In the exam room, the distinction between one type of visit and another isn't always clear. It's important to know when — and how — you can bill for both.

In family medicine, it's common for a medical problem to crop up during a routine preventive visit, or for a preventive service to crop up during a problem-oriented visit. For example, let's say you're finishing up a Medicare annual wellness visit when the patient lifts his shirt and says, “Oh yeah, I'd also like you to look at this rash,” which results in a prescription. Or, at a follow-up visit for a patient's chronic condition, you notice he is overdue for a flu shot and colorectal screening, so you perform a preventive visit too.
From a coding perspective, there is a bright line between a preventive medicine visit and a problem-oriented visit. One is for promoting health and wellness, and the other is for addressing an acute or chronic medical problem. But in the exam room, the distinction isn't always clear. The question for family physicians is this: When does the work in the exam room warrant billing for two distinct services?
The answer lies in knowing the requirements for various preventive medicine and Medicare wellness visits, knowing when you've done enough beyond those requirements to also bill for a separate E/M service, and knowing how to document and code it all. The good news is the 2021 E/M coding changes made it easier than it used to be.
KEY POINTS
- When physicians and other clinicians address a medical problem during a preventive or wellness visit, they can often bill for both services.
- Knowing the core components of preventive or wellness visits can help physicians recognize when they have done enough work beyond those requirements to bill for a separate evaluation and management service.
- Because preventive and wellness visits come with no cost sharing, it's best practice to explain to patients that a separate service performed during the same visit may result in a charge to them.
PREVENTIVE MEDICINE VISITS
Preventive medicine visits (CPT codes 99381-99397) are for patients covered by commercial insurance, Medicaid plans, and some Medicare Advantage plans. Patients value these visits because they are not subject to co-pays and deductibles. After age two, one preventive visit is covered annually.
According to CPT, preventive medicine visits are “comprehensive preventive medicine evaluation and management services of an individual including an age and gender appropriate history, examination, counseling/anticipatory guidance/risk factor reduction interventions, and the ordering of laboratory/diagnostic procedures.”
Codes 99381-99387 are for new patients and 99391-99397 are for established patients. Both are further broken down by age group. The extent of the exam, the content of the counseling and anticipatory guidance, and the recommended screenings and immunizations vary depending on the patient's age and gender. “Comprehensive” in the CPT definition is not synonymous with the comprehensive exam required in other E/M services. This is a common misconception among physicians and patients alike.
CPT states that if a new or existing problem is assessed and managed at the time of the preventive visit, the physician should also bill a problem-oriented visit (an office visit) on the day of the preventive care. But insignificant problems that do not require extra work should not be billed as office visits. If a patient comes in for a preventive visit and the clinician also looks at a rash or notices the patient's blood pressure is elevated, these observations alone are not enough to bill a problem-oriented E/M visit. There must be some medical decision making (MDM) that occurs, such as prescribing a topical treatment for the rash or choosing not to prescribe a medication for the high blood pressure and instead suggesting the patient change his diet.
