Shifting from an individual physician in-basket to a team-based in-basket pool can reduce physician clerical work and restore joy in practice.

While electronic health records (EHRs) were originally touted as an efficiency tool to help ease practice for physicians, recent studies have linked the additional clerical work of EHRs with greater rates of physician burnout and dissatisfaction.1–4 With the rise of EHRs, many physicians have found that they spend more time charting and managing their personal in-basket than providing direct patient care. One study examining physician work activities during office hours found that physicians spend 27% of their time on direct clinical face time with patients and 49% of their time on EHR and desk work.5
To address this problem, many organizations have implemented team-based care models. However, for these models to succeed, they must include optimization of the EHR — specifically, to address physician in-basket volume. This article describes how our group converted from individual to team in-basket pools and achieved a significant reduction in physician in-basket work.
KEY POINTS
- Moving from an individual physician in-basket to a team-based in-basket pool helps teams filter the physician’s in-basket and call attention to only those messages in need of physician review.
- This approach resulted in a 93% reduction in clinicians’ total volume of ED/Hospital Summary and Care Coordination messages and a 62% reduction in Results Folder messages.
- Keys to success are team training, clear protocols, excellent communication, and clinician willingness to engage in the process.
HISTORY OF THE MODEL
Presbyterian Medical Group implemented the patient-centered medical home model (PCMH) in 2009 and, a year later, adopted the EHR, which had many positive outcomes but also shifted nonclinician work to clinicians. Prior to the EHR, the clinical, clerical, and clinician teams were able to carry out much of their work independent of one another. The EHR created interdependent workflows across the health care team that contributed to many inefficiencies. For example, the nursing team members depended on the physician to finalize orders in the system and route messages before they could complete their work. The physician’s response was also a rate-limiting step for the clerical team’s work related to referrals, follow-up messages, patient scheduling inquiries, etc. Many workflows depended on the physician to set the pace for the team and proved to be inefficient. When coupled with a busy practice, workflow dependency often resulted in batching of work, a backlog of messages, loss of productivity, and an inefficient practice style resulting in dissatisfaction for the physician, patient, and team. The increased volume of work in clinicians’ personal in-baskets also limited their time available for direct patient care.
To address this, our organization piloted “PCMH 2.0,” which expands the traditional team-based care model, shifting work to the right team member to be completed in real time and ensuring top of licensure performance for clinicians. Key elements of this approach include the following:
- Moving from an individual physician in-basket to a team-based in-basket pool, which filters the physician’s in-basket and calls attention to only those messages in need of physician review,
- Making workflow changes that leverage the skills of clinical support staff and utilize nursing-initiated protocols to more efficiently manage certain types of messages, such as laboratory and imaging results,
- Improving clinician documentation to make it more actionable so the clinical team can act on the physician’s documented care plan and complete the recommended next steps for patient management.
The initial two-clinician pilot at one clinic has expanded to include nine family medicine/internal medicine clinicians and four pediatric clinicians within the same clinic. We have also rolled out the model to another five-clinician family medicine clinic. Further roll-out has been on pause because our organization is in the process of changing our nursing skill levels, which will better utilize medical assistants (MAs).
While this optimization model does not eliminate in-basket work for physicians, it reduces the amount significantly.
HOW IT WORKS
The physician’s personal in-basket is comprised of several folders including Patient Calls, Rx Requests, Care Coordination, Care Messages, Cosign-Clinic Orders, ED/Hospital Summary, Results Folder, and Staff Messages. But with the incorporation of the team-based pool, physicians can now focus primarily on the top three folders in their personal in-basket: Patient Calls, Rx Requests, and Results Folder, all of which have already been filtered by their team.
High-volume and less critical folders, such as ED/Hospital Summary, Care Coordination, and Results Folder are largely managed by the team pool utilizing protocols. In our initial pilot, this approach resulted in a 93% reduction in clinicians’ total volume of ED/Hospital Summary and Care Coordination messages and a 62% reduction in Results Folder messages (see “In-basket reduction potential”). This was accomplished by filtering messages (e.g., normal results) out of the physician’s in-basket and addressing them through nurse-initiated protocols.
