From wellness visits to opting out, here are nine commonly asked questions about Medicare.

Medicare, the federal health insurance program established in 1965, serves more than 60 million Americans and made up 21% of total national health expenditures in 2019.1 It is one of the main players in U.S. health policy, supporting a range of efforts to reform payment models and delivery systems. Yet Medicare can leave physicians confused and frustrated about how to deliver high-quality care while adhering to its many rules. This article answers common questions physicians face in navigating patients' Medicare coverage and benefits.
KEY POINTS
- The components of the Welcome to Medicare visit, the initial annual wellness visit, and subsequent annual wellness visits can be confusing; see the table of requirements.
- If you provide other medically necessary services on the same date as a Medicare wellness visit, you can bill for them separately, but explain to patients why you recommend these services and what the out-of-pocket costs are likely to be.
- Physicians who opt out of Medicare are not prevented from seeing Medicare patients, but neither they nor the patient can bill Medicare for what would otherwise be a covered service.
WHO IS ELIGIBLE FOR MEDICARE?
Eligibility criteria for patients to enroll in Medicare include being 65 or older, receiving at least 24 months of Social Security Disability Insurance benefits or certain Railroad Retirement Board disability benefits, or having specific qualifying conditions such as amyotrophic lateral sclerosis and end-stage renal disease requiring dialysis or a kidney transplant. To enroll in Medicare, an individual must also be either a U.S. citizen, a lawfully present non-citizen with enough work credits to qualify for premium-free Part A, or a lawful permanent resident (green card holder) with five years of continuous residence in the U.S. immediately prior to Medicare enrollment. Individuals who are not lawfully present (undocumented) are ineligible to receive Medicare coverage.
Adults who begin collecting Social Security before they turn 65 are automatically enrolled in Medicare Parts A and B once they meet one of these eligibility criteria. Those who have not yet started collecting Social Security will need to take steps to enroll in Medicare once they are eligible.2
WHAT IS THE DIFFERENCE BETWEEN PARTS A, B, C, AND D?
Medicare Part A covers inpatient hospital care, skilled nursing facility services, and long-term care hospitals. Medicare Part B services are primarily delivered in the out-patient setting and encompass preventive medicine and the “medically necessary services” needed to diagnose or treat medical conditions. Parts A and B make up original (or traditional) Medicare.
Patients can also elect to enroll in a Medicare Advantage plan, Part C. These plans are offered by private companies that receive a fixed payment per month from Medicare for beneficiaries' care. Medicare Advantage plans offer all the same coverage for services as original Medicare but may have different rules for things like out-of-network services, out-of-pocket costs, and referrals. They may also offer additional benefits, such as vision, hearing, dental, or health and wellness programs. Some Medicare Advantage plans also cover preventive medicine visits (CPT codes 99381-99397), while traditional Medicare does not. Most Medicare Advantage plans include Medicare prescription drug coverage, Part D.
Patients who are uncertain about which type of Medicare they have can check their enrollment status and coverage at https://www.mymedicare.gov.
WHAT IS A “WELCOME TO MEDICARE” VISIT?