Once you've documented your MDM, you can bill an E/M visit using codes 99202-99215 with the preventive medicine visit code. Make sure to add modifier 25 to the E/M code to signal to the payer that two distinct visits were done on the same day.
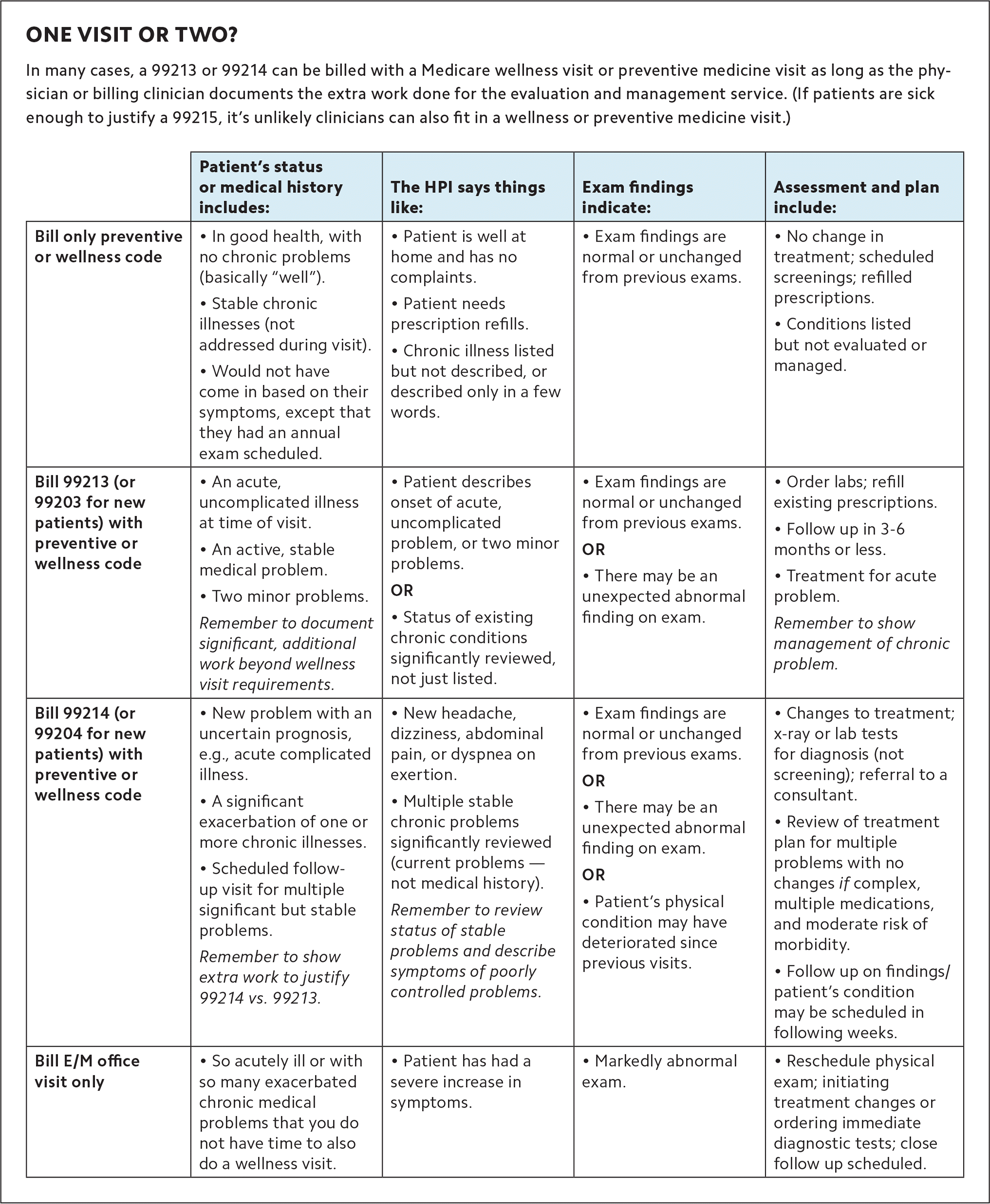
For more details on when to bill both visits, how to level the E/M portion, and what to include in your documentation, see “One visit or two?”
ONE VISIT OR TWO?
| Patient's status or medical history includes: | The HPI says things like: | Exam findings indicate: | Assessment and plan include: | |
|---|---|---|---|---|
| Bill only preventive or wellness code |
|
|
|
|
| Bill 99213 (or 99203 for new patients) with preventive or wellness code |
Remember to document significant, additional work beyond wellness visit requirements. |
|
|
Remember to show management of chronic problem. |
| Bill 99214 (or 99204 for new patients) with preventive or wellness code |
Remember to show extra work to justify 99214 vs. 99213. |
Remember to review status of stable problems and describe symptoms of poorly controlled problems. |
|
|
| Bill E/M office visit only |
|
|
|
|
MEDICARE WELLNESS VISITS
Original (traditional) Medicare does not cover CPT codes 99381-99397, because Medicare has its own wellness visits with their own “G” codes and requirements. As mentioned, some Medicare Advantage plans do cover the preventive medicine CPT codes in addition to Medicare wellness visits. However, a Medicare wellness visit and a preventive visit should not be billed on the same date of service. Medicare developed the Initial Preventive Physical Examination (IPPE, also known as the “Welcome to Medicare” visit) (G0402) and initial and subsequent annual wellness visits (G0438 and G0439) to encourage Medicare patients to receive screenings and preventive care, and to work with their physicians to develop a personalized prevention plan.1 The requirements are slightly different for the three codes, but in general they require collecting or updating medical, family, and social history; screening for depression; evaluating the patient's ability to perform activities of daily living; assessing the patient's safety at home; recording vital signs; asking about opioid and substance use; and providing guidance about preventive services and a personalized prevention plan (for more details, see the table in “Medicare 101: Navigating the Rules for Coverage and Benefits in Clinical Practice”). Similar to CPT's preventive medicine visits, Medicare wellness visits do not require a full head-to-toe physical exam.
The assessment and management of acute or chronic problems are not components of the IPPE or annual wellness visits. When that service is medically necessary during a Medicare wellness visit, the physician can also bill for a problem-oriented E/M office visit on the same day, again using the appropriate CPT code (99202-99215) with modifier 25.
SELECTING THE LEVEL OF SERVICE FOR THE E/M CODE
Hopefully you're now familiar with the E/M coding rules that changed in 2021.2 Performing a problem-oriented E/M service on the same date as a wellness visit adds a layer of complexity when it comes to choosing the level of service for the E/M code. But, as mentioned, the new rules actually make it easier than it was before.
