Electronic messaging has the potential to improve care and strengthen patient relationships, but without clear expectations and boundaries, it also has the potential to erode work-life balance for clinicians.

Patient electronic messaging refers to the mode of secure communication that generally takes place via HIPAA-compliant, confidential, web-based communication platforms connected to electronic health records (EHRs). Patients, physicians, staff, or other providers can initiate messages anywhere internet access is available. The COVID-19 pandemic dramatically increased the number of patient electronic messages and the number of new users.1 In our health care system, from March 2020 to 2022, unique users of electronic messaging increased from approximately one in four patients to one in three. We also saw a doubling of total individual patient-initiated electronic messages, from approximately 11,000 to 22,000 per month in a system of 70,000 patients.
Although electronic messaging is the fastest-growing mode of patient communication, satisfaction with the technology varies. According to a retrospective analysis of 5,971 patients and 267 clinicians in 16 clinics in northern California, patients were extremely satisfied with electronic messaging, but physicians and staff were only generally satisfied even though electronic messages are associated with reductions in telephone call volumes,2 improvements in patient outcomes,3 and increases in overall patient satisfaction.4 Patients who use messaging most frequently have higher numbers of complex chronic diagnoses and more outpatient visits.5 As demand for timely electronic communication increases, intentional management strategies are becoming essential for clinicians. Message utilization has tremendous potential to improve care and strengthen patient-clinician relationships. However, it also has the potential to erode work-life balance for clinicians.6
With this in mind, we have reviewed and identified current best practices for electronic message management. These 12 practical tips are not meant to be taken as inflexible rules. We recognize there will be clinical exceptions; however, we hope these tips will empower primary care physicians and care teams to review and improve their patient electronic messaging habits. The overall goals are improved communication, effective teamwork, efficient workflow, and patient and clinical team satisfaction.
KEY POINTS
- Electronic messaging has the potential to improve patient outcomes and strengthen the patient-clinician relationship; however, it also has the potential to erode work-life balance for clinicians.
- Efficient message management starts with establishing team expectations for common message types and following best practices, such as using standardized text templates and keeping responses brief.
- Setting boundaries around electronic messaging helps patients understand when this mode of communication is most appropriate and when a face-to-face or other type of visit is needed.
1. ROUTE MESSAGES THROUGH CLINICAL TEAM MEMBERS
While it is tempting for physicians to have initial direct access to all patient messages and contacts, message management is more efficient as a team effort utilizing staff support as much as possible. Many messages can be handled independently by support staff following standardized orders and workflows, thereby decreasing the number of messages clinicians must handle. This can help improve the timeliness of responses to patients and allows clinicians to focus on essential or higher acuity tasks. For messages that require physician input, staff can at least do the initial information gathering and then carry out the physician’s instructions.