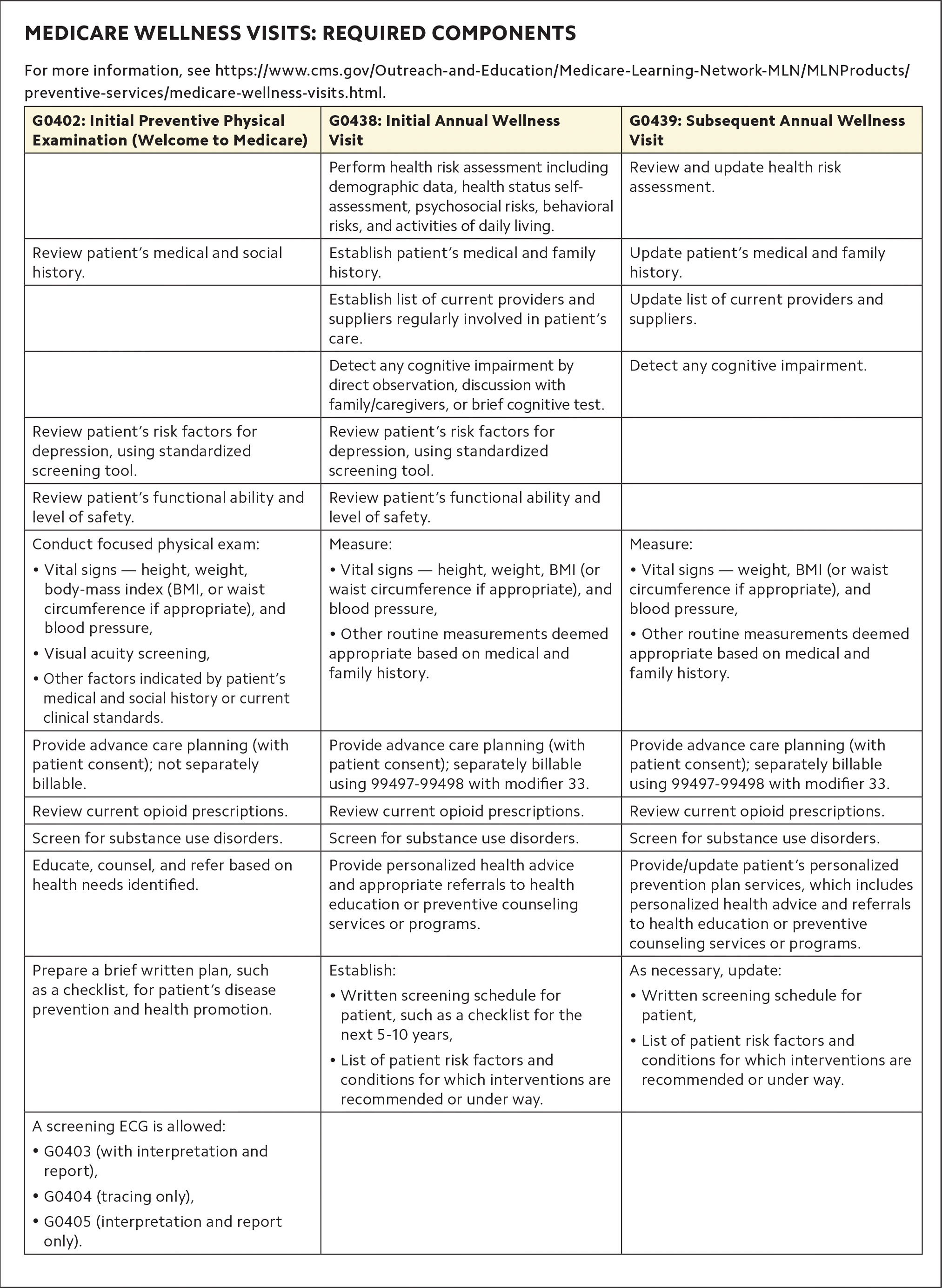
Patients with Medicare Part B are entitled to a free “Welcome to Medicare” visit, also called an Initial Preventive Physical Examination (IPPE, code G0402), in their first 12 months of coverage. The goal of the IPPE is health promotion and disease detection, but it is not a comprehensive, head-to-toe physical exam. Specific elements of the visit are shown in the table below.
Many of the required steps can be completed using questionnaires administered by nursing staff during the visit. All appropriate health screenings and vital sign assessments must be documented during the visit for it be covered. After reviewing, screening, examining, and discussing the patient's health and health risk factors, clinicians should prepare a brief written plan for the patient's disease prevention and health promotion.3 This can include a checklist of appropriate screening tests and immunizations covered by Medicare Part B. The patient should be given a printed copy of this plan or have electronic access to it.
At this visit, Medicare also covers an electrocardiogram (ECG) if deemed appropriate by the clinician. It requires a separate code (G0403, G0404, or G0405), and this is the only time an ECG is covered as a screening by Medicare.