When selecting a code (99202-99215) using the new E/M guidelines for office and outpatient services, physicians may use either total time on the date of the visit or MDM. History and exam are no longer necessary to select the level of service (though they should still be documented to provide the best care). This makes it easier to select a level of service for the problem-oriented visit when it's combined with a wellness or preventive visit because there are fewer overlapping components when coding based on MDM. The E/M service is your assessment and management of an acute or chronic condition, which is not required in either CPT preventive services or Medicare wellness visits.
It's trickier to code the E/M service based on time because you must make sure to only count the time spent managing the problems, not the time spent on the preventive or wellness service. The February 2021 CPT Assistant newsletter was particularly clear on this, stating “if time is used for selection of a level of the office/outpatient E/M code, the time spent on the preventive service cannot be counted toward the time of the work of the problem assessment because time spent performing a service cannot be counted twice. The code for the problem-assessment portion of the encounter will likely be selected based on MDM.”3 It might make sense to consider MDM-based coding as the best practice when combining E/M visits with wellness visits.
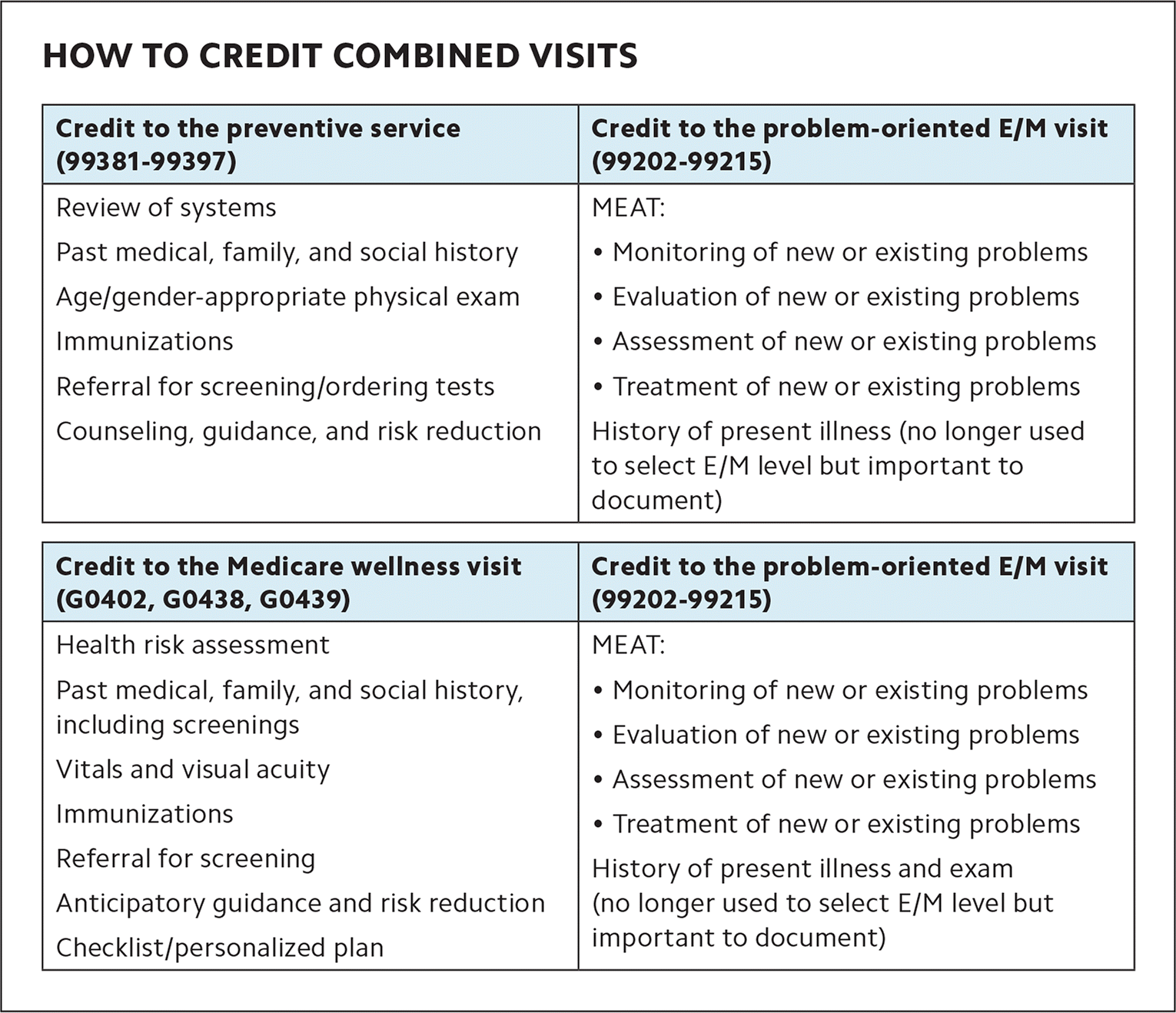
A problem-oriented visit includes the history of the problem and any symptoms or complaints related to it. It may or may not include a physical exam or data review (e.g., notes reviewed, tests ordered, tests reviewed, or independent historian). It includes the evaluation and management of a problem or condition. When these components are documented in addition to the preventive visit, add a problem-oriented visit code. For more on which components are required for which visits, see “How to credit combined visits.”
