Key Points for Practice
• Accurate measurement of blood pressure is essential to categorize blood pressure, stratify cardiovascular risk, and guide management.
• A target blood pressure of less than 130/80 mm Hg is recommended for adults with confirmed hypertension and cardiovascular disease, or a 10-year atherosclerotic cardiovascular disease risk of 10% or more.
• Adults with elevated blood pressure or stage 1 hypertension whose estimated 10-year risk of atherosclerotic cardiovascular disease is less than 10% should be treated with nonpharmacologic interventions.
From the AFP Editors
Meta-analyses of observational studies have shown that elevated blood pressure (BP) and hypertension are associated with an increased risk of cardiovascular disease (CVD), end-stage renal disease, subclinical atherosclerosis, and all-cause mortality. A person's risk of hypertension is influenced by various genetic and environmental factors, such as being overweight or obese; diet; alcohol intake; and fitness level. The American College of Cardiology (ACC) and American Heart Association (AHA) recently updated their guideline on the prevention, detection, evaluation, and treatment of high BP in adults. The ACC/AHA recommendations were based on a systematic review that addressed the following questions:
- Is there evidence that home BP monitoring (HBPM) and/or ambulatory BP monitoring (ABPM) are superior to office-based BP measurement by a health care professional for preventing adverse outcomes and achieving better BP control?
- What is the optimal BP target for antihypertensive therapy in adults?
- In adults with hypertension, do various antihypertensive drug classes differ in their comparative benefits and harms?
- In adults with hypertension, does initiating treatment with antihypertensive pharmacologic monotherapy vs. combination therapy differ in comparative benefits and harms on specific health outcomes?
Estimates of the prevalence of hypertension are greatly influenced by the choice of cutoffs used to categorize elevated BP and hypertension, the methods used to establish the diagnosis, and the population studied. The prevalence of hypertension among U.S. adults is substantially higher when the definitions in this guideline are used vs. the definitions in the Seventh Report of the Joint National Committee, but nonpharmacologic therapy would be recommended for most patients with newly diagnosed hypertension based on the current guideline.
Definitions
To prevent and treat hypertension, BP should first be categorized as normal (less than 120 mm Hg systolic and less than 80 mm Hg diastolic), elevated (120 to 129 mm Hg systolic and less than 80 mm Hg diastolic), stage 1 hypertension (130 to 139 mm Hg systolic or 80 to 89 mm Hg diastolic), or stage 2 hypertension (at least 140 mm Hg systolic or at least 90 mm Hg diastolic). Patients whose systolic and diastolic BPs are in different categories should be assigned to the higher category (i.e., a patient with a BP of 128/82 mm Hg should be diagnosed with stage 1 hypertension).
BP Measurement and Out-of-Office Monitoring
Although BP measurement in the office setting is relatively easy, errors are common and can result in a misleading estimation of a patient's true BP. Accurate measurement and recording are essential to categorize BP, ascertain BP-related CVD risk, and guide management of hypertension. Most systematic errors in BP measurement can be avoided by having the patient sit quietly for five minutes before a reading is taken, supporting the limb used to measure BP, ensuring the BP cuff is at heart level, using the correct cuff size, and deflating the cuff slowly. Because individual BP measurements tend to vary, a single reading is inadequate for clinical decision making. Using the average of two or three measurements taken on two or more separate occasions will minimize random error and provide a more accurate basis for estimation of BP. Out-of-office BP measurement in conjunction with telehealth counseling or clinical interventions is recommended to confirm the diagnosis of hypertension and for titration of BP-lowering medication. ABPM is generally accepted as the best out-of-office method, but HBPM is often a more practical approach.
White Coat and Masked Hypertension
White coat hypertension is characterized by elevated BP measurements in the office setting but normal readings on ABPM or HBPM. In contrast, masked hypertension is characterized by normal office readings but ABPM/HBPM readings that are consistently above normal. The risk of CVD and all-cause mortality in persons with masked hypertension is similar to that in those with sustained hypertension, and about twice as high as in persons with normal BP. Some studies have identified a small increase in the risk of CVD complications and all-cause mortality in patients with white coat hypertension.
The prevalence of white coat hypertension ranges from 13% to as high as 35% in some populations. In adults with untreated systolic BP greater than 130 mm Hg but less than 160 mm Hg, or diastolic BP greater than 80 mm Hg but less than 100 mm Hg, it is reasonable to screen for white coat hypertension using daytime ABPM or HBPM before the diagnosis of hypertension is made. Screening for masked hypertension with ABPM or HBPM is reasonable in adults whose untreated office BP is consistently 120 to 129 mm Hg systolic or 75 to 79 mm Hg diastolic.
