Am Fam Physician. 2020;101(1):49-52
Author disclosure: Dr. Lembke disclosed that she has received consulting fees as a medical expert witness on the plaintiff side in federal and state opioid litigation.
Case Scenario
My patient is a 54-year-old construction worker who has been taking prescribed opioids for more than a decade for chronic knee and back pain. During the past year, he has admitted that he feels “stuck on these drugs.” His pain is not well controlled, and his wife has complained that he seems “out of it.” We have talked about reducing his prescription or stopping opioids, but he is reluctant and worried. How can I help my patient taper his regimen to minimize withdrawal and maximize his chances for success?
Commentary
Decreasing or discontinuing long-term opioid therapy (opioids taken daily for 30 days or longer) is clinically challenging, especially in patients on high dosages (e.g., morphine equivalent is greater than 90 mg per day).
BROACHING THE SUBJECT
Suggesting an opioid taper can trigger extreme anxiety in patients. The physician should acknowledge this feeling, normalize it, and express empathy for the patient’s distress.
Begin by telling the patient, “I’ve been thinking a lot about your chronic pain.” This communicates that the benefit of an opioid taper has been carefully considered and that the plan for a taper is not impulsive or retaliatory. It is rather the result of careful deliberation, including medical assessment of risk vs. benefit.
Arrange extra time to discuss this delicate topic. Anticipate the patient’s strong emotional reaction. Pledge your support through this difficult process. Facilitating a good therapeutic alliance increases the chances of a successful taper.
RISK–BENEFIT CALCULATION
The risk–benefit calculation helps determine whether the relative benefits of opioid therapy outweigh the risks and whether a dose decrease or full taper is indicated.3 This calculation is not about any specific dose of opioids but about weighing the risks and benefits in a given patient and tapering to a place where benefits exceed risks, including the risks of a taper.
An opioid taper should be considered when any of the following situations occur:
Failure to provide significant analgesia despite incremental dose increases,
Lack of functional improvement over time,
Prescription of high dosages of opioids (morphine equivalent is greater than 90 mg per day),
Significant physical risk factors are present (e.g., sleep apnea, prolonged QT interval, pulmonary disease),
Adverse effects of medication interfere with quality of life,
Dangerous coprescribing (e.g., benzodiazepines, muscle relaxants, other sedatives),
Patient request.
ADDICTION HAPPENS
Think of the four Cs (control, compulsion, craving, continued use despite consequences) to remember the 11 diagnostic criteria for substance use disorders from the Diagnostic and Statistical Manual of Mental Disorders, 5th ed. (DSM-5).4 Control refers to out-of-control use (e.g., using more than intended); compulsion refers to mental preoccupation with using and using against a conscious desire to abstain; craving refers to physiologic and/or mental states of wanting; and continued misuse despite consequences refers to persistent misuse despite social, legal, economic, interpersonal, and other problems that arise as a result of use.
It is important to distinguish between dependence and addiction. Someone who takes a prescribed daily opioid pill for pain may be dependent on opioids (i.e., needs more and more medication to get the same effect [tolerance]) and may experience opioid withdrawal when cutting back or discontinuing use; however, the person is not addicted to opioids by virtue of taking them as prescribed. This individual would meet criteria for a diagnosis of opioid dependence, physiologic, but not a diagnosis of opioid use disorder.
It is possible to have an opioid use disorder without being dependent. Someone who binges on opioids to the point of respiratory suppression or risking death, but does not take opioids daily, will not develop the tolerance and withdrawal symptoms (i.e., physical dependence) that arise with daily use. This individual would meet criteria for a diagnosis of opioid use disorder; however, they would not have a diagnosis of opioid dependence, physiologic.
Patients who become addicted to prescription opioids may take more of the medication than directed; hoard the medication and take a single large dose to achieve an altered mental status; take the medication to improve mood and energy rather than to treat pain; spend a lot of time and effort trying to get more medication; crave the medication; or get into personal, occupational, or medical difficulties because of use of the medication.
