A step-by-step approach that saves time coding E/M office visits can now be tailored to hospital and nursing home E/M visits as well.

Following the major revisions to coding evaluation and management (E/M) office visits in 2021,1 a similar revamp has been made for coding E/M visits in other settings. Effective Jan. 1, 2023, the history and physical examination requirements have been eliminated for coding hospital and nursing home visits.2 As with office visits, hospital and nursing home coding is now based solely on medical decision making (MDM) or total time (except for emergency department visits, which must be coded based on MDM, and hospital discharge visits, which must be coded based on time). This further streamlines E/M coding, creating one unified set of rules for office, nursing home, and hospital visits.
Hospital and nursing home E/M visits are divided into three groups: initial services (i.e., admissions), subsequent services, and discharge services. According to the American Medical Association (AMA), initial visits are “when the patient has not received any professional services from the physician or other qualified health care professional or another physician or other qualified health care professional of the exact same specialty and subspecialty who belongs to the same group practice, during the inpatient, observation, or nursing facility admission and stay.”2 After the patient has received care from that group once, all other visits are subsequent until the discharge service. When the patient transitions from inpatient to observation, or vice versa, that does not begin a new stay eligible for an initial services visit.
CPT codes 99234-99236 are for patients admitted to the hospital and discharged on the same date. For patients with multi-day stays, use 99221-99223 for initial services, 99231-99233 for subsequent visits, and 99238-99239 for discharge services.
Initial nursing home visits are coded with 99304-99306. CPT is deleting the code for nursing home annual exams (99318), which will instead be coded as subsequent nursing home visits (99307-99310).
Two sets of observation care codes (99217-99220 and 99224-99226) should no longer be used as of Jan. 1. Observation services have instead been merged into the corresponding initial service, subsequent service, and discharge codes.
These changes open the door to a simpler, quicker coding process. Many of the principles that already apply to E/M office visit coding now apply to hospital and nursing home E/M coding, but there are some differences in the details. This short guide can help physicians navigate the changes.
KEY POINTS
- Coding for evaluation and management (E/M) visits in hospitals and nursing homes is now much like coding E/M office visits.
- This unified set of coding rules allows physicians to quickly code nearly all visits using a template that starts with total time.
- There are a few key differences to be aware of, such as total time spent past midnight on the date of service can be counted for hospital E/M visits, but not for office E/M visits.
MEDICAL DECISION MAKING
Determining the level of MDM for hospital and nursing home visits is now much like doing so for office visits.3 The four MDM levels are straightforward, low, moderate, and high. They are determined by three factors: the number and complexity of problems addressed, the amount and complexity of data reviewed, and the patient's risk of complications, morbidity, or mortality.
If you feel confident coding office visits based on MDM, you can use that knowledge to code hospital and nursing home visits based on MDM as follows:
- A level 1 initial or subsequent hospital visit requires the same MDM components as a level 3 office visit,
- A level 2 initial or subsequent hospital visit requires the same MDM components as a level 4 office visit,
- A level 3 initial or subsequent hospital visit requires the same MDM components as a level 5 office visit.
Several medical decisions that are more common in hospitals than office settings carry enough risk that, when paired with high-level problems, they call for the top visit level. These include the decision to escalate hospital care (e.g., transfer to the intensive care unit), the decision to deescalate care or discuss do-not-resuscitate orders due to poor prognosis, the decision to use IV narcotics or other drugs that require intensive monitoring, and decisions regarding emergency surgery for patients with or without risk factors or non-emergency surgery for patients with risk factors.
TOTAL TIME
There are new time thresholds for each level of service for initial hospital visits, subsequent hospital visits, and nursing home visits to use when you are coding by total time. Instead of offering a time range like office visits (e.g., a 99214 office visit requires 30–39 minutes), nursing home and hospital care visits require that you meet or exceed specific times (e.g., a 99232 subsequent hospital visit requires 35 or more minutes).
When coding initial hospital visits by total time, you can count all the time you spend caring for the patient on admission even if some of it extends after midnight on the calendar day of the admission. According to the AMA, “a continuous service that spans the transition of two calendar dates is a single service and is reported on one calendar date. If the service is continuous before and through midnight, all the time may be applied to the reported date of service.”3 This differs from office visits, for which you may count only the time on the date of the visit. Otherwise, the definition of total time for hospital and nursing home E/M visits is similar to that of office visits. It includes the time you personally spend on E/M for that patient before, during, and after the face-to-face services. It does not include staff time, time spent on separately reportable procedures, travel time, or teaching time.
