The 2022 updates don't include massive E/M coding changes like last year, but several changes are much-needed and relevant to family physicians.

Once again, the start of a new year brings changes to CPT coding, Medicare payment policy, and Medicare's Quality Payment Program (QPP). Some of this year's changes are much-needed, which will hopefully lessen the pain of adjusting to them. Here's what's most relevant to family physicians.
CPT CHANGES
There are several noteworthy CPT changes this year, including some related to evaluation and management (E/M).
Office and other outpatient E/M services. Last year CPT made substantial changes to new and established patient E/M codes (99202-99215).1 This year CPT clarified several aspects of those changes, including the following:2
- Specifying which activities do not count when time is used to determine the level of service: travel, teaching that is general and not limited to management of that specific patient, and time spent on other, separately reported services.
- Clarifying when to report a test that is considered but not selected after shared decision making: A test that is considered but not performed counts as long as the consideration is documented. For example, the physician may explain to the patient that a diagnostic test the patient requested would have little benefit.
- Defining “analyzed” for reporting tests in the data column: “Analyzed” means using data as part of the medical decision making process. Tests that do not require an analysis still count if they are a factor in diagnosis, evaluation, or treatment.
- Clarifying the definition of a “unique” test: Multiple results of the same tests during an E/M service are considered one unique test. Tests with overlapping elements are not considered unique even if they have distinct CPT codes.
- Clarifying what is meant by “discussion” between physicians/other qualified health care professionals (QHPs) and patients: “Discussion” requires a direct, interactive exchange. Sending notes does not count.
- Clarifying who decides the difference between major and minor surgery: The classification of major and minor surgery is determined by the meaning of those terms when used by a trained clinician. It is not determined by payers' classifications of surgical packages.
KEY POINTS
- CPT clarified aspects of last year's E/M coding changes, including the definition of a “unique” test, what “discussion” between physicians and patients means, and the difference between major and minor surgery.
- There are several telehealth-related changes this year, including a Medicare provision for ongoing coverage of audio-only mental health services under certain conditions.
- The Centers for Medicare & Medicaid Services has increased the rates it pays for chronic care management and for administering several vaccines.
Principal care management services. CPT added a new category of principal care management (PCM) codes (99424-99427) to the “Care Management Services” section. Unlike chronic care management and complex chronic care management, PCM focuses on medical or psychological needs caused by a single, complex chronic condition expected to last at least three months. PCM services include establishing, implementing, revising, or monitoring a care plan directed toward that single condition. PCM codes can be reported by different physicians or QHPs in the same calendar month. Clinical documentation should reflect coordination of care among the managing clinicians.
Codes 99424 and 99425 are for services personally provided by a physician or QHP. Codes 99426 and 99427 are for services provided by clinical staff under the direction of a physician or QHP. Codes 99424 and 99426 are for the first 30 minutes per calendar month. Codes 99425 and 99427 are add-on codes for each additional 30 minutes per calendar month. PCM services that require fewer than 30 minutes a month are not reported separately. You can only report code 99427 twice in a calendar month. If the treating physician or QHP personally performs any care management services but does not meet the 30-minute threshold, those services can be counted toward the required time for the clinical staff codes.
All PCM services require the following elements:
- One complex chronic condition expected to last at least three months that places the patient at significant risk of hospitalization, acute exacerbation or decompensation, functional decline, or death,
- The condition requires development, monitoring, or revision of the disease-specific care plan,
- The condition requires frequent adjustments in the medication regimen, or the management of the condition is unusually complex due to comorbidities,
- Ongoing communication and care coordination between relevant clinicians providing care.
Remote therapeutic monitoring and treatment. CPT added three new codes for remote therapeutic monitoring of the respiratory and musculoskeletal systems. The codes are for reviewing and monitoring data related to signs, symptoms, and therapeutic responses during a 30-day period. The monitoring can include objective, device-generated data or subjective data provided by the patient. A physician or QHP must order the service, and the device must be a medical device as defined by the Food and Drug Administration (FDA). Do not report these codes with other physiologic monitoring services or if the monitoring is less than 16 days. Use code 98975 to report device setup and patient education. Use codes 98976 and 98977 to report supplying the device for scheduled recordings and/or programmed alert transmissions (98976 is for respiratory system monitoring, and 98977 is for musculoskeletal system monitoring).
