline in supplemental benefits, such as prescription drugs, dental care and eyeglasses.
Thirty-nine percent reported incurring higher premiums for supplemental benefits.
Twenty-two percent said they had to change their personal provider.
Forty-three percent reported being more worried about being able to pay their health care bills.
At the time of the study, HMOs had terminated 43 of their 347 Medicare risk contracts and reduced their service areas under another 54 contracts, affecting about 400,000 beneficiaries. Two-thirds of the disenrolled beneficiaries elected to join another HMO.
The study was conducted by the Henry J. Kaiser Family Foundation, the Barents Group LLC and Westat Inc.
AHCPR becomes AHRQ, refines mission
The Agency for Health Care Policy and Research (AHCPR) is now known as the Agency for Healthcare Research and Quality (AHRQ), pronounced “arc.” The change came in December when President Clinton reauthorized the agency until 2005 by signing the Healthcare Research and Quality Act of 1999.
AHRQ is now the lead federal agency on quality-of-care research and will be working to promote evidence-based medicine, to reduce medical errors and to expand research on the cost and utilization of health care services, among other priorities.
HMOs don't have to disclose physician incentives, says court
A federal appeals court in New Orleans recently affirmed a lower court's dismissal of a lawsuit that would have forced five Texas HMOs to disclose financial incentives paid to physicians. The case centered on whether the HMOs violated the Employee Retirement Insurance Security Act by not telling patients of their financial arrangements with physicians. According to the Jan. 5 Hartford Courant, the plaintiffs claimed that the financial incentives hurt patients by causing physicians to keep referrals and testing to a minimum.
Later this month, the U.S. Supreme Court is expected to hear arguments on whether a trial should be granted in a similar case.
Quote. End quote.
“At least the [HMO] industry now believes it has something to prove to the public rather than simply being interested in proving to Wall Street that it can limit costs and make a profit.”
Jamie Court of Consumers for Quality Care, in the Nov. 29 USA Today, responding to an American Association of Health Plans memo that praised United Health Group's recent announcement to end preauthorization requirements and urged health plan executives to consider other creative approaches to improve patient care and manage costs.
Y2K Update $100 billion and barely a hiccup
At 11 p.m. Dec. 31, 1999, it was man over machine at New York's Mount Sinai Medical Center as hospital staff made final preparations to bring in the new year. According to the Jan. 3 Wall Street Journal, pitchers were filled with water, elevator use was off-limits and extra staff stood ready to manually pump air into patients if respirators failed. All this despite the estimated $25 million to $40 million dollars the hospital spent to ensure that its medical equipment and computer systems were Y2K compliant. When the ball dropped in Times Square, nothing out of the ordinary occurred at Mount Sinai, and only minor glitches were detected elsewhere in the United States. Federal and state governments and U.S. corporations spent an estimated $100 billion to fix possible Y2K glitches, with apparent success. The final Y2K test will come Feb. 29, the first leap year to occur in a new millennium since 1600.
Computer-based courses among HCFA's new education programs
The Health Care Financing Administration (HCFA) recently launched several free provider training programs that go beyond reading the traditional manual to understand Medicare regulations. HCFA is testing computer-based training (CBT) courses and satellite broadcasts to educate physicians in a number of Medicare-related topics, including the following:
Computer-based training —Adult Immunization, Fraud and Abuse, Front Office Management, HCFA-1450 Form (UB92), HCFA-1500 Form, Home Health Agency, ICD-9 Diagnosis Coding, Introduction to the World of Medicare, Medicare Secondary Payer, and Women's Health. The interactive, self-paced CBT modules can be downloaded to your computer from www.medicaretraining.com/cbt.htm.
Satellite broadcasts — Fraud and Abuse: Proactive Measures to Avoid Becoming a Victim, Resident Training: What Every Medical Resident Needs to Know About Medicare, Steps to Promoting Wellness: Adult Immunizations, and Steps to Promoting Wellness: Women's Health. Free videotapes of the 1999 broadcasts are available from www.medicaretraining.com/satellite.htm.