A SIMPLER WAY TO CODE
Like the 2021 changes to office visit E/M coding, the 2023 changes should make coding hospital and nursing home E/M visits simpler and quicker.
The universal coding template suggests coding by time first if that will appropriately credit you for the work you did. It's the most straightforward and easy method. But if you believe MDM will credit you for a higher level of work, then step 2 is to determine what level of problems (low, moderate, or high) you addressed and whether you managed (prescribed, adjusted, or decided to keep the same) a prescription medication. Answering those two questions allows you to code most visits quickly using MDM. For the few visits that remain, you will need to proceed to steps 3 or 4, which may require you to tally data points and are therefore more time-consuming.
The template was adapted from a prior FPM article on office E/M coding4 by adding nursing home and hospital visit times and relabeling office-visit level 3, 4, and 5 problems as low-, moderate-, and high-level problems.
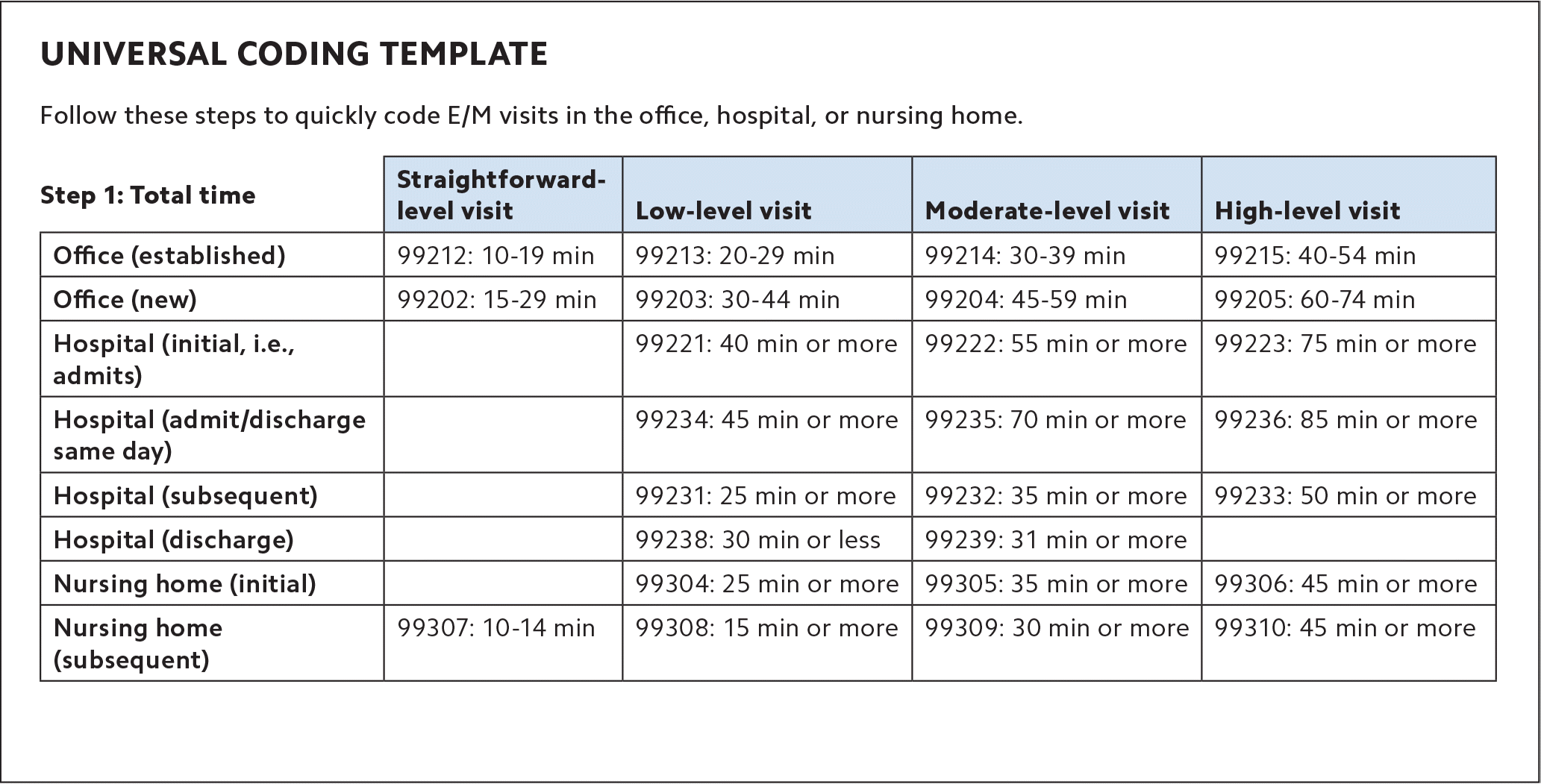
UNIVERSAL CODING TEMPLATE
| Straightforward-level visit | Low-level visit | Moderate-level visit | High-level visit | |
|---|---|---|---|---|
| Office (established) | 99212: 10–19 min | 99213: 20–29 min | 99214: 30–39 min | 99215: 40–54 min |
| Office (new) | 99202: 15–29 min | 99203: 30–44 min | 99204: 45–59 min | 99205: 60–74 min |
| Hospital (initial, i.e., admits) | 99221: 40 min or more | 99222: 55 min or more | 99223: 75 min or more | |
| Hospital (admit/discharge same day) | 99234: 45 min or more | 99235: 70 min or more | 99236: 85 min or more | |
| Hospital (subsequent) | 99231: 25 min or more | 99232: 35 min or more | 99233: 50 min or more | |
| Hospital (discharge) | 99238: 30 min or less | 99239: 31 min or more | ||
| Nursing home (initial) | 99304: 25 min or more | 99305: 35 min or more | 99306: 45 min or more | |