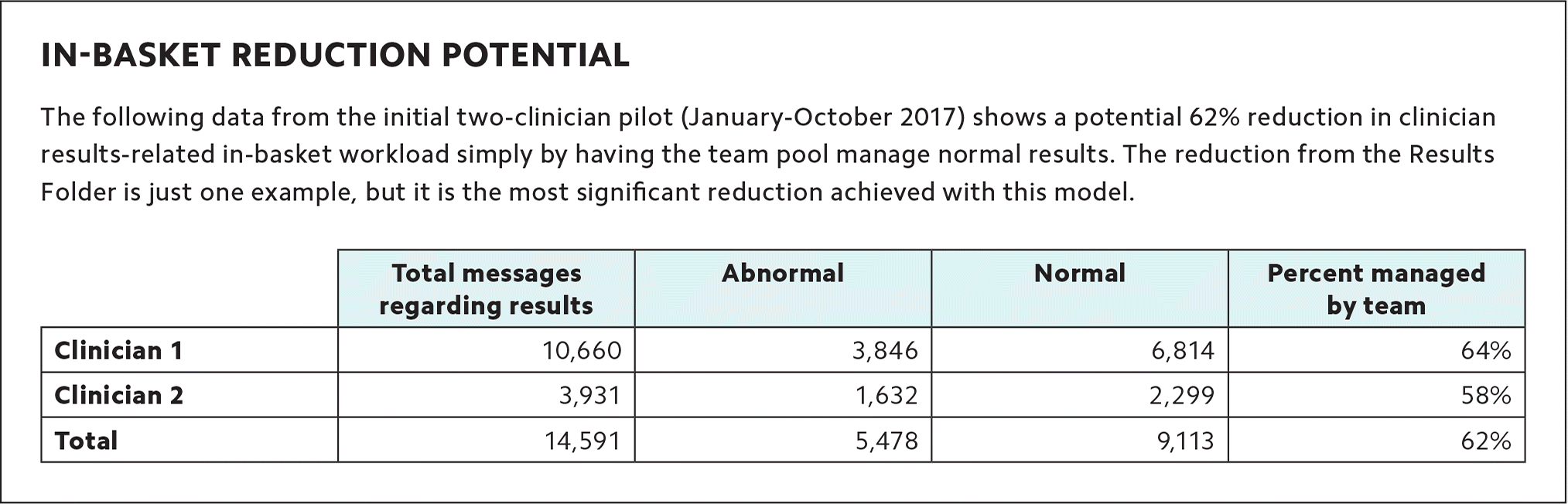
| Total messages regarding results | Abnormal | Normal | Percent managed by team | |
|---|---|---|---|---|
| Clinician 1 | 10,660 | 3,846 | 6,814 | 64% |
| Clinician 2 | 3,931 | 1,632 | 2,299 | 58% |
| Total | 14,591 | 5,478 | 9,113 | 62% |
Our team pools include the following clinical support staff (see the full list of their responsibilities):
- One MA or licensed practical nurse (LPN) per physician in a primary support role,
- One registered nurse (RN) per physician in a team nurse role,
- One RN for every two physicians in a care manager role.
The higher licensure and scope of practice of the RNs initially allowed them to address some messages our MAs couldn’t. However, more recently, our organization has expanded the scope of practice for MAs, allowing us to better leverage their role in this model. They too can now use protocols to manage messages in the team pool without having to consult the physician. The RNs are available to support the MAs and can now primarily focus on their specialized skill set of patient assessment, triage, and nurse visits.
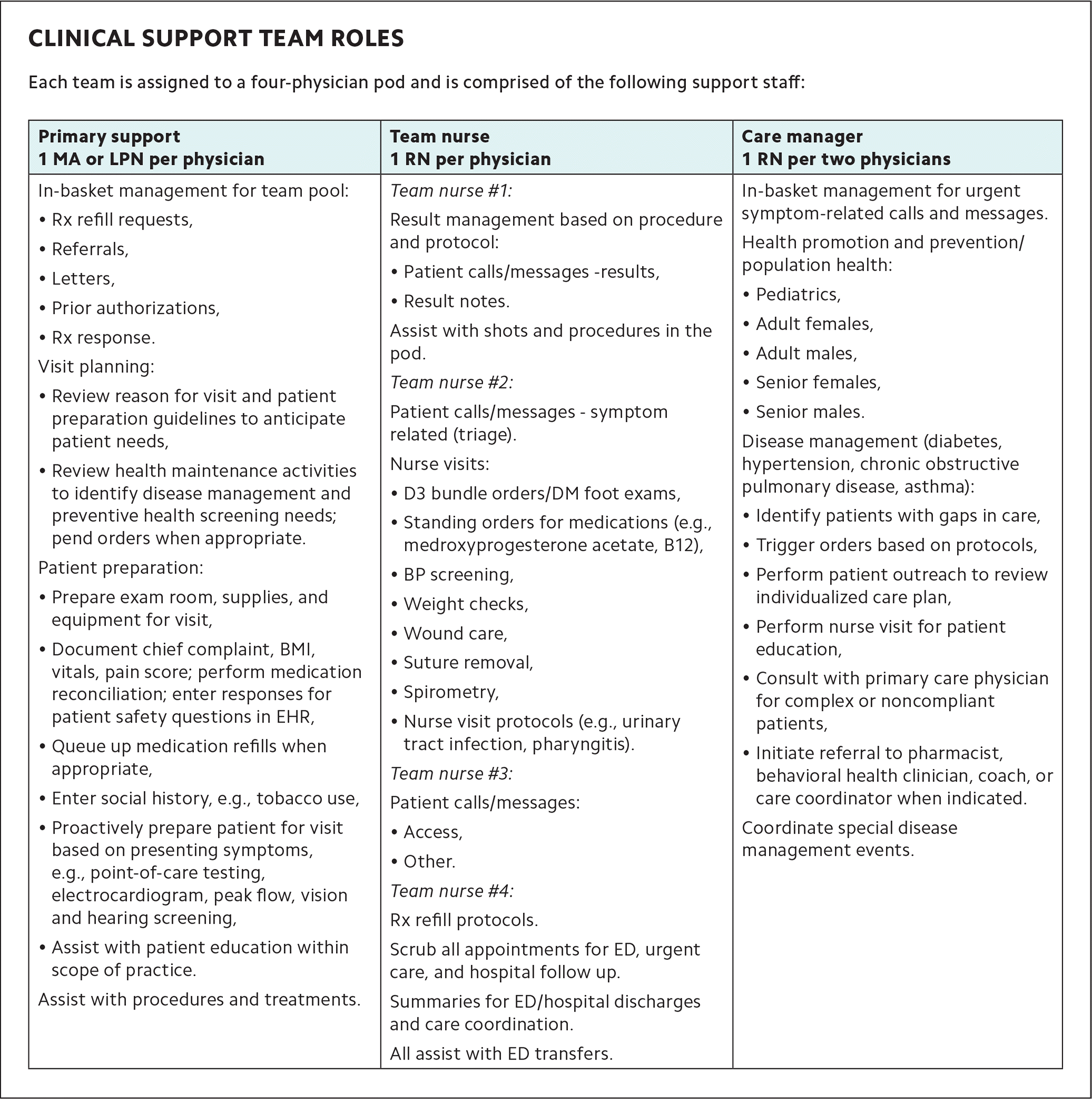
| Primary support 1 MA or LPN per physician | Team nurse 1 RN per physician | Care manager 1 RN per two physicians |
|---|---|---|
In-basket management for team pool:
Visit planning:
Patient preparation:
Assist with procedures and treatments. | Team nurse #1: Result management based on procedure and protocol:
Assist with shots and procedures in the pod. Team nurse #2: Patient calls/messages - symptom related (triage). Nurse visits:
Team nurse #3: Patient calls/messages:
Team nurse #4: Rx refill protocols. Scrub all appointments for ED, urgent care, and hospital follow up. Summaries for ED/hospital discharges and care coordination. All assist with ED transfers. | In-basket management for urgent symptom-related calls and messages. Health promotion and prevention/population health:
Disease management (diabetes, hypertension, chronic obstructive pulmonary disease, asthma):
Coordinate special disease management events. |