Treatment
Physicians caring for patients with high BP should focus on overall patient health, with an emphasis on reducing the risk of future adverse CVD outcomes. All patient risk factors should be managed in an integrated fashion with a comprehensive set of nonpharmacologic and pharmacologic strategies.
NONPHARMACOLOGIC INTERVENTIONS
Weight loss is recommended to reduce BP in adults who are overweight or obese. A heart-healthy diet and increased physical activity through a structured exercise program are recommended. Sodium intake should be reduced, and potassium should be supplemented unless contraindicated. Alcoholic drinks should be limited to two per day for men, or one per day for women.
PHARMACOLOGIC TREATMENTS
The use of BP-lowering medications is recommended for secondary prevention of recurrent cardiovascular events in patients with clinical CVD and an average BP of 130 mm Hg or greater systolic or 80 mm Hg or greater diastolic. Medication is recommended for primary prevention in adults with an estimated 10-year risk of atherosclerotic CVD of 10% of more and an average BP of 130 mm Hg or greater systolic or 80 mm Hg or greater diastolic. (A risk calculator is available at http://tools.acc.org/ASCVD-Risk-Estimator-Plus.)
First-line agents include thiazide diuretics, calcium channel blockers, and angiotensin-converting enzyme inhibitors or angiotensin receptor blockers. Initiation of BP-lowering therapy with two first-line agents of different classes (as separate agents or in a fixed-dose combination) is recommended for adults with stage 2 hypertension and an average BP more than 20/10 mm Hg above their target. Therapy with a single agent is reasonable in adults with stage 1 hypertension and target BP less than 130/80 mm Hg. The dosage should be titrated and additional agents added sequentially to achieve the BP target. Simultaneous use of an angiotensin-converting enzyme inhibitor or angiotensin receptor blocker, and/or renin inhibitor is not recommended.
Treatment Goals
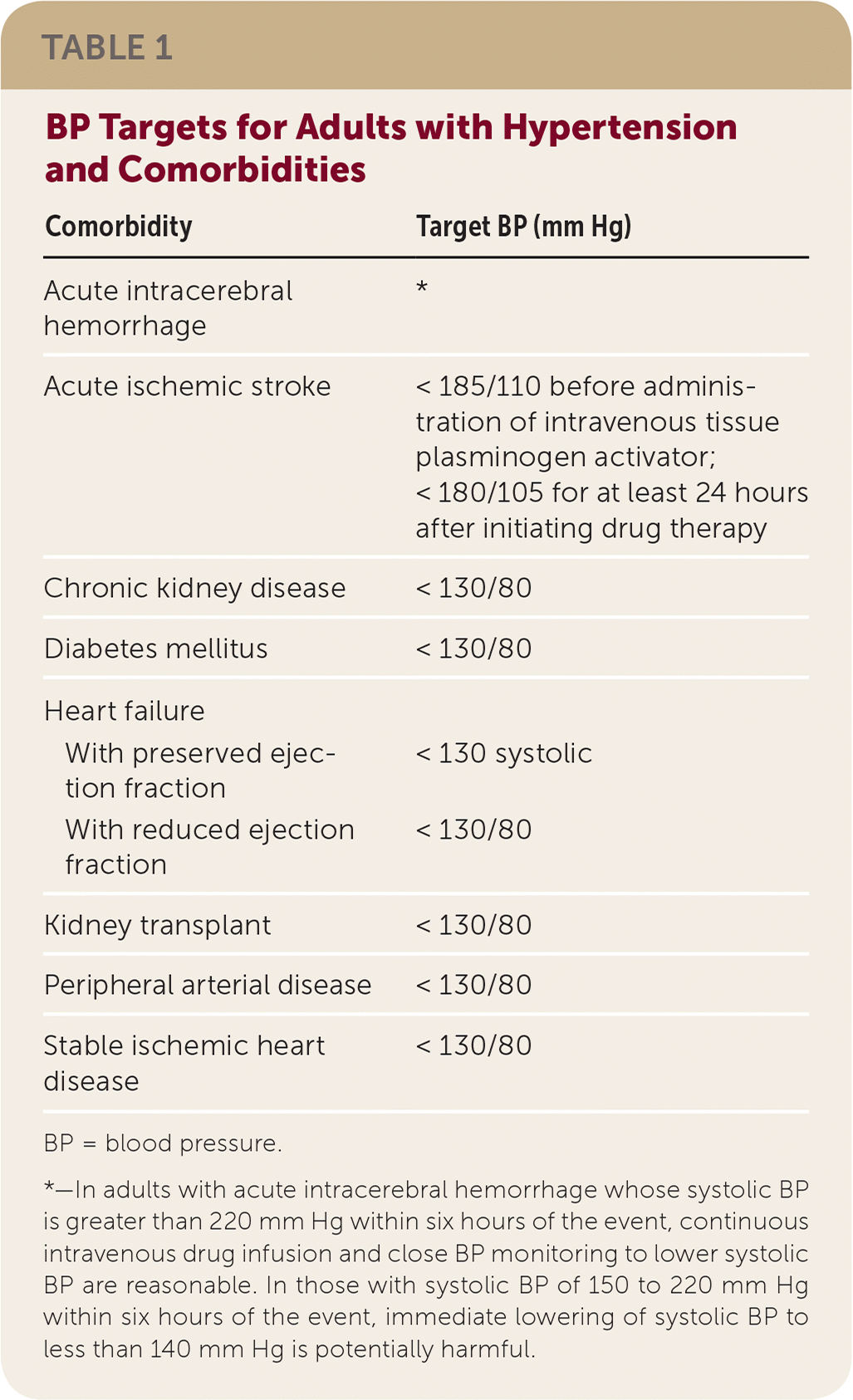
A target BP of less than 130/80 mm Hg is recommended for adults with confirmed hypertension and CVD or a 10-year atherosclerotic CVD risk of 10% or more. A target of less than 130/80 mm Hg may be reasonable for adults with confirmed hypertension but no additional markers of increased CVD risk. Target BPs for adults with hypertension and comorbid conditions are shown in Table 1.
TABLE 1. BP Targets for Adults with Hypertension and Comorbidities
| Comorbidity | Target BP (mm Hg) | |
|---|---|---|
| Acute intracerebral hemorrhage | * | |
| Acute ischemic stroke | < 185/110 before administration of intravenous tissue plasminogen activator; < 180/105 for at least 24 hours after initiating drug therapy | |