| Nursing home (subsequent) | 99307: 10–14 min | 99308: 15 min or more | 99309: 30 min or more | 99310: 45 min or more |
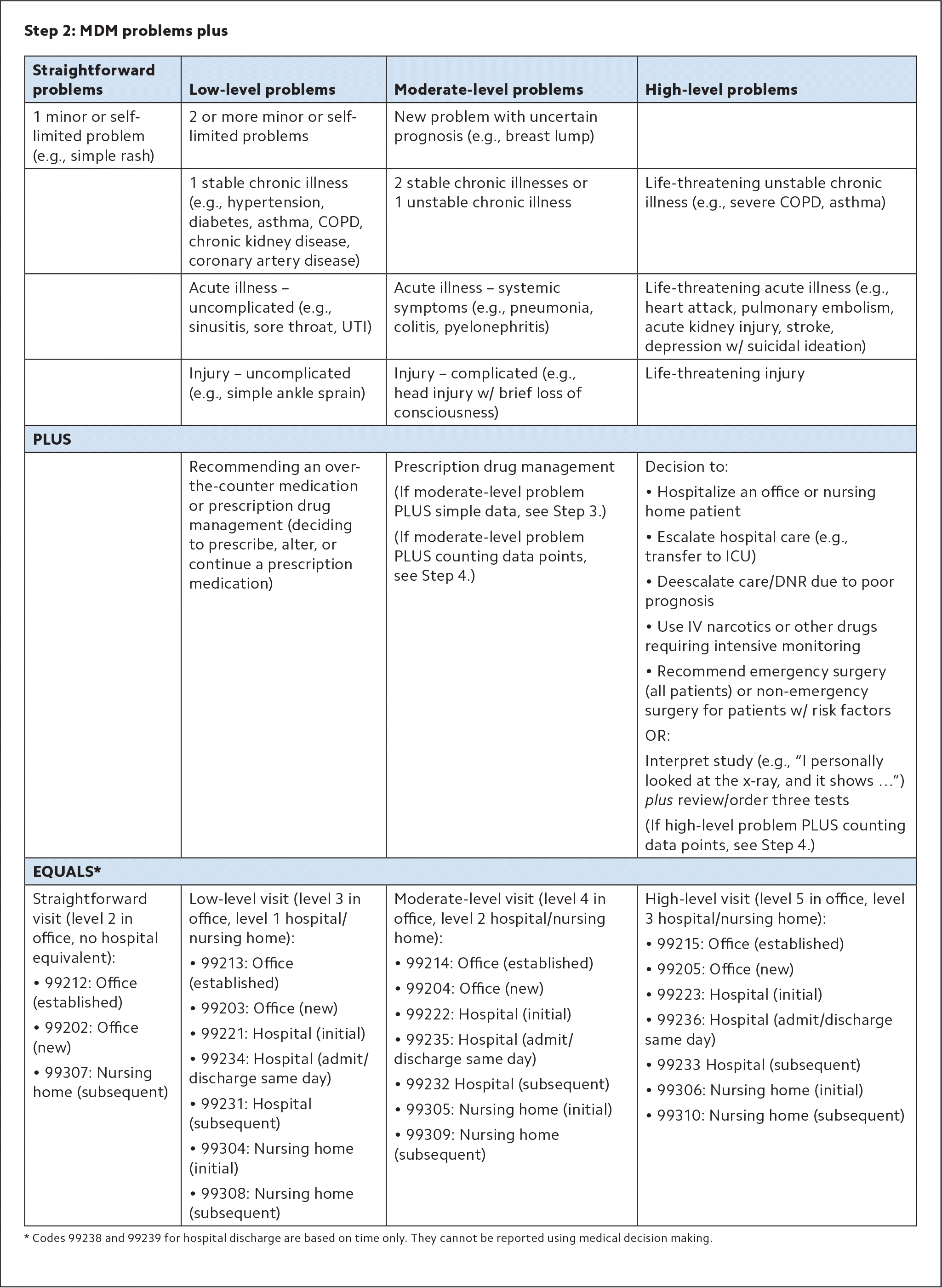
| Straightforward problems | Low-level problems | Moderate-level problems | High-level problems |
|---|---|---|---|
| 1 minor or self-limited problem (e.g., simple rash) | 2 or more minor or self-limited problems | New problem with uncertain prognosis (e.g., breast lump) | |
| 1 stable chronic illness (e.g., hypertension, diabetes, asthma, COPD, chronic kidney disease, coronary artery disease) | 2 stable chronic illnesses or 1 unstable chronic illness | Life-threatening unstable chronic illness (e.g., severe COPD, asthma) | |
| Acute illness – uncomplicated (e.g., sinusitis, sore throat, UTI) | Acute illness – systemic symptoms (e.g., pneumonia, colitis, pyelonephritis) | Life-threatening acute illness (e.g., heart attack, pulmonary embolism, acute kidney injury, stroke, depression w/ suicidal ideation) | |
| Injury – uncomplicated (e.g., simple ankle sprain) | Injury – complicated (e.g., head injury w/ brief loss of consciousness) | Life-threatening injury | |
| PLUS | |||
| Recommending an over-the-counter medication or prescription drug management (deciding to prescribe, alter, or continue a prescription medication) | Prescription drug management (If moderate-level problem PLUS simple data, see Step 3.) (If moderate-level problem PLUS counting data points, see Step 4.) | Decision to:
OR: Interpret study (e.g., “I personally looked at the x-ray, and it shows …”) plus review/order three tests (If high-level problem PLUS counting data points, see Step 4.) | |
| EQUALS* | |||
Straightforward visit (level 2 in office, no hospital equivalent):
| Low-level visit (level 3 in office, level 1 hospital/nursing home):
| Moderate-level visit (level 4 in office, level 2 hospital/nursing home):