CPT also added two new codes for treatment management services that stem from remote therapeutic monitoring. You can report these codes when a physician or QHP uses the results of remote therapeutic monitoring to manage the patient under a specific treatment plan. The codes require at least one interactive communication with the patient or caregiver. As with the monitoring codes, a physician or QHP must order the service, and the device must be a medical device as defined by the FDA. Code 98980 is for the first 20 minutes of service during a calendar month, and code 98981 is an add-on code for each additional 20 minutes. Do not report services of fewer than 20 minutes. You can report these services in addition to chronic care management, transitional care management, PCM, and behavioral health integration. Time spent on other separately reported services, including E/M services, cannot be counted toward the time of the remote therapeutic monitoring and treatment management services.
Vaccine and administration codes. CPT 2022 includes five new vaccine codes and nine new vaccine administration codes related to COVID-19. For administering a COVID-19 vaccine, report the vaccine product code with the corresponding immunization administration code.3 All COVID-19 vaccine codes are listed in the vaccine section of CPT and in a new Appendix Q.4 If more updates occur during the year, they can be found at https://www.ama-assn.org/practice-management/cpt/category-i-vaccine-codes.
Other new vaccine codes for 2022 include the following:
- 90671: Pneumococcal conjugate vaccine, 15-valent (PCV15), for intramuscular use,
- 90677: Pneumococcal conjugate vaccine, 20-valent (PCV20), for intramuscular use,
- 90626: Tick-borne encephalitis virus vaccine, inactivated; 0.25 mL dosage, for intramuscular use,
- 90627: Tick-borne encephalitis virus vaccine, inactivated; 0.5 mL dosage, for intramuscular use,
- 90759: Hepatitis B vaccine (HepB), 3-antigen (S, Pre-S1, Pre-S2), 10 mcg dosage, three-dose schedule, for intramuscular use.
Other services. The list of reportable telehealth services continues to expand. CPT identifies codes that can be reported using telemedicine with a star symbol (★) and lists them in Appendix P. This year CPT has added code 99211 to the list and included patient- and caregiver-focused health risk assessment codes 96160 and 96161. Inpatient prolonged services codes 99356 and 99357 also join the list.
CPT has revised the guidelines for repair (closure) to specify that chemical cauterization, electrocauterization, or wound closure utilizing adhesive strips as the sole repair material are included in the appropriate E/M code. CPT also revised the definition of a simple repair to clarify that hemostasis and local or topical anesthesia are not reported separately.
MEDICARE PHYSICIAN FEE SCHEDULE CHANGES
The Centers for Medicare & Medicaid Services (CMS) was set to lower the 2022 conversion factor (i.e., the amount Medicare pays per relative value unit, or RVU) from $34.89 to $33.59, but Congress intervened in December with a one-year rate increase of 3%. The new conversion factor is $34.6062, nearly the same as last year.
Telehealth. As the pandemic continues, CMS will retain all services temporarily added to the Medicare telehealth services list until the end of 2023. CMS will also implement telehealth mental health provisions enacted by the Consolidated Appropriations Act of 2021. This includes removing geographic restrictions and adding the patient's home as an eligible originating site for telehealth services for the diagnosis, evaluation, or treatment of a mental health disorder. This change extends beyond the pandemic. Telehealth services for mental health may be furnished in the patient's home if the physician or other clinician provided an item or service in person within the six months before the initial telehealth service, and within the 12 months before any subsequent telehealth service.
CMS has revised its definition of “interactive telecommunications system” to permit audio-only tele-mental health services provided to beneficiaries in their homes under certain conditions. Again, an in-person service must be furnished within six months of an initial audio-only mental health service and within 12 months of any subsequent audio-only mental health service. CMS will only cover this for physicians or providers who have the capacity to furnish two-way audio-video telehealth services but use audio-only because the beneficiary can't use, doesn't wish to use, or doesn't have access to two-way audio-video technology. CMS will create a modifier to identify audio-only services furnished to patients in their homes.