MEDICARE WELLNESS VISITS: REQUIRED COMPONENTS
| G0402: Initial Preventive Physical Examination (Welcome to Medicare) | G0438: Initial Annual Wellness Visit | G0439: Subsequent Annual Wellness Visit | ||
|---|---|---|---|---|
| Perform health risk assessment including demographic data, health status self-assessment, psychosocial risks, behavioral risks, and activities of daily living. | Review and update health risk assessment. | |||
| Review patient's medical and social history. | Establish patient's medical and family history. | Update patient's medical and family history. | ||
| Establish list of current providers and suppliers regularly involved in patient's care. | Update list of current providers and suppliers. | |||
| Detect any cognitive impairment by direct observation, discussion with family/caregivers, or brief cognitive test. | Detect any cognitive impairment. | |||
| Review patient's risk factors for depression, using standardized screening tool. | Review patient's risk factors for depression, using standardized screening tool. | |||
| Review patient's functional ability and level of safety. | Review patient's functional ability and level of safety. | |||
Conduct focused physical exam:
| Measure:
| Measure:
| ||
| Provide advance care planning (with patient consent); not separately billable. | Provide advance care planning (with patient consent); separately billable using 99497-99498 with modifier 33. | Provide advance care planning (with patient consent); separately billable using 99497-99498 with modifier 33. | ||
| Review current opioid prescriptions. | Review current opioid prescriptions. | Review current opioid prescriptions. | ||
| Screen for substance use disorders. | Screen for substance use disorders. | Screen for substance use disorders. | ||
| Educate, counsel, and refer based on health needs identified. | Provide personalized health advice and appropriate referrals to health education or preventive counseling services or programs. | Provide/update patient's personalized prevention plan services, which includes personalized health advice and referrals to health education or preventive counseling services or programs. | ||
| Prepare a brief written plan, such as a checklist, for patient's disease prevention and health promotion. | Establish:
| As necessary, update:
| ||
A screening ECG is allowed:
| ||||
WHAT IS AN “ANNUAL WELLNESS VISIT”?
After their first 12 months of coverage, or 12 months after their “Welcome to Medicare” visit, patients with Medicare Part B are entitled to an initial annual wellness visit (code G0438). Subsequent annual wellness visits (code G0439) may be provided every 12 months thereafter. These visits are not comprehensive, head-to-toe physical examinations. Specific elements of these visits are listed in the table above.
The goal of annual wellness visits is to develop or update a personalized prevention plan of services, including the following:
- A written preventive screening and services plan for the next 5–10 years based on recommendations from the U.S. Preventive Services Task Force and Advisory Committee on Immunization Practices, the patient's health risk assessment, health status, and screening history, and appropriate Medicare-covered preventive services,
- A list of patient-specific risk factors and conditions along with treatment options,
- Health education or preventive counseling (including weight loss, physical activity, smoking cessation, fall prevention, and nutrition).
A copy of the plan should be furnished to the patient, either in print or electronically, upon completion of the visit.
The visit can optionally include advance care planning discussions at the patient's discretion (separately billable using 99497-99498 with modifier 33). One notable difference from the Welcome to Medicare visit is that Medicare does not cover a screening ECG ordered or performed during an annual wellness visit.
Previous articles in FPM provide practical strategies for how to use team-based care6 to cover the long and sometimes confusing list of elements required for these visits.