| High-level visit (level 5 in office, level 3 hospital/nursing home):
|
Step 3: MDM with simple data
Moderate-level problem PLUS one of the following:
- Interpret one study (e.g., “I personally looked at the x-ray, and it shows …”),
- Discuss patient management or a study with an external physician (one who is not in the same group practice as you or is in a different specialty or subspecialty),
- Modify workup or treatment because of social determinants of health.
EQUALS moderate-level visit, even without medication management (see codes in Step 2).
Step 4: MDM counting data points
Moderate-level problem PLUS at least three points from data counting (below),
EQUALS moderate-level visit (see codes in Step 2).
High-level problem PLUS at least two of these three:
- Interpret one study (e.g., "I personally looked at the x-ray, and it shows..."),
- Discuss patient management or a study with an external physician,
- At least three points from data counting (below),
EQUALS high-level visit (see codes in Step 2).
Data counting:
- Review/order unique test/study: 1 point for each,
- Review external notes: 1 point for each unique source,
- Assessment requiring use of an independent historian (family member or other person who can provide a reliable history for a patient who is unable to): 1 point max.
Documentation to support your coding should also be easier going forward. While documenting a medically appropriate history and physical exam is still certainly important for good patient care, it's no longer required for coding; therefore, you should be able to determine the code level from only a few lines of documentation. The quiz below provides some examples to pair with the coding template for practice.
Hopefully, using this step-by-step approach to the 2023 E/M coding changes will allow you to code many types of visits more quickly and accurately so you can spend more time with your patients and less time on the computer.
