How payers assign patients to you will affect how your practice is evaluated and paid for value in the future.

When Congress passed the Medicare Access and CHIP Reauthorization Act (MACRA) in 2015, physicians hailed the demise of the sustainable growth rate formula, which had for many years threatened annual cuts in Medicare reimbursement. Now that MACRA regulations have been finalized, we are learning the extent to which Medicare payment will be transformed.1 Our payments will now be directly connected to the quality and cost of the care we provide. Those of us who provide higher quality, lower cost care will be paid more, and those who do not will be paid less. To accomplish its stated goal of tying 90 percent of all Medicare payments to quality or value by 2018, the Centers for Medicare & Medicaid Services (CMS) must know exactly which Medicare patients are yours – and which are not.2
The process that commercial and government payers use to assign patients to the physicians who are held accountable for their care is called attribution. Think of the patient lists that insurers send in the mail. If you review them at all, some names you recognize, some leave you scratching your head, and some are missing. Yet those lists will increasingly affect how much you are paid, regardless of whether the patients named on them are seen in your office. Understanding how attribution works is an important first step to succeeding in the new payment environment. Knowing which patients are attributed to you by each payer and how value-based payment programs affect different segments of your patient population will help you target your health care team's resources most effectively.
Which patients are yours?
When we think about whose patients are whose, many perspectives come into play. For example, I may see Mrs. Smith every fall and spring for her allergies, but she may see another physician every summer for her annual physical. Mrs. Smith may consider both of us “her doctor,” but her insurance company may not see it that way. The insurer may attribute her to the physician who performed her most recent annual wellness visit or to the one who saw her most recently. Attribution approaches vary, but they share common elements:
Timing. Attribution can be prospective, meaning the payer tells you at the beginning of the measurement year what patients you will be responsible for over the next 12 to 24 months. It can also be retrospective, meaning you find out at the end of the year which patients are in your panel and payers measure your care by looking back at the previous 12 to 24 months. According to the National Quality Forum, two-thirds of implemented attribution models use retrospective timing.3
Type of attribution rule. Some payers attribute patients to the physician who provided the majority of the patient's care. If no physician provided more than 50 percent of the patient's care, they may attribute the patient to the physician who provided the most, or the plurality, of the patient's care. Other payers assign patients to the physician who provided the plurality of the patient's primary care. Since most payers rely on claims data to attribute patients, two fundamental questions must be answered:
- How do payers define patient care? Some use inpatient and outpatient evaluation and management (E/M) codes. Others use only outpatient E/M codes.
- How do payers determine who provided patient care? Some, such as Medicare, use allowed charges. Others use relative value units (RVUs) or even the number of patient visits.
Exclusivity. The majority of payers attribute each patient to only one doctor.3 But some attribute patients to multiple doctors, meaning the same patient might be attributed to you, the family physician down the street who saw the patient once, and the patient's cardiologist.
Level of attribution. Some payers attribute patients to individual physicians, and others attribute patients to a group practice or even an accountable care organization (ACO), if the physician or group belongs to one. Whether patients should be assigned to individual clinicians or to groups or health systems is controversial. For physicians, it may feel unfair for payers to assign a patient's quality and cost measures to them when they do not control all of the factors that influence those measures.
The fact that payers use different methods of attribution further complicates practices' efforts to identify and take care of their patient populations in the ways payers expect. For example, Aetna uses either a majority or a plurality of total charges. Blue Cross Blue Shield applies a more complex hierarchy that looks initially at which physician billed the plurality of RVUs, then who billed the plurality of the outpatient E/M codes, and finally who billed the plurality of total charges. United Healthcare, on the other hand, just looks at which primary care doctor billed the majority of the charges. Attribution is simplest in health maintenance organizations (HMOs) and Medicare Advantage (MA) plans, because patients typically must choose a physician from a list of approved providers when they enroll in the insurance plan, and future changes must be patient-initiated.3
The changing landscape of Medicare attribution
The burning question is how will attribution work under MACRA?
The MACRA final rule stipulates specific attribution methods for each of the two payment pathways defined in the regulations.1 (See “Attribution methods under MACRA.”) All physicians enrolled in Medicare must choose between these two payment pathways – the Merit-Based Incentive Payment System (MIPS) or the Advanced Alternative Payment Model (Advanced APM). Physicians seeing a small volume of Medicare patients are excluded. (See “Medicare Payment Reform: Making Sense of MACRA,” FPM, March/April 2016.)