Finally, CMS is permanently adopting payment for code G2252 (Brief communication technology-based service, e.g., virtual check-in, by a physician or other QHP who can report E/M services, provided to an established patient, not originating from a related E/M service provided within the previous seven days nor leading to an E/M service or procedure within the next 24 hours or soonest available appointment; 11–20 minutes of medical discussion). The national (not geographically adjusted) 2022 Medicare payment allowance for this code was estimated at $27.21 in the nonfacility (e.g., office) setting, though this could change with the conversion factor.
Vaccine administration. Effective Jan. 1, 2022, CMS will pay $30 per dose for administering the influenza, pneumococcal, and hepatitis B vaccines. CMS will also maintain the current payment rate of $40 per dose for administration of the COVID-19 vaccines through Dec. 31 of the year in which the COVID-19 public health emergency ends. After that, CMS will reduce the COVID-19 vaccine administration payment rate to match other Medicare Part B vaccines.
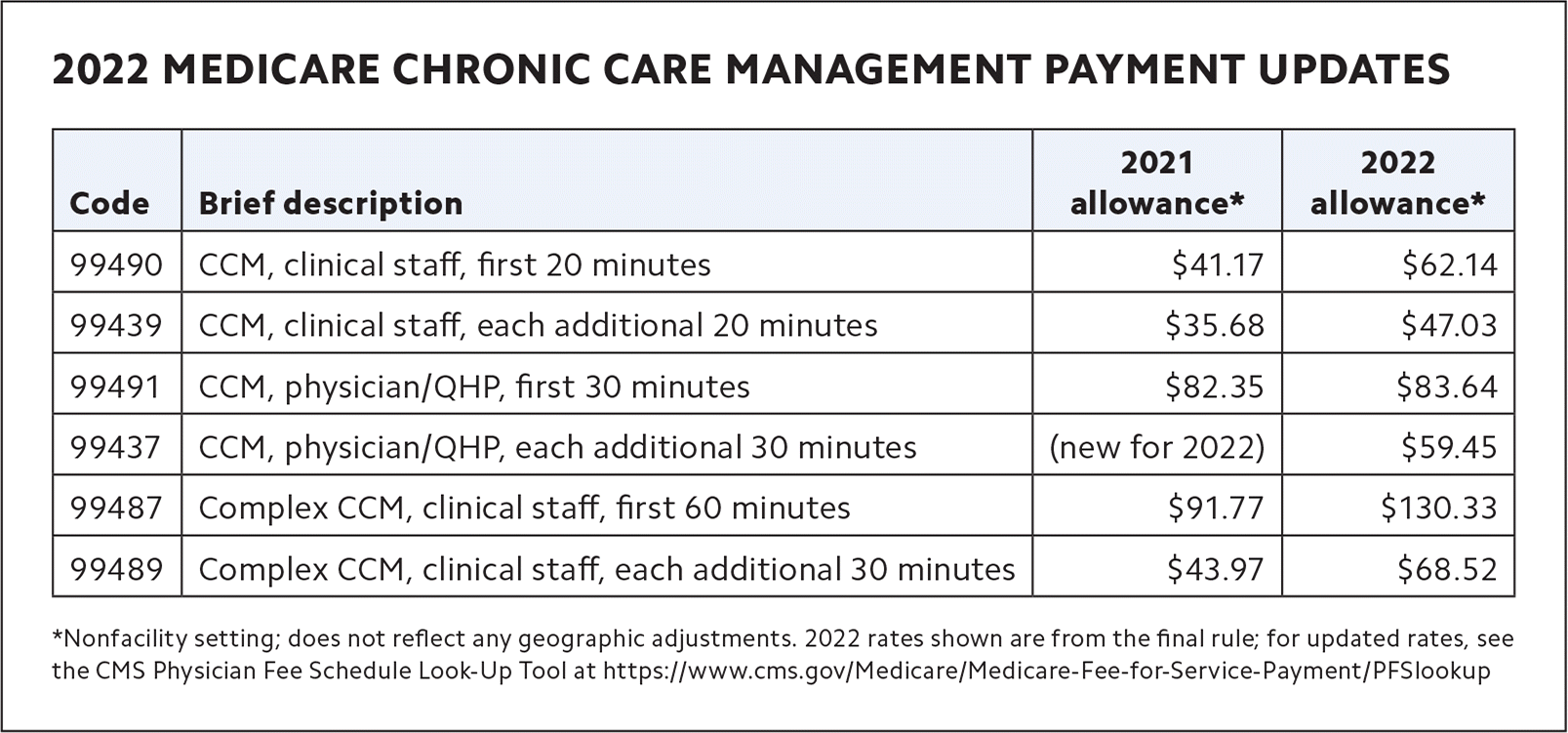
Chronic care management. CMS is increasing the RVUs for chronic care management codes, resulting in increased payment rates (see “2022 Medicare chronic care management payment updates”). For example, payment for code 99490 (Chronic care management, clinical staff, first 20 minutes) will increase about 50%. This also may change with the conversion factor.
2022 MEDICARE CHRONIC CARE MANAGEMENT PAYMENT UPDATES
| Code | Brief description | 2021 allowance* | 2022 allowance* |
|---|---|---|---|
| 99490 | CCM, clinical staff, first 20 minutes | $41.17 | $62.14 |
| 99439 | CCM, clinical staff, each additional 20 minutes | $35.68 | $47.03 |
| 99491 | CCM, physician/QHP, first 30 minutes | $82.35 | $83.64 |
| 99437 | CCM, physician/QHP, each additional 30 minutes | (new for 2022) | $59.45 |
| 99487 | Complex CCM, clinical staff, first 60 minutes | $91.77 | $130.33 |
| 99489 | Complex CCM, clinical staff, each additional 30 minutes | $43.97 | $68.52 |
*Nonfacility setting; does not reflect any geographic adjustments. 2022 rates shown are from the final rule; for updated rates, see the CMS Physician Fee Schedule Look-Up Tool at https://www.cms.gov/Medicare/Medicare-Fee-for-Service-Payment/PFSlookup
