These strategies for recruiting and retaining staff can help medical practices survive the “Great Resignation.”

The struggle of medical staff retention and turnover is not new to many practices and health systems. Depending on the size of a practice, staff turnover as low 20%, in our experience, can disrupt the clinic, leading to workflow inefficiencies, adding stress to the remaining staff and clinicians, affecting patient care, and impeding team-based care and transformation efforts.1 The financial cost to replace staff members has been estimated at about 20% of their salary.2 Non-financial costs can include losses in quality, continuity of care,3,4 and time as practices train new staff members in clinic workflows, protocols, EHRs, and clinician expectations.
The staff turnover rate in many medical practices was already high pre-COVID-19. One cross-sectional analysis of 77 family medicine practices found a two-year turnover rate of 53% for staff (e.g., nurses, medical assistants, and office staff).5 The mass exit of employees during the COVID-19 pandemic, commonly referred to as the “Great Resignation,” has only made matters worse. As of late February 2022, only 22% of primary care practices reported being fully staffed, 52% reported having changed staffing ratios with fewer staff per clinician, and 68% reported having open positions they cannot fill.6
KEY POINTS
- Depending on the size of a practice, staff turnover as low 20% can disrupt the clinic, but many practices have a two-year staff turnover rate of more than 50%.
- Strategies to improve staff retention should focus on improving communication, practice environment, and the responsiveness of administration, as well as staff members' relationships, sense of control, sense of efficacy, and involvement with patients.
- Staff recruitment strategies should include offering competitive compensation, work-life benefits, and an expanded scope that allows staff to work at the top of their license.
WHY STAFF LEAVE
Staff members choose to leave their positions for a variety of reasons.5,7 Some staff leave for personal reasons. For example, they may want to pursue educational or professional opportunities, or they may have a personal expectation regarding the appropriate length of tenure at a specific position or location. Staff may also leave due to family reasons, housing costs, school districts, commute times, availability of public transportation, etc.
These departures are difficult for practices to prevent. However, many staff elect to leave for reasons directly related to their organization:
- A lack of career mobility within the organization (e.g., no promotion opportunities with adequate compensation increases),
- A lack of status given to staff compared with the status of clinicians or administrators, which can affect the dynamics of these working relationships and lead to poor team function and lower job satisfaction,
- Limited roles and responsibilities for medical staff,5 often below their training and abilities and usually blamed on system restrictions or state regulations regarding scope of practice.8
While burnout is frequently asserted as a cause of staff turnover, this association is not well-established in the literature. A longitudinal cohort study involving 740 primary care clinicians and staff in a health system found that burnout predicted clinician turnover but did not predict staff turnover.7 The study also found no association between staff engagement and turnover; however, it measured engagement narrowly, as “the likelihood that the respondent would recommend their clinic as a place to work.”
Competition for skilled workers from other employers, whether from the health care sector or other industries, also contributes to difficulties in retaining staff.
To gain additional insight into why employees leave, practices should consider implementing exit interviews.9
STRATEGIES FOR STAFF RETENTION
Competitive wages and benefits (including work-life benefits) are an important part of staff retention, especially in today's competitive work environment. However, raising wages isn't always possible and won't be effective alone.
To identify additional strategies for staff retention, practices should focus on factors that increase staff satisfaction.
In interviews with 30 medical assistants in nine primary care practices transforming into team-based care models, researchers identified four areas associated with staff fulfillment at work:10
- Relationships with colleagues (includes personal connections and psychological safety),
- Involvement with patients (includes increased continuity, patient appreciation, and patient disclosure of information),
- A sense of control over their work,
- A sense of efficacy (being able to do their jobs effectively).
A survey gauging staff and clinician engagement at a large academic family medicine department identified the following drivers of staff satisfaction:11
- Communication,
- Ability to give input,
- Being respected,
- A sense of trust/safety,
- A positive work environment,
- Responsiveness of administration.