ATTRIBUTION METHODS UNDER MACRA
The Medicare Access and CHIP Reauthorization Act describes the patient attribution method for the Merit-Based Incentive Payment System (MIPS). Advanced Alternative Payment Models (APMs) may decide their own methods. For comparison, this chart lists attribution methods for MIPS and two types of Medicare accountable care organizations (ACOs).
| Category | Merit-Based Incentive Payment System (MIPS) | Medicare Shared Savings Program ACO | Next Generation ACO |
|---|---|---|---|
| Timing | Retrospective |
| Prospective |
| Measurement period | One year | Two years | Two years |
| Type of attribution rule | Plurality | Plurality | Plurality |
| Data used | Medicare Part B allowed charges for outpatient E/M codes (no inpatient or emergency department codes), Medicare wellness visits, transitional care management, and chronic care management codes. | Medicare Part B allowed charges for office visits, rest home visits, home visits, and Medicare wellness visits provided by primary care physicians and non-physician professionals (physician assistants, advanced practice nurses, and clinical nurse specialists). | Medicare Part B allowed charges for office visits, rest home visits, home visits, and Medicare wellness visits provided by primary care physicians and non-physician professionals (physician assistants, advanced practice nurses, and clinical nurse specialists). Patients can voluntarily align with ACO. |
| Exclusivity | Single physician | Single ACO | Single ACO |
| Level | Individual physician, but physicians can report and receive bonuses or penalties as a group or virtual group. | ACO | ACO |
| Basis |
| Unique APM participant identifier and physician's NPI. ACO treated as collection of TINs. | Unique APM participant identifier and physician's NPI. ACO treated as collection of TINs. |
| Tie breaker | Physician who provided most recent primary care service. |
| Primary care physician who provided most recent primary care service. |
| Patient exclusions | Not eligible for or not participating in Medicare Part B (for example, participating in a Medicare Advantage plan). |
|
|
The MIPS program will follow the attribution method currently used by Medicare's Value-Based Payment Modifier Program with a slight modification. It is retrospective, looking back one to two years for a plurality of allowed charges for outpatient services only. Under MIPS, each Medicare beneficiary will be attributed to a single physician based on the National Provider Identifier (NPI). The patients of physicians who are members of group practices will be attributed first to the individual physician using the NPI and then to the group practice based on its Taxpayer Identification Number (TIN). The Value-Based Payment Modifier Program used only the TIN, but the authors of the MACRA final rule incorporated the NPI to more accurately attribute patients within group practices, especially those with multiple locations and large numbers of physicians and other clinicians. Medicare uses a two-step algorithm to determine attribution. (See “Medicare's two-step attribution method.”) MIPS will also use common definitions for outpatient primary care (E/M codes are specified) and primary care providers (physicians, physician assistants, advanced practice nurses, clinical nurse specialists, and certified registered anesthetists).
MEDICARE'S TWO-STEP ATTRIBUTION METHOD
Medicare beneficiaries who do not receive any primary care services are not attributed. If they do receive primary care services from a physician, Medicare uses the following process to determine to whom the patient is attributed.
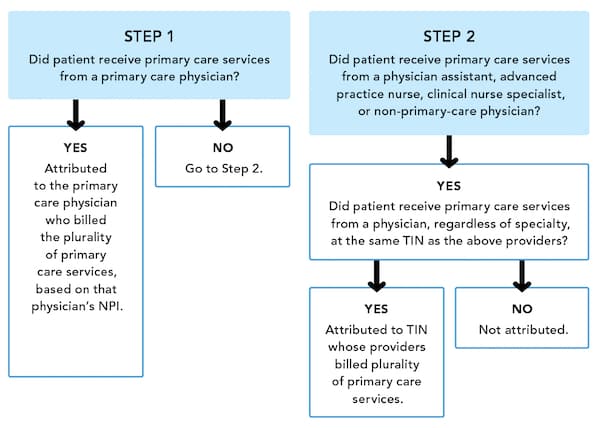
If you are participating in an Advanced APM such as a Medicare ACO or a patient-centered medical home, your Medicare patients will be attributed to you based on the attribution method used by the APM. The attribution methods used by Medicare ACO programs share common elements with those used by MIPS. Medicare tends to use the same models repeatedly, which gives both it and physicians the benefit of consistency and means you are likely to see these methods used in other programs in the future. (For examples of patient attribution under current rules and MACRA, see “Patient attribution scenarios.”)