HOW TO CREDIT COMBINED VISITS
| Credit to the preventive service (99381-99397) | Credit to the problem-oriented E/M visit(99202-99215) |
| Review of systems Past medical, family, and social history Age/gender-appropriate physical exam Immunizations Referral for screening/ordering tests Counseling, guidance, and risk reduction | MEAT:
History of present illness (no longer used to select E/M level but important to document) |
| Credit to the Medicare wellness visit (G0402, G0438, G0439) | Credit to the problem-oriented E/M visit(99202-99215) |
| Health risk assessment Past medical, family, and social history, including screenings Vitals and visual acuity Immunizations Referral for screening Anticipatory guidance and risk reduction Checklist/personalized plan | MEAT:
History of present illness and exam (no longer used to select E/M level but important to document) |
EXAMPLES
Let's look at some examples of when it would be appropriate to bill for a problem-oriented E/M code (CPT 99202-99215) along with a preventive or wellness visit.
Patient 1: A 70-year-old male, established patient with a history of diabetes and hyperlipidemia comes in for a Medicare annual wellness visit. All required components of the wellness visit are completed. The patient then asks for a refill of his diabetes medication. The physician asks the patient if he is taking his medication as prescribed and following the diet recommendations discussed during the last visit. The physician also performs a focused physical exam, discusses medication management for diabetes and hyperlipidemia, and orders maintenance labs. The physician documents her significant review of the patient's problems, bills for the annual wellness visit with code G0439, and adds a 99214 E/M code because she addressed two stable chronic illnesses and performed prescription drug management. She adds modifier 25 to the E/M code.
Patient 2: A 32-year-old female, new patient comes in for a preventive medicine visit required by her employer. The physician completes all requirements for the preventive visit. During the history portion, the patient tells the physician that she has been having some knee pain exacerbated by running. The physician obtains additional history about the pain, examines her knee, tells her to reduce her running until the pain subsides, and gives her a handout on knee exercises. He also recommends she try a knee brace and follow up if the pain does not lessen with rest. The physician documents the extra work done to address the knee issue, then bills code 99385 for an initial preventive medicine visit for a patient age 18–39, along with E/M code 99203 because he addressed one acute, uncomplicated injury. He adds modifier 25 to the E/M code.
Patient 3: A 49-year-old female, established patient comes in for her annual preventive visit. The physician completes all requirements for the preventive visit. The patient then mentions she has been excessively tired recently and has been having trouble sleeping. The physician obtains a detailed history of the problems, does a thorough physical exam, and orders some labs (complete blood count and thyroid-stimulating hormone). The physician documents the extra work, then bills code 99396 for a periodic preventive medicine visit for a patient age 40–64 and E/M code 99213 for addressing two acute illnesses (fatigue and insomnia) and ordering two labs. The physician adds modifier 25 to the E/M code.
WORKFLOW TIPS
It's hard to plan for surprise problems that come up during a preventive or wellness visit. But your staff can help by asking patients up front if they have any other issues that need to be addressed. This step should occur when staff are scheduling or confirming patient visits, allowing you to block off more time if necessary.
Scheduling staff should also be aware that Medicare wellness visits have strict rules about how often they can be billed. They must be separated by at least 12 months from the previous wellness visit. Having staff check eligibility for Medicare wellness visits using the HIPAA Eligibility Transaction System can help you avoid denials.4 The timeframes for CPT preventive visits are more forgiving; they can be performed once every plan year (usually a calendar year, but some plans vary).
Patients who know their preventive/wellness visit will be covered with no deductible or co-pay may mistakenly assume all services provided during that visit, including E/M, will be no cost to them. It is best to educate patients on the costs associated with a problem-oriented office visit and let them know that performing one with a preventive or wellness visit will result in the same co-pay they would incur if the problem-oriented visit was on a different day. Most patients will accept this, because getting both visits in the same trip is more convenient for them. Posting flyers in the exam rooms or waiting room about the difference between preventive/wellness visits and problem-oriented visits, and the costs associated with each, can also prevent patient dissatisfaction.
Physicians could ask these patients to return for the problem-oriented visit on another day, but if time allows for providing both services at the current visit, it is only fair and reasonable to do so. Knowing the rules for combined visits, and the convenience they offer patients, should give physicians the confidence to bill fully for their services.