If the default in your EHR system is to route all messages through you, the physician, talk to your IT staff or vendor about changing this configuration so that messages are first routed to your clinical team members.
2. ESTABLISH TEAM EXPECTATIONS FOR COMMON MESSAGE TYPES
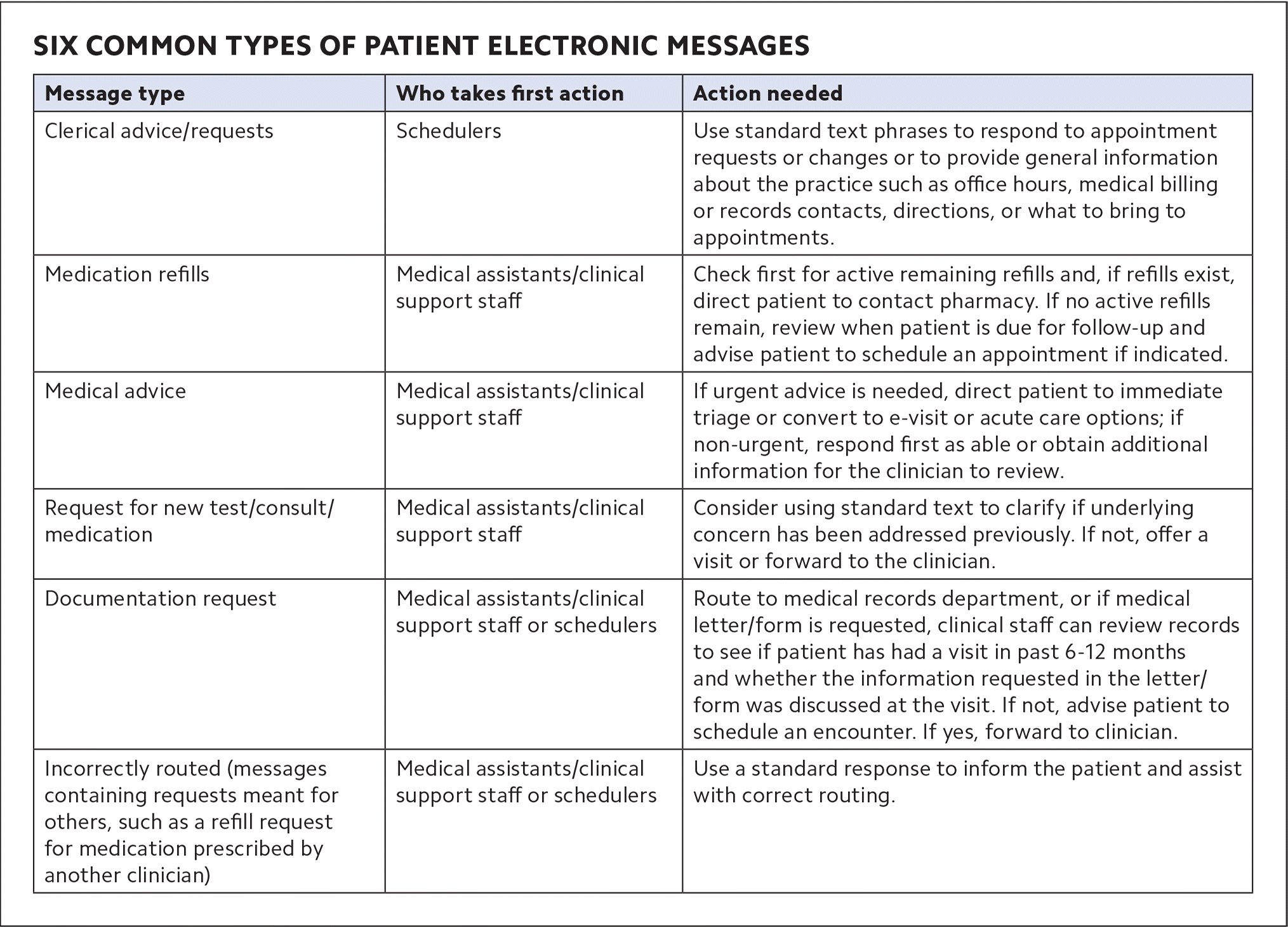
Care teams should proactively review the most common message types and create clear expectations as to how to manage each scenario. (See “Six common types of patient electronic messages.”) For example, for medication refill requests, medical assistants can first check for active remaining refills and, if they exist, direct patients to contact their pharmacy. If no active refills remain, medical assistants can review when follow-up is due and advise the patient to schedule an appointment if indicated.
Practices can benefit from designating a physician to provide message management training to new staff and clinicians regarding recommended workflows as well as standardizing text templates for the most common message types. Additionally, teams should anticipate and encourage converting electronic communication to e-visits such as telephone or video appointments when clinically appropriate. This approach may provide better quality of care that is patient-centered and may better capture the workload.
SIX COMMON TYPES OF PATIENT ELECTRONIC MESSAGES
| Message type | Who takes first action | Action needed |
|---|---|---|
| Clerical advice/requests | Schedulers | Use standard text phrases to respond to appointment requests or changes or to provide general information about the practice such as office hours, medical billing or records contacts, directions, or what to bring to appointments. |
| Medication refills | Medical assistants/clinical support staff | Check first for active remaining refills and, if refills exist, direct patient to contact pharmacy. If no active refills remain, review when patient is due for follow-up and advise patient to schedule an appointment if indicated. |
| Medical advice | Medical assistants/clinical support staff | If urgent advice is needed, direct patient to immediate triage or convert to e-visit or acute care options; if non-urgent, respond first as able or obtain additional information for the clinician to review. |
| Request for new test/consult/medication | Medical assistants/clinical support staff | Consider using standard text to clarify if underlying concern has been addressed previously. If not, offer a visit or forward to the clinician. |
| Documentation request | Medical assistants/clinical support staff or schedulers | Route to medical records department, or if medical letter/form is requested, clinical staff can review records to see if patient has had a visit in past 6–12 months and whether the information requested in the letter/form was discussed at the visit. If not, advise patient to schedule an encounter. If yes, forward to clinician. |
| Incorrectly routed (messages containing requests meant for others, such as a refill request for medication prescribed by another clinician) | Medical assistants/clinical support staff or schedulers | Use a standard response to inform the patient and assist with correct routing. |
3. KEEP RESPONSES BRIEF — 1–3 SENTENCES AT MOST
Use dot phrases or auto-text to quickly insert a standard, friendly, personalized greeting and professional closure. Then, get straight to the core information. Aim for a body of 1–3 sentences maximum. When it comes to health care communications, less is usually more meaningful for you and the patient. Save longer narratives or anticipatory guidance for synchronous encounters. If you notice yourself or team members delving into longer narratives, consider it an opportunity to convert the encounter to another mode of communication, such as telehealth or a face-to-face visit.