Focusing on actionable physician documentation has also helped save time and improve efficiency. With physicians clearly articulating their treatment planin their note, clinical staff can move forward with the next steps in patient care without needing to message the physician or wait for more instruction. For example, a physician can document the next steps in managing an abnormal thyroid stimulating hormone lab value, such as making a change to the current medication regimen or ordering future labs. This detailed charting allows the clinical team to proceed and act on the physician’s care plan.
Our team has noted several benefits of using this model, including the following:
- The ability to onboard/ramp up new physicians to a full schedule more quickly,
- The potential to achieve full productivity and come off of salary protection/guarantee,
- Improvements in worklife balance,
- Increased morale as staff are able to contribute to their highest level of licensure,
- Less chance for error as labs and messages follow the team pool, not an individual physician or other provider, who may leave, transfer, etc.,
- Improved coverage during times of lean staffing (e.g., during the COVID-19 pandemic) because the team pool approach is not person dependent,
- Greater overall efficiency.
THE SECRET SAUCE FOR SUCCESS
The success of our team-based in-basket pool model is based largely on the clinical support team’s ability to work together and divide the duties. This requires team training, clear protocols, and excellent communication via daily huddles, secure chat/EHR messaging, and frequent bi-directional physician-staff communication. Each RN specializes in an area (e.g., triage or result management); however, each can also rotate duties as needed.
Equally important to the model’s success is clinician willingness to engage in the process. Clinicians must be able to relinquish control of their personal in-basket and allow the nursing team to complete prescription refills, send normal lab letters, and coordinate care based on approved protocols. Physician engagement and consensus in development of clinical protocols is also important.
While transforming to a new practice style is certainly challenging for staff and clinicians, we believe it is worth the effort. For us, the efficiencies gained have led to greater joy in medicine.

