Fam Pract Manag. 2000;7(4):17
HCFA pays $3 million to insure deceased
The Health Care Financing Administration (HCFA) paid $3.1 million in capitated payments to HMOs between January 1993 and April 1999 for 102 beneficiaries who had died, according to a recent audit by the Department of Health and Human Services (HHS).
The improper payments resulted because HCFA failed to stop payments in a timely manner and, in some cases, did not know that the patients had died.
Although HCFA has recouped approximately $1.2 million of the payments, HHS has since found that HCFA has been paying for an additional 157 deceased beneficiaries, resulting in another erroneously paid $1.1 million.
AMA drops physician accreditation program
The AMA's board of trustees has decided to discontinue the accreditation of physicians through the American Medical Accreditation Program (AMAP), citing an inability to attract enough physicians and insurance plans to make the program financially viable. The AMA established the program in 1996 to set standards of clinical practice for physicians and to hold them accountable for their performance. According to a memo from D. Ted Lewers, MD, chair of the AMA board of trustees, the AMA will continue to explore other, more financially viable options to develop high-quality physician standards of practice.
Quote. Endquote.
“Physicians who are forced to follow these guidelines are forced to commit malpractice. … There are no data or clinical studies that show the recommendations are safe. Zero. None. Nothing. The guidelines don't reflect reality.”
Thomas Cleary, MD, head of pediatric infectious diseases at the University of Texas-Houston Medical School, one of two physicians suing Milliman & Robertson for falsely linking their names with pediatric care guidelines that have “no basis in sound medical practice,” according to the March 5 Houston Chronicle.
Evidence-based guidelines available online
The National Guideline Clearing-house now has almost 700 evidence-based clinical practice guidelines available on its Web site (www.guideline.gov), which was launched just over one year ago. The site is continually updated and enables health care professionals to compare clinical recommendations submitted by 125 health care organizations, associations, medical societies and federal agencies.
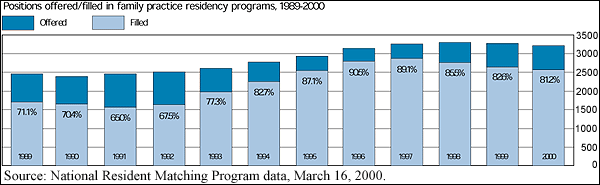
Match results: Third straight drop for family practice
For the third consecutive year, the number of filled positions in family practice residency programs has dropped, according to preliminary data from the National Resident Matching Program. Of 3,206 positions offered this year, 2,603 (or 81.2 percent) were filled, and only 1,833 (or 57.2 percent) were filled by U.S. seniors.
The primary care components of internal medicine and pediatrics also saw decreases in the number of positions filled, as did obstetrics/gynecology. Anesthesiology and emergency medicine were among the biggest winners of the year.
Potential reasons for the decreased interest in primary care may be students' observations of the hassles of managed care, the perceived threat of midlevel providers and the rise in medical student debt, which averages $90,745.
But in spite of the recent drops, family practice has had a strong decade experiencing, six consecutive years of increases between 1991 and 1997.