E/M services. Physicians who teach residents should know that CMS policy changes may affect payment for their services. Specifically, when total time is used to determine the office/outpatient E/M visit level, only the time the teaching physician was present can be included. Also, for those teaching under Medicare's “primary care exception,” only medical decision making can be used to select the E/M visit level.
The agency is also refining its longstanding policies for split (or shared) E/M visits:
- Defining split (or shared) E/M visits as those provided in the facility setting by a physician and a nonphysician provider (NPP) in the same group. The physician or NPP who provides the substantive portion of the split visit should bill for it.
- Clarifying that the substantive portion of the visit can be history, physical exam, medical decision making, or more than half the total time (except in cases of critical care, when the substantive portion of the visit can only be more than half the total time). In 2023, CMS will define the substantive portion of the visit as more than half the total time.
- Establishing that split (or shared) E/M visits can be reported for new or established patients, initial and subsequent visits, and prolonged services.
CMS will require modifier FS on claims to identify these services. Documentation in the medical record must identify the two individuals who performed the visit, and the individual who provides the substantive portion must sign and date the medical record.
MEDICARE QUALITY PAYMENT PROGRAM CHANGES
Much of the Quality Payment Program will remain the same for performance year 2022. However, CMS is making a few notable changes to the Merit-based Incentive Payment System (MIPS).
MIPS quality performance category. In 2022, CMS will assess eligible clinicians on two additional administrative claims measures (as applicable):
- Risk-standardized acute unplanned cardiovascular-related admission rates for patients with heart failure,
- Clinician/group risk-standardized hospital admission rates for patients with multiple chronic conditions.
The data completeness threshold will stay at 70% for 2022 and 2023.