Patients who develop an opioid use disorder should be referred for treatment. Of the available opioid use disorder treatments, robust evidence supports opioid agonist therapy in the form of buprenorphine/naloxone (Suboxone) or methadone maintenance5 (see previous articles in American Family Physician about buprenorphine therapy6 and medical treatment options for opioid use disorder7).
VELOCITY MATTERS (AND SO DOES VALIDATION)
Velocity. The standard recommendation to decrease opioid doses by 5% to 10% of the starting dose every one to two weeks8 is intolerable for many patients using long-term opioid therapy for chronic pain. Many patients need to decrease by less than 5% every month, with even smaller decrements toward the end of the taper.9 Some patients require many months to wean off chronic opioid therapy, especially those who have taken opioids daily for decades.
It may be helpful to keep the same dosing cadence (e.g., twice daily, three times daily), especially in the beginning of the taper. The brain is habituated to having the medication at set times. If the patient is on a regimen of taking doses two times or three times a day, keep that schedule during the taper for as long as possible.
Patient involvement, and appropriate autonomy, is vital to success in tapering. If the patient takes several different opioids, let the patient decide which medication to taper first. Include the patient in the decision of how much to taper and when.
Breaks in the taper are appropriate. Patients can maintain a given dose for some period before continuing. For example, if the patient has an important event scheduled and does not want to risk being in low-grade withdrawal, including subtle psychological symptoms of withdrawal such as anxiety, irritability, and dysphoria, it is reasonable