4. ASK FOR CLARIFICATION
If your initial impression of the request is unclear, send a brief immediate reply asking the patient to clarify or provide more information. For example, “Greetings. Thanks for your message. Please send more information about your request for blood tests and ENT referral so that we may better help you.” Avoid spending extra time extrapolating or responding to different possible scenarios.
5. DO NOT START A MEDICATION VIA MESSAGING THAT YOU HAVE NEVER PRESCRIBED FOR THE REQUESTING PATIENT
As a general rule, it is not a good idea to begin new medications that have never been prescribed to the patient without a thorough evaluation (e.g., reviewing interactions and providing anticipatory guidance about potential side effects). New medications are rarely able to be thoughtfully initiated with patient electronic messaging and deserve a documented synchronous encounter. Enforcing proper use and adherence or upholding antimicrobial stewardship when responding to a new prescription request is much more challenging via message. There may be a few exceptions, including over-the-counter medications or very low-risk medications such as topicals; however, in general, when you are considering a new medicine, encourage the patient to use another care modality.
6. DO NOT BEGIN A NEW WORKUP VIA MESSAGING FOR A PROBLEM YOU HAVE NEVER ADDRESSED
We do not recommend using patient electronic messaging alone to order diagnostic tests for a new problem for which you have never seen the patient. Messaging often does not allow for the same level of thoroughness and communication that synchronous care allows. When diagnostic decisions are made without obtaining a complete history or performing or documenting exam findings, important aspects of care can be missed. This may result in excess or incorrect test orders. It is important to keep in mind that care delivery via electronic methods can be reviewed for appropriateness by medical-legal review. In the end, if a new workup is planned, including new radiology or lab tests, it is best to complete a synchronous visit.
7. ESTABLISH A COVERAGE PLAN
All clinicians need to have a coverage plan for patient electronic messages when they are away from the office. Ideally, health care systems would incentivize message coverage. A coverage plan ensures timely responses, which strengthens messaging rapport as well as patient satisfaction. It also helps clinicians avoid a pileup of messages upon return to work. Coverage plans should apply to all members of the care team engaging in messaging, including support staff.
8. ENCOURAGE APPROPRIATE USE
Patient electronic messaging is an excellent platform for certain care items, but it is not well suited for all types of care. Health care systems and primary care teams will likely need to provide education to patients regarding the basics of patient electronic messaging use:
- Messages are for refills and simple health-related questions,
- Messages are not for urgent or serious medical issues,
- Messages are part of the medical record and may be seen by anyone on the care team.
In addition, set clear expectations for response turnaround time. In our system, the expected response time is within three business days.
9. SET BOUNDARIES
Patients who use electronic messaging are typically well-meaning and are seeking a cost- and time-effective answer to a clinical concern. However, they may reach out with requests that are not managed best via electronic messaging. Clinicians and staff must learn to recognize when these requests are inappropriate and set clear boundaries. For example, for patients with unstable mental health or substance abuse concerns, let them know your team welcomes them to use electronic messaging for general health concerns but not to address acutely unstable issues. Once you have provided clear expectations and documented reminders, if the patient continues to send inappropriate messages, consider letting the patient know your team will not respond to them.
10. USE ELECTRONIC MESSAGING FOR TEST RESULTS
For non-critical test results, consider using patient electronic messaging instead of mailing paper results. This typically saves time for staff and postage costs for practices. It also results in faster communication and action. Patients appreciate having electronic access to results. In some chart systems, patients have almost immediate access to results, so sending communication with your interpretation can help preempt questions and facilitate patient education. Keep in mind that for any critical alert, such as a positive cancer screening, ensuring receipt of communication is critical. Electronic messaging systems may or may not be able to effectively track receipt. Therefore, for critical results, it is best to first use synchronous modes of communication, such as phone calls, then consider options that can track patient receipt, such as certified mail.