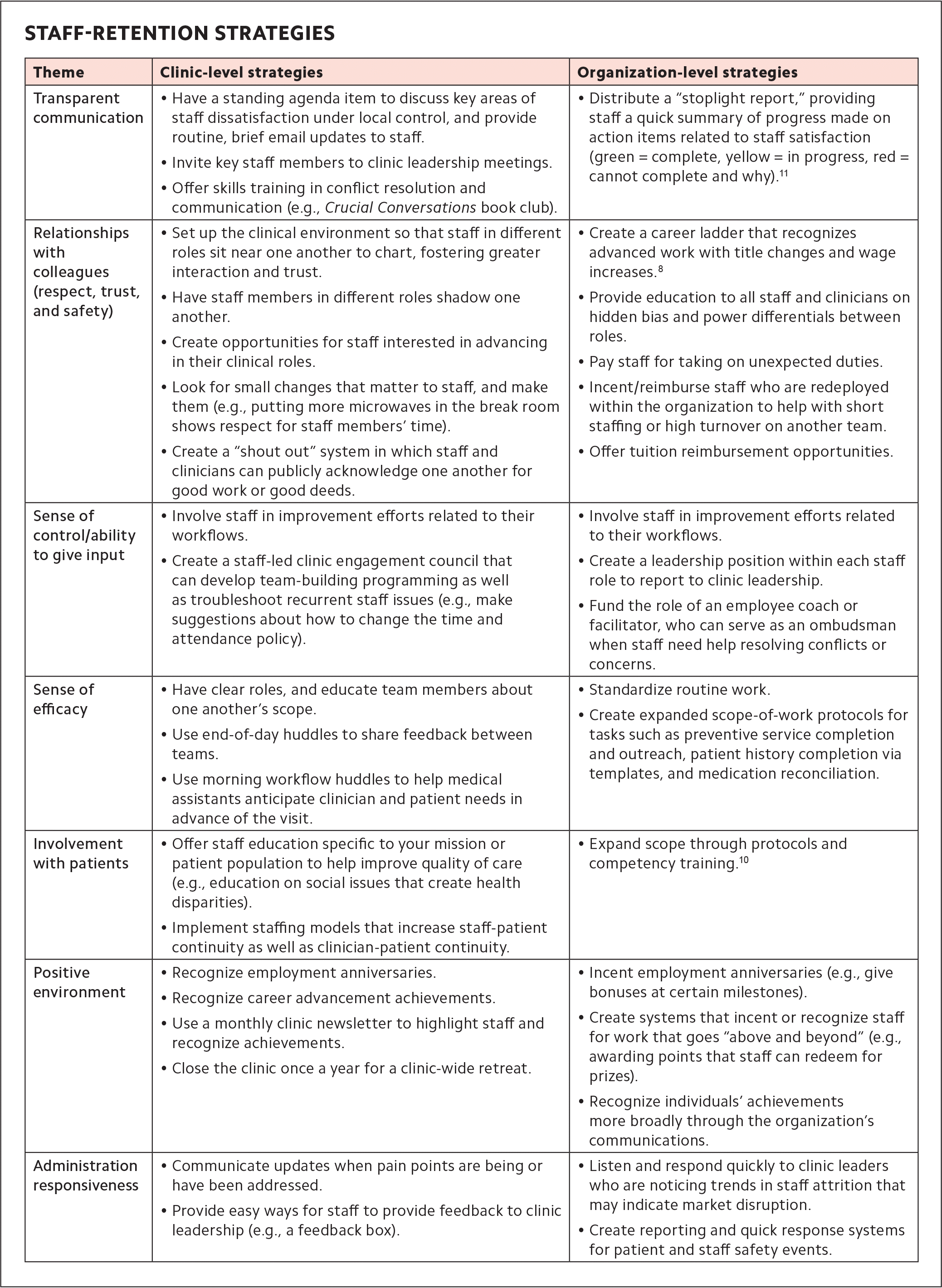
We have used these themes to identify specific, actionable strategies for staff retention. For example, under the theme “Sense of control/ability to give input,” possible strategies include the following:
- Involve staff in improvement efforts related to their workflows,
- Create a staff-led clinic engagement council that can create team-building programs as well as troubleshoot recurrent staff issues (e.g., make suggestions about how to change the time and attendance policy).
See the full list of staff-retention strategies.
Practices should also routinely survey staff to gauge satisfaction. Consider following up on surveys with staff focus groups to better understand the data. Then, use clinic-wide or department-level meetings to collectively review the feedback and set priorities for improvement.11
STAFF-RETENTION STRATEGIES
| Theme | Clinic-level strategies | Organization-level strategies |
|---|---|---|
| Transparent communication |
|
|
| Relationships with colleagues (respect, trust, and safety) |
|
|
| Sense of control/ability to give input |
|
|
| Sense of efficacy |
|
|
| Involvement with patients |
|
|
| Positive environment |
|
|
| Administration responsiveness |
|
|
STRATEGIES FOR STAFF RECRUITMENT
Competition for highly qualified medical staff is strong, particularly in dense health care markets or geographic areas with limited medical staff training programs. The following strategies can help improve staff recruitment to primary care practices.
Offer an attractive employment package. As noted earlier, a competitive compensation and benefits package is certainly important in this job market, but what if a practice can't offer the highest wages in town? Offering desirable work-life benefits (such as adequate time off, flexible schedules, or remote work, if applicable to the position) and having a positive practice culture can aid recruitment. (See the related article “Creating a Positive Clinic Culture.”)
Offer an expanded scope. Having all staff members working at the top of their license is associated with improvements in quality and experience for patients, staff, and clinicians.12–14 Offering an expanded scope, and including this information in job postings, can help practices attract high-quality applicants. Training for scope expansion is usually provided by the primary care clinic or health system after a hiring decision has been made. For some roles (such as medical assistants in family medicine), this additional on-the-job training can be time-consuming and labor intensive for the practice, particularly at times of staff growth or turnover. Within our system, we've removed this additional training from the clinical environment and created a centralized MA Academy. Doing so reduced the in-clinic training time for medical assistants from nine weeks to two weeks, lightening the training burden on practice staff.
Ask for referrals. Let your staff, colleagues, and other professional contacts know that you are hiring, and ask them to refer strong candidates to you. You can even consider providing a bonus to staff when someone they referred gets the job and stays for at least six months.
Create centralized ambulatory hiring within a health care system. In this model, staff apply and are hired to a job position within the organization, but they are not assigned to a specific clinic until they undergo additional training and are deemed appropriate for a high-scope position.
Partner with local medical staff training organizations. Serving as a clinical training site for these organizations can become a way to screen potential future applicants while acclimating them to the expectations and culture of your individual practice.
WHERE TO START
There are many reasons why clinic staff choose to stay or leave. Some reasons are personal and beyond the practice's control, but other reasons are directly related to the organization and deserve its attention. Understanding key drivers of staff satisfaction can help practices develop strategies to help with retention. Actionable strategies that improve practice communication, practice environment, and the responsiveness of administration, as well as improve staff members' relationships, sense of control, sense of efficacy, and involvement with patients, can be helpful places to start.