DOCUMENTATION AND CODING QUIZ
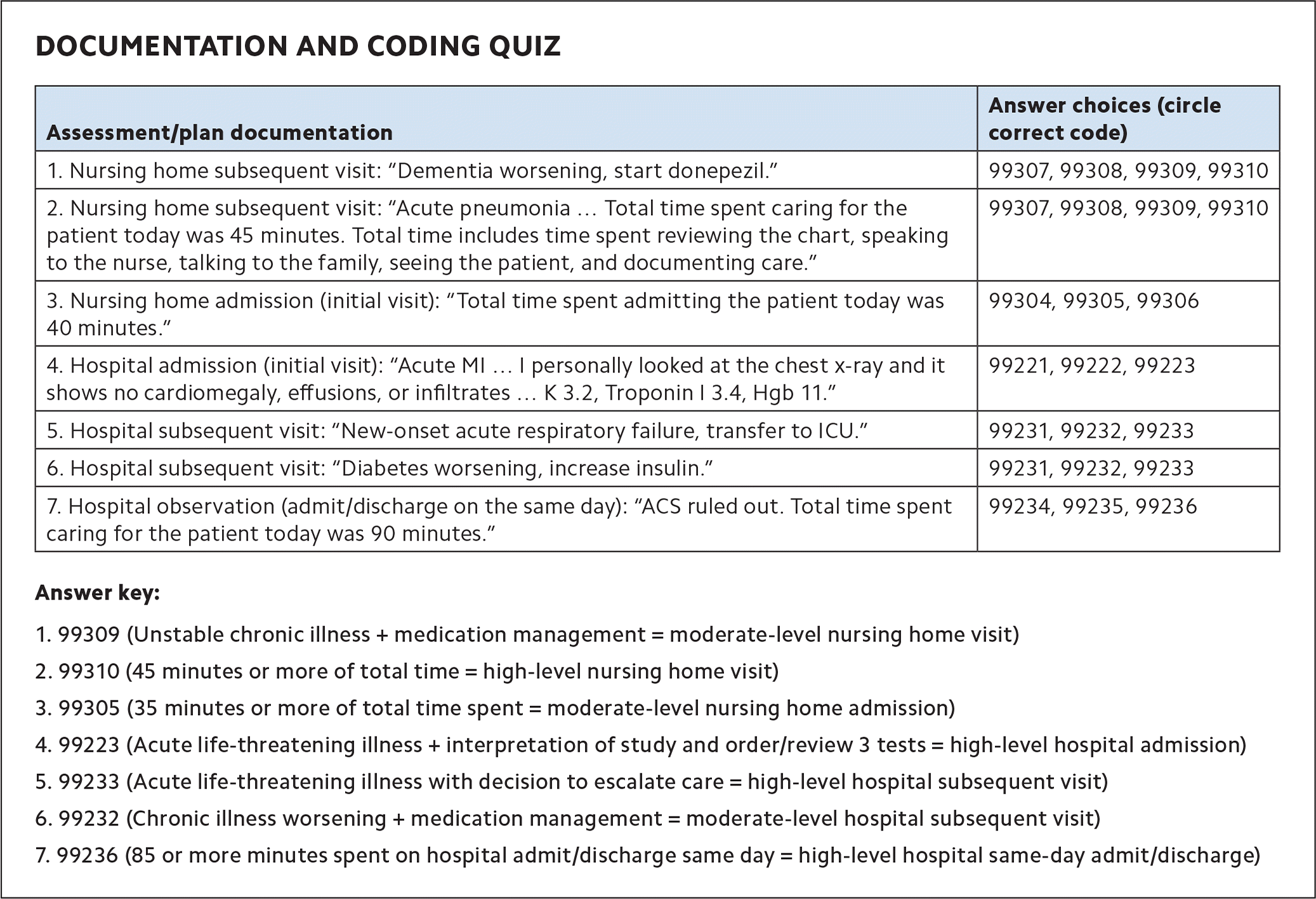
| Assessment/plan documentation | Answer choices (circle correct code) |
|---|---|
| 1. Nursing home subsequent visit: “Dementia worsening, start donepezil.” | 99307, 99308, 99309, 99310 |
| 2. Nursing home subsequent visit: “Acute pneumonia … Total time spent caring for the patient today was 45 minutes. Total time includes time spent reviewing the chart, speaking to the nurse, talking to the family, seeing the patient, and documenting care.” | 99307, 99308, 99309, 99310 |
| 3. Nursing home admission (initial visit): “Total time spent admitting the patient today was 40 minutes.” | 99304, 99305, 99306 |
| 4. Hospital admission (initial visit): “Acute MI … I personally looked at the chest x-ray and it shows no cardiomegaly, effusions, or infiltrates … K 3.2, Troponin I 3.4, Hgb 11.” | 99221, 99222, 99223 |
| 5. Hospital subsequent visit: “New-onset acute respiratory failure, transfer to ICU.” | 99231, 99232, 99233 |
| 6. Hospital subsequent visit: “Diabetes worsening, increase insulin.” | 99231, 99232, 99233 |
| 7. Hospital observation (admit/discharge on the same day): “ACS ruled out. Total time spent caring for the patient today was 90 minutes.” | 99234, 99235, 99236 |