to defer the next decrement in dose. It is imperative never to go backward during the taper (i.e., increase the dose). Going back up on the dose risks losing the hard work already invested. Nonaddictive medications can help relieve symptoms of withdrawal (Table 1). Benzodiazepines must be avoided when treating opioid withdrawal because they can lead to dependence and addiction.10 Time is the most important ally in opioid withdrawal. Counsel patience with your patients.
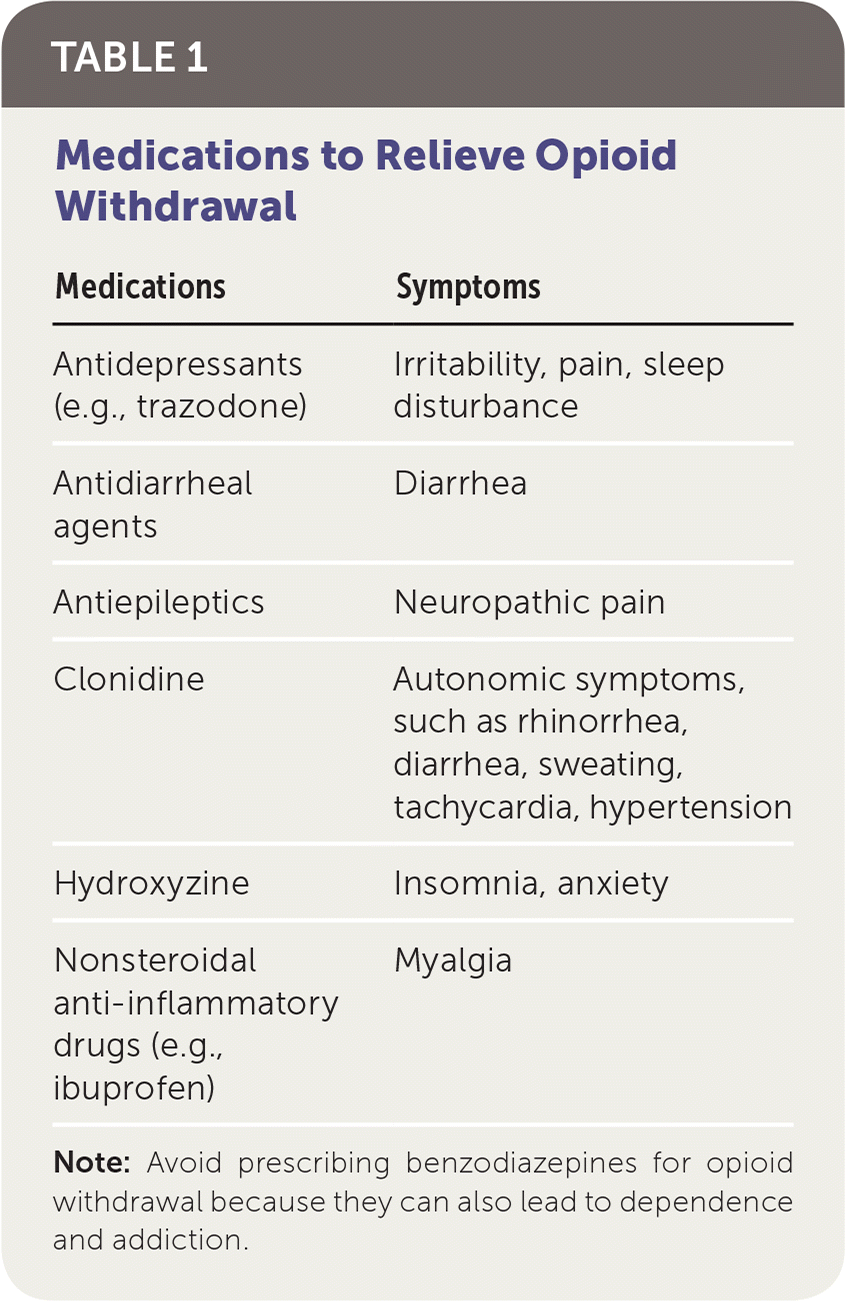
| Medications | Symptoms |
|---|---|
| Antidepressants (e.g., trazodone) | Irritability, pain, sleep disturbance |
| Antidiarrheal agents | Diarrhea |
| Antiepileptics | Neuropathic pain |
| Clonidine | Autonomic symptoms, such as rhinorrhea, diarrhea, sweating, tachycardia, hypertension |
| Hydroxyzine | Insomnia, anxiety |
| Nonsteroidal anti-inflammatory drugs (e.g., ibuprofen) | Myalgia |
If opioid use disorder is detected and diagnosed (see Addiction Happens section), normalize the disease of addiction and make provisions for treatment.
Validation. Physicians need to emphasize the arduous nature of opioid withdrawal (Table 2) so that when patients do experience intense withdrawal, they feel validated and understood.
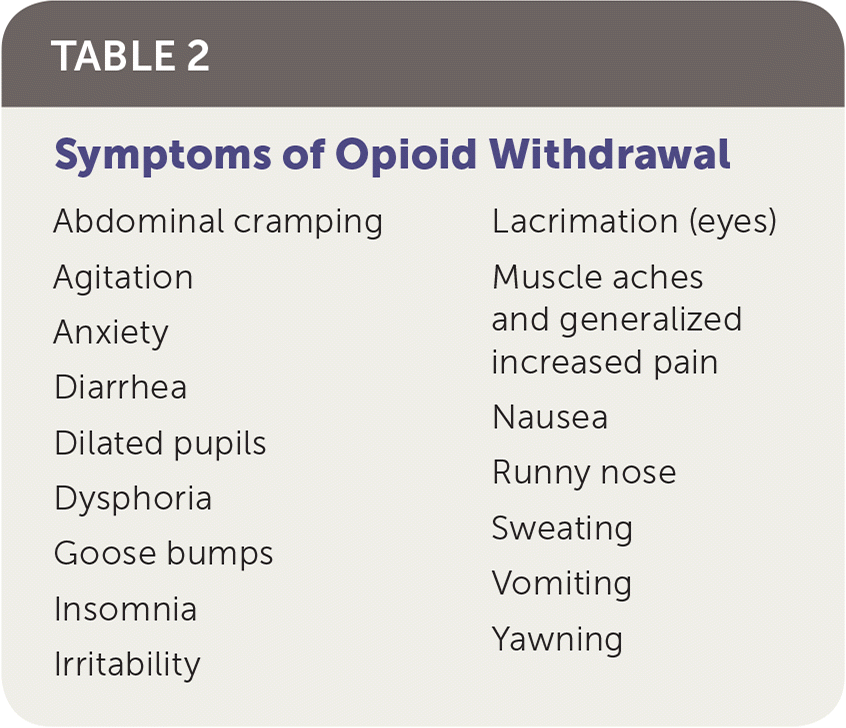
| Abdominal cramping |
| Agitation |
| Anxiety |
| Diarrhea |
| Dilated pupils |
| Dysphoria |
| Goose bumps |
| Insomnia |
| Irritability |
| Lacrimation (eyes) |
| Muscle aches and generalized increased pain |
| Nausea |
| Runny nose |
| Sweating |
| Vomiting |
| Yawning |
Physicians should warn patients that their body pain will get worse each time the opioid dose is decreased, but that with time and with the body adjusting to the new lower dose (approximately four weeks), the pain level will return to baseline.