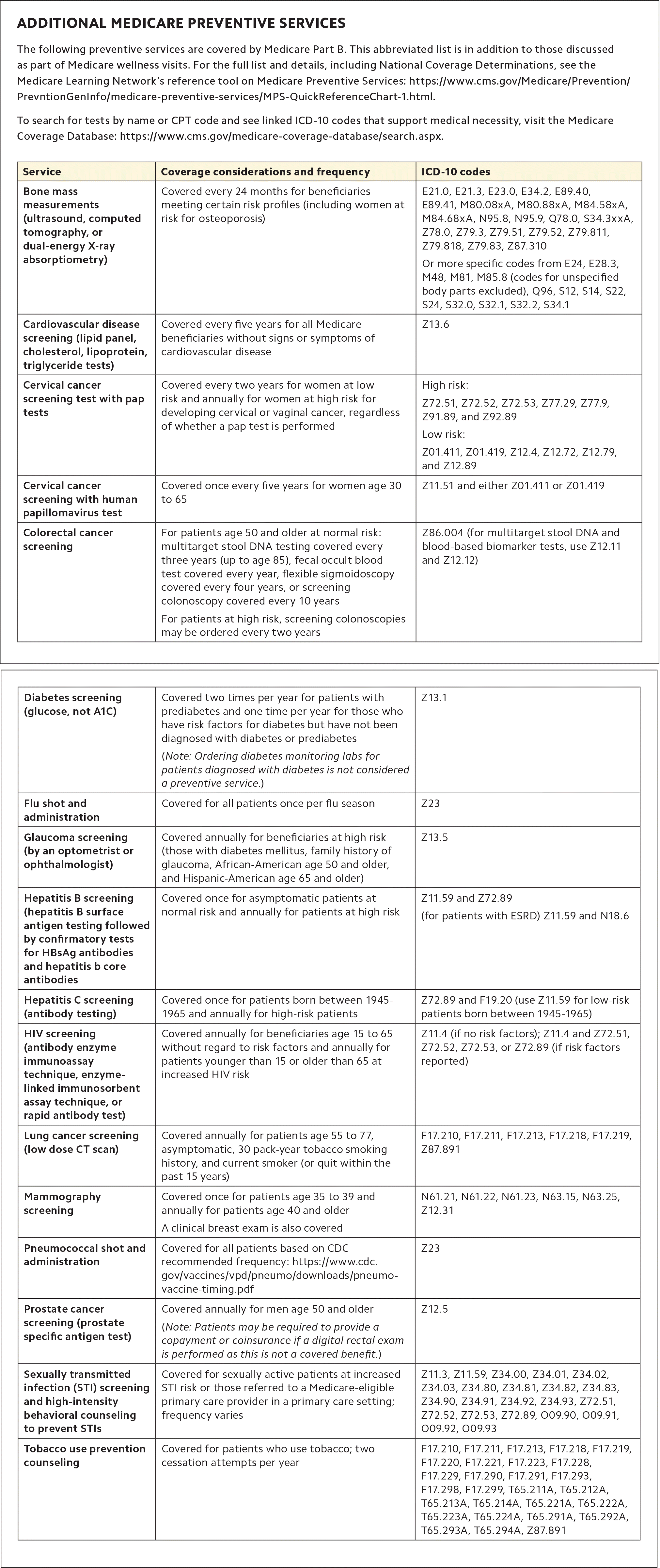
For a list of preventive services that can be included as part of Medicare wellness visits without additional cost to the patient, see the table below. The table also includes linked ICD-10 codes that support medical necessity.
ADDITIONAL MEDICARE PREVENTIVE SERVICES
To search for tests by name or CPT code and see linked ICD-10 codes that support medical necessity, visit the Medicare Coverage Database: https://www.cms.gov/medicare-coverage-database/search.aspx.