| Chronic kidney disease | < 130/80 | |
| Diabetes mellitus | < 130/80 | |
| Heart failure | ||
| With preserved ejection fraction | < 130 systolic | |
| With reduced ejection fraction | < 130/80 | |
| Kidney transplant | < 130/80 | |
| Peripheral arterial disease | < 130/80 | |
| Stable ischemic heart disease | < 130/80 | |
BP = blood pressure.
*—In adults with acute intracerebral hemorrhage whose systolic BP is greater than 220 mm Hg within six hours of the event, continuous intravenous drug infusion and close BP monitoring to lower systolic BP are reasonable. In those with systolic BP of 150 to 220 mm Hg within six hours of the event, immediate lowering of systolic BP to less than 140 mm Hg is potentially harmful.
Follow-Up
Adults with elevated BP or stage 1 hypertension whose estimated 10-year risk of atherosclerotic CVD is less than 10% should be treated with nonpharmacologic interventions and reevaluated in three to six months. Those with stage 1 hypertension whose estimated risk is 10% or more should receive BP-lowering therapy in conjunction with nonpharmacologic interventions, then undergo repeat evaluation in one month. Adults with stage 2 hypertension should be evaluated by or referred to a primary care physician within one month, receive a combination of nonpharmacologic interventions and BP-lowering medications (with two agents from different classes), and undergo repeat evaluation in one month. Adults with very high BPs (systolic BP of 180 mm Hg or higher, or diastolic BP of 110 mm Hg or higher) should be evaluated quickly and provided drug therapy.
Editor's Note: The American Academy of Family Physicians (AAFP) does not endorse the 2017 ACC/AHA guideline on hypertension and continues to endorse the 2014 Evidence-Based Guideline for the Management of High Blood Pressure in Adults. The AAFP also supports its 2017 guideline, which was codeveloped with the American College of Physicians: Pharmacologic Treatment of Hypertension in Adults Aged 60 Years or Older to Higher Versus Lower Blood Pressure Targets (https://www.aafp.org/patient-care/clinical-recommendations/all/hypertension-over-60.html). For more details, see the accompanying editorial by Dr. LeFevre and AAFP News article (https://www.aafp.org/news/health-of-the-public/20171212notendorseaha-accgdlne.html).
Guideline source: American College of Cardiology/American Heart Association
Evidence rating system used? Yes
Systematic literature search described? Yes
Guideline developed by participants without relevant financial ties to industry? No
Recommendations based on patient-oriented outcomes? Yes
Published source:J Am Coll Cardiol. [published online ahead of print November 7, 2017]