PATIENT ATTRIBUTION SCENARIOS
The following patient cases illustrate how attribution methods work now and under the Medicare Access and CHIP Reauthorization Act (MACRA):
| Patient | History | Attribution (current Medicare) | Attribution (MACRA) |
|---|---|---|---|
| “TC” | Saw a local physician last year for a Medicare annual wellness visit, two chronic disease visits, and one acute visit. She has also seen her gynecologist for well-woman exams in the past two years. She saw her primary care physician twice this year for a chronic disease visit and an acute visit. After the physician disclosed his plans to retire, she established care with a new family physician. She has since come in for a cold and scheduled her annual wellness visit. | TC remains attributed to her prior primary care physician because he has billed the plurality of Medicare Part B allowed charges in the previous calendar year and billed the plurality of charges so far this year. | TC would remain attributed to her prior primary care physician under the Merit-Based Incentive Payment System (MIPS) because he has provided the plurality of Medicare Part B allowed charges. Once the claim for her most recent acute visit clears, however, the new practice gains plurality and attribution. |
| “KG” | Sees her family physician only when she is sick but periodically calls for health advice. She normally sees her gynecologist once a year for a well-woman exam but did not have a physical the last two years because of her schedule. Her most recent contact with any type of clinician was an urgent care visit for a urinary tract infection. | KG is not attributed to anyone because she has not received any primary care services besides one visit to an urgent care clinic, which does not count toward attribution. | KG still would not be attributed to anyone. However, she would be attributed to a physician she saw for a single acute visit. |
| “BW” | Has seen her family physician for seven years as part of a Medicare Advantage plan. During the previous calendar year, she visited her physician five times, including two acute visits, two chronic care visits, and an annual wellness visit. This year she has been seen four times, including one acute visit, two chronic care visits, and an annual wellness visit. | BW is attributed to her physician because she chose him as her primary care physician when she first selected a Medicare Advantage plan and selected the same plan for the current calendar year. | BW still would be attributed to her physician, but her care would be excluded from MIPS because she is enrolled in a Medicare Advantage plan. |
| “RJ” | Has for several years received care from a family medicine clinic whose physicians participate in a Medicare Shared Savings ACO. This year, he switched to a new clinic whose physicians participate in a Next Generation ACO. So far this calendar year, he has seen his new physician once for a chronic disease visit. Last year, RJ saw his previous primary care physician four times. He has not had an annual wellness visit this year or last, and was admitted to a hospital earlier this year for a stroke and discharged to a skilled nursing facility. | RJ remains attributed to his former practice because attribution to an existing Medicare ACO excludes him from attribution to a new Medicare ACO. | RJ would remain attributed to his former practice but under the Next Generation ACO rules could voluntarily assign his care to the new practice. |
| “CN” | Has been going to the county health clinic for primary care because of a lack of insurance. He turned 65 this year, enrolled in Medicare, and scheduled an appointment with his wife's primary care physician. | CN is not attributed to anyone because he is a new Medicare beneficiary this calendar year. | CN would be attributed to his new physician once he completes his initial visit and Medicare receives a claim with the physician's Taxpayer ID Number. |
What if you think CMS is wrong?
Attribution is based on claims data, which can take months to be fully adjudicated. Even under the best circumstances, CMS can make mistakes, attributing to you patients you have rarely or never seen, and attributing to others patients to whom you have provided extensive services. Under MACRA, erroneous determinations about the quality and cost of your care will affect your Medicare payment rate.
If you think CMS has made attribution or other errors, you may appeal by requesting a “targeted review.” However, these reviews are allowed only under certain circumstances. Specifically, you have to believe that 1) the measures or activities submitted to CMS and used to determine your bonus under MIPS have “calculation errors” or “data quality issues;” 2) performance category scores were incorrectly assigned to you; or 3) you should have been excluded from part or all of MIPS because you treat too few Medicare patients to participate. The final rule released in October does not specifically state that you can appeal incorrect patient attribution, but it also does not specifically exclude attribution of patients as grounds for an appeal.
The best way to deal with attribution problems is to identify and avoid them in the first place by asking your payers these key questions:
- Do they measure prospectively or retrospectively? How far back?
- How much patient care do you have to provide to meet the threshold of attribution?
- What data do they use to measure care?
- Do they attribute patients exclusively to a single physician or multiple ones?
- Do they identify providers by NPI?
- Do they attribute to an individual provider, the provider's group, or the group's ACO?
Ultimately, attribution is a confusing and wonky policy that exists in the background of your dealings with Medicare and other payers – that is, until a payer reduces your payment rate after evaluating your attributed panel and finding areas where your care is lacking. Taking time to understand attribution can help you understand the patient population you are accountable for and maximize reimbursement for the care you provide.