| Service | Coverage considerations and frequency | ICD-10 codes |
|---|---|---|
| Bone mass measurements (ultrasound, computed tomography, or dual-energy X-ray absorptiometry) | Covered every 24 months for beneficiaries meeting certain risk profiles (including women at risk for osteoporosis) | E21.0, E21.3, E23.0, E34.2, E89.40, E89.41, M80.08xA, M80.88xA, M84.58xA, M84.68xA, N95.8, N95.9, Q78.0, S34.3xxA, Z78.0, Z79.3, Z79.51, Z79.52, Z79.811, Z79.818, Z79.83, Z87.310 Or more specific codes from E24, E28.3, M48, M81, M85.8 (codes for unspecified body parts excluded), Q96, S12, S14, S22, S24, S32.0, S32.1, S32.2, S34.1 |
| Cardiovascular disease screening (lipid panel, cholesterol, lipoprotein, triglyceride tests) | Covered every five years for all Medicare beneficiaries without signs or symptoms of cardiovascular disease | Z13.6 |
| Cervical cancer screening test with pap tests | Covered every two years for women at low risk and annually for women at high risk for developing cervical or vaginal cancer, regardless of whether a pap test is performed | High risk: Z72.51, Z72.52, Z72.53, Z77.29, Z77.9, Z91.89, and Z92.89 Low risk: Z01.411, Z01.419, Z12.4, Z12.72, Z12.79, and Z12.89 |
| Cervical cancer screening with human papillomavirus test | Covered once every five years for women age 30 to 65 | Z11.51 and either Z01.411 or Z01.419 |
| Colorectal cancer screening | For patients age 50 and older at normal risk: multitarget stool DNA testing covered every three years (up to age 85), fecal occult blood test covered every year, flexible sigmoidoscopy covered every four years, or screening colonoscopy covered every 10 years For patients at high risk, screening colonoscopies may be ordered every two years | Z86.004 (for multitarget stool DNA and blood-based biomarker tests, use Z12.11 and Z12.12) |
| Diabetes screening (glucose, not A1C) | Covered two times per year for patients with prediabetes and one time per year for those who have risk factors for diabetes but have not been diagnosed with diabetes or prediabetes (Note: Ordering diabetes monitoring labs for patients diagnosed with diabetes is not considered a preventive service.) | Z13.1 |
| Flu shot and administration | Covered for all patients once per flu season | Z23 |
| Glaucoma screening (by an optometrist or ophthalmologist) | Covered annually for beneficiaries at high risk (those with diabetes mellitus, family history of glaucoma, African-American age 50 and older, and Hispanic-American age 65 and older) | Z13.5 |
| Hepatitis B screening (hepatitis B surface antigen testing followed by confirmatory tests for HBsAg antibodies and hepatitis b core antibodies | Covered once for asymptomatic patients at normal risk and annually for patients at high risk | Z11.59 and Z72.89 (for patients with ESRD) Z11.59 and N18.6 |
| Hepatitis C screening (antibody testing) | Covered once for patients born between 1945–1965 and annually for high-risk patients | Z72.89 and F19.20 (use Z11.59 for low-risk patients born between 1945–1965) |
| HIV screening (antibody enzyme immunoassay technique, enzyme-linked immunosorbent assay technique, or rapid antibody test) | Covered annually for beneficiaries age 15 to 65 without regard to risk factors and annually for patients younger than 15 or older than 65 at increased HIV risk | Z11.4 (if no risk factors); Z11.4 and Z72.51, Z72.52, Z72.53, or Z72.89 (if risk factors reported) |
| Lung cancer screening (low dose CT scan) | Covered annually for patients age 55 to 77, asymptomatic, 30 pack-year tobacco smoking history, and current smoker (or quit within the past 15 years) | F17.210, F17.211, F17.213, F17.218, F17.219, Z87.891 |
| Mammography screening | Covered once for patients age 35 to 39 and annually for patients age 40 and older A clinical breast exam is also covered | N61.21, N61.22, N61.23, N63.15, N63.25, Z12.31 |
| Pneumococcal shot and administration | Covered for all patients based on CDC recommended frequency: https://www.cdc.gov/vaccines/vpd/pneumo/downloads/pneumo-vaccine-timing.pdf | Z23 |
| Prostate cancer screening (prostate specific antigen test) | Covered annually for men age 50 and older (Note: Patients may be required to provide a copayment or coinsurance if a digital rectal exam is performed as this is not a covered benefit.) | Z12.5 |
| Sexually transmitted infection (STI) screening and high-intensity behavioral counseling to prevent STIs | Covered for sexually active patients at increased STI risk or those referred to a Medicare-eligible primary care provider in a primary care setting; frequency varies | Z11.3, Z11.59, Z34.00, Z34.01, Z34.02, Z34.03, Z34.80, Z34.81, Z34.82, Z34.83, Z34.90, Z34.91, Z34.92, Z34.93, Z72.51, Z72.52, Z72.53, Z72.89, O09.90, O09.91, O09.92, O09.93 |
| Tobacco use prevention counseling | Covered for patients who use tobacco; two cessation attempts per year | F17.210, F17.211, F17.213, F17.218, F17.219, F17.220, F17.221, F17.223, F17.228, F17.229, F17.290, F17.291, F17.293, F17.298, F17.299, T65.211A, T65.212A, T65.213A, T65.214A, T65.221A, T65.222A, T65.223A, T65.224A, T65.291A, T65.292A, T65.293A, T65.294A, Z87.891 |
ARE OTHER SERVICES COVERED ON THE SAME DATE AS A MEDICARE WELLNESS VISIT?