CMS had intended to sunset the CMS Web Interface as a reporting mechanism starting in 2022, but is now extending it for another year. Starting with the 2023 performance year, though, those who have been using the interface will have to switch to another reporting mechanism (e.g., a qualified clinical data registry).
CMS is making the following scoring policy changes in 2022:
- Establishing a scoring floor for the first two years that measures are included in the program. Measures in their first year will receive 7–10 points. Measures in their second year will receive 5–10 points. Measures must have a benchmark and meet data completeness and case minimum criteria to qualify for the scoring floor.
- Ending bonus points for reporting additional outcome and high-priority measures, and for end-to-end electronic reporting.
MIPS cost performance category. CMS finalized the addition of five new episode-based cost measures: melanoma resection, colon and rectal resection, sepsis, diabetes, and asthma/chronic obstructive pulmonary disease.
MIPS improvement activities category. CMS updated its improvement activity inventory and is modifying the criteria for nominating new activities. The agency is adding seven new activities and modifying 15 existing activities, with a focus on increasing health equity.5
MIPS promoting interoperability (PI) category. Beginning in performance year 2022, CMS will apply automatic reweighting of the PI category to small practices and clinical social workers. CMS also made a few changes to the reporting requirements for the PI category. Practices must accept or claim an applicable exclusion to two registry measures that were previously optional: immunization registry reporting and electronic case reporting. CMS added a fourth exclusion option for electronic case reporting: Practices may claim an exclusion if they use certified EHR technology that does not meet the electronic case reporting certification criterion before the selected performance period. Practices that accept the remaining registry reporting measures (public health registry, clinical data registry, or syndromic surveillance) will earn five bonus points toward their PI score.
CMS also added a new, required attestation-based measure. Practices must attest to conducting an annual assessment of the High Priority Practices of the Safety Assurance Factors for EHR Resilience (SAFER) Guides.
MIPS scoring policies. CMS typically establishes quality measure benchmarks using data from two years before the performance period. Therefore, CMS will base benchmarks for the 2022 MIPS performance period on data from 2020.
CMS will continue to double the complex patient bonus for the 2021 performance year and cap it at a maximum of 10 points. The agency will revise the complex patient bonus starting with performance year 2022 and limit it to clinicians who have a median or higher value for at least one of the two risk indicators. CMS will update the formula so the bonus targets clinicians who have a higher share of socially or medically complex patients.
Beginning in 2022, CMS must set the performance threshold at either the mean or median of all MIPS scores from a previous period. As such, CMS is using the mean final score from the 2017 MIPS performance year. The performance threshold for 2022 is 75 points, and the exceptional performer threshold is 89 points. Eligible clinicians will receive a payment increase or decrease of up to 9% on their Medicare Part B claims in 2024, depending on how their performance compares to the threshold.
By law, the quality and cost categories must be equally weighted by performance year 2022, so they will both count for 30% of the final score this year. The improvement activities and promoting interoperability performance category weights remain unchanged at 15% and 25%, respectively.
The “extreme and uncontrollable circumstances” policy allows MIPS participants to request reweighting for any of the performance categories. CMS will automatically apply the exception to performance year 2021 because of the COVID-19 pandemic.6
Medicare Shared Savings Program (MSSP). CMS made relatively minor changes to the Alternative Payment Model Performance Pathway (APP) overall, but one exception relates to MSSP participants. CMS extended the CMS Web Interface reporting option for MSSP accountable care organizations (ACOs). They will have the option to report through either the interface or the APP measure set through the 2024 performance year but will be required to report the APP measure set beginning in 2025.
CMS is also delaying an increase of the MSSP quality performance standard to the 40th percentile of all MIPS quality scores until the 2024 performance year. CMS established a quality performance standard incentive for ACOs that report using the APP measure set for the 2022 or 2023 performance years.
CONSULT YOUR PAYERS
These are not all the updates to the Medicare physician fee schedule, Quality Payment Program, or CPT codes. But this is a high-level list of the most important changes you need to know in 2022. As always, individual payers may approach these changes differently, so you're advised to consult with those in your area to find out how they will handle them.