Many patients believe the physical pain they experience during opioid withdrawal is evidence of their need for medication and/or the enduring pain they will experience without opioids. However, the increased pain patients experience after the dosage decrease does not indicate progression of their underlying pain condition. Rather, the pain represents time-limited, opioid withdrawal–mediated pain.11 Patients with chronic pain who successfully taper down or off of long-term opioid therapy often report improved pain.12,13
OTHER STRATEGIES FOR COPING WITH PAIN
Other treatments for pain should be offered during the taper if not already in place. These include nonopioid medications and nonpharmacologic treatments such as physical therapy, massage, and psychotherapy. Therapeutic interventions can be incorporated into the primary care visit.
First, teach patients mindfulness practices. An example would be to ask them to acknowledge the pain, notice whether something in the environment is making it worse at the moment, and then remember the top three reasons that they want to stay off opioids (e.g., my kids, I do not want to feel dependent on something, my health).
Second, teach patients opposite action skills: acting opposite to the emotional urge in the service of pursuing values or goals. Many patients with chronic pain become obsessively focused on their pain and let it limit their participation in many activities. By contrast, patients can engage in counteractivities, within reason, despite pain being present. This does not mean asking patients to go beyond safe limits, but rather to engage in engrossing physical and mental activities as tolerated, despite being in pain.
Regarding the patient in the case scenario, the physician could use the BRAVO protocol for broaching the subject of tapering his opioid prescription. The physician should be empathetic and address the risks and benefits of the taper. The physician could then provide a tapering plan, if warranted, and suggest alternate strategies for addressing pain. Table 3 lists other resources on tapering opioid use. Physicians can also see the recent Health and Human Services Guide for tapering long-term opioid use for guidance.1
| American Family Physician pamphlet on opioid risks and side effects https://www.aafp.org/patient-care/public-health/pain-opioids.html https://www.aafp.org/patient-care/clinical-recommendations/all/opioid-prescribing.html |
| Dialectical behavior therapy, cognitive behavior therapy, and Living Well with Chronic Illness workshops can be helpful to patients through the tapering process and beyond Body in Mind: https://bodyinmind.org |
| First-person account of patient tapering off of long-term opioid therapy Laura’s Story: https://www.youtube.com/watch?v=75PEivn1IOk |
| National Academy of Medicine – Tapering Guidance for Opioids: Existing Best Practices and Evidence Standards https://nam.edu/event/webinar-tapering-guidance-for-opioids-existing-best-practices-and-evidence-standards/ |
| Oregon Pain Guidance: Tapering—Guidance and Tools https://www.oregonpainguidance.org/guideline/tapering/ |
| Stanford School of Medicine: How to Taper Patients Off of Chronic Opioid Therapy https://online.stanford.edu/courses/som-ycme0022-how-taper-patients-chronic-opioid-therapy |
| U.S. Department of Health and Human Services: HHS Guide for Clinicians on the Appropriate Dosage Reduction or Discontinuation of Long-Term Opioid Analgesics https://www.hhs.gov/opioids/sites/default/files/2019-10/Dosage_Reduction_Discontinuation.pdf |