If you provide other medically necessary services on the same date as an annual wellness visit or a Welcome to Medicare visit, you must bill for them separately using modifier 25 appended to the appropriate evaluation and management (E/M) code. The patient's deductible and coinsurance or copayment would apply for these other services (see https://www.medicare.gov/your-medicare-costs). Therefore, before proceeding, it's a best practice to explain to patients why you recommend these services and what they are likely to cost. (See the article “Combining a Wellness Visit With a Problem-Oriented Visit.”)
If you perform preventive services (e.g., a screening pap smear) during a Medicare annual wellness visit, they too are separately billable. In this example, you would use code Q0091 for the screening pap smear in a Medicare patient.
HOW DO I CONTACT MY MEDICARE ADMINISTRATIVE CONTRACTOR (MAC)?
There are seven MACs that service different regions of the country. To look up the MAC for your state, go to https://www.cms.gov/Medicare/Medicare-Contracting/FFSProvCustSvcGen/MAC-Website-List.
WHAT'S THE LATEST ON MEDICARE COVERAGE FOR TELEHEALTH?
For the duration of the COVID-19 public health emergency, the Centers for Medicare & Medicaid Services (CMS) will pay for professional Medicare telehealth services furnished to beneficiaries in all areas of the country in all settings. These visits will be considered the same as in-person visits and paid at the same rate as regular in-person visits. Services covered include the Medicare annual wellness visit and Medicare preventive services. CMS continues to update a blanket list of waivers for the duration of the emergency (see https://www.cms.gov/files/document/summary-covid-19-emergency-declaration-waivers.pdf).
The 2022 Medicare Physician Fee Schedule final rule extended coverage for in-home tele-mental health services — including audio-only services — beyond the COVID-19 public health emergency. It also allows federally qualified health centers and rural health clinics to continue with telehealth after the public health emergency. But it did not provide the same extension to other types of telehealth.
HOW DOES A CLINICIAN OPT OUT OF MEDICARE?
Clinicians can individually choose not to accept Medicare insurance by opting out of Medicare. After opting out, clinicians set their own fees for the services they provide and are no longer able to submit claims to or receive payments from Medicare. This decision applies to all the settings where they practice. It does not prevent them from seeing patients with Medicare, but the physician and patient must enter into a private contract that prevents either side (including the health care system the physician works for) from submitting any claim to Medicare for what would otherwise be a covered service. Opted-out physicians and their patients may not receive payments under Medicare Advantage plans either.
A previous article in FPM provides practical steps for how to opt out and stay out of Medicare7 for clinicians who do not want to adhere to Medicare's complicated billing rules. Clinicians should keep in mind how opting out of Medicare will limit accessibility for patients who cannot afford to pay for services out of pocket.
Note that opting out differs from non-participating. Non-participating physicians may accept Medicare assignments on a claim-by-claim basis. They are paid 95% of the fee schedule amount by Medicare for assigned claims and can charge their Medicare patients up to the “limiting charge,” which is 115% of the Medicare-allowed amount for non-participating providers.
WHERE CAN CLINICIANS LOOK FOR ANSWERS TO OTHER QUESTIONS ABOUT MEDICARE?
Searching for answers about Medicare benefits and coverage is made more complicated by the number of different websites and sources intended for patients, clinicians, researchers, and policymakers. Here are three key resources for clinicians:
Keeping up with Medicare's changing policy landscape can seem like a daunting task to a busy clinician. Efficiently finding reliable resources to learn more about Medicare benefits can help clinicians meet their patients' health care needs.