11. SEEK WORKLOAD CREDIT
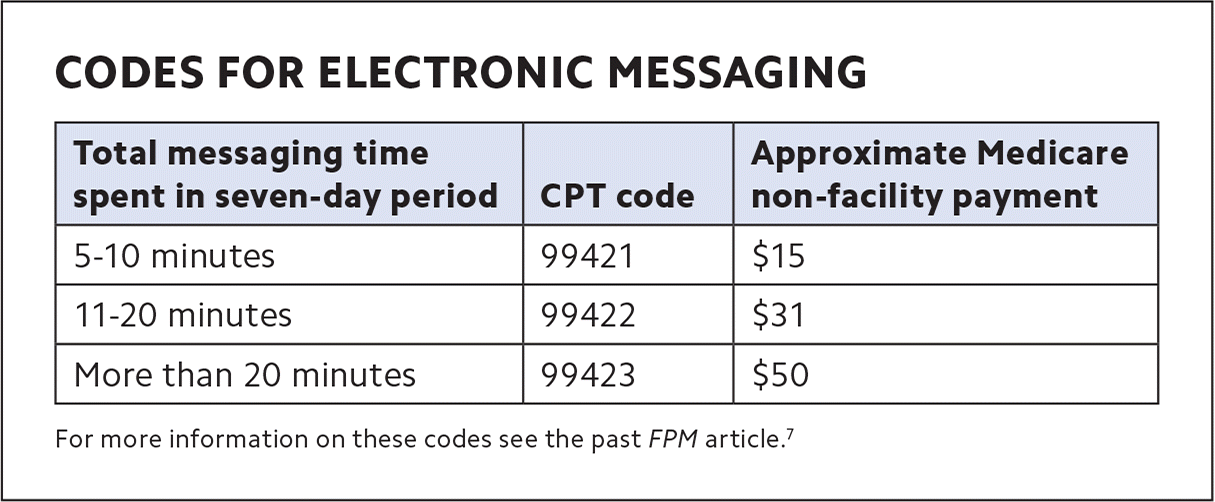
Many clinicians and teams are not receiving workload credit for electronic messaging with patients. If your electronic system tracks workload or other work units, inquire whether your messaging workload can also be tracked. Consider using CPT codes for messages. The 2020 E/M update included CPT codes that may be billed by clinicians responding to patient-initiated electronic messages based on total time spent in a seven-day period as long as there is no synchronous encounter billed during the same period.7 Consult with your practice management, billing, and technology experts to ensure encounter types and CPT codes are realized and submitted. Your billing staff may need to review local insurance requirements to determine whether and how these claims should be submitted.
CODES FOR ELECTRONIC MESSAGING
| Total messaging time spent in seven-day period | CPT code | Approximate Medicare non-facility payment |
|---|---|---|
| 5–10 minutes | 99421 | $15 |
| 11–20 minutes | 99422 | $31 |
| More than 20 minutes | 99423 | $50 |
12. ENCOURAGE USE OF ELECTRONIC MESSAGING
Practices may encourage utilization of electronic messaging in many ways. First, make it easy for patients to register for electronic messaging while waiting at your office by offering easily accessible guest Wi-Fi and equipping waiting rooms with outlets and universal charging stations for portable devices. Display information in waiting areas and on the practice website about using electronic messaging. Consider using mass electronic communication to send announcements to patients about clinical offerings or public health concerns to enhance quality of care, including reminders about immunizations or important health screenings. Finally, educate new staff and clinicians about electronic messaging so they are comfortable using it with patients.
GUIDING TEAMS TO EFFECTIVE USE
The success of patient electronic messaging depends on its use and implementation by primary care teams. Given the increased message demand and utilization associated with the COVID-19 pandemic, there has never been a better time to consider implementing and improving message workflows. These 12 tips represent an approach to guiding teams to effectively utilize this growing care modality. More research is needed to determine how staffing models may adjust workload to support message growth in the future.
Although electronic messaging can have a positive impact on safety and quality of care,8 clinicians (who are rarely compensated for time spent on messaging) understandably display some ambivalence. We believe creating clear expectations around messaging, including recognizing its limitations, will help empower clinicians to effectively harness this modality to its maximum positive